Testicles
Synonyms
Lat. = Testis (pl. Testes)
English: testicles
definition
The paired testes (testis) count together with the epididymis, the spermatic duct and the male sex glands (Vesicle gland and prostate) to the internal male genital organs.
They are used to produce the sperm cells (Sperm) and are located below the male member. Every testicle is on the spermatic cord,hung up“And lies loosely in the surrounding scrotum. They serve as gonads for the production of sperm and hormones, which is regulated by the hypothalamus and pituitary gland.

Function of the testicles
The testes are used on the one hand to produce hormones, the androgens, and on the other hand to form sperm for reproduction.
The Leydig cells, which mainly produce testosterone, are responsible for hormone synthesis. Testosterone is important on the one hand for stimulating the formation of sperms, on the other hand for the development and maintenance of the function of the other genital organs.
The development of the sperm is essentially made possible and supported by the Sertoli cells. They form a supporting framework of cells in which the sperm mature from the germ cells.
The epididymis act as a store for sperm. They also serve to develop their function.
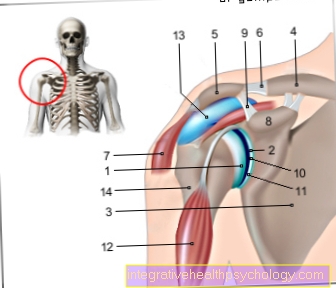
Illustration of the testes and epididymides

Testicles and epididymis
- Testicles - Testis
- Epididymis - Epididymis
- Scrotum - scrotum
- Epididymis -
Cauda epididymidis - Epididymis -
Corpus epididymidis - Vas deferens -
Deferens duct - Urinary bladder -
Vesica urinaria - Tendril vein plexus -
Pampiniform plexus - Testicular artery -
Testicular artery - Epididymis -
Caput epididymidis - Connective tissue cover -
Tunica albuginea - Testicular walls -
Septula testis - Testicular lobe -
Lobuli testis
You can find an overview of all images by Dr-Gumpert at :medizinische images
Development of the testicles
In the course of embryonic development, the testis migrates from the abdominal cavity through the inguinal canal to its definitive place in the scrotum. The reason for the relocated position of the testicles is the lower temperature there, which is necessary for the development of the testicle and the formation of sperm.
The testis-determining factor (TDF) on the Y chromosome, which only men have, is responsible for the development of the testes. This causes the preliminary stages, the still indifferent gonads, to develop into the definitive testicle.
The systems of the female sexual organs are reduced by the anti-Müllerian hormone (AMH). This hormone is produced by special cells in the testicle, the Sertoli cells.
Cells in the testis, the Leydig cells, begin in the 8th embryonic week with the formation of the hormone testosterone, which causes the formation of the male genitals.
Anatomy of the testes

The testicles (Testis) are located outside the abdominal cavity in the scrotum. One epididymis (lat. Epididymis) sits on the back, within the scrotum.
The testicles have an elongated, oval shape with a diameter of 3 cm and a length of 4 cm.
In the testicle begins a system of different canals (Latin = tubules) and passages (Latin = ductus), which leave the organ at the mediastinum, a central pole, and in the epididymal canal, the Ductus epididymidis, flow. This continues as the ductus deferens, then runs through the inguinal canal into the abdominal cavity and connects to the urethra via the short ductus ejaculatoius.
You might also be interested in: Scrotum
Histology of the testicle
The testicle is divided microscopically (Testis) in about 370 testicular lobules (Lobuli testis), which are separated from each other by connective tissue septa. Each testicular lobe in turn consists of 1 to 4 testicular tubules (Seminiferous tubules), which are strongly compressed by twisting them up.
The seminiferous tubules are formed by two types of cells, the Sertoli cells and the germ cells of sperm development. The Sertoli cells provide a supportive environment for the germ cells from which sperm cells arise.
