Bisphosphonates
Manufacturer
Bisphosphonates are now sold by almost all well-known manufacturers.
The first substance that was brought onto the market was Fosamax®. Most of the information exists about this substance. The active ingredient alendronic acid or alendronate is still the so-called lead substance for osteoporosis in need of therapy. The effectiveness of new substances is being tested against this drug.
Other manufacturer names of bisphosphonates are for example:
- Actonel ®
- Fosamax®
- Fosavance®
- Bonviva®
- ......
Further information on bone density measurement can be found here.

What is bisphosphonate?
Bisphosphonate is the chemical name of the active ingredient in various drugs that are used to treat from tumor especially in the head area but also in other locations and especially for the treatment of osteoporosis can be used.
Also in the Gynecology - next to the Orthopedics and Dentistry - we will find the bisphosphonates at Breast cancer Use. They are taken as tablets or given as an infusion. However, their absorption, i.e. the uptake into the body, is very low and ranges from 1 to 10%. Most of it is active on the bone, the rest is excreted.
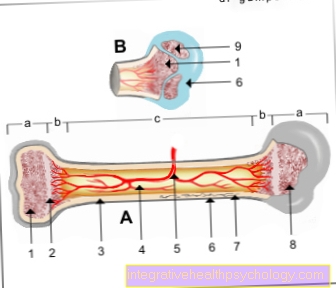
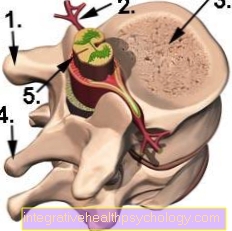
The bone is subject to constant build-up and breakdown. In the osteoporosis the breakdown by the bone-breaking cells outweighs the osteoclasts.
Calcium is lost and the bone becomes porous. There is a risk of breakage and pain. The treatment of osteoporosis with bisphosphonates is based on the inhibition of osteoclast activity.
Effect of bisphosphonates
Bisphosphonates accumulate in the bone and inhibit degradation processes there, so that the bone substance is stabilized.
In the bone there are cells that, like small phagocytes, always eat a small part of the bone and thus break it down. In addition, there are cells that continuously produce bone substance and thereby renew the bone and strengthen it.
In women after the menopause, in old age in general or in diseases of the bone such as tumor diseases, the building processes decrease. That is why there is an excess of bone loss. As a result, the bone loses stability and becomes brittle.
In addition, increased bone resorption can lead to pain. One reason for this pain is that tumor cells and their harmful ingredients and signaling substances accumulate in the bone in tumor diseases, which are released when the bone is broken down. After taking bisphosphonates, they are stored in the bones and released during remodeling processes. Their main effect is to inhibit the cells that break down the bone.
As a result, the balance is shifted in favor of bone structure. Since the breakdown of all substances in the bones is reduced by bisphosphonates, they lead to a reduced release of harmful substances, especially in the case of tumor diseases of the bone marrow. As a result, fewer signal substances that could activate and attract other tumor cells are released and the pain associated with tumor diseases is reduced.
Bisphosphonates can also be used in the context of bone edema in the knee, whereby bone loss is reduced. For more information, read our article: Bone edema of the knee
Active ingredients of bisphosphonates
The active ingredients of bisphosphonates can be differentiated according to whether they contain nitrogen or not.
The substances with nitrogen, such as alendronic acid (Fosamax®) and ibandronic acid (Bonviva®) usually have a stronger effect.
Although both groups of active ingredients attack at a different point, they all cause a loss of function of the bone-degrading cells, which ultimately leads to the death of these cells.
The nitrogen-free bisphosphonates include etidronic acid (Didronel®) and clodronic acid (Bonefos®).
In all groups there are drugs that are taken in tablet form and drugs that are given through an access into the patient's vein.
In tablet form, in particular, all active ingredients must be taken with a glass of water at least half an hour apart from meals, as they combine with substances such as calcium and can therefore no longer be adequately absorbed.
There are similar problems when taking the active ingredients with iron, magnesium or zinc at the same time.
Ibandronic acid can be given as a tablet or as an infusion, the other drugs mentioned are taken in tablet form. The active ingredient reaches the blood directly via a venous access and is therefore completely available regardless of whether it is absorbed in the intestine. However, attention must be paid to the exact dosage, since both the effect and the undesirable side effects can be stronger.
Indications for bisphosphonates
Bisphosphonates are used in diseases that are associated with increased bone loss. These include, for example:
- Paget's disease (Osteodystrophia deformans)
- Tumor-associated hypercalcemia
- Bone loss (Osteolysis) in the context of tumor diseases (including tumor metastases) and
- postmenopausal osteoporosis, a disease popularly known as "bone loss" in women after menopause.
