Vaginal infection
definition
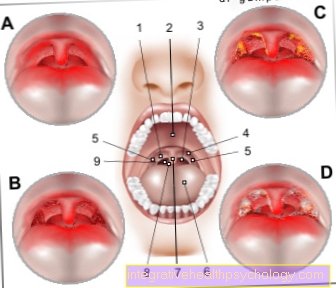
A vaginal infection is the pathological entry of various microorganisms into the vagina and a disease triggered by it. There are various microorganisms, or pathogens, that can cause a vaginal infection. A distinction is made between bacterial, viral and fungal infections of the vagina and infections caused by other microorganisms (protozoa). A vaginal infection that also affects the vulva and labia is also known as vulvovaginitis.

causes
The causes of a vaginal infection are very diverse. Whenever the natural vaginal flora is attacked or not intact, the conditions for germs and pathogens to penetrate the tissue are given.This is the case, for example, with people with chronic diseases such as diabetes or skin diseases such as neurodermatitis. Excessive or inadequate intimate hygiene can also be the cause of a vaginal infection. Aggressive washing lotions change the acidic pH value of the vagina and thus enable the body's own - actually harmless - fungi to cause an infection. Even after antibiotic therapy, the acidic vaginal environment can be affected. Fungal infections caused by the yeast Candida albicans tend to develop in such cases. Such an imbalance also causes bacterial infestation of the vagina.
The body's own lactic acid bacteria in the vagina can be attacked by various factors, such as increased hygiene. This changes the pH of the vagina and leads to an overgrowth of other bacteria in the vagina. Usually it is the pathogen Gardnerella vaginalis. Frequent sexual intercourse, antibiotic therapy and a hormonal imbalance, for example a lack of estrogen, favor the occurrence of the bacterial infection. There are also numerous other pathogens that can cause a bacterial infection of the vagina. Examples of this are chlamydia or Neisseria gonorrhoeae, a pathogen that causes the disease gonorrhea (gonorrhea). These pathogens are usually transmitted through sexual intercourse. The so-called trichomonas colpitis is also caused by transmission during sexual intercourse. Trichomonads are tiny microorganisms that typically cause foamy, greenish discharge.
You can find out more about the topic here sexually transmitted diseases.
Bacterial causes
The most common bacterial infection of the vagina is bacterial vaginosis. In contrast to a respiratory tract infection, for example, in which the pathogen is transmitted from person to person, bacterial vaginosis is caused by an imbalance in the vaginal flora. There are naturally many lactic acid bacteria, also known as Döderlein bacteria, in the vagina, which ensure an acidic pH value to protect the vagina. If this Döderlein flora is attacked, for example through excessive intimate hygiene, other germs can colonize the vagina. Mostly it is the germ Gardnerella vaginalis. Bacterial vaginosis is characterized by a thin discharge that has an unpleasant fishy odor. Symptoms can be completely absent. When bacterial vaginosis causes symptoms, they can vary widely. Itching, a burning sensation in the vagina, and a burning sensation when urinating are possible.
However, bacterial infection of the vagina can also result from the transmission of bacteria. Usually this happens during sexual intercourse. Typical pathogens are chlamydia or gonococci.
mushroom
A fungal infection of the vagina is also known as candida vulvovaginitis. It is a common infection that almost every woman experiences at some point in her life. The fungus that causes vaginal thrush is the yeast Candida albicans. In small quantities, it colonizes the vagina and does not cause infection. However, if the vaginal flora is attacked, it can multiply and displace other important microorganisms. Then the typical symptoms of vaginal fungus develop, namely itching, whitish discharge and burning sensation in the vagina. Women who suffer from diabetes mellitus, are pregnant, have HIV or another disease that attacks the immune system, have increased vaginal thrush. Vaginal fungus can also occur after antibiotic therapy. Incorrect intimate hygiene can also unbalance the vaginal flora and thus promote a fungal infection.
Read more on the topic: What drugs are there for vaginal thrush? or yeast in the vagina
A vaginal infection after taking antibiotics
Antibiotic therapy can cause the vaginal flora to be attacked. An undesirable side effect of antibiotic therapy is that "good bacteria", i.e. those that are naturally found in the body, are also attacked. These include the important lactic acid bacteria in the vagina. They ensure an acidic pH value that protects the vagina from invading microorganisms and pathogens. If the number of lactic acid bacteria is reduced, the pH value rises and other germs can settle and multiply. Therefore, fungal infections and bacterial vaginosis can develop after antibiotic therapy.
Viruses
Viruses can also cause vaginal infections. A common pathogen is genital herpes, which is sexually transmitted. The virus that causes this clinical picture is the herpes simplex virus, which is also responsible for the occurrence of cold sores. An infection manifests itself as redness and swelling of the genital region, a feeling of tension, itching and burning. The initial infection, when the virus first enters the body, is asymptomatic. The virus stays in the body for a lifetime, but only triggers symptoms through the presence of certain trigger factors, such as stress or a weakened immune system.
