Pancreatic hormones
introduction
The pancreas hormones include the following:
- insulin
- Glucagon
- Somatostatin (SIH)

education
Education:
The hormones of the pancreas are produced in the so-called Langerhans cells, of which three different types are known:
- alpha-,
- beta and
- delta cells.
The hormone glucagon is produced in the alpha cells, insulin in the beta cells and somatostatin (SIH) in the delta cells, whereby these three different hormones mutually influence their production and release. The beta cells make up about 80%, the alpha cells 15% and the delta cells the rest.
The hormone insulin as a pancreatic hormone is a protein (peptide) from a total of 51 amino acids, which are divided into an A and a B chain. Insulin is created from a precursor protein, the pro-insulin, after splitting off a protein residue (C chain). The receptor of this hormone is composed of four subunits (Heterotetramer) and is located on the cell surface.
In addition, an important digestive enzyme is initially formed in the pancreas as an inactive precursor. It is trypsinogen, which is converted into the active form trypsin in the intestine and plays a crucial role in the digestion of proteins.
Find out more at: Trypsin
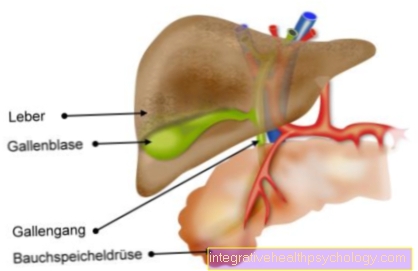
Illustration of the pancreas

- Body of
Pancreas -
Corpus pancreatis - Tail of the
Pancreas -
Cauda pancreatisauda - Pancreatic duct
( execution course) -
Pancreatic duct - Duodenum lower part -
Duodenum, pars inferior - Head of the pancreas -
Caput pancreatis - Additional
Pancreatic duct -
Pancreatic duct
accessorius - bile duct -
Common bile duct - Gallbladder - Vesica biliaris
- Right kidney - Ren dexter
- Liver - Hepar
- Stomach - Guest
- Diaphragm - Diaphragm
- Spleen - Sink
- Jejunum - Jejunum
- Small intestine -
Intestine tenue - Colon, ascending part -
Ascending colon - Pericardium - Pericardium
You can find an overview of all Dr-Gumpert images at: medical illustrations
regulation
The hormones of the pancreas are mainly regulated with the help of blood sugar and dietary protein. The fatty acid level plays a lesser role in the release of hormones.
A high blood sugar level promotes the release of insulin, while a lower one promotes the release of glucagon.
Both hormones are also stimulated by breakdown products of food protein (amino acids) and the vegetative nervous system. The sympathetic nervous system promotes the release of glucagon via noradrenaline, while the parasympathetic nervous system promotes the release of insulin via acetylcholine. Free fatty acids from body fat inhibit glucagon secretion, but promote the release of insulin.
In addition, the release of insulin is influenced by other hormones of the gastrointestinal tract (e.g. secretin, GLP, GIP), as these hormones make the beta cells more sensitive to glucose and thus increase the release of insulin.
Inhibiting hormones also exist, for example amylin or pancreatostatin. To regulate the glucagon level, there are also other substances that promote release (gastrointestinal tract hormones) or inhibit (GABA).
The hormone somatostatin is released when there is an increased supply of sugar, protein and fatty acids and inhibits the release of both insulin and glucagon. Furthermore, other hormones force the release of this hormone (VIP, secretin, cholecytokinin, etc.).
function
The hormones in the pancreas mainly affect the metabolism of carbohydrates (sugar). Furthermore, they participate in the regulation of protein and fat metabolism as well as in other physical processes.
Also read: Functions of the pancreas
Effect of insulin
The hormone insulin lowers blood sugar by absorbing glucose from the blood into cells (especially muscle and fat cells), where the sugar is broken down (Glycolysis).
The hormone also promotes sugar storage in the liver (Glycogenesis). In addition, insulin has an anabolic effect, which means generally “building up” the body's metabolism and stimulates the storage of energy substrates. For example, it promotes the formation of fats (Lipogenesis), thus has a lipogenic effect and increases the storage of protein, especially in the muscles.
Furthermore, insulin serves to support growth (growth in length, cell division) and has an influence on the potassium balance (potassium uptake into the cell by insulin). The final effect is the increase in heart strength through the hormone.
Read more about insulin and giving up insulin.
Glucagon

