Intervertebral disc
Synonyms
Medical: Intervertebral disc
English: discogenic
Intervertebral disc, intervertebral discs

anatomy
The Band washers (lat. Disci intervertebrales) form the flexible Connection between all vertebraewith which they are firmly fused. An exception is the articulated connection between the skull and the first cervical vertebra (Atlas), as well as the first and second cervical vertebrae (Axis). Overall, it is found in humans 23 intervertebral discswhich make up about a quarter of the total length of the spine.
Each intervertebral disc can be inserted into two components organize. An internal gelatinous core, the Nucleus pulposus (usually simply called "nucleus") and an outer ring of fibers surrounding it (Annulus fibrosus). The latter consists of fibrous cartilage tissue with a high content of collagen, giving it a firm, pressure-resistant and coarse consistency. On closer inspection it can be seen that it is arranged from circularly arranged lamellae. The outermost rays radiate into the cover plates of the bony vertebral bodies, while the inner lamellae in turn partially radiate into the gelatinous core of the intervertebral disc, so that the transition between the ferrule and nucleus is rather blurred.
The Gelatinous core Like the fibrous cartilage surrounding it, it contains only a few cells. Instead of collagen, however, it consists mainly of long-chain sugars, the so-called glycosaminoglycans. These are characterized by a high water-binding capacity, so that the gelatinous core from up to 85% water consists. This creates a swelling pressure inside the intervertebral disc, which puts the outer fiber ring under tension. Only the interaction of the two components gives the intervertebral discs their characteristic properties, which make them indispensable for the proper functioning of our spine.
In everyday life, this construction is subjected to constant stress tests in the form of movements and shocks, which, however, can be effectively cushioned and passed on to the vertebral bones thanks to the construction described above. Apart from this, the intervertebral discs must of course also be uninterrupted Carry body weight. This load naturally increases in the direction of the tailbone when standing and sitting. For this reason, both the vertebral bodies and the intervertebral discs between them steadily increase in diameter from the neck downwards. Nonetheless, they can be found at a distance most herniated discs and other spinal disorders in the field of Lumbar spine.
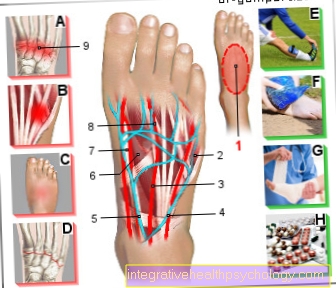
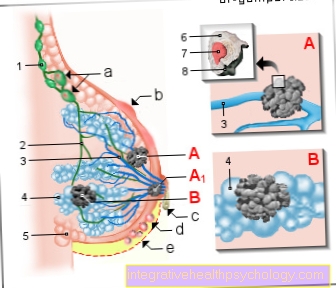
Illustration of an intervertebral disc

- Intervertebral disc
(Intervertebral disc) -
Discus inter vertebralis - Gelatinous core -
Nucleus pulposus - Fiber ring -
Annulus fibrosus - Spinal nerve -
Spinal nerve - Spinal cord - Medula spinalis
- Spinous process -
Spinous process - Transverse process -
Transverse process - Upper articular process -
Superior articular process - Intervertebral hole -
Intervertebral foramen - Vertebral bodies -
Corpus vertebrae - Front longitudinal ligament -
Longitudinal anterior ligament
You can find an overview of all Dr-Gumpert images at: medical illustrations
Function of the intervertebral discs
The intervertebral disc acts like a shock absorber due to the elastic gelatinous core. It cushions shocks elastically.
Furthermore, due to its elastic properties, it can deform when moving. This is the basic requirement for the mobility of the spine.
Diseases of the intervertebral disc
In the course of life wears out the intervertebral disc. The fiber ring will crack.
Due to the swelling pressure of the gelatinous core, it can escape. The consequence is one disc prolapse. A herniated disc does not necessarily have to lead to discomfort. Only when the herniated disc can affect the spinal cord or nerves chronic back pain, Sensory disturbances or paralysis arise.
You can find detailed information on this topic at:
- disc prolapse
- chronic back pain
- Lumbar spine syndrome
- Cervical spine syndrome
A preliminary stage of the herniated disc is Disc protrusion (Protusio = Protrusion).
The fiber ring gives way due to its wear and tear and bulges at the weakest point due to the swelling pressure of the gelatinous core. However, the fibrous ring is still intact, the gelatinous nucleus has not yet emerged.
Almost all people have one in old age Disc protrusion on. Therefore, bulging should be viewed as a normal wear process. A protrusion can also indicate an impending herniated disc.
