Postoperative complications / complications after surgery
Introduction / definition
The term postoperative complications includes all problems that arise after an operation and that can be very serious. Some of the complications require intensive medical monitoring and rapid therapy.
Furthermore, postoperative complications do not always occur immediately after the operation, but often only in the course of 2 to 14 days afterwards. The occurrence of postoperative complications can largely be avoided by:
- the exclusion of some risk factors,
- good supervision and
- optimal surgical planning.
Risk factors
There are some preoperative factors that make postoperative complications much more likely.
These include:
- old age
- Malnutrition or obesity,
- Diabetes mellitus
- High blood pressure, vascular stenosis
- chronic obstructive pulmonary disease,
- Nicotine or alcohol abuse,
- Kidney failure or heart disease.
All of these risk factors should be ascertained in a detailed admission interview before the operation so that appropriate measures can be taken before, during and after the operation.
Problems can also arise during the operation that significantly increase the incidence of postoperative complications.
These include:
- insufficient volume,
- inadequate respiratory and circulatory monitoring or
- severe fluctuations in blood pressure.
But also a long operation time, the opening of several body cavities and large blood losses can lead to postoperative complications.
Even postoperatively, some circumstances can lead to complications. Here too, inadequate volume administration, too early removal of the ventilation tube and inadequate monitoring play a key role in the occurrence of complications. Inadequate physiotherapeutic breathing therapy, poor hygiene and electrolyte imbalances can also lead to serious complications.
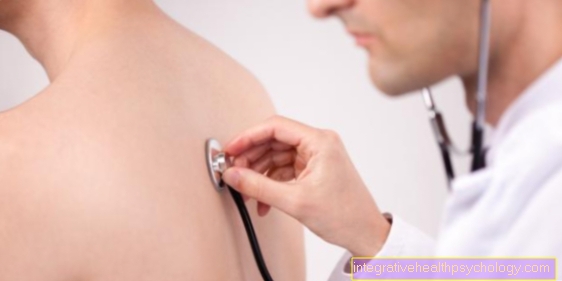
Complications affecting the lungs
The ability of the lungs to function largely determines recovery and the occurrence of complications. Physiotherapy respiratory therapy at an early stage can prevent pneumonia or other complications.
Pleural effusion
The pleural effusion is an accumulation of water between the lungs and the lung membrane. On the one hand, it can occur in the case of a weak heart and then leads to bilateral symptoms. A unilateral pleural effusion occurs reactively after removal of the spleen, partial removal of the liver or as a result of any infection in the abdominal cavity. Clinically, a pronounced pleural effusion leads to dyspnoea and smaller collapsed lung sections. Smaller pleural effusions are initially not noticed.
In the case of effusions below 200ml per side, it is not necessary to drain the liquid with a needle (puncture), otherwise the puncture should be performed using ultrasound.
More on this topic on our page for Pleural effusion.
Pneumothorax
A pneumothorax is the collapse of a lung, usually postoperatively after a central venous catheter has been inserted or as a result of long-term ventilation. The pleura, the lung membrane, is pierced so that air flows into the pleural space and the lungs are compressed from the outside. Depending on the severity, pneumothorax is associated with shortness of breath and increased heart rate. It can be diagnosed by listening to the other sides and tapping the lungs and requires rapid treatment.
This consists of the installation of a chest drain. With the help of the drainage, the air is released from the pleural space and the lungs can expand again.
More on this topic on our website Pneumothorax.
Atelectasis
Atelectasis is a collapsed section of the lung. A segment or main bronchus is usually obstructed by a plug of mucus, more rarely by blood or a foreign body. This means that the affected area continues to be supplied with blood, but oxygen can no longer be absorbed in this area. There is less breathing on the affected side. The diagnosis is mainly symptom-oriented and made through percussion and auscultation.
Therapy is carried out by appropriate positioning in order to loosen the obstruction of the mucus plug. In addition, tapping and vibration therapy. At the same time, drugs are administered to dissolve the secretion.
More about this on our website Atelectasis
pneumonia
Pneumonia is pneumonia, which is one of the main complications after an operation. It is often caused by insufficient ventilation during postoperative pain-related and insufficient breathing activity. Pneumonia can also occur with long-term ventilation. Clinically, there are fast and shallow breaths, fever, sputum when coughing and shortness of breath.
The therapy consists of a pronounced physiotherapeutic breathing therapy to completely ventilate the lungs. Antibiotics are also given.
More about this on our website Pneumonia.
