Pleural effusion
introduction

Lies a Pleural effusion before, has Fluid between the lungs and the chest wall accumulated. A pleural effusion can lead to Shortness of breath, a slightly elevated body temperature to fever to lead. The examination results often reveal a decreased breathing sound.
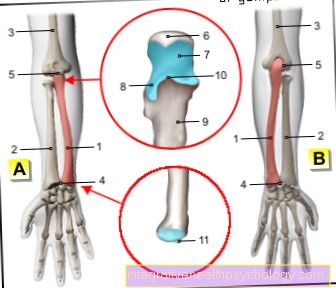
Under the Pleura one understands the pleura, which extends over the lungs. The pleura consists of two sheets, an inner and an outer leaf. The inner sheet (Visceral pleura) is on the surface of both lungs, while the outer sheet (Parietal pleura) the inner walls of the Rib cage, the top of the Diaphragm and the Pericardium lines and thus separates the lungs from the adjacent structures.
There is a with between the two leaves Liquid-filled cavity, of the Pleural space, in which a negative pressure is created, so that a collapse / collapse of the lungs is prevented. Usually located in the pleural space five to ten milliliters of liquid. Collects more fluid there, it is a pleural effusion. The pleura absorbs around ten milliliters of fluid a day and also produces around ten milliliters of new fluid. Is this Balance disturbed, a pleural effusion occurs.
causes
For the Development of a pleural effusion various causes come into question. The most common are malignant tumors (in particular Lung tumors), bacterial pneumonia or tuberculosis.
Pleural effusion can also occur in diseases that not primarily the lungs concern, as with malignant diseases of other organs or at heart-, Kidneys- and Liver disease, just like rheumatic diseases.
Malignant tumors make the total most of the triggers they are responsible for about half of all pleural effusions, so that the pleural effusion always indicates a malignant (malicious) Basic illness must be clarified.
The second most common cause is the bacterial one lung infection with a share of about 30%.
Everyone tenth Pleural effusion comes through a Heart failure conditions.
If the pleural effusion occurs as a result of pneumonia, the Inflammation can also spread to the effusionso that the fluid at the puncture is usually purulent. The typical symptoms like Shortness of breath and fever then occur in this case significantly reinforced on. If a purulent pleural effusion develops in the course of the inflammation, one speaks of a Pleural empyema.
Type of effusion
With a pleural effusion one differentiates between a so-called transudative and exudative pleural effusion. The distinguishing feature between the two types is the protein content of the liquid.
Is the effusion a transudative pleural effusion, this contains only a little protein - one speaks of a transudate: the protein content is this less than 30 g / l. The quotient of the protein concentration in the effusion and the protein concentration in the blood serum is less than 0.5.
However, the existence of a transudate does not allow any direct conclusions.
A transudate occurs when the balance between the formation and absorption of the pleural fluid by the pleura is disturbed. However, the cause does not lie in the pleura itself. Most often, a transudative effusion occurs in the context of right heart failure, pulmonary embolism or liver cirrhosis. Cirrhosis of the liver causes damage to the liver, which can lead to a decreased production of the protein albumin come, whereby the protein content of the effusion is reduced.
One speaks of an exudate when the liquid has a high protein content. Due to the high protein content, the exudate is correspondingly heavier than the transudate. The protein content is over 30 g / l. The quotient of the protein concentration of the effusion and the blood serum is greater than 0.5.
Exudates occur in the context of inflammation or tumor diseases. The inflammation or the tumor increases the permeability of the pleura or pleura or hinders the flow of lymph from the pleural space, so that more fluid can collect there.
In addition to these effusions, special forms of the pleural effusion sometimes occur. This can lead to an accumulation of blood within the pleural space (a so-called Hemothorax, read more about this) or to an accumulation of lymph (Chylothorax).
A rheumatic disease or tuberculosis can lead to the development of a Pseudochylothorax come. In doing so, the liquid looks like the effusion milky-cloudy like lymph, however, is not actually of lymphatic origin. As a further complication, bacterial inflammation can lead to an accumulation of pus within the pleural space, a so-called Pleural empyema.
Pleural empyema is also a form of pleural effusion and describes a collection of pus in the lungs. It is therefore advisable to deal with this topic as well: Pleural Empyema - What's Behind It?
Left and right pleural effusion
A pleural effusion occurs both unilaterally and bilaterally.
If it is a one-sided effusion, it is usually the right side of the lung affected. The reason for this is the anatomical structure of the lungs.
The right lung has three lobes, while the left has only two parts due to the displacement by the heart.
As a result, the area of the covering pleural leaves is larger on the right side. A wider area is capable of increased fluid production. This results in the increased occurrence of right-sided pleural effusions.
Symptoms
The most common symptom that occurs in the course of a pleural effusion is shortness of breath (Dyspnea), which occurs mainly during physical exertion. In addition, there is often a high temperature up to fever. Sometimes those affected also report a feeling of tightness in the chest. The severity of symptoms increases with the amount of fluid that has accumulated and also depends on the cause of the effusion.