The seminiferous tubules are then placed over short straight tubules (Recti tubules) into reticulated tubules (Rete testis) continued. These lead to further duct systems, the Efferent ductswhich lie at the upper pole of the testicle. This is then followed by Ductus epididymidis as Deferens duct at.
In its entirety, the duct system of the testicle is enclosed by a tough connective tissue capsule, the tunica albuginea. A two-layer serous covering (Tunica vaginalis). The inner leaf adjacent to the tunica albuginea is called the epiorchium, the outer one is called the periorchium. In between there is a gap containing a little liquid (Cavitas serosa scroti). On top of it lie two fasciae (fascia spermatica interna and externa), the tunica dartos consisting of smooth muscles, the dermis and finally the scrotal skin of the scrotum.
The tissue between the duct system is made up of loose connective tissue, blood and lymph vessels and cells between them. These cells between the testicles are called Leydig cells. They are used for the production of sex hormones, the androgens.
How big is a normal testicle?
The exact size and volume of the testicles can be determined with the help of an ultrasound examination. The norm for the size of the testicles in adult men is indicated by the following values:
The length is usually between 4-5cm. The width is 2-3cm. The normal volume is 15-35ml in adults.
In boys, the normal values are based on the respective phase of development and puberty. In medicine, these are classified according to the so-called Tanner stages.
- Before puberty, in stage I, the testicle volume is still less than 1.5 ml.
- As development progresses, the testes in stage II enlarge to a volume of 6ml.
- In stages III and IV, the size of the penis increases along with the volume of the testicles, which is then 12-20ml.
- When stage V is reached, development is finally complete and the values correspond to those of an adult.
Testicles of different sizes
Although the two testicles lie together in the scrotum, they are biologically to be regarded as two separate organs. Therefore, there may well be a size difference between the two sides. First of all, this is not a cause for concern and, to a lesser extent, usually has no disease value.
However, if you notice a one-sided increase or decrease in size, you should always have a one-off diagnosis by a doctor in order to rule out possible diseases as the cause. Testicular cancer in particular often causes no symptoms for a long time as they grow. In order to be able to recognize and treat them at an early stage, it makes sense to have changes in the testicles clarified by a doctor promptly.
Signs that can indicate a disease are, for example, pain or redness, a very pronounced difference in size, palpable hardening or nodules in the testicles, a change in size in a short time or an indefinite feeling of heaviness in the entire scrotum or limited to one of the two testicles.
One-sided swelling of the testicles can be caused by inflammation or injuries, e.g. a water or testicle hernia, testicular varicose veins or testicular torsion.
A one-sided testicle reduction can also be the result of injuries or testicular torsion. Furthermore, circulatory disorders are a possible cause of a difference in size of the testicles.
Diseases of the testicle
Twisted testicle
Due to their anatomical structure and their location, the testicles are very susceptible to external influences such as heat or injuries. The most common injury is the twisting of a testicle (Testicular torsion).
The causes of a twisted testicle are usually traumatic events (for example a kick in the testicle). But there are also congenital, twisted testicles. This already happens in the womb. If a testicle is twisted, it wraps itself around the testicle stalk with the epididymis (Spermatic cord). The main problem here is the lack of blood supply.
The vessels that supply the testes run parallel to the spermatic cord. A twisted testicle is a medical emergency and should be treated by a doctor as soon as possible, as the lack of blood supply can lead to testicle death and infertility.
Read more on the topic: Testicular torsion
Undescended testicles
In contrast to other organs, the male testicles are not placed in their later location in the scrotum, but only shift there in the later stages of development before birth. However, this can lead to errors or interruptions. This leads to one or both testicles remaining at a point between the place of formation in the abdominal cavity and not reaching the actual location in the scrotum. This is called undescended testicles.
The most common place where the testicle is instead is the inguinal canal. One then speaks of so-called inguinal testicles. Another form is the so-called sliding ode. Here, the testicle is also located in the inguinal canal, but it can be moved back into the scrotum by hand from the outside. The reason for this is usually a spermatic cord that is too short or a cremaster muscle that is too strong.