Respiratory failure
Respiratory failure is a breathing disorder and is one of the main complications, as it leads to an insufficient supply of oxygen to all organs. There is a drop in oxygen saturation and, in some cases, the CO2 concentration also increases. Symptoms of shortness of breath appear as superficial hackling, cyanosis (blue discoloration of the skin and mucous membranes), confusion, restlessness and fear.
Therapy is initially the administration of oxygen through so-called oxygen glasses. If this measure does not lead to a sufficient increase in saturation, the patient must be mechanically ventilated. Close control of blood gases and permanent control of oxygen saturation are essential.
Read more on the subject at: Decreased oxygen saturation
Pulmonary embolism
Pulmonary embolism is one of the most dangerous postoperative complications. The cause is a deep leg or pelvic vein thrombosis due to insufficient blood flow or too little exercise. For this reason, all patients who are severely restricted in their mobility postoperatively are treated with thrombosis prophylaxis. If this blood clot loosens, it is transported to the large pulmonary veins, where a large bronchus is laid. Suddenly there is massive shortness of breath with breath-related pain, an increase in heart rate and a drop in blood pressure.
Therapy consists of administering oxygen and dissolving the clot with the help of anticoagulant drugs in therapeutic doses. In the event of inadequate therapy, pulmonary embolism can be fatal.
More on this important topic on our website Pulmonary embolism.
Complications affecting the heart
Complications after heart surgery
Heart surgery can be performed on the beating or standing heart, depending on the treatment.
In such cases, when it is necessary to stop the heart during the surgical procedure, there is a risk of developing special complications. During the heart operation, the circulatory system must be powered by a heart-lung machine. Only in this way can the vital organs be supplied with oxygen and nutrients. The procedures that are now used as standard are relatively safe, but postoperative complications can still occur after a heart operation using a heart-lung machine. Above all, the formation of blood clots, which can lead to a stroke or a heart attack, plays a crucial role in this context.
Other typical postoperative complications after performing heart surgery are based on the type of surgical intervention. Above all, the wound pain after heart surgery is perceived by many of the affected patients as very stressful. For this reason, targeted pain therapy should be initiated immediately after the heart operation. In this context, the principle applies that after a heart operation, a patient may receive as many painkillers as they actually need. Adequate pain relief has been shown to have a positive effect on the healing process.
In addition, the temporary occurrence of pronounced fatigue and general weakness is one of the most common postoperative complications after extensive heart surgery. The reason for this is the fact that operations on the heart are a great burden on the organism, which can lead to physical and psychological exhaustion. This possible postoperative complication can be problematic especially for elderly and generally debilitated patients. A recovery phase of a few weeks should therefore be planned for even after complication-free heart surgery.
In addition, many patients report postoperative complications that affect memory after heart surgery. Concentration disorders, memory gaps or confusion in a heart operation are mainly caused by the anesthesia and the changed circulatory conditions during the surgical procedure. In patients who already suffered from memory problems before the heart operation, the symptoms can worsen for a few days. Hallucinations are also typical postoperative complications after a heart operation. Furthermore, the induction of general anesthesia can interrupt the day-night rhythm. This can lead to pronounced sleep disorders within the first few nights. Severe pain after heart surgery can exacerbate this phenomenon.
In addition, temporary visual disturbances are one of the most common postoperative complications after heart surgery. The visual disturbances occur in the affected patients within the first few weeks after the surgical procedure and manifest themselves in the form of: blurred vision, eye flickering and / or visual hallucinations.
Depending on the type and severity of the heart disease that requires surgical treatment, postoperative cardiac arrhythmias can also occur. The so-called "atrial fibrillation" is one of the most common cardiac arrhythmias that occur as a postoperative complication after a heart operation. This manifests itself in an irregular, rapid pulse and palpable palpitations. In most cases, this postoperative complication can be treated with medication without any problems. However, some of the affected patients may need electrical cardioversion, where an electrical pulse is used to restore normal heart rhythm.
The occurrence of fluid retention, so-called edema, is one of the typical postoperative complications after a heart operation. In affected patients, fluid shifts into the tissue during the surgical procedure. Clinically, this complication can be recognized by rapid weight gain and severe swelling in the hands and feet. In many cases, the excess fluid is eliminated without medical intervention within the first postoperative days. If this is not the case, diuretic therapy must often be initiated.