Another indication for bisphosphonates is also used for diagnostic purposes in the context of nuclear medicine skeletal scintigraphy.
Due to their anti-osteolytic properties, bisphosphonates have an inhibitory effect on the breakdown of bones. This effect is mainly mediated by the inhibition of so-called osteoclasts (bone-eating cells). Since they are stored directly in the bone after resorption, they can develop their effect quickly at the target location. For this reason, bisphosphonates are used in diseases that lead to excessive osteoclast activity and thus severe bone loss. In fact, they are currently the most commonly prescribed drugs for treating osteoporosis.
Read more on this topic at: Transient osteoporosis
Bisphosphonates are widely used, especially for the treatment of osteoporosis in women during and after the menopause. Due to their mechanism of action, bisphosphonates can also be used in men to contain osteoporosis-related bone changes. In the so-called glucocorticoid-mediated osteoporosis, bone loss provoked by the tissue hormones can be observed. In these cases too, bisphosphonates are able to prevent the progression of bone damage by inhibiting bone-eating cells.
Another typical indication for the use of bisphosphonates is the disease known as glass bone disease (technical term: Osteogenesis imperfecta) known disease. It is a hereditary disease that leads to changes in collagen synthesis in those affected and thus to extremely brittle bones.
In addition, drugs from this group of drugs are approved for the treatment of bone metastases that lead to excessive bone loss.
Another classic indication for the administration of bisphosphonate-containing drugs is so-called Paget's disease. This disease is a focal change in the bone structure. In the affected patients, pathologically increased bone remodeling can usually be demonstrated. In the course of these diseases there is an increase in bone formation and breakdown in alternating phases. Since both phenomena take place in different compartments of the bone, the result is a disturbed architecture with severe restrictions on the load capacity. Bisphosphonates are mainly used in Paget patients to contain the bone loss phases. Since one can also make use of the inhibition of the osteoclast function here to prevent the disease from progressing rapidly.
In addition, bisphosphonates are now used for endocrine therapy in hormone-sensitive breast cancer. According to an extensive study from 2009, the recurrence-free survival time of breast cancer patients was significantly increased by taking the bisphosphonate zoledronate.
In addition to the therapeutic indications, bisphosphonates can also be found in diagnostics. In connection with 99m-technetium, a radioactive tracer, bisphosphonates can be used in nuclear medicine examination procedures. In this field, bisphosphonates are administered in particularly low, pharmacologically ineffective doses. The accumulation in the bone can, however, be observed with a special camera and thus indications of bone changes can be obtained.
Side effects of bisphosphonates
As with all highly effective drugs, there is unfortunately also the Bisphosphonate Side effects.
We call them side effects, but in reality they are also effects that we don't want to have. Next Intolerance of the stomach can also be bisphosphonate conditional Bone necrosis in the jaw occur. However, this undesirable side effect is very rare. It is not a question of the destruction of the bone tissue caused by bacteria, but a spontaneous, aseptic process.
Pine necrosis during therapy with bisphosphonates
The term necrosis means that cells are hit so badly by damage of any kind that they die and decay.
This damage can be, for example, radioactive radiation, poisons or drugs.
Necrosis of the jaw can also develop during therapy with bisphosphonates, which strongly influence the remodeling process of the jawbone.
The bone becomes more unstable and tends to break. In addition, the jaw necrosis manifests itself in the fact that more and more bones are exposed under the oral mucosa.
Purulent spots appear in the mouth area. Without any other cause, the teeth loosen and sometimes fall out.
This damage to the jawbone can lead to severe inability to chew. To definitely speak of necrosis of the jaw, the open areas that reach to the bone must exist at the same point for at least eight weeks.
In addition, it must be established with certainty that the cause of the necrosis is really bisphosphonate therapy. For this it must be ensured that no therapy with radioactive substances has taken place in the head and neck area.
Other therapies such as certain chemotherapy for cancer diseases or taking medication that affects the bone structure must not have taken place.
Symptoms of jaw necrosis during therapy with bisphosphonates
The symptoms are for the most part painless.
Soft tissue swelling, loosening of the teeth, exposed jawbones or even protracted inflammation of the tooth support system can be signs of this bone necrosis caused by bisphosphonates.
It is not yet known why such symptoms occur in rare cases. It is doubtful whether tooth extraction or the treatment of the tooth supporting apparatus are the possible causes. In any case, the doctor and dentist should look after the patient together.