The pendulum testicle is a special form of undescended testicles. During development, the testicles have been completely lowered into the scrotum, but the testicles can spontaneously shift out of the scrotum. In contrast to the other forms of undescended testicles, therapy is not absolutely necessary as long as the testicle is located in the scrotum for the greater part of the time.
Since the displacement of the testicles can only be delayed, you can wait until the age of 1 to see whether the lowering will happen by itself. Supportive therapy with hormones can be carried out from the 3rd month of life, which normally initiate the displacement of the testicles in the body. If this is not successful, the testicles should be surgically relocated to avoid infertility.
For more detailed information, see Undescended testicles.
Inflammation of the testicles
Testicular inflammation usually occurs due to pathogens that have been carried over, e.g. as part of urinary tract infections. Since, depending on the localization of the actual cause of the infection, the pathogens to be expected differ and this is decisive for the choice of the appropriate therapy, in the case of testicular inflammation one should always look for other infections in the body.
Read more about this in our main article: What are the causes of testicular inflammation?
Typical symptoms of testicular inflammation are sudden, severe testicular pain, swelling, and reddening and overheating of the affected testicle. Furthermore, there is usually a very pronounced feeling of illness with exhaustion and weakness as well as fever. Since more serious clinical pictures such as testicular torsion or testicular tumors with similar symptoms can appear, they should always be clarified by a doctor.
Therapy usually takes the form of bed rest, cool compresses, elevated testicles and antipyretic medication. If the infection is caused by bacteria, antibiotics are also used.
Read on below: Inflammation of the testicles
Ingress of water in the testicles
A water rupture, a so-called hydrocele, is an accumulation of fluid between the layers of tissue that surround the testicles. These layers of tissue are mainly formed by a part of the peritoneum which, when the testicle descends from the abdominal cavity, bulges around the testicle and, with it, protrudes into the scrotum. Normally, the connection to the abdominal cavity recedes over time so that there is no longer an open connection. If this does not happen completely, fluid can spill from the abdomen into the testicles, collect there and lead to swelling of the testicle. However, this is usually painless.
The diagnosis is usually made by palpating the testicle and an ultrasound examination. Small, symptom-free hydroceles can be observed. However, if there is a strong increase in size, surgical treatment should be carried out.
So-called secondary hydroceles, i.e. an accumulation of fluid as a side effect of another disease, can occur, for example, in the context of inflammation or testicular injuries. First of all, the underlying disease should be treated. If the accumulation of fluid is very large or if additional symptoms arise, surgical removal should also be considered here.
Find out more at: Water in the testicle
Testicular hernia
A testicular hernia is not an injury to the testicle, as the name might suggest, but a displacement of parts of the intestinal loops into the scrotum.
This can happen if part of the peritoneum turns inside out through a weak point in the connective tissue of the abdominal wall. Due to the weight of the organs in the abdominal cavity and pressure from the inside, the protuberance can enlarge and spread through the inguinal canal over the outer inguinal ring into the scrotum. The testicular hernia is therefore a special form of the inguinal hernia.
A testicle hernia is usually noticeable as a swelling of the testicle with no noticeable signs of inflammation. Pulling pains in the area of the testicles and groin can also occur. The testicular hernia is diagnosed primarily through a physical examination, and ultrasound imaging can be used as a support.
Testicular hernias are treated therapeutically by surgically relocating the intestinal loops and closing the tissue hernia. As a rule, the procedures are carried out in a minimally invasive manner. Small testicular fractures that do not cause any symptoms do not have to be treated immediately but can also be observed. However, since there is always the risk of entrapment of the intestinal loops, an operation may also be advisable here.
If you suspect a testicle hernia, it is therefore essential to consult a doctor.
Read more on the topic: Testicular hernia
Testicular cancer
Testicular cancer (Testicular cancer) is the most common type of cancer in men.