General
Put simply, glucagon is the “antagonist” of insulin in that it raises blood sugar levels. It can be used therapeutically in cases of severe, life-threatening low blood sugar (hypoglycaemia). Often, glucagon is popularly referred to as the "hunger hormone".
Education and Distribution
The peptide hormone is produced by the A cells of the islets of Langerhans in the pancreas and consists of 29 amino acids.
When the blood sugar level drops, but also when the amino acid concentration rises and the free fatty acids decrease, glucagon is released into the bloodstream. Some digestive system hormones also promote secretion. Somatostatin, on the other hand, inhibits secretion.
Effects
Glucagon initially aims to mobilize our body's energy reserves. It promotes fat breakdown (lipolysis), protein breakdown, glycogen breakdown (glycogenolysis), especially in the liver, as well as the production of sugar from amino acids. As a whole, this can raise blood sugar levels. Furthermore, more ketone bodies are produced, which can be used as an alternative source of energy by e.g. our nervous system in the event of hypoglycaemia.
Glucagon deficiency
If the pancreas is damaged, a glucagon deficiency can occur. However, the simultaneous insulin deficiency is more in the foreground. Because isolated glucagon deficiency does not normally result in any profound disturbances, as the body can easily compensate for this condition by, for example, reduced insulin release.
Glucan excess
In very rare cases, an A-cell tumor of the islets of Langerhans cells can be responsible for an excessive glucagon level in the blood.
insulin

General
Insulin is the central metabolic hormone in our body. It regulates the absorption of sugar (glucose) in the body cells and also plays an important role in diabetes mellitus, also popularly known as "diabetes".
Education and Synthesis
In the B cells of the islets of Langerhans in the pancreas, the 51 amino acid long peptide hormone insulin, consisting of an A and B chain, is formed.
During the synthesis, insulin goes through inactive precursors (preproinsulin, proinsulin). For example, the C-peptide is split off from proinsulin, which is of considerable importance nowadays in the diagnosis of diabetes.
distribution
Rising blood sugar levels are the main trigger for the release of insulin. Certain hormones from the gastrointestinal tract, such as gastrin, also have a stimulating effect on insulin release.
Effects
First and foremost, insulin stimulates our cells (especially muscle and fat cells) to absorb high-energy glucose from the blood and thus causes a lowering of the blood sugar level. It also promotes the creation of energy reserves: glycogen, the storage form of glucose, is increasingly stored in the liver and muscles (glycogen synthesis). In addition, potassium and amino acids are absorbed more quickly in muscle and fat cells.
Diabetes mellitus and insulin
Insulin and diabetes mellitus are closely linked in many ways! In both type 1 and type 2 diabetes, a deficiency in the important hormone is in the foreground. While type 1 is characterized by the destruction of the insulin-producing islets of Langerhans, type 2 is characterized by a reduced sensitivity of the body cells to insulin.
In recent years, the incidence of type 2 diabetes has increased significantly. It is estimated that every 13th person in Germany now suffers from the disease. Obesity, a high-fat diet and lack of exercise play a major role in the development.
Nowadays, human insulin can be produced artificially and used to treat diabetes mellitus. In this way, the essential lowering of the blood sugar level and the energy supply of the cells can be guaranteed. To do this, patients inject the hormone with a small needle ("insulin pen", "insulin pen") under the skin.
Somatostatin

General
Somatostatin is the "inhibitor" of our hormonal system. In addition to inhibiting the release of numerous hormones (e.g. insulin), experts suspect a role as a messenger substance in the brain. In particular, the hormone suffers from its effect as an antagonist of the growth hormone somatotropin.
Education and Synthesis
Somatostatin is made by many cells in our body. The D cells of the pancreas, specialized cells of the stomach and small intestine, and cells of the hypothalamus produce somatostatin. At 14 amino acids, it is a very small peptide.
distribution
Similar to the release of insulin, high blood sugar levels in the blood play a major role. But also a high concentration of protons (H +) in the stomach, as well as increasing concentrations of the digestive hormone gastrin, promote the release.
Effects
Ultimately, somatostatin can be understood as a kind of “universal brake” on the hormonal system. It inhibits digestive hormones, thyroid hormones, glucocorticoids and growth hormones. These include e.g.
- insulin
- Glucagon
- TSH
- Cortisol
- Somatotropin
- Gastrin.
In addition, among other things, somatostatin reduces the production of gastric juice and enzymes in the pancreas. It also inhibits gastric emptying and thus lowers digestive activity.
Somatostatin in therapy
Artificially produced somatostatin, called octreotide, can be used in modern medicine to treat some clinical pictures. In acromegaly, i.e. the huge growth of the nose, ears, chin, hands and feet, octreotide can be successful.