Read more on the topic: Post-op swelling
In addition to these rather harmless, easily treatable postoperative complications after heart surgery, more serious complaints can also be caused. Infections and wound healing disorders in particular can be a clinical problem. If the sternum is cut during the heart operation, bone healing disorders can subsequently occur.
In addition, in the case of open heart surgery, there is a risk of neurological complications. Individual nerve fibers can be affected during heart surgery. As a result, symptoms of paralysis and sensory disturbances can occur. The paralysis of the diaphragm in particular is a serious problem.
Cardiovascular failure
The acute cardiovascular failure is accompanied by a sudden drop in blood pressure.
Clinically, patients become pale and the skin turns bluish, arms and legs become cold as the blood supply is restricted to major organs. Such failure is caused by a significantly too high heart rate, shortness of breath, too shallow rapid breathing and pulmonary edema.
Therapy consists of adequate oxygen administration, ventilation if necessary, creation of a venous access and slow volume administration. In addition, the patients must be monitored by intensive care.
The derailed cardiac insufficiency is the result of an acute pump failure of the heart, for example a heart attack, pulmonary embolism or various cardiac arrhythmias. Clinically, the patients suffer from shortness of breath, significantly increased heart and respiratory rates, which, however, lead to ineffective oxygen uptake and oxygen transport.
Therapy consists of elevating the upper body, lowering the volume, administering oxygen and treating the high heart rate with medication.
Continuity syndrome
A continuity syndrome is the patient's limited ability to cooperate with the risk of self-endangerment through postoperative, uncontrolled motor restlessness, states of confusion or other variable accompanying symptoms. Depending on the extent of the limited cooperation, the breathing therapy can become ineffective and the uncontrolled restlessness can lead to a lack of sleep, which can lead to physical exhaustion after about 2 days. Predisposing for a continuity syndrome are, for example, alcohol and drug abuse, stress, sleep deprivation and long periods of rest after surgery. The symptoms usually begin acutely and are very individual in terms of severity and intensity. They usually worsen at night and can lead to disorientation, panic attempts to escape and the forcible removal of catheters and probes.
Therapy and prophylaxis consists of a continuous administration of clonidine, which both lowers blood pressure and helps against restlessness, and continuous blood pressure and heart rate monitoring.
You can find more on this topic on our website Continuity syndrome.
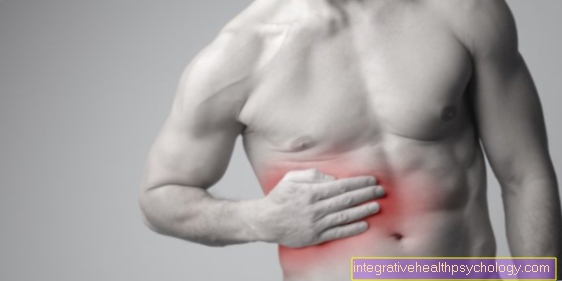
Stress ulcer
Stress ulcers are acute lesions of the upper gastrointestinal tract. The cause is an expired shock phase, which can often be days ago.
Predisposing factors are major interventions, multiple trauma, burns, septic complications or injuries to the central nervous system. Clinically, the stomach contents are bloody, possibly with vomiting of blood. In some cases, the organ is perforated with an acute abdomen and free air under the diaphragm.
Therapy consists of gastric lavage with 14 ° C cold water and an attempt at endoscopic hemostasis. If the attempt is unsuccessful, the bleeding must be stopped surgically. To avoid a stress ulcer, oral food is given early, and a gastric tube is inserted to relieve the stomach and control bleeding. Pharmacological prophylaxis with proton pump inhibitors is also possible.
You can find out more about ulcers and their various forms on our gastric ulcer page.
Fever after an operation
Since a postoperative increase in temperature is part of the post-aggressive metabolism, a slight increase in temperature below 38.5 ° C up to 3 days postoperatively is not critical.
Initially significantly increased temperature and any increase in temperature beyond these 3 days requires thorough clarification and, if necessary, therapy, as fever can be a clear sign of an infection. The cause can be wound or urinary tract infections. Both should be checked by regular checks of the wound and urine and, if the diagnosis is positive, treated with antibiotics.
In the event of a wound infection, it must be opened and cleaned. Pneumonia also leads to fever and should be urgently clarified and treated.
If central venous catheters are in place, these are often the cause of infections, as bacteria can accumulate on the materials. The fever suddenly rises sharply, the entry point is red and there are no further symptoms. Initially, the catheter should be removed immediately and examined for bacteria. A new catheter should only be inserted after 24 hours.