Further information on this topic can be found at: Disc protrusion
In addition to the removal of the intervertebral disc, a Intervertebral disc prosthesis implanted. It remains to be seen how important the intervertebral disc prosthesis will be in the future.
Inflammation of the intervertebral disc
Inflammation of the intervertebral discs is a very seldom encountered disease. In technical terminology, it is called "Discitis" designated. In addition, inflammation of the vertebral body often occurs at the same time. In this case, there is talk of spondylodiscitis. The causes of spondylodiscitis are diverse. In most cases, however, it is caused by a bacterial infection, more rarely a virus or fungus.
The pathogens usually get into the area of the intervertebral discs as part of a surgical procedure or an injection. However, in most cases it is difficult to detect the pathogen, so the diagnosis is preferably made using imaging methods such as magnetic resonance imaging (MRI) in combination with increased levels of inflammation in the blood.
The severity and course of an inflammation of the intervertebral disc usually vary greatly from person to person. Completely symptom-free courses as well as severe pain and general symptoms such as fever, fatigue and chills are possible. Most feared are neurological symptoms and neuropathic pain as a result of the infection spreading to the spinal nerves or the spinal cord.
Imagines purulent abscess in the spinal canal this can lead to in the worst case Symptoms of paraplegia to lead.
The Treatment of spondylodiscitis and in the case of a bacterial infection, pure discitis also consists primarily of an infection that is adapted to the pathogen Antibiotic therapy. In addition, an adequate drug therapy with anti-inflammatory drugs is given according to the pain Painkillers began.
It is also important to keep the affected spinal area for several weeks immobilize. A corset or an orthosis can be used for this.
Infections in the lumbar spine area usually require bed rest, as immobilization is hardly possible here. If the disease cannot be brought under control by any other means, a surgical intervention carried out during which the abscess is cleared out.
The forecast a disc inflammation is total rather bad. The disease is only fatal in a few cases. Permanent neurological impairment, such as disorders of sensitivity and motor skills, are not uncommon. A relapse, i.e. the recurrence of inflammation, occurs in about 7% of patients.

Figure disc protrusion
View from above:
- Nucleus pulposus
Gelatinous core - Annulus fibrosus
Fiber ring - disc prolapse

Figure herniated disc
View from above:
- Nucleus pulposus
Gelatinous core - Annulus fibrosus
Fiber ring - disc prolapse
Symptoms of damage to the cervical disc
Most damage to intervertebral discs remains symptom-free for a long time or even never becomes noticeable. Only when the outer fiber ring is so worn that the gelatinous core of the intervertebral disc bulges and presses on neural structures will this be noticeable to the patient. The exact symptoms that occur here depend primarily on the height of the spine at which the herniated disc occurred and how severely the nerve root is affected by the protrusion of the disc. So do yourself Herniated discs of the cervical spine (Cervical spine) mainly through Discomfort in the arm and shoulder region noticeable. It is important to know that slight nerve damage only causes sensory disorders such as tingling and numbness, while higher-grade damage results in muscle weakness.
As for the cervical spine, herniated discs are most common between the 5th and 6th and the 6th and 7th cervical vertebrae.
The spinal nerves emerging at this level supply the thumb and the forearm on the thumb side, as well as the index, middle and ring fingers and parts of the palm and back of the hand.If sensory disturbances occur in these regions, this indicates a herniated disc in the said section of the spine. Muscle weaknesses in the case of a severe herniated disc can affect various muscles, such as the triceps brachii muscle.
Symptoms of damage to the lumbar disc
In the case of a herniated disc in the lumbar spine, the following also applies: most damage to intervertebral discs does not cause any symptoms and is therefore only diagnosed as an incidental finding or not at all. Correspondingly severe intervertebral disc damage, however, inevitably leads to the fact that the outer fibrous ring is no longer able to stabilize the gelatinous nucleus against the stress to which the spine is exposed. The nucleus jelly then bulges out and exerts pressure on the neighboring spinal nerves or even the spinal cord itself. If this is the case, specific symptoms occur depending on the height of the herniated disc in the spine or depending on which spinal nerve is damaged.
Is it possible to have a herniated disc in the absence of pain? You can read more about this under: Is there a herniated disc without pain?
The spinal nerves, which come off at the level of the lumbar spine, are mainly responsible for the motor and sensitive supply of the legs. Slight herniated discs at this level of the spine initially cause sensory disturbances such as tingling or numbness, especially on the front and side legs. Higher-grade herniated discs also lead to impairment of the motor nerve fibers located deeper in the nerve cord, so that now also a weakness of the leg muscles occurs.
