blood
Synonyms in a broader sense
Blood cells, blood plasma, blood cells, erytrocytes, platelets, leukocytes
introduction
The function of the blood consists primarily as a transport mechanism. These include nutrients that are transported from the stomach via the liver to the respective target organ, e.g. muscles. In addition, metabolic products such as urea as an end product are transported to the respective excretory organs via the blood.

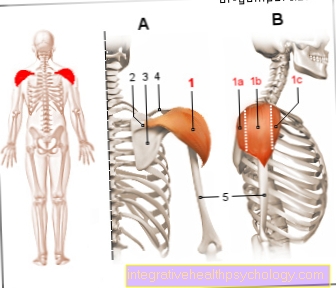
Illustration blood

Blood - Sanguis
- Red blood cells
= red blood cells -
Erythrocytes - White blood cells
= white blood cells -
Leukocytes
2.1 - granulocyte
a - Basophils
b - Eosinophils
c - Neutrophils
2.2 - lymphocytes
2.3 - monocytes - Blood plasma
- Platelets -
Platelets - Oxygenated blood
(blue) - Oxygenated blood
(red) - Heart - Cor
You can find an overview of all Dr-Gumpert images at: medical illustrations
Transport function of the blood
Other substances are transported through the blood:
- Gases such as oxygen, carbon dioxide or nitrogen
- Active ingredients such as vitamins, enzymes and hormones
- Antibodies
- water
- warmth
- Electrolytes
Read more on the subject at: Duties of blood
Amount of blood
The amount of blood in the human body is approx. 7-8% of the body mass. For a man weighing 70 kilos, this corresponds to around 5 liters of blood. With younger children the proportion is approx. 8-9%, with wrestlers approx. 10%. A longer stay at higher altitudes also causes an increase in the amount of blood (Hypervolemia).
A blood volume that is decreased from normal is considered to be Hypovolemia and occurs in the event of profuse sweating or acute blood loss. A healthy adult can easily tolerate a 10-15% loss of blood volume. If there is an acute blood loss of more than 30%, hypovolemic shock occurs.
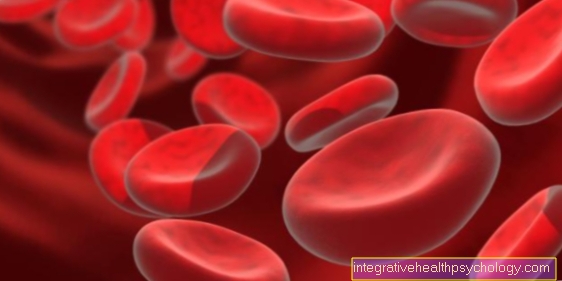
Blood cells
About 55% of the blood volume consists of blood plasma, 45% of blood cells. The blood cells swim in the yellowish blood plasma. The percentage of blood cells in the blood is called the hematocrit level. The normal hematocrit value in men is around 45%, in women around 41% and in children around 37%. If the hematocrit value of the blood increases, the blood becomes more viscous and the viscosity (internal friction) increases. This increases the resistance to blood flow.
A distinction is made between blood cells:
- Red blood cells (erythrocytes)
- White blood cells (leukocytes)
- Blood platelets (thrombocytes)
Read more about blood tasks here
Blood types
AB0 - blood group system based on glycolipid antigens (A and B). People whose red blood cells only have antigen A or B have blood group A or B. People who have both antigen A and B have blood group AB. If one does not have an antigen, one speaks of blood group 0.
European blood groups:
- 45% blood group 0
- 40% blood group A
- 11% blood group B
- 4% blood group AB
Compatible blood transfusions
Blood group A and B are only compatible for blood of the same blood group and blood group 0. Blood group AB is compatible with all blood groups. Blood group 0 is only compatible with blood group 0. If the wrong blood group is transfused, the blood clots and leads to anaphylactic shock.
Rhesus blood group system
The name is based on the discovery of the antigen in the blood of the rhesus monkey. People whose red blood cells have the D antigen are referred to as RH +. If the D antigen is missing, it is called RH-.
Blood plasma
As already mentioned, the blood plasma makes up about 55% of the total blood volume. The blood plasma is blood without cells. The blood plasma consists of approx. 90% water and 10% solid components such as protein, electrolytes and representatives of carbohydrates.