In most cases, those affected are not severely limited in their general condition by the symptoms. Smaller effusions with a fluid accumulation of up to 500 milliliters are usually not symptomatic. If the pleural effusion occurs within a short period of time, it is usually caused by a (stronger) Accompanying shortness of breath. However, if the effusion occurs slowly, there will only be a shortage of breath after some time, when a lot of fluid has already accumulated in the pleural space.
You might also be interested in: These are the symptoms that will help you identify water in your lungs
Diagnosis

If a pleural effusion is suspected from a medical point of view, the attending physician begins tapping and listening to the airways. A muffled tapping sound (especially at the lower lungs) and reduced breathing noises speak in favor of fluid accumulation.
If this confirms the suspicion, an ultrasound examination follows, in which the pleural space is found and, in the case of a pleural effusion, increased fluid accumulation becomes visible. When the patient is standing, the fluid collects between the underside of the lungs and the diaphragm. This manifests itself in the ultrasound as a so-called anechoic substance - you can see a black accumulation.
If the ultrasound examination is not sufficient to establish the diagnosis, an X-ray of the thorax (detectable from amounts of 250-300 ml) or computed tomography can be used.
Since the cause of the pleural effusion always has to be clarified, the next thing is a puncture of the pleural effusion so that a sample of the fluid can be obtained, which can then be examined in the laboratory, so that one can infer the cause of the pleural effusion and thereby treat the underlying disease can. The puncture is performed under ultrasound control so that the doctor performing the procedure does not inadvertently penetrate the lungs during the puncture. For the puncture, a fine needle is inserted into the area of the lower ribs and fluid is removed via the puncture needle.
The color and consistency of the liquid alone can allow initial conclusions to be drawn about the cause. For example, a bloody liquid suggests a malignant cause. The protein content, weight and cell content are then determined in the laboratory. When it comes to cells, particular attention is paid to inflammatory and tumor cells. During the puncture, the doctor should pay particular attention to sterile work, as otherwise environmental germs can get into the chest and lead, for example, to pleural empyema.
If the puncture does not provide any information about the cause of the pleural effusion, a so-called Thoracoscopy be performed. Thoracoscopy is a surgical examination in which a camera system is inserted into the chest through a skin incision. A gas (usually carbon dioxide) is used to expand the layers of the pleura so that they can be easily seen.
therapy
The therapy is aimed primarily at the underlying disease that triggers it, such as tumor disease. In addition, physical therapy can be used as part of Breathing exercises, Thermal radiation or chest wraps can be used to increase the patient's wellbeing.
A pleural puncture can also be used for therapy, which is already used in the context of diagnostics. This is mainly done if the underlying disease of the pleural effusion cannot be treated and if the accumulation of fluid leads to severe shortness of breath, which in extreme cases occurs even at rest. As a rule, with this relieving puncture, amounts of liquid between 500 ml and one liter are removed.
If the pleural effusion does not regress or if a bacterial infection leads to an accumulation of pus within the pleural space, permanent drainage can be created. A rubber tube is inserted into the area of the effusion via a needle as a guide rail, which then lingers there for a few days. If necessary, the excess liquid can be continuously sucked off via this system via a valve.
If there is an infection, the pleura can be rinsed and treated with antibiotics via this system.
Also with a non-treatable cause, such as the malignant pleural mesothelioma, the so-called Pleurodesis are used. For this, the inner and outer sheets of the pleura are glued together with the help of medication, so that no more fluid can collect between them. As medication come for it Tetracycline or Bleomycin in question, as well as the mineral talc.
If a pleural effusion occurs as a result of a long-term bacterial infection, severe suppuration or adhesions within the pleural space may occur. In this case, the adhesions or the so-called pleural rinds that form can be surgically removed. This process is known as Decortication. The decortication allows the lungs to fully develop again.
Read about this too Pleural puncture
The pleural effusion in pneumonia
If fluid collects in the space between the pleural leaves, the pleura and the lungs, it is called a Pleural effusion. This can have numerous causes. About a third of the time it is one lung infection or pneumonia. The triggers are usually bacteria or viruses.
In pneumonia, an inflammatory reaction takes place that can spread to the pleura. At the beginning one speaks of a pleurisy, i.e. an inflammatory involvement of the pleura.
As a result, a liquid, protein-rich effusion develops from inflammatory cells. Complaints in the form of pain occur primarily in relation to breathing.
As the volume of the pleural effusion increases, the difficulty breathing increases. The pain decreases at the same time. Other typical symptoms of pneumonia are a sudden cough with purulent sputum, an increased breathing and pulse rate and a significant increase in temperature. A Ultrasound examination provides an indication of a Peura effusion from 50ml.
The CT is able to detect even the smallest volumes.
Antibiotic therapy for pneumonia plays an important role in therapy. In this way, the cause of the effusion is treated. The pleural puncture can also be used to relieve pressure in an acute situation. A so-called thorax suction drainage, on the other hand, promotes small amounts of effusion over several days. It is used when the space between the pleural leaves is infected or an effusion persists.