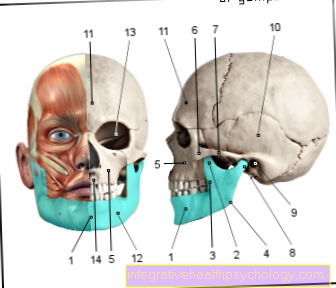
Temporomandibular joint osteomyelitis
introduction
Under one Osteomyelitis one understands an inflammation of the Bone marrowcaused by an infection.
This inflammation can be either acute or chronic occur. Not infrequently, such an infection affects the Jawbone.
Of the Lower jaw is affected up to six times more often than the upper jawwhich is mainly due to the fact that the Vascular supply in this bone is worse.
causes
Causes of a Osteomyelitis in this location can:
- Dental disease
and - Dental infections
- dead teeth
- Tooth removals (tooth extractions)
- Abscesses
or - Cysts in the mouth
- open jaw fractures / broken jaw
- purulent sinus infections
or - by Irradiation
damage caused to this area.
The pathogens that can be responsible for such an inflammation include:
- Staphylococcus aureus
- Prevotella melaninogenica
- Enterococci
- Pseudomonas
and - Klebsiella
Symptoms
The Symptoms one Osteomyelitis of the jaw differ depending on whether it is a acute or chronic osteomyelitis acts.
A acute osteomyelitis Fortunately, there are only relatively rare nowadays, because this represents a serious clinical picture.
Patients suffer from a greatly reduced general condition (severe illness):
- the body temperature is increased
- strong pain
- Swelling (thick cheek)
and - the flow of pus
are typical.
Sometimes it comes to Loosening and the Individual teeth fall out and spontaneous Fractures of the jawbone, since bone tissue perishes (these areas are called bone necrosis, dead bone areas are also called Sequester).
The local complaints with a chronic osteomyelitis are similar but do not appear as suddenly and are generally somewhat less pronounced.
Systemic symptoms such as fever are usually absent.
In addition, this clinical picture can also lead to:
- Bad breath
- Malfunctions
and - Lymph node swelling (e.g. on the lower jaw)
come. Sometimes it also happens that the teeth no longer match so well (Occlusion disorders).
In severe cases, this chronic form can persist for months or even years.
Pain

A Inflammation of the bone marrow in the jaw (osteomyelitis) can show various symptoms.
Often the osteomyelitis arises as a result of one Abscess, for example after the Wisdom teeth removal. It is characteristic that after opening the abscess the pain disappear first, then however come back.
Osteomyelitis in the jaw is possible mostly with pain hand in hand. But this pain must not continuously available It is even more common that the patient has an infection that is painful, followed by one pain-free period in which the infection slowly spreads and then osteomyelitis in the jaw occurs, which then again with stronger pain connected is. However, it is important to know that pain in osteomyelitis can occur in the jaw, but it does exist no clear indication and must not necessarily present be.
Many patients have hardly any pain despite progressive osteomyelitis in the jaw, it is therefore important to look for other symptoms such as Swelling or displacement of the jaw to pay attention. It is just as important, however, that Not ignoring pain and waiting until it disappears since pain-free periods are not atypical despite progressive osteomyelitis in the jaw.
Diagnosis
First off are a survey of the Medical history (anamnesis) and an examination of the affected area by a doctor (preferably a ENT doctor or one dentist) necessary.
When diagnosing osteomyelitis in the acute stage, an increased Sedimentation rate (ESR) and a large number of white blood cells in the blood count (Leukocytosis) a major role.
For both forms of Osteomyelitis applies that they are im X-ray image can be recognized, but sometimes quite late.
As a rule, they are better Computed tomography (CT), Magnetic resonance imaging (MRI) or even that Bone scintigraphy.
However, all of these procedures are also more expensive and complex, which is why they are only used if the suspicion could not be confirmed beforehand. You can only secure the diagnosis with one Tissue removal (biopsy) the affected region.
An important differential diagnosis for osteomyelitis im Jawbone is a Bone tumor.
therapy
The therapy depends on the severity of the disease. Sometimes, in the initial stages, conservative therapy with an appropriate one is sufficient antibioticwhich should usually be done over about three weeks.
They are also a medicinal option Bisphosphonates that will help breakdown Bone substance to prevent.
If the conservative treatment does not promise any improvement or has already been tried unsuccessfully, a surgical intervention can also be carried out. Here sequesters and dead pieces of the Bone away. Sometimes some teeth need to be removed as well. In addition, the outermost layer of bone be removed (decortication) to ensure better blood flow to the bone. Here, too, it is extremely important to consistently continue antibiotic therapy.
The last option is always the (partial) resection of Jawbonewhich can be replaced with plates or grafts if necessary.
surgery
Osteomyelitis in the jaw should be avoided first always conservative be treated if the condition still allows this. Since it is an inflammation, it should first an antibiotic given to stop the inflammation and thus prevent the progression of osteomyelitis.
In addition, a hyperbaric oxygen therapy to be carried out around bacteriathat survive only in conditions without oxygen (Anaerobes) kill.
However, osteomyelitis in the jaw is common so advancedthat just an operation can still help. This surgery must be of advanced osteomyelitis dead jawbones removed as well as the outermost layer of boneso that the remaining jawbone still intact is one improved blood circulation (Vascularization) receives.
In particularly bad cases however, it can be a complete part of the jaw removed must be because the bone area has already died. This is known as Partial resection of the jaw. Even if this is one drastic intervention this is still possible because otherwise the inflammation keep moving forward can and not just the jawbone but also other bones of the Skull can attack. This is absolutely to be avoided. So that the jaw is "filled" with bone again, either Bone grafts or plates used to stabilize the jaw.
course
Usually takes the Osteomyelitis in the jaw one good courseas good treatment options are available.
The most serious complication acute osteomyelitis is the Chronification this state. Some develop osteomyelitis as part of it Tooth loss, impaired chewing function or the spread of the infection to other parts of the body.
prophylaxis
To one Osteomyelitis of the jaw To prevent this, adequate hygiene of the oral cavity and teeth is the most important measure (this also includes regular Checkups at the dentist!).
You should also try to cope with the use of Antibiotics not to be too generous, as bacteria then have an easier time trying an infection and are already resistant to the corresponding antibiotics.
If the pain and swelling in the jaw area are unclear, a doctor should be consulted immediately.