Blood poisoning is the spread of bacteria from a source of infection into the entire bloodstream. Since fulminant sepsis can be fatal, the cause should be found and treated urgently.
Please also read the article: Fever after surgery
Passage disruption of the gastrointestinal tract
Postoperatively, symptoms of paralysis of the gastrointestinal tract can occur. Stomach paralysis can be caused by peritonitis, potassium deficiency, abscesses or hematomas. Clinically, nausea, vomiting, belching, bloating, and gastroesophageal reflux occur.
Therapy consists of placing a nasogastric tube, intravenous administration of peristaltic drugs and laxative measures.
Intestinal paralysis is one of the most common postoperative complications and results from normal postoperative intestinal paralysis. Immobility of the bowel is still normal up to 4 to 5 days postoperatively, if it lasts longer, it requires clarification and therapy. The intestine can be immobile due to external manipulation, an insufficient supply of oxygen or hematomas and abscesses in the abdomen. Clinically, patients suffer from bloating, nausea and vomiting after anesthesia. The intestinal noises are very meager and electrolyte imbalances can occur.
First, a nasogastric tube should be inserted, and the intestine should be stimulated with medication. The best way to avoid postoperative intestinal paralysis is early oral feeding and early mobilization.
Secondary bleeding
Postoperative bleeding into the wound area and not completely closed vessels or coagulation defects occur.
Bleeding in the throat is particularly dangerous, as even small amounts can narrow the windpipe and cause shortness of breath.
Clinically, massive secondary bleeding leads to a drop in blood pressure due to the loss of blood and to an increase in pulse, in which the heart tries to compensate for the loss by pumping harder. The drains draw blood and the wound area may increase in size.
The therapy depends on the extent of the rebleeding. In the event of major secondary bleeding, the wound must be reopened in order to find and eliminate the cause of the bleeding.
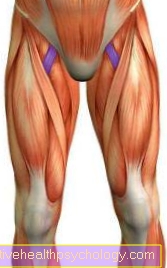
Complications after a hip replacement
In general, the insertion of an artificial hip joint is a medical standard. This surgical method is a relatively safe procedure that can usually be carried out safely and without problems due to the high level of experience. Nevertheless, postoperative complications can occur in some cases after a total hip replacement.
Above all, the so-called “general operational risks”, which can arise regardless of the type of surgical intervention, play a decisive role in this context. The most common general postoperative complications following hip replacement surgery include blood loss, the development of inflammatory processes and the occurrence of thrombosis.
The type of surgery can also cause specific postoperative complications. Immediately after the hip replacement surgery, bacterial pathogens can migrate into the artificial hip joint and lead to inflammatory processes or infections there.
In addition, the dislocation, also called dislocation, of the individual parts of the TEP is one of the most common postoperative complications.
Read more on the subject at: Hip dislocation after a hip prosthesis
In addition, in the course of the healing process, there may be a loosening of the hip TEP components and the associated restriction of joint function. These early postoperative complications can be observed again and again, but occur comparatively rarely.
Fewer than one in one hundred hip replacement operations lead to the occurrence of serious postoperative complications that require treatment. However, it must be noted in this context that new complications can occur after a hip replacement surgery, even after several weeks to months.
The most common late postoperative complication that can occur in the course of a hip replacement surgery is the formation of new bone substance in the area of the joint. In medical terminology, this phenomenon is called "periarticular ossification". This new bone formation can vary in extent depending on the patient and cause further complaints. Depending on the extent of the new bone formation, the patients suffer from pain and significant restrictions in the range of motion even after a successful hip replacement.
Read more on the topic: Hip prosthesis causes pain
Postoperative complications that occur in the course of a hip replacement can, however, largely be prevented. Above all, the one-time irradiation of the hip joint with ionizing radiation leads to a reduction in postoperative complications. This method should be performed within 24 hours before and 72 hours after the planned operation. This method is particularly advantageous for those patients who have an increased risk of new bone formation in the hip joint.
Possible factors that increase the risk of postoperative complications after hip replacement are:
- New bone formation after previous surgical interventions
- Significant mobility restrictions in front of the hip replacement device
- ankylosing spondylitis
- Pronounced tissue damage during the surgical procedure
Complications after bowel surgery
In the case of bowel surgery, a distinction must be made between general and specific postoperative complications. Immediately after the surgical procedure, bleeding may occur within the operating area, which may make another surgical procedure necessary.