There are now good therapeutic options so that patients can often be cured. Early detection is particularly important in testicular cancer.
Because especially in the early stages, many patients can be helped well. Symptoms of testicular cancer are mostly lumpy changes or an increase in the size of the testicle. If the testicle feels heavy or hurts, this can also be an indication of testicular cancer.
But especially pain, especially in the early stages, is very rare. If you have a painful testicle, you should also rule out other diseases or injuries such as twisting of the testicles.
If testicular cancer is suspected, the doctor can quickly palpate it and confirm it with an ultrasound examination so that, in the best case scenario, therapy can begin immediately. This significantly increases the chances of recovery. Through regular self-examination of the testicles, every man can help to identify testicular cancer at an early stage and, if necessary, to increase his own chances of recovery.
Testicular varicose veins
Similar to the veins of the legs, varicose veins can also occur in the veins that are responsible for the drainage of blood from the testicles. This is called Varicocele. A primary varicocele is caused by weak venous valves in the spermatic vein. This leads to a backflow or an insufficient outflow of blood and a backflow into the venous plexus of the testicle.
This leads to the typical symptoms of a feeling of heaviness in the scrotum and an increasing swelling of the testicle, especially when standing. As a rule, primary varicoceles appear on the left side.
A distinction must be made between secondary varicoceles which are caused by an obstruction to the flow of the veins from the outside, such as a constriction by a tumor. Primary varicoceles are usually only treated if there is a very clear difference in the size of the testicles, severe symptoms or impaired fertility.
As therapeutic measures, obliteration of the vessels using a catheter or surgical obliteration or ligature are available. Secondary varicoceles are treated by treating the underlying disease.
Testicular atrophy
Testicular atrophy is the reduction in testicular volume or functional testicular tissue. The normal volume of a testicle is between 15-35 ml. However, a reduced volume does not mean that the functionality of the testicle has also been lost. As a rule, up to a volume of 1ml, an, albeit limited, production of sperm and sex hormones can be detected. As a rule, synthesis no longer takes place below this limit, as the proportion of functional testicular tissue is too low.
In most cases, the shrinkage of the testicle can already be recognized during the inspection of the scrotum or palpated during the examination. The exact volume is determined with the help of ultrasound. In order to check the functionality of the testicle and to find an indication of possible causes, the levels of the sex hormones are determined. On the one hand, there are LH and FSH, which are responsible for stimulating the testes, and, on the other hand, testosterone, which is produced in the testes.
The possible causes of testicular atrophy are many. On the one hand, there may be genetic changes, such as Klinefelter syndrome. On the other hand, previous damage such as circulatory disorders, testicular fractures, inflammation or testicular torsion can lead to subsequent testicular atrophy.
The consumption of certain substances such as alcohol or anabolic steroids can also be a possible cause. Like the causes, the therapies are also very different and essentially consist of eliminating the cause, e.g. the surgical restoration of blood circulation or treatment of the inflammation with the help of medication.
Here is the main article Testicular atrophy.
Testicular mumps
Under one Mumps orchitis one understands an inflammation of the testicles which occurs in the context of an infection with mumps.
Mumps is described as one of the typical childhood diseases, as over 80% of those infected are between six months and 15 years old. Although there has been an effective vaccine against the disease since the 1970s, sufficient immunization has still not been achieved in the population in Germany, which means that the first illnesses increasingly extend into adulthood.
Up to a third of men who become infected with the disease in adulthood experience an accompanying inflammation of the testicles. This manifests itself primarily in a very strong, usually one-sided swelling of the testicle and an associated significant difference in the sides. Furthermore, the affected testicle is very sensitive to touch and very painful to external pressure. Furthermore, there is usually a reddening and overheating of the testicle.
In the context of mumps, there are also fever, fatigue and, usually before the onset of testicular inflammation, inflammation and swelling of the parotid gland.