Plasma proteins
One liter of blood contains around 60-80g of protein. Due to its size, it cannot penetrate the plasma wall and has a water-attracting force (colloid osmotic pressure). The water from the interstitial space is thus drawn back into the capillary. The level of the colloid osmotic pressure (normal value approx. 25mmHg) does not determine the size of the protein molecules, but their number. The small molecular albumins are 75% involved in the colloid osmotic pressure. A decrease in albumin consequently increases the extravascular and decreases the intravascular fluid volume and thus leads to edema. In addition, albumins take on a transport function for ions and exogenous substances such as antibiotics. Globulins are larger molecules that have a transport function. In addition, the globulins contain immunoglobulins, which act as a defense against bacterial foreign substances. Their proportion is around 32g per liter of blood plasma.
Fibrinogen is important for blood clotting and is represented with approx. 3g per liter of blood. In addition to the water-binding function, defense function and transport function, the protein contained in the blood is important as an amino acid reservoir. The amount of electrolytes in the blood is approx. 9g / liter and is mainly determined by Na + and Cl-.
Other components of the blood plasma:
In addition to proteins, the blood contains glucose, free fatty acids, cholesterol, enzymes and hormones, but only in very small amounts.
Defense function of the blood
If foreign substances such as bacteria get into the bloodstream, either a non-specific defense function by phagocytes or the specific defense action of the so-called immune reaction occurs. The immune system of the human organism has more than 1 billion lymphocytes for this specific defense function. The lymphocytes are formed in the lymph nodes, spleen and bone marrow and transported into the bloodstream. The human body's antibodies are around 100 million trillion.
The lymphocytes are divided into T-form for the specific cellular defense and B-form for specific humoral defense. The B lymphocytes are responsible for producing large amounts of antibodies. They are shaped in the lymph nodes and tonsils for their specific task and released into the blood and lymphatic system. Upon contact with the antigen, the B lymphocytes multiply and transform into plasma cells and produce antibodies. The T lymphocytes take over the function if not all pathogens have been killed by the unspecific defense or specific humoral defense. The T lymphocytes are shaped in the thymus for their respective task. The T lymphocytes dock with their specific receptors on the antigen. The T lymphocytes are responsible for killing bsp. Cancer cells but also transplanted tissue.
Another form of lymphocytes are the null cells, which make up around 10% of all lymphocytes and take on unspecific "killer functions".
Active immunization
Active immunization is used to prevent life-threatening infections. In this process, the body is administered weakened, but still living, pathogens that trigger the formation of antibodies. E.g. vaccination against swine flu, measles, diphtheria.
Passive immunization
In passive immunization, antibodies are administered that have been formed in the organism against the specific antigen. The result is an immediate effect compared to active immunization.
Hemostasis
If body tissue is opened in the event of an injury, the body's own hemostasis occurs. On the one hand, the vascular wall is narrowed in front of and behind the exit point in order to lower the blood pressure locally. On the other hand, platelets accumulate on the connective tissue fibers of the wound edges to stop the bleeding. A wound drop, the so-called thrombus, forms at the point where the blood exits. However, this cannot close the wound permanently due to the rise in blood pressure. In the liver, the prothrombin has to be converted to thrombin by the influence of vitamin K, which converts fribrinogen into fibrin and ultimately closes the wound.
In addition to these endogenous hemostasis mechanisms, there are so-called emergency medical measures for hemostasis. By elevating the affected area, blood pressure can be lowered locally. Normally, a compression bandage is sufficient to temporarily stop the blood leak. A so-called fibrin glue is used in surgery. This type of tissue adhesive avoids surgical sutures.
Read more about the topics Quick value and general tasks from the blood
Gas transport of the blood
The oxygen transport function (transport) of the blood and the removal of carbon dioxide and lactic acid make it possible to exercise over a longer period of time. The oxygen diffuses through the thin wall of the alveoli into the pulmonary capillaries. From there it gets into the flowing blood to the respective successor organ. The carbon dioxide diffuses from the muscles with the bloodstream to the lungs and finally to the pulmonary alveolus.