By far the greatest number of herniated discs occur between the 4th and 5th lumbar vertebrae (herniated disc L4 / L5) and between the 5th lumbar and 1st coccyx vertebrae (herniated disc L5 / S1). In addition to the skin of the lateral leg, the spinal nerves branching out here supply the quadriceps femoris muscle, the large thigh muscle, among other things. A correspondingly severe herniated disc can lead to problems when walking and to a weakening of the patellar tendon reflex. In addition to other nerves, these same spinal nerves are also involved in the formation of the sciatic nerve (the sciatic nerve). A painful condition that is caused by irritation of the sciatic nerve is called sciatica.
Read more about this under: Symptoms of a herniated disc of the lumbar spine
Surgery for a herniated disc
Like other tissues in the body, the intervertebral discs are subject to a constant process of wear and tear. This long-term damage can lead to a displacement of the gelatinous nucleus of the intervertebral disc. Should the outer fiber ring the intervertebral disc tearcan do this in one disc prolapse result. If the fiber ring is still intact, so that the intervertebral disc bulges as a whole into the spinal canal, it is called protrusion, an incomplete herniated disc. Both are often symptom-free, but can also cause severe pain and nervous deficits.
According to recent studies, the number of disc operations doubled between 2005 and 2010. Still can ultimately 90% herniated discs conservative, especially by means of an effective one Pain therapy and physiotherapy, be treated. However, surgical intervention is absolutely necessary if serious symptoms, so-called "red flags" occur. It is worth knowing that muscle weakness or paralysis only occurs as a result of severe nerve damage while Sensory disturbances already for slight nerve damage occur.
For this reason, the "red flags"of the herniated disc especially increasing or sudden onset Muscle paralysis, as well as paralysis of the bladder and rectal muscles, which can lead to permanent stool and urinary incontinence.
Also the so-called Cauda Equina Syndrome represents a serious one warning sign This results in a compression of the nerve cords of the cauda equina, the extension of the spinal cord in the lowest part of the spinal canal. Damage to these nerve cords mainly results in sensory disturbances and muscle weakness in the legs.
Risks of intervertebral disc surgery
Even if serious complications and side effects in operations on the intervertebral disc are generally rare, it should be noted that the interventions always involve certain risks. Since these can potentially be serious due to the spatial proximity of the intervertebral disc and nerves or spinal cord, the necessity of a surgical intervention should be carefully considered in advance.
One of the most frequently The complications that occur and are unfortunately difficult to prevent Scarring in the operating area, which can lead to an entrapment of the nerve root or the outer skin of the spinal cord (Dura mater) and cause corresponding complaints. Furthermore, it can also be a direct one as part of the operation Injury to the dura mater come. As a result, fluid escapes through this spinal cord. Although this is completely reproduced within a few hours, severe headaches and / or nausea can occur after the operation.
This complication occurs roughly 1 to 2 % all disc operations.
Apart from that, in very rare cases a infection occur. Easy Pain directly after the operation, however, are to be expected and should therefore not be overrated. They can usually be treated well by taking common pain relievers.
Also worth mentioning is the Recurrence rate in intervertebral disc operations, i.e. how many patients are affected by herniated discs again despite the operation. Currently this is between about 5 - 10%. A relapse usually occurs within the first three months, but can only become noticeable after several years. If there is actually another herniated disc, a new operation is recommended.
Duration of the disc surgery
Disc surgery takes a long time dependent of the used Surgical technique. As with surgical interventions in other parts of the body, minimally invasive procedures take more time than open surgical methods. Apart from that, play too extent of the herniated disc and the anatomical conditions of the patient.
Overall, however, in most cases the duration of the operation should be 30 to 60 minutes can be expected. Immediately after the procedure, the patient remains under observation for a few hours until the anesthesia has completely worn off and acute complications have been ruled out.
Duration of illness after the intervertebral disc surgery
Typically, most patients already do two to three days after the operation it is possible to have your everyday activities to pursue. However, it should be noted that you should not run too long distances in the first few days. The duration for which the freshly operated person runs every day should be deliberately increased slowly. Up to one month after the operation, the patient should also neither drive nor sport float. Also should be up to three months after the surgery no weights over 15 kg become.
How long the actual sick leave will be after the operation is difficult to predict and depends heavily on the course of the disease after the operation. Depending on the type of occupation the patient may have to take sick leave for several months. Patients who have to work hard physically need significantly more recovery time than office workers.