Therapy usually consists of bed rest, elevated testicles, cooling compresses, and anti-inflammatory and antipyretic drugs. Consequences of the disease can be a decrease in the size of the testicles and, in rare cases, infertility.
You might also be interested in: Mumps symptoms, treatment & vaccination
Testicular rupture - The burst testicle
As a result of a blunt force on the testicles, it can happen that they burst. One then speaks of a testicular rupture. Great force is required to cause such a rupture at all. This is about 50kg.
In the course of the injury, the inner testicle sheaths tear, especially the so-called tunica albuginea. This forms the innermost layers of tissue and is responsible for the strength of the testicles due to its connective tissue structure. The tear can lead to massive bleeding. These can usually be seen from the outside as bruises. Furthermore, a testicular rupture manifests itself with massive pain and reactions from the body such as nausea and vomiting.
An ultrasound examination or an MRI is performed to determine the extent of the injury. The amount of blood that has accumulated can also be determined and the need for an operation can be assessed. Therapy then, except in the case of very limited injuries, usually consists of surgically exposing the testicle to clear out the accumulated blood and to seal the testicular membrane.
Pain in the testicle
A twisted testicle is a very painful experience for the man.
The pain caused by twisting the testicles is often very different and depends heavily on the cause or the age of the patient.
With a twisted testicle that has already formed in the womb, there is hardly any pain, the newborn behaves completely normally. However, if an infant continues to cry for no apparent reason, a pediatrician should do one Testicular torsion exclude.
Should the infant actually suffer from a twisted testicle, this can be done through Palpation of the testicle find out that a twisted testicle is often hard. A palpable finding can therefore give the first indications of congenital testicular torsion.
In toddlers, abdominal pain occurs when the testicle is twisted. These are of a diffuse character and cannot be precisely localized. It is not uncommon for side effects to occur. The children refuse to eat or vomit. In older children, adolescents or adults, accidents or other trauma are usually the cause of a twisted testicle.
The pain is then strongest, especially directly in the testicles, but accompanying pain can also occur here. The pain usually starts suddenly and very violently. Sometimes the patients also complain of abdominal pain, especially in the lower abdomen and the groin area.
It is precisely this abdominal pain that sometimes makes the patient feel sick or vomit. Pain in the kidney area can also occur.
The severity of the pain makes patients very pale and suffering from Racing heart and Sweats. Quite a few patients also pass out from the pain. In addition to the nature of the pain, the color and size of the testicle can also provide information about possible testicular twisting. If the testicle is red or bluish in color, swollen and painful, a doctor should be consulted. It is most likely a twisted testicle.
Causes of swollen testicles
Swelling of the testicle can have a number of possible causes. Basically, such a swelling can first be classified according to its character and course. It can appear suddenly and be very painful or develop slowly and be associated with little pain.
- If severe pain suddenly occurs, testicular torsion should always be considered, as this requires immediate therapy.
- If the swelling is related to trauma, a testicular rupture or a testicular hematoma could be a possible cause.
- Inflammation of the testicle or adjacent structures are usually accompanied by other symptoms such as reddening, swelling and overheating.
- If the swelling develops over a long period of time and is painless or painless, a water or testicle hernia, testicular varicose veins, cysts or tumors may be the reason.
In any case, a detailed diagnosis should be carried out by a doctor in order to avoid more serious illnesses and possible effects on fertility (Fertility) to be excluded.
For more information, see: Swollen testicles- what's behind it?
Causes of tingling testicles
Parasitic sensations such as tingling are generally very unspecific. Therefore, without further symptoms it is difficult to determine the cause of these sensations. Possible causes can be pathological processes in the testicles such as circulatory disorders, inflammation or tumors.
However, abnormal sensations such as tingling often indicate irritation of nerves. This can either affect the nerve endings directly on the testicles or the scrotum, but on the other hand it can also radiate from the back and the spine and pull along the nerve pathways into the testicles. It is therefore advisable to consult a doctor in the event of persistent symptoms in order to rule out possible pathological causes.
