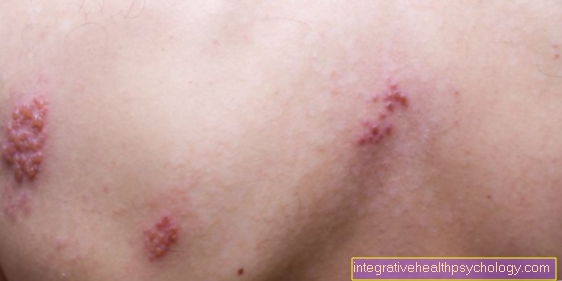
Inflammation of the prostate
definition

The E.ignition of the prostate is one of the most common urogenital diseases in the male population: around 10% of men suffer from one once in a lifetime Prostatitis. It occurs preferentially between the 20 and 50 years of age but can ultimately also affect older men.
The prostate is generally considered a relative organ prone to inflammationwhat by the strong blood circulation, the large number of glands and the direct connection with the urethra is conditional, the latter being a gateway for potential pathogens.
The inflammation of the prostate goes in many cases with a simultaneous inflammation of the Epididymis (Epididymitis) or des Ureter (Urethritis) hand in hand. A distinction is made between an acute inflammation and a chronic prostate inflammation, whereby the chronic form can often arise from an acute, which has not healed.
If no causative pathogen can be detected in the course of the examination and diagnosis, one speaks of a abacterial prostatitis or from one chronic pelvic pain syndrome. This type of prostate inflammation is the most common.
If no organic causes for the patient's complaints can be found, it can also be one Prostatodynia act that to the psychosomatic shape circle is counted.
causes
The most common causes of inflammation of the prostate include pathogens in the context of urethritis, cystitis or epididymitis, which rise to the prostate in the form of a urinary tract infection and infect it. In the course of the inflammatory process, immune cells (white blood cells, leukocytes) accumulate in the tissue of the prostate, which leads to swelling and tissue irritation.
In the case of young men, these are predominantly Chlamydia and Ureaplasma, older men, on the other hand, are more likely to suffer Inflammation of the prostatecaused by the gram-negative rod bacteria normally found in the intestine Escherichia coli (E. coli) is triggered. Among the more rare pathogens Klebsiella and Mycobacteria in the context of tuberculosis.
In this regard, the causes for the development of a Urinary tract infection in men it is always also a major risk factor for prostatitis: for example Kidneys- and Bladder stones, Diabetes mellitus, a weakened immune system, Tumors, to little drinking and cold (Sitting on cold surfaces, wet swimming trunks, etc.). The latter leads to a reduced blood flow in the area of the small pelvis, which makes it difficult to quickly wash up immune cells when bacteria penetrate and thus promotes inflammation.
Introduced pathogens are always possible urological examinations or. Interventions, like this for example when laying and lying one Urinary catheter, the removal of a prostate biopsy or a uroscopy may be the case.
A narrowing or obstruction of the urethra - through - also favors the colonization of the urinary organs bacteria, so that the risk of a spread infection of the prostate increases significantly here as well.
The spread of pathogens from foci of inflammation outside the genitourinary system via the Blood and lymphatic systems, but should always be considered in the diagnosis.
The cause of that chronic pelvic pain syndrome or the abacterial prostate inflammation have not yet been fully clarified. According to some theories, certain Microorganismsthat cannot be cultivated and therefore also undetectable can be a possible trigger, but also Voiding disorders. Urine outflow problems from the bladder cause it to develop over time Urine buildup and Increase in volume of the bladderthat then pressure on the immediate adjacent prostate can exercise. Because of this chronic pressure, it can eventually become one Tissue irritation and finally to one abacterial inflammation come.
Likewise, a Inflammation of the bladder even on the prostate spread out or a Nerve irritation in the immediate vicinity of the prostate adulterated prostate pain to lead. One is even possible overactive immune system, which is part of a Autoimmune reaction attacks the prostate tissue and leads to inflammatory damage.
As the cause of the occurrence of the so-called Prostatodyniathat is caused neither by an organic disease nor by bacteria becomes a Over-excitability of the pelvic floor muscles suspected that tends to cramp and thus the Pain symptoms can cause.
Symptoms
The symptoms of a acute inflammation the prostate are primarily the occurrence of high fever (with possible chills), Pain at the bowel movement and Burn at the Urination (Alguria, Dysuria) a frequent need to urinate (Pollakiuria), although only small amounts of urine can be released. Complete urinary retention may occur. Can join Pain in the Anal-, dam-, Testicles-, element-, Afford-, Move- or Pubic area such as Pain during and / or after the ejaculation. In addition, you can Blood in the urine and or Ejaculate stand out.
The chronic prostate inflammation however, is of the Symptoms here more unspecific: a slight feeling of pressure in the perineal area, impaired sexual function (Erectile dysfunction) and - as in the case of acute inflammation - a permanent one Urge to urinate With Sensation of pain at the Urination.
diagnosis
There are several ways to diagnose inflammation of the prostate.