Despite these prospects, the above precautionary measures should be taken seriously in any case. Compliance with these significantly reduces the likelihood of another herniated disc and thus the need for a new operation.
Surgical methods of a herniated disc
A surgical technique that is seldom used to this day is the insertion of a Intervertebral disc prosthesis after removing your own intervertebral disc.
The most common method is what is known as a microdiscectomy. The surgical team gains access to the intervertebral disc through an incision a few centimeters long above the spine. The emerged is under X-ray control Disc tissue subsequently evaporatesso that the compressed nerve root can be relieved and the cause of pain can be eliminated.
The procedure is mostly under general anesthetic, rarely also under Regional anesthesia performed and is therefore completely painless. In specialized centers, this surgical technique can also be performed on an outpatient basis.
In addition to this surgical procedure, there are also minimally invasive methods such as Percutaneous laser disc decompression (PLDD). These are enjoying increasing popularity as they are said to be less traumatic due to the small surgical field. In terms of their success rate, however, they are not superior to microdiscectomy.
Laser therapy
In addition to open surgery, there are also intervertebral disc surgery minimally invasive Surgical procedure. These also include the so-called "Percutaneous laser disc decompression"(PLDD). Their biggest advantage is that they under regional anesthesia is carried out so that the patient is spared general anesthesia in any case.
The indications for a PLDD basically correspond to those of other surgical procedures for the intervertebral disc. So the procedure is above all in the case of progressive or sudden severe nerve damage used, which manifest themselves mainly in a muscle weakness of the legs and a functional impairment of the urinary bladder and the rectum.
However, the laser procedure is not suitable for every patient and every stage of intervertebral disc disease. Conservative measures are usually sufficient for mild intervertebral disc symptoms, while for higher-grade diseases it is often difficult to achieve symptom improvement through PLDD.
At the beginning of the procedure, a puncture cannula and then a laser fiber are inserted through the skin into the gelatinous core of the intervertebral disc. Since this is not done with open surgery, the positioning must be checked radiologically, i.e. by means of CT or X-ray.
As a result of the energy of the laser beam, proteins are denatured in the tissue of the intervertebral disc and the liquid evaporates. This results in a shrinking of the intervertebral disc and ultimately a relief of the compressed nerve root. In retrospect, only a small punctiform scar will be visible on the surface. The procedure can rightly be described as very gentle and is therefore enjoying increasing popularity in neurosurgery.
Exercises for damage to the intervertebral disc
Various measures can be taken to prevent a herniated disc or a relapse after a herniated disc. Learning a good posture in everyday life and regular training of the core and back muscles play an important role here. For this training, on the one hand, special exercises can be carried out at home or back-friendly sports can be practiced. The latter traditionally include sports such as cycling, swimming and table tennis.
When targeted Building the back muscles Above all, emphasis should be placed on strengthening the small, deep-seated muscles. This group of muscles, known as “autochthonous”, runs from vertebra to vertebra along the entire spine and is of enormous importance when it comes to the stability of the spine. Since it responds primarily to fast movements, it can be trained, for example, by an asymmetrical movement of the arms. For this, a shoulder-width stand should be taken in a slightly crouching position. The arms are now quickly moved back and forth for about 30 seconds. This causes a slight rotational movement in the upper body, which activates the autochthonous muscles. The exercise should be repeated two to three times after a one-minute break and performed daily. However, it is important that the Back held straight becomes!
Despite all the motivation to train the back muscles, two things should be considered: the best evening exercises are of little value if you remain inactive during the day! Even the occasional stretching, stretching and walking around in the office or climbing stairs is helpful and sensible. Second, in addition to exercising your back, they shouldn't forget that too Abdominal muscle training important is. As an opponent of the back muscles, it is very important for the stability of the spine. If it is untrained compared to the back, the pelvis tilts forward and a hollow back is formed. Sit-ups with legs raised at a 90-degree angle or the alternating raising of arms and legs in a quadruped position are very back-friendly exercises.
Jogging with a damaged disc
Running training has been enjoying increasing popularity for some time and has now developed into a real national sport. For many athletes who have been jogging for years, sport has understandably become an important part of their everyday life. The consequences of an intervertebral disc damage can be all the more serious for runners. But first: in principle, jogging is still possible with damage to the intervertebral discs possible. It should be noted, however, that running training can be stressful for the joints and spine, despite all the advantages for the circulatory system. Especially when running on hard surfaces, the spine is exposed to vibrations with every step, which can lead to further damage to the intervertebral discs. If you do not want to give up running, you should therefore take a few measures to prevent a herniated disc.
