Bronchiectasis
Bronchiectasis is a disease that is characterized by permanent widening of areas of the airways. Affected are the bronchi, which are located downstream of the windpipe, i.e. deeper in the lung tissue.
The extensions are sac-shaped or cylindrical and often filled with purulent fluid.

causes
The bronchi are Part of the respiratory system. Must go through them inhaled and exhaled air through with every breath. There are several causes that can cause enlargements to form in the bronchi, which are medically described as bronchiectasis.
In principle, will two different forms the bronchiectasis differentiated.
- The innate form can occur in connection with various diseases, whereby Cystic fibrosis, Kartagener Syndrome, alpha-1 antitrypsin deficiency and certain forms of pneumonia are to be listed as triggering causes. Congenital cause can also Malformations during the embryonic phase underlie. In this form of birth dilatation of the bronchi, which is a source of infection. Overall, the congenital form of bronchiectasis is one very rare disease.
- The second form of bronchiectasis is called acquired bronchiectasis designated. In earlier times this form of bronchiectasis mostly arose as Consequence of diseaseswhich usually occur in childhood, such as whooping cough or measles. Nowadays, thanks to relatively extensive standard vaccination, this cause is much rarer. However, acquired bronchiectasis can still occur today. This can be caused by several factors. Infections and inflammation of the airways, for example Influenza viruses can damage them and cause bronchiectasis. It should be mentioned here that infections that occur in childhood and adolescence in particular can damage the tissue to the extent that bronchiectasis can develop later. Also can foreign body or Tumors Cause widening of the airways.
In some rare cases, bronchiectasis can also occur idiopathic arise. That means that no obvious reason can be found which can explain the origin of the disease.
Diagnosis of bronchiectasis
Affected people often come to their family doctor typical symptoms of this respiratory disease. The specialists in diagnosing and treating this clinical picture are those Specialists in pulmonology, for which the family doctor usually issues a referral.
Bronchiectasis is usually diagnosed using a imaging procedure: the high resolution Computed Tomography (HR-CT of the lungs). The Medical history of the affected persons also give the treating physicians clues to assess the severity of the disease. Most important are Nature and duration of the complaints, and whether these are worse in certain situations than in others. Behaviors like Smoke and the use of medication and the information whether Similar diseases in the family are also important for the respective doctor.
A physical examination can rule out other respiratory diseases or confirm the diagnosis of bronchiectasis. For this, the attending physician can use the lung and the airways listen with a stethoscope and examine other symptoms (see below).
With the help of a lung function test, the functionality of the lungs and the airways can be examined, which can be greatly reduced in bronchiectasis, but also in other clinical pictures.
In the end that also plays MRI of the lungs an increasing role. In particular, the contrast agent helium (a gas that is non-toxic to humans) can better visualize the brochiectasis in the MRI.
Frequency distribution
thanks regular vaccinations and modern antibiotic therapy are the acquired bronchiectasis nowadays significantly less than before. Most bronchiectasis in Germany occur due to other diseases, mostly cystic fibrosis. Studies examining the frequency distribution within a given population come up with different numbers. So describes a study from the USA 52 cases of bronchiectasis per 100,000 population, whereas a study from Australia 3.7 cases in a population of 100,000 describes.
Symptoms
People who suffer from bronchiectasis mainly complain about productive, i.e. slime producing, to cough. When coughing comes usually slimy, foul smelling secretion to the fore which one also be bloody can and is typical for the clinical picture of bronchiectasis. If you were to fill the secretion into a glass or tube, you would observe three shifts can. There would be foam at the top, mucus in the middle, and pus at the bottom.
Since bronchiectasis go hand in hand with strong inflammatory processes of the respiratory tract, unspecific symptoms of inflammation can also be associated with the clinical picture. This would turn into a increased body temperature, but also show with pneumonia.
Since the bronchi are an important part of the system of the Breathing gas exchange represent and therefore equally one important part of the oxygen supply Our body often has symptoms that are associated with a reduced oxygen supply. These are especially on the hands Changes in chronic oxygen deficiency relatively easy to judge. Step there after a while Watch glass nails, such as Drumstick fingers on. The term watch glass nails describes the phenomenon that the connective tissue under the nail enlarges (hypertrophied), and in response to this, the nails bulge upwards, somewhat resembling a watch glass. The drumstick finger symptom has the same cause and describes one Change in the phalanges of the fingerswhich increase in size with chronic oxygen deficiency.
therapy
The clinical picture of bronchiectasis runs chronically and is from today's perspective basically not curable. Basic diseases that are responsible for the development of bronchiectasis should always be treated first. The current therapy principles are based on the attempt to prevent the disease from progressing. The usual approaches to therapy are generally divided into three different groups.
- The medical therapy relies on, among other things Medicationthat have an expectorant effect. These drugs include, for example N-acetylcysteine, its permanent use in patients with bronchiectasis however controversial is. Adequate hydration However, it is recommended in any case for affected people so that the secretion is not too thick and can be easily coughed up. Another drug, which is especially indispensable for frequent inflammation of the airways Antibiotics. Targeted therapy using sputum analysis can prevent life-threatening pneumonia and other complications. If the attending physician diagnoses inflammatory reactions of the bronchial tissue, a targeted cortisone therapy be indexed.
- The second indispensable form of therapy in bronchiectasis is the physical treatment of those affected. This can and should in part be carried out independently and regularly by the person concerned. The so-called "bronchial toilet" is important here Bronchial secretions coughed up daily should be. It is important to perform this maneuver precisely so that most of the mucus is mobilized from the airways. Expectorant medication can be taken to support this.
First the secretion should pass light tapping on the upper back be solved and then Coughed up with bowed torso and elbows on the knee become. There are various aids that can also make it easier to cough up the mucus. These tools range from Vibratory massagers to dissolve the phlegm on specific exercises that can be learned that make expectoration easier. Coughing up is important because the secretion bacteria collect that can cause inflammation and even dangerous complications like a Inflammation of the brain (Brain abscess) can trigger. - The third option of treatmentwhich can be quite useful in some cases is the surgical removal of lung tissue. However, this only makes sense if the drug and physical therapy are unsuccessful and an operation makes a successful treatment possible and likely. The operation can either be a whole lobe of the lung (Lobectomy) or just part of the flap, so one Lung segment (Lung segment resection) must be removed.
In the case of very advanced disease processes, the Lung transplant represent the remedy of the last choice.
forecast
The prognosis in those with bronchiectasis is this generally relatively good. Depending on the therapy, it can Significantly prevents progression of the disease become. Modern antibiotic therapies and consistent physical therapy, which avoids infections as much as possible, ensure that the Lifetime with this clinical picture usually not shortened.
course
The course of the disease in patients with bronchiectasis depends on the cause of the development of irreversible bulges in the large bronchi (bronchiectasis). If the cause is, for example, an inherited disease such as cystic fibrosis, the disease manifests itself early. If the cause is acquired later, for example through COPD, tuberculosis or a tumor, the disease does not start until later.
Since it is a chronic disease, the disease cannot actually be "cured", only the progression of the disease can be slowed down or stopped. The course of the disease is also dependent on factors such as the age of the patient, concomitant diseases, onset of the disease, compliance with preventive measures and therapy. Bronchiectasis occurs as a result of repeated inflammation of the airways and the disturbed outflow of bronchial secretions. Since the damage to the lung tissue is irreversible and the disease is chronic, it is desirable to diagnose the disease as early as possible in order to avoid worsening of symptoms and progression of the disease. The most important thing for positively influencing the course is regular mobilization of the secretion and coughing up. Ventilation of the airways should try to avoid infections of the lungs and prevent infections from breeding.
Read more on the topic: Signs of tuberculosis and Mucous bronchi
Life expectancy
Nowadays, the life expectancy of patients with bronchiectasis is hardly limited. Since the bronchial sacs are irreversible, the course can be significantly improved by avoiding infections and treating them with the help of targeted antibiotic therapy and a regular bronchial toilet, thereby reducing the complication rate enormously. Thanks to modern medicine and therapeutic measures and additional preventive measures, complications such as the aforementioned frequent bronchopulmonary infections, pulmonary bleeding and large accumulations of pus in the form of pleural empyema or lung abscess occur less frequently. The life expectancy of patients with bronchiectasis was very limited in earlier years, i.e. before the introduction of effective antibiotic therapy. But due to good basic immunization, regular booster vaccinations and separate vaccinations for high-risk patients, the prognosis and thus life expectancy has improved considerably over the years.
roentgen
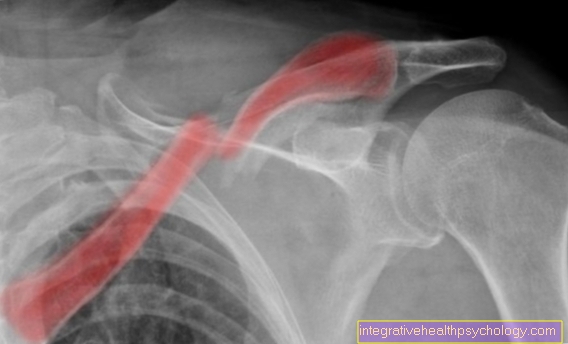
A chest x-ray can be very helpful if bronchiectasis is suspected, but is not sufficient to confirm the diagnosis alone. In the x-ray of patients with bronchiectasis, the sac-shaped or cylindrically shaped expansions of the bronchi, often inflammatory thickened bronchial walls can be seen. This results in a picture of parallel lines, also known as “tram lines” or known as rail signs.A liquid level may also be visible. In the late stage, the damage to the lungs becomes apparent as the lung tissue is replaced by numerous thin-walled and possibly fluid-filled cavities. The picture is similar to that seen in the terminal stages of pulmonary fibrosis and is called the "honeycomb lung".
Find out more about the topic here: X-ray of the chest
CT
A high-resolution computed tomography (HR-CT), a high-resolution imaging of the chest (CT-thorax), is a reliable method of detecting bronchiectasis. There are parallel and inflammatory thickened walls of the bronchi, the so-called "tram lines" or "rail signs". The bronchi appear enlarged, filled with air and often filled with mucus. Since the bronchi are accompanied by blood vessels and these are placed around the enlarged bronchi, this results in a typical "signet ring structure".
When do you need an operation?
Surgical therapy is considered particularly in younger patients with bronchiectasis, the frequent occurrence of hemoptysis (coughing up blood) and failure of conservative therapy or particularly severe disease. The operation is particularly effective when the changes only affect a specific section of the lungs on one side. The surgical techniques that can be considered here are the removal of part of the lung (lung segment resection) or a complete lobe of the lung (lobectomy).
Course of the operation:
Depending on the extent of the bronchiectasis findings, either part of the lung (lung segment resection) or a complete lung lobe (lobectomy) is removed. If the bronchiectasis is unilateral, surgery is the treatment of choice. Depending on the size and localization of the findings, one or more segments are cut out following the segment boundaries of the lungs during lung surgery under general anesthesia.
more information on this topic
Further information from the field of lungs and lung diseases:
- to cough
- lung infection
- Anatomy lungs
- Pulmonary function test
- Bronchitis symptoms
- Bronchitis cause
You can find an overview of all lung diseases at: Diseases of the lungs.