Is It Normal for the Testicles to Move?
It is completely normal for the testicles to move slightly within the scrotum. The movement is caused by the contraction of the cremaster muscle, also known as the testicle lifter. This consists of fibers of the abdominal muscles which continue downward in a loop and envelop the spermatic cord and part of the testicles. When the muscle contracts, the testicles are drawn towards the body. This mechanism is part of the body's temperature regulation and is used to ensure the optimal temperature for sperm production through the body heat, even in cold ambient temperatures.
In some boys and men, the kremaster muscle is inherently too pronounced. This can result in the testicle being pulled out of the scrotum into the groin when the muscle contracts. One then speaks of so-called pendulum testicles. As long as the testicle is in the scrotum for most of the time, this does not need to be corrected. If, on the other hand, the testicles are predominantly in the groin, surgical therapy should be considered. The high temperature to which the testicles are exposed within the body can otherwise lead to fertility problems.
Can testicles sweat?
Man's sperm production is a very temperature-sensitive process. The optimal range is 34-35 ° C. However, the testes themselves do not play a role in regulating temperature.
The scrotum in particular takes on the task of ensuring the optimum temperature. For this reason, there are many sweat glands in the skin of the scrotum. If the temperature is too high, e.g. due to tight clothing or a high ambient temperature, these are used to produce sweat and to release its heat to the outside through evaporation.
Testicular implant
A testicular implant or testicular prosthesis is an artificial replica of the testicle. They are used in reconstructive surgery, e.g. to restore aesthetics after the removal of a testicle in testicular cancer. They are also used in cosmetic surgery, e.g. to adjust the testicle size in the case of an existing testicular atrophy.
The implants are usually made of silicone to achieve a natural consistency and are available in different sizes. They serve purely optical purposes and, like breast implants, cannot take on any functional tasks.
Exclusion criteria for the insertion of a testicular implant are e.g. previous abscesses as well as permanent inflammations, cysts and pronounced damage to the tissue e.g. by X-rays.
You can find out more about this under: Testicular Implants - Why Are These So Popular? or Testicular prosthesis
What is a testicular bank?
A testicular bank is a special positioning pillow that is used to elevate the male genitals and testicles. This can be necessary, for example, in the event of inflammation of the testicles or after operations.
In addition, these pillows can be used to prevent contractures in the genital area of bedridden patients. In addition to these areas of application, the special positioning cushions are also suitable for micro-positioning in other areas of the body and, due to their small size, especially for use with children. The typical size is 20x20cm.
Palpate the testicle
Every man should palpate his testicles himself at regular intervals.
This is not just important for treating a sore testicle Testicular torsion to exclude, but also to recognize possible changes within the testicles. At Pain in the testiclesAs can happen with twisted testicles, palpation is often very uncomfortable.
Therefore, it is enough to raise the testicle a little. If the pain intensifies, one can assume that the testicle is twisted. In this case, see a doctor as soon as possible.
But even if there is no acute pain, the man should feel himself. Everyone can set their own time period, for example once a month. If you follow a fixed pattern during the self-examination, it becomes even easier to recognize possible changes. The testicle should first be examined for any external changes such as swelling or discoloration.
Then each testicle should be alternately picked up and compared with the other in terms of structure and size. However, many men naturally have two testicles of different sizes. A difference in size does not have to be due to illness. Then each testicle is palpated with the thumb and the other four fingers and gently pressed.
The male member is pushed to the side with one hand while the other hand is used to feel the testicle. When palpating is particularly on structural changes like node or Swelling to pay attention to. If you feel an irregularity in one or even both testicles or if you are not sure, then it is advisable to consult a doctor so that you can rule out serious diseases.
Recommendations from the editorial team:
You might also be interested in:
- Testicular pain
- Testicular cancer
- Testicular prosthesis
- Undescended testicles
- Inflammation of the testicles
- Water in the testicle