First of all, routes should be chosen which lead over unpaved or tarred paths. Especially Forest tracks are particularly soft and therefore suitable for running. Next to it should Footwear be worn, which cushions the inevitable impacts on the intervertebral discs as well as possible.
Last but not least, it must also be said that if the intervertebral discs are damaged, running alone is not enough to adequately train the back muscles. In addition to running, you should definitely do exercises from Trunk and back muscles are in the training plan. Your family doctor or other doctor treating you should definitely be given more detailed information and advice on this subject. In case of doubt, it is he who knows your symptoms and the extent of your intervertebral disc disease best and can assess the risks.
Can the intervertebral disc be rebuilt?
The tissue of our intervertebral discs consists of a special form of cartilage tissue, the fiber cartilage. In addition to the intervertebral discs, there are also the mensiks and the articulated connection between the two pubic bones (Pubic symphysa) from this tissue. As with other forms of cartilage, most of the fibrous cartilage is made up of an organized network of collagen fibers that bind large amounts of water. Cells on the other hand are hardly to be found here, as is typical of cartilage. In fact, fiber cartilage contains even fewer cartilage cells than the other types of cartilage. These are able to maintain the functionality of the already existing fiber cartilage under moderate stress, can repair minor damage to the intervertebral discs and are also able to react to chronic stress to a certain extent.
However, they can cause severe damage to the structure of the intervertebral discs due to permanent incorrect loading not compensate. For a number of years, intensive research has been carried out on the possibility of the regeneration of cartilage and now there are various methods, especially for articular cartilage, which are intended to restore the damaged cartilage. However, to date none of these forms of treatment has been able to deliver satisfactory results. Unfortunately, this is also currently the case for the fiber cartilage of the intervertebral discs Conclusion that once destroyed cartilage tissue cannot be rebuilt.
Intervertebral disc presses on a nerve
The Sciatic nerve (Sciatic nerve) is the longest and thickest nerve in the human body.Similar to the nerves of the upper extremities, however, it does not only originate in one spinal cord segment. Instead, it arises from the nerve plexus of the "sacral plexus" and receives nerve fibers from segments L4 to S3.
From this it can be concluded that every herniated disc that presses on the nerve root of a spinal nerve arising at this level, sciatic pain (colloquially "sciatica", also called sciatica). Most often, the cause is a herniated disc at the level of the lower lumbar spine.
The symptoms caused by nerve root irritation of the sciatic nerve are usually very characteristic, so that the cause is usually easy to diagnose. Above all, that is typical Pain symptoms, which is called "sciatica" in technical terms. This is characterized by pain that is felt as tearing or pulling, which radiates from the buttocks into the back of the thigh through the lower leg and into the foot. This can be aggravated by sneezing, coughing or the abdominal press, as this increases the pressure in the abdominal cavity, which means that the intervertebral disc also presses on the nerve root. Furthermore, abnormal sensations such as tingling or numbness can occur in the same area. In the case of a pronounced herniated disc, muscle weakness and paralysis in the leg, as well as urinary incontinence, can also develop.
Diagnosis and treatment of herniated discs, which affect the sciatic nerves, are otherwise the same as for other herniated discs. Here, too, a significant reduction in symptoms can often be achieved solely by maintaining a healthy posture, exercising and losing weight.
Intervertebral disc presses on the spinal cord
If the nucleus pulposus bulges out as part of a herniated disc, it can press on various neural structures of the spinal canal. In many cases, this affects the nerve roots of the spinal nerves, which arise from the spinal cord and emerge from the spinal canal through the intervertebral holes. In other cases, however, the intervertebral disc can put pressure directly on the spinal cord.
The symptoms that occur here are basically similar to those of root irritation of the spinal nerves. In their intensity, however, they usually exceed this. So can the strongest pain in the arms and legs and Paresthesia such as numbness, temperature changes or numbness. On the other hand are too Signs of paralysis or spasms of the muscles are possible. The function of the sphincter muscles of the bladder and rectum can also be impaired, leading to fecal or urinary incontinence. Potency disorders can also be a result of impairment of the spinal cord.
Any herniated disc, which Incontinence or paralysis entails, provides one medical emergency which should be treated as soon as possible, as permanent nerve damage can be the result.
Link tip
We still have a link tip:
On starker-ruecken.com you will find hundreds of posts on the topic in the intervertebral disc blog Intervertebral disc.