Pulmonary edema
Definition - what is pulmonary edema?
In the first place, pulmonary edema is, very simply, an accumulation of fluid in the lungs. The reasons for this are very different. However, among the most common are those
- Infection of the lungs,
- the heart failure
- as well as related renal insufficiency.
There are two different types of pulmonary edema:
The interstitial type, where the fluid is in the lung tissue, and the intra-alveolar type, where the fluid is in the cavities of the lungs, i.e. the small alveoli.

causes
There are numerous causes for the development of pulmonary edema. The most important are listed and explained below.
A very broad distinction is made between cardiogenic and non-cardiogenic pulmonary edema.
Cardiogenic pulmonary edema
In so-called “cardiogenic pulmonary edema”, the cause lies in the heart failure. The mechanism is as follows: By
- high blood pressure,
- a narrowing of the aortic valve
- or due to genetic defects
there is a chronic pressure load on the left ventricle. The chamber can initially compensate for this pressure load by causing the heart muscle to thicken. At some point, however, the load becomes so great that the chamber also dilates, i.e., to a certain extent, wears out. Then at the latest it can no longer work properly and thus no longer transports enough blood through the circulation. This causes the blood to accumulate in the sections of the vascular system in front of the left heart. This is the lungs. When blood backs up, high pressure builds up in the vascular system of the lungs, which forces fluid out of the lung capillaries into the lung tissue.
Non-cardiogenic pulmonary edema
The group of non-cardiogenic pulmonary edema includes all pulmonary edema whose cause is not related to the heart.
This includes the following causes:
Infections
If pneumonia occurs as a result of infection with bacteria or viruses, the entire lung tissue is irritated. If the pulmonary capillaries are damaged, they will leak. This creates holes in the vessels, so to speak, through which fluid can get into the tissue.
On the other hand, pulmonary edema can also cause infection. The accumulation of fluid in the tissue is the perfect breeding ground for germs, so that they can multiply particularly quickly and cause pneumonia. In a sense, this is a vicious circle, and for this reason pulmonary edema should be treated as quickly and effectively as possible.
Toxic
Certain substances that are toxic, ie “poisonous”, on the lungs can also trigger pulmonary edema. On the one hand, these substances include certain gases, such as smoke gas or chlorine gas, but excessive administration of oxygen can also cause toxic irritation of the lung tissue.
On the other hand, certain drugs can also be the culprit: Various antibiotics and chemotherapy drugs have lung-damaging properties.
By aspiration
“Aspiration” means, so to speak, the “swallowing” of liquids or food into the lungs. This often happens when the doctor has to intubate a patient who has not fasted, i.e. who has recently eaten. However, even in the event of a drowning trauma with fresh or salt water, liquid that does not belong there gets into the lungs. The lung tissue reacts very irritably and pulmonary edema quickly develops.
Oncotic pulmonary edema
Oncotic pulmonary edema is an accumulation of fluid in the lungs caused by a protein deficiency. In order for the liquid components of the blood to stay in the vessels, a certain amount of proteins must be present in the blood. These “attract” water, so to speak. If the blood does not contain enough proteins, the water escapes the vessels and quickly reaches the lung tissue, but theoretically all other tissues (leg edema, ascites etc.) as well.
There are two main causes of a protein deficiency in the blood: First of all, there is malnutrition. This also triggers a generalized protein deficiency in all tissues, which is also called “hunger edema”.
The second cause is liver failure. The liver is our central metabolic organ. In addition to numerous other tasks, it also produces the various proteins that circulate in the blood: Among other things, albumin, the central transport protein of the blood, the coagulation factors and so-called "acute phase proteins", which are mainly released during inflammation. If the liver is damaged due to hepatitis, chronic alcohol abuse or toxic causes, it can no longer perform its normal tasks, such as the production of proteins. There is also a protein deficiency here, and fluid escapes from the vascular system.
High elevation pulmonary edema
The high-altitude pulmonary edema arises from staying in high mountains, especially when climbing quickly. At over 3000m above sea level, the oxygen partial pressure in the air is significantly reduced. This means that you breathe in much less oxygen in one breath than you do at sea level. There is of course a lack of oxygen for normal body functions. The body tries to compensate for this by increasing the breathing rate. However, insufficient oxygen saturation also causes the pulmonary vessels to contract. This leads to increased pressure in the vessels, causing the capillaries to leak and allow fluid to escape into the tissue. To avoid this side effect of staying at high altitude, it is advisable to ascend slowly. This allows the body to get used to the new composition of the air and to adapt slowly so that pulmonary edema does not occur.
Pulmonary edema after pleural puncture
In the course of a pleural effusion, i.e. an accumulation of fluid in the lung membrane, it may be necessary to aspirate this liquid from the lung membrane through a puncture. If too much fluid is sucked out, pulmonary edema can develop as a reaction to the changing pressure conditions, which also affect the lungs. The negative pressure so to speak sucks the blood from the vessels into the alveoli. For this reason, it is advisable not to remove more than 1200ml of liquid at once.
Read more about it
For more detailed information, read our article: Causes of water in the lungs.
diagnosis
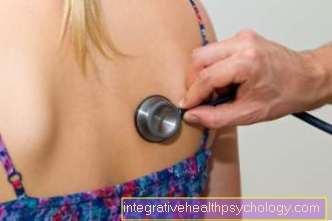
A clinical examination is part of the basic diagnosis of suspected pulmonary edema. On the one hand, this includes auscultation of the lungs, i.e. listening with a stethoscope. If there is liquid in the alveoli, you can hear a so-called wet rattling noise when breathing. Interstitial pulmonary edema is often inaudible.
In addition, it is noticeable during percussion, i.e. tapping the lungs, that the tapping sound is dampened by the accumulation of fluid. A healthy lungs are filled with air; in this case the knocking sound sounds to a certain extent hollow.
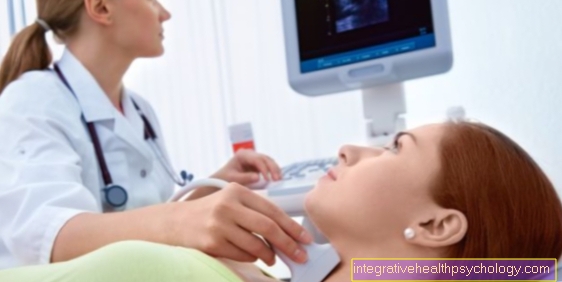
In addition, the pulmonary edema is made visible using imaging diagnostics, using the X-ray image.
What do you see in the x-ray?
It can be recognized by typical signs in an x-ray of the chest. These include:
-
the frosted glass shading, i.e. a diffuse, spotty drawing of the lung tissue,
-
perihilar shadows, i.e. whitish markings around the area of the lungs where the vessels enter and exit,
-
as well as the so-called "Kerley B-Lines", horizontal lines in the lung tissue.
Overall, the pulmonary edema appears as diffuse, white spots on the X-ray.
These stages exist
The course of pulmonary edema is divided into four stages.
- Stage 1: First, a "interstitial pulmonary edema”, This means that the water does not accumulate in the alveoli but within the lung tissue.
- Stage 2: In the second stage, the "alveolar pulmonary edema”, The water then also gets into the cavity of the lungs, ie the alveoli.
- Stage 3: In the third stage, so much fluid has already accumulated in the alveoli that it reaches the airways, the bronchi. A whitish foam then forms there, which can escape through the mouth when coughing.
- Stage 4: The last, most serious stage describes the life-threatening complication of the pulmonary edema, the so-called “asphyxia”. Asphyxia is the total respiratory and circulatory arrest caused by insufficient oxygen supply.
As has just been made clear, if left untreated, pulmonary edema can turn into a life-threatening emergency. For this reason, rapid diagnosis and immediate initiation of therapeutic measures is essential.
What symptoms do I use to recognize pulmonary edema?
There are specific physical symptoms that suggest pulmonary edema. Their severity depends on the stage of the pulmonary edema and is also variable from patient to patient.
The most common, important symptoms include:
-
The shortness of breath, also known as “dyspnea” in technical terms. The patient cannot breathe properly and accordingly suffers from a lack of oxygen, which he tries to compensate by breathing quickly.
-
An intensified, loud breathing noise can also occur. If the pulmonary edema was triggered by heart failure, these symptoms are also referred to as "cardiac asthma".
-
In the case of pulmonary edema, coughing occurs more frequently. This is due to the accumulation of fluid in the lungs, which triggers a persistent coughing urge to remove the fluid that hinders the exchange of oxygen from the alveoli.
-
The “sputum”, the mucus that is coughed up from the lungs, is often frothy or bloody. The color is aptly described as "flesh water-colored".
-
Racing heart.
-
Cyanosis, which is bluish discoloration of the skin, lips and tongue.
-
Inner unrest up to fear of death.
For a detailed explanation of the symptoms, see: These symptoms help you identify water in your lungs.
therapy
The following are to be used as immediate therapeutic measures:
-
First, the patient is seated and the legs are lowered in order to lower the blood pressure in the pulmonary vessels and not to worsen the pulmonary edema.
-
The secretion is sucked off. Sedation may be necessary.
-
The oxygen supply is increased by giving additional oxygen through the nasogastric tube.
-
Supportive CPAP breathing, i.e. mechanical positive pressure ventilation, may also be required.
Depending on the cause of the pulmonary edema, you will then intervene causally to tackle the problem “at the root”.
-
If the cause of the pulmonary edema is heart failure, the heart function is supported to make it easier for the blood to pump. In doing so, antihypertensive drugs and dehydrating tablets, so-called “diuretics”, are given so that the general pressure in the blood vessels is reduced and the tendency for fluid to escape from the blood vessels is reduced.
-
Even with renal insufficiency, there is too much water in the vascular system. In this case, the patient has to go on dialysis in order to remove the water masses from his body from outside, so to speak.
-
In the case of toxic or allergic pulmonary edema, steroids are given to suppress the immune reaction.
Duration
Since pulmonary edema can have very different causes, as mentioned above, it is not possible to give a generalized duration of the illness. Since it is a symptom of an underlying disease, such as heart failure, the recovery time depends heavily on how quickly the underlying disease is successfully treated. The duration of a pulmonary edema thus varies between a few days and several weeks.
Is there a cure?
With regard to the healing of pulmonary edema, it is again true that the success of the therapy depends heavily on the pathological situation that triggered it. This is again about combating the cause of the pulmonary edema.
If it is caused by pneumonia, the condition generally improves as soon as antibiotic therapy begins to work. Once the pneumonia has been treated, the pulmonary edema usually also disappears.
In the case of pulmonary edema caused by heart failure, the heart function must be strengthened or, if necessary, the heart must be relieved with medication. The primary goal is to lower the body's water content. Dehydrating drugs, so-called diuretics, remove water from the body so that pulmonary edema can also improve quickly.
If the pulmonary edema is due to chemotherapy drug use in cancer, it is only logical that it will not go away until chemotherapy drug therapy is in place. It is then, so to speak, an undesirable side effect of the therapy, which is accepted because of the cancer.
Life expectancy with pulmonary edema - what is the course?
First of all, it should be said that pulmonary edema is usually not the reason for a person's death, but rather the underlying disease that is also the cause of the edema.
If pulmonary edema is adequately treated or the causes for it eliminated, nobody will die of pulmonary edema. However, if it is not treated and the edema progresses to stage 4, it can lead to cardiovascular arrest, which is life-threatening.
The pulmonary edema is also a good breeding ground for bacteria that can cause pneumonia. Pneumonia is a life-threatening disease which, in the worst case, can lead to death, especially in the elderly, sick and weak.
Overall, it can be said that the severity and consequences of the pulmonary edema are extremely variable and the patient's condition must be considered in the individual case and depending on the previous illnesses.
Also read our article: Life expectancy with water in the lungs.