Furthermore, the occurrence of inflammatory processes and the development of wound healing disorders are among the most common postoperative complications after an intestinal surgery. In these cases, the affected patients often develop general symptoms with a significant increase in core body temperature and / or pronounced chills. Especially in open interventions with large incisions, weak points can remain in the abdominal wall during or after the healing of the scar, so that an umbilical hernia can occur as a special form of incisional hernia (incisional hernia). This is particularly likely because the navel is a physiological scarring of the tissue of the abdominal wall. It poses a risk for abdominal organs to leak out of the abdomen.
Find out more about this topic in our article Umbilical hernia.
In addition, pain in the area of the abdominal cavity is one of the typical postoperative complications that can be observed even after successful bowel surgery. During the stay in the clinic, this pain can be effectively alleviated by administering adequate pain medication.
An intestinal surgery is usually performed under general anesthesia. The substances administered can have a lasting effect on both the cardiovascular system and the gastrointestinal tract. In this context, after the general anesthesia has been withdrawn, there is a risk that bowel function will be restricted over a longer period of time.
In general, it can be assumed that post-operative complications that arise immediately after the surgical procedure can be treated more easily. The specific postoperative complications after performing an intestinal surgery, however, usually require more extensive therapy. Above all, the paralysis of individual sections of the intestine is one of the most feared post-operative complications after an intestinal operation. The cause of this phenomenon is the immigration of immune cells which lead to local inflammation in the surgical area. However, the activated immune cells not only remain in the area of the operated intestinal sections but also reach other areas of the intestine via the bloodstream. The occurrence of extensive inflammatory processes can provoke a malfunction of the nerve fibers that regulate the control of bowel movements. In the long run, this can cause a so-called intestinal obstruction through various mechanisms. Attempts to restore nerve function after the inflammatory processes have subsided are still considered almost impossible to this day.
In addition, late postoperative complications can occur even after a successful bowel surgery. If parts of the intestine have to be removed during the surgical procedure, this can negatively affect both the utilization of individual food components and the absorption of fluids in the body's circulation. As a result, the affected patients often suffer from severe deficiencies and persistent diarrhea.
Another postoperative complication that can occur after an intestinal surgery with removal of large sections of the intestine is pain after eating. In many cases, these complaints are triggered by overuse of the residual intestine.
Furthermore, scar tissue can develop in the course of the intestinal surgery. This can be irritated by the passage of the chyme. If this leads to chronic irritation of the intestinal mucous membrane, this can lead to inflammatory processes. For this reason, food intake should be strictly regulated immediately after the intestinal surgery. In most cases, only dietary food can be consumed over a longer period of time. This is the only way to prevent overuse of the intestine and prevent rupture of the intestinal walls within the operating area.
In order to reduce the risk of the occurrence of the typical postoperative complications after an intestinal surgery, the affected patients should strictly adhere to the medical rules of conduct. Violation can lead to serious problems which in most cases require lengthy and extensive treatment.
Complications after ovarian removal
In most cases, the ovaries are removed under general anesthesia. For this reason, general postoperative complications can occur shortly after surgery. The substances used in general anesthesia can cause cardiovascular problems immediately after the ovaries have been removed. The drugs used for general anesthesia are now relatively well tolerated, but some patients may experience nausea and / or vomiting. In addition, the activity of the gastrointestinal tract and the urinary bladder is restricted by common anesthetic drugs. In the course of this, postoperative constipation (technical term: constipation) and / or urinary retention can occur.
The most common postoperative complications after removal of the ovaries include the occurrence of secondary bleeding and the development of inflammatory processes in the area of the operation. The risk of rebleeding is a serious problem when the ovaries are removed. The reason for this is the fact that large amounts of blood can seep into the body cavity before the rebleeding is clinically evident. Checking the specific blood values can reduce the risk under certain circumstances. Furthermore, the recently operated woman can develop wound healing disorders.
In addition to these general postoperative complications, specific complications after ovarian removal also play a crucial role. During the operation, the urinary bladder, ureters, or intestines may be injured. Immediately after the surgical procedure, these injuries often show through extensive functional losses in the affected organ. In addition, the operation can lead to the formation of scar tissue, which can lead to discomfort over a longer period of time. Depending on the extent of the tissue damage, the affected patients still suffer from severe abdominal pain weeks after the surgical procedure. In addition, in some cases the surgical procedure has a strong influence on the hormonal cycle. For this reason, many of the women affected develop persistent spotting for weeks.
Further information is available under our topic: Removing the ovaries