As part of the physical examination at the doctor's, a digital rectal examination (the attending doctor manually examines the last section of the intestine and can also feel the prostate) can already provide information about the size and nature of the prostate: an inflamed prostate is usually mild enlarged and tender on pressure. If an abscess has already formed on the prostate during the course of the inflammation, it can also be felt.
Another quick and easy way to get information about an inflammation of the prostate is to take a blood sample. In acute prostatitis, the inflammation levels in the blood can be significantly increased, as can the inflammatory cells (leukocytes) and the prostate-specific antigen (PSA) as organ-specific markers. In the case of chronic prostate inflammation, on the other hand, it may well be that there are no pathological changes in the patient's blood.
In addition to the blood sample, a urine sample can also indicate an inflammation of the prostate: acute prostatitis is noticeable in the urine through massive amounts of inflammatory cells (leukocytes), bacteria and red blood cells, whereas the chronic form can be normal here too.
Also known is the so-called four-glass test, in which both the first urine and the midstream urine, the urine after prostate massage and the prostate secretion are examined for signs of inflammation and for pathogen diagnostics. Examining a sample of ejaculate can also help determine inflammation.
The primary imaging diagnostic is the ultrasound examination (sonography), in which inflammatory changes in the prostate tissue, the size of the prostate and abscess formation can be shown. The ultrasound examination is usually carried out through the anus. Another possibility of examination is the MRI.
Read more on the topic MRI of the prostate
Uroflowmetry can be used as an additional examination to check for urinary flow and urination disorders. Here, the maximum urine flow and the amount of urine released in a certain time are measured.
If there is a suspicion of a narrowing of the urethra, a so-called urethrography can be performed, whereby a contrast agent is injected into the urethra and an X-ray of the urinary system is taken
In order to rule out possible differential diagnoses such as benign prostate enlargement or prostate carcinoma, a prostate biopsy can be performed if the previous findings are unclear.
therapy

The acute and the chronic prostate inflammation differ in individual aspects in the therapeutic procedure.
The acute, bacterial inflammation is primarily with one prescribed by the respective doctor antibiotic treated in high doses to combat the causative agent (e.g. Co-trimoxazole, cephalosporins, gyrase inhibitors). Exactly which antibiotic is chosen depends on the exact one Determination of pathogen and pathogen resistance as part of the diagnosis.
If necessary, a temporary Drainage of the urine from the bladder by means of a Catheter (Urinary catheter) to be necessary. Should be part of the inflammation purulent abscess have developed in or around the prostate, this must be surgically opened. In addition, can Painkiller and antispasmodic medication may be given.
A chronic form of prostatitis is also tried with Antibiotics to counteract, but this often does not lead to the desired success. This is mostly a long-term antibiotic therapy, which - as with the acute form - with pain reliever and relax Medication can be combined.
Alternative therapeutic approaches, such as the administration of, achieve better results Phytotherapeutic agents (Medicines made from medicinal plants) such as quercetin (natural pigment made from certain fruits and herbs, which acts as a radical catcher and antioxidant) or pollen extracts. Also Alpha blockers (e.g. Tamsolusin), 5-alpha reductase inhibitors (e.g. Finasteride) and the Antifungal agent Mepartricin can improve symptoms of chronic inflammation of the prostate.
As an accompanying therapy for acute or chronic prostate inflammation, the use of warm hip baths or that Wear warm clothes possible what through an improved Blood circulation in the small pelvis for Decongestion and relief of pain and tension can lead.
Other home remedies that can be used to treat the symptoms are drinking Fireweed tea, one vegetarian diet and herbal alternatives like Nettle root, Pumpkin seeds, Rye pollen, Pumpkin and Saw palmetto fruits.
Also in the homeopathy there are specific therapeutic approaches for prostate ailments in the context of inflammation: this includes the ingestion of Aristolochia, Clematis or Sabal Serrulatum (Medicinal plants) in a dosage prescribed by an alternative practitioner.
forecast
The forecast of the Prostatitis depends largely on the course and the start of therapy. An acute one, quickly with antibiotic Treated prostate inflammation usually heals without consequences and therefore has a very good prognosis. Approx. 60% of the patients show no more symptoms after 6 months, in approx. 20% goes the acute inflammation in a chronic form over. In terms of prognosis, this is worse; it often happens over many years to always recurring flare-ups.
In addition, a chronic inflammation of the prostate (but also an untreated acute prostatitis) leads to permanent infertility can lead: through the inflammatory process it can lead to one Bonding or Strictures (urethral strictures) to a (in) complete Closure of the draining seminal ducts come. A relocation of the Vas deferens can thus restrict or disrupt the transport of sperm.
On the other hand, the Sperm function (Sperm motility) themselves and the Composition of the ejaculate through secondary inflammatory reactions impaired become.