Symptoms
A vaginal infection is characterized by various, characteristic symptoms. Fungal infections usually manifest themselves as severe vaginal itching and a burning pain at the entrance to the vagina, which is especially aggravated by sexual intercourse. There is also a crumbly, white discharge.
Bacterial vaginosis, on the other hand, is often symptom-free and is only noticeable through a changed discharge. This is very thin and has an unpleasant, fishy odor. In some cases, symptoms such as a burning sensation in the vagina, itching or a burning sensation when urinating may also occur.
Here is the main article Vagina burns.
Gonorrhea is also often symptom-free. It also rarely causes discomfort to the vagina, but rather settles in the internal reproductive organs, such as the ovaries and the uterus. As a result, common symptoms are more likely to be stomach pain, fever or nausea.
A chlamydial infection, on the other hand, causes urination discomfort, such as burning pain, and can also lead to abdominal pain. An infection with trichomonads manifests itself as reddening of the vulva and the labia, severe itching and the formation of blisters on the vagina. Burning vaginal pain and painful urination are also typical. When infected with trichomonads, the discharge is yellowish-green, has an unpleasant smell and is characterized by foam formation.
Discharge from a vaginal infection
Many vaginal infections change the natural discharge of the vagina. This is very impressive, for example, with a fungal infection. The otherwise milky-whitish discharge is thickened with a fungal infection, white and has a crumbly consistency. Other infections are also characterized by typical changes in the discharge. A trichomonad infection, for example, is characterized by a foamy, greenish discharge. The common bacterial vaginosis, on the other hand, leads to a thin discharge with an unpleasant, fishy odor. A purulent and bloody discharge can be found with an infection with the sexually transmitted chlamydia. However, this discharge does not leave the vagina, but is found on the cervix. The gynecologist can see this during the vaginal examination. It is the same with gonorrhea. Here, too, there is a purulent discharge on the cervix.
Learn more about this under: Discharge from the vagina
diagnosis
At the beginning of the examination, the gynecologist asks a few questions in order to narrow down the cause of the infection. The questions relate to symptoms such as vaginal burning, itching, discharge, or pain. Furthermore, the question of unprotected sexual intercourse or changing sexual partners, as well as symptoms in the partner, is very important in order to be able to diagnose sexually transmitted diseases, for example. This is followed by the physical examination, during which the gynecologist looks at the vagina and can determine changes such as redness, swelling and discharge. A smear can be taken to determine the pathogen. Cultivation is necessary for bacteria that cannot be seen under the microscope. However, this examination takes several days to weeks. The quick pH measurement using a test strip is an indication of a disturbed vaginal flora, which is typical for a fungal infection or bacterial vaginosis.
Is there a test for a vaginal infection?
Various examinations and tests are available to diagnose a vaginal infection. A very important test done by a gynecologist is the amine test. This test is done if bacterial vaginosis is suspected. The gynecologist first takes a swab from the vagina and then drizzles the swab material with 100% potassium hydroxide solution. The lye causes the typical, fishy odor of the discharge in bacterial vaginosis to intensify.
Another important test when diagnosing a vaginal infection is pH measurement. With the help of a test strip that is streaked along the inside wall of the vagina, the pH value is measured on the basis of the color change. An increased pH value indicates an imbalance in the natural vaginal flora and is typical of vaginal infections. A pH test can also be purchased from the pharmacy as a self-test for home use. One example of this is the Canestest® product. The pH measurements only provide information about the change in the pH value of the vagina and cannot determine the type of infection.
There are also various questionnaires that can be carried out as a self-test at home. Based on various questions regarding the symptoms, antibiotic therapy, sexual behavior and the like, it can be determined whether a vaginal infection is likely.
treatment
There are several aspects to treating a vaginal infection. On the one hand, combating pathogens is the focus of the treatment, on the other hand, the restoration of the healthy vaginal flora is of great importance. A vaginal thrush is treated with an active ingredient that attacks the fungus. The common antifungal drug of choice is clotrimazole. It is used as a vaginal cream or suppository for local therapy. In the case of a stubborn fungus, tablets that contain the active ingredients itraconazole or fluconazole are used (see also: Antifungal medication). After the fungal infection, it is important to restore the vaginal flora with the help of lactic acid bacteria and vitamin C tablets. This therapy is usually done with the help of vaginal suppositories. Bacterial vaginosis or other bacterial infections are treated with antibiotic agents. For some infections, it may be necessary to have your partner treat you as well.
Home remedies for vaginal infection
If you have a vaginal infection, you should avoid using home remedies. Although home remedies such as vinegar rinses, lemon rinses or chamomile seat baths