Prophylaxis of pine necrosis in therapy with bisphosphonates
Prophylaxis is not yet known. Individual patient requirements can pose a risk. Therefore, the dentition should always be rehabilitated before therapy with bisphosphonate. This includes the treatment of carious teeth as well as the elimination of inflammatory processes in the oral cavity. A regular visit to the dentist is recommended.
Therapy of bisphosphonate-associated jaw necrosis
The treatment of bisphosphate-associated bone necrosis is difficult and lengthy. It includes the removal of the submerged, dead bone and the covering of the defect.
Incidence of pine necrosis in therapy with bisphosphonates
In patients receiving bisphosphonates as tablets, pine necrosis is very rare, with an incidence of 0.0007% per year.
This undesirable side effect occurs most frequently in patients with tumor diseases who receive a very high dose of bisphosphonates through an access directly into the vein.
Pine necrosis occurs in 0.8-12% of patients per year.
In the disease of multiple myeloma, in which white blood cells develop into malignant cells, immigrate in particular into the bone marrow and spread there, the incidence of pine necrosis with bisphosphonate therapy is 1-10%.
Risk of pine necrosis during therapy with bisphosphonates
The risk of developing jaw necrosis from treatment with bisphosphonates is heavily dependent on other factors that themselves increase the risk of jaw necrosis.
For example, drugs such as hormone preparations that are used to treat tumor diseases of the prostate or breast can lead to bone loss.
To avoid this, bisphosphonates are used. If jaw necrosis occurs during therapy with both drugs, it is difficult to say which drug is the main cause of the complications.
Other known risk factors are old age, smoking and diabetes mellitus. In addition, dentures that always press the same places on the jaw can lead to a breakdown of the bone.
Long-term inflammation and infections in the tooth and jaw area also permanently damage the tissue and, if the therapy is inadequate, can promote necrosis of the jaw. For this reason, the dentist should perform a check-up before starting therapy and ensure good oral hygiene.
In addition, the risk increases with the frequency and dose of bisphosphonates. In particular, areas of the jaw that are only covered with a very thin layer of the oral mucosa are often affected. The lower jaw has the greatest risk of developing jaw necrosis.
To this topic have dedicated a completely separate topic: Bisphosphonate-associated jaw necrosis
Therapy of pine necrosis
The most important therapy approach for jaw necrosis caused by bisphosphonates is to prevent the aggravation and spread of the necrosis and the development of new necrosis.
First of all, the pain that has occurred should be treated. In addition, infections can be prevented by means of an antibacterial mouthwash even before taking the bisphosphonates. If an infection already exists, it is treated with antibiotics. However, if the affected areas of the jaw are no longer able to repair themselves, the damaged part of the bone must be removed by a surgeon.
Particular attention should be paid to necroses that have not yet reached the surface of the jaw. The remaining, not yet affected part is covered again with the normal oral mucosa. Thereafter, the pain will continue to be treated. Furthermore, the tissue in the wound area can heal better through the administration of oxygen.
If renewed eruptions occur after the diseased bone parts have been removed, it may be that additional, very large sections of the jaw have to be separated. First, different plates are screwed on as a replacement. However, if the disease shows signs of stagnation, these can be permanently replaced by bone parts that are removed from another part of the body.
Interactions in therapy with bisphosphonates
The interaction of the bisphosphonates consists particularly in the fact that they have chemical properties that bind certain positively charged substances.
These are, for example, calcium, iron or magnesium. The binding means that fewer bisphosphonates and fewer other substances are absorbed into the body. Since only a very small proportion of the bisphosphonates reaches the great bloodstream and the bones anyway, this interaction can greatly weaken the effect of the bisphosphonates.
If there is not enough free calcium in the body, which is needed to build a stable bone, the bones lose their strength. To prevent this, the bisphosphonates should be taken at least half an hour apart from meals.
Bisphosphonates and renal insufficiency
Bisphosphonates are mainly excreted via the kidneys (eliminated renally). This must be taken into account in patients with impaired renal function. Dose adjustments may need to be made in patients with mild to moderate renal impairment.
The use of bisphosphonates is contraindicated in patients with severe renal insufficiency, i.e. a creatinine clearance of less than 30-35 ml / min.
It is also known that - irrespective of any existing renal insufficiency - if bisphosphonates are infused too quickly, complex formation with calcium ions can lead to acute renal failure.
Read more under our topic: Renal failure
Summary
In summary, it can be said that necrosis of the Jawbone, caused by the therapy with bisphosphonate as a side effect represent a rare complication.
The cause of the occurrence is still largely unclear. The symptoms are uncharacteristic and mostly painless.
Therapy consists in removing the submerged bone and restoring the bone structure. The prophylaxis consists in the rehabilitation of the teeth followed by more careful Oral hygiene and supervision by the dentist.