Sacral fracture
introduction
A sacral fracture is the bony break of the sacrum, which is also called the sacrum. Isolated sacral fractures are rare (approx. 10% of cases). Much more often they arise as a result of severe trauma in combination with other injuries.
Sacral fractures belong to the pelvic fractures and usually arise in the context of a severe injury (multiple trauma) due to a fall from a great height, a high-speed trauma in a traffic accident, in the event of a spill or trapping. In these cases, a sacral fracture is usually combined with other serious injuries, such as internal bleeding, other bone fractures or pelvic floor injuries. But even without the serious accompanying injuries, sacral fractures can lead to severe instability of the spine and its consequences. This is because the entire trunk load from the spine is initially only borne by the sacrum, which then distributes it further to the pelvis and thighs.

Causes of a sacral fracture
Sacral fractures usually arise as part of a fall from a great height, which leads to a direct fall Force acting on the sacrum comes. However, a sacral fracture can also arise as a result of indirect violence, for example through the leverage of the thighbone (femur) or through the transmission of the force along the leg. This is one example High speed traumas an important role.
osteoporosis
Both the frequency of osteoporosis-related sacral fractures and their clinical significance are increasing.
The reason for this, in addition to the aging population, is demographic change. So it happens that even the smallest injuries and accidents lead to sacral fractures more and more frequently, as the bony structures are weakened and less resistant. These osteoporotic fractures require separate assessment and therapeutic care.
A relevant aspect for surgical care is that in the case of an existing osteoporosis, the osteosynthesis material that has been introduced must also be fixed in the pelvis. It can also be useful to fill the screw material with cement to ensure better stability.
You may also be interested in the following topics:
- Therapy of osteoporosis
- Active against osteoporosis
Appointment with ?

I would be happy to advise you!
Who am I?
My name is I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
In order to be able to treat successfully in orthopedics, a thorough examination, diagnosis and a medical history are required.
In our very economic world in particular, there is too little time to thoroughly grasp the complex diseases of orthopedics and thus initiate targeted treatment.
I don't want to join the ranks of "quick knife pullers".
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You will find me:
- - orthopedic surgeons
14
You can make an appointment here.
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
For more information about myself, see - Orthopedists.
Classification according to Tile and Denis
Basically, the Sacral fracture according to Denis classified, however - because they are to the Pelvic injuries belongs to - also according to the general criteria Pelvic ring injury to be grouped.
Pelvic ring injuries after Tile classified and differentiate the severity of pelvic instability.
- Type-A-Fractures include this stable fractures, in which despite small bony tears still a intact pelvic ring is located.
- Type B- Describe fractures partially unstable pelvic fracturesbecause they have a partial tear in the posterior pelvic ring.
- Type-C Describe fractures completely unstable fractures, because with them the rear pelvic ring completely broken is. 45% of these C-fractures are sacral fractures.
The classification after Denis gives information about the Stability of the sacrum yourself and about eventual accompanying nerve injuries. These nerve injuries are more likely, the more central (medial) the fracture of the tailbone is.
- Type 1- Denis's fractures are also referred to and described as transalar sacral fractures lateral fractures of the sacrumthat are located between the sacrum and the iliac vane (Ala).
- Type 2 includes Fractures of the sacrum, the through the little holes (Foramina sacralia ant. Et post.) Go.
- Type 3 according to Denis includes all transverse, as well as all centrali.e. towards the middle of the body located, fractures. These types of sacral fractures go with a high rate Risk for accompanying Nerve damage hand in hand.
Symptoms
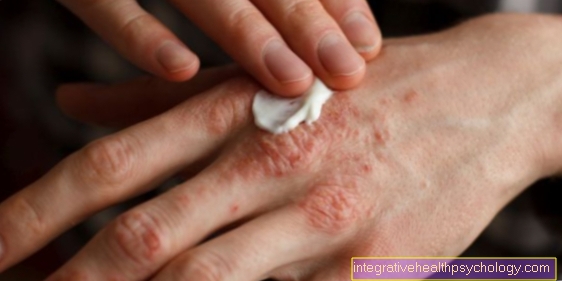
A typical symptom of a sacral fracture is the severe pain in the sacrum area, which increases especially when sitting. Often there are hematomas around the sacrum, it is sensitive to tenderness and small blood drains around the anal region.
If nerves are also affected as part of the sacrum fractures, this can lead to sensory disturbances and motor failures in the genitals, buttocks and inner thighs (so-called "breeches anesthesia"). In severe cases, this could be accompanied by fecal and urinary incontinence and erectile dysfunction. Since a sacral fracture is often combined with a pelvic ring fracture, loss of gait and soft tissue injuries can also be a consequence and symptom
Diagnosis
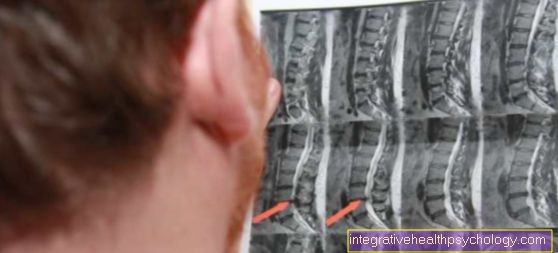
The diagnosis of a sacral fracture includes a complete medical history, which provides information about the mechanism of the injury and existing symptoms. Often this information is sufficient to arrive at the correct diagnosis. In spite of everything, a clinical examination and an x-ray of the pelvis in 2 planes (pelvic overview and pelvic oblique view) should always be carried out to confirm the diagnosis. In addition, a CT (computer tomography) can be performed in order to better localize the fracture and to identify any accompanying injuries.
During the clinical examination, it is particularly important to pay attention to any motor or sensory deficits, as well as to ascertain the vascular status (feel pulses of the legs and feet!). In this way, possible vascular and nerve injuries can be detected early and serious consequences can be avoided.
therapy
A non-dislocated, i.e. not dislocated sacral fracture can in most cases be conservative, i.e. treated without surgery. First of all, bed rest is adhered to for 3-4 weeks, followed by a slow build-up of the load with crutches.
To avoid secondary dislocations (slipping of the fractions), regular follow-up checks should be undertaken. Surgical stabilization should always be used in the case of severe (i.e. fractures associated with vascular or nerve injuries), unstable or displaced fractures of the sacrum. This is usually done with the help of a plate fixation or a screw connection
Surgical treatment of the fracture
Surgical repair of the sacral fracture is only carried out in the case of a dislocated or unstable fracture, whereas simple and non-dislocated fractures can be treated conservatively (non-surgically).
Various osteosyntheses are available for surgical treatment. These include the angular stable implants, plate and screw osteosyntheses. Depending on the fracture, the lower part of the spine or the pelvis must also be supplied with the osteosynthesis material during the operation. Stabilizing the rear pelvic ring is particularly important, which enables early mobilization and functionality. In addition, if necessary, surgical decompression, i.e. relief of nerve and vascular structures, should be carried out.
physical therapy
Physiotherapy plays a role both in the conservative and in the operative care of sacral fractures.
It ensures that the affected person remains mobile under controlled conditions, despite being immobilized and taking care of himself. With the help of a physiotherapist, those affected learn how to use the crutches correctly in order to only expose the sacrum to a partial load at the beginning. In addition, as part of physiotherapy, muscle building training takes place, as the muscular apparatus of the hips and legs has often noticeably regressed due to bed rest and rest.
forecast
The prognosis of a sacral fracture always depends on the severity of the injury and any accompanying injuries. If a sacral fracture occurs in isolation, it has good healing tendencies.
Duration
The exact duration of the sacrum fracture depends heavily on the type of injury and the accompanying injuries.
In the case of purely conservative sacral fractures, partial weight bearing with crutches should be possible again from about 4 weeks. The healing process of more complicated and surgically treated fractures is usually a bit more tedious. A full load may only take place after 6-12 weeks. In addition, after the sacrum fracture has healed, the implants must be removed. This usually takes place after about half a year. Overall, a fracture of the sacrum is an injury that takes weeks to months to heal and requires patient waiting and cooperative cooperation with regard to the therapy of the person concerned.
Anatomy of the sacrum
The sacrum or also called the sacrum is a wedge-shaped bone, of the consists of 5 fused vertebrae and forms the back of the bony pelvis. On the anterior and posterior side of the sacrum there are 4 paired angled holes, which are called Sacral foramina anterior (= front) and posterior (= rear). The pelvic blades adjoin the sacrum at the side, the sacrum goes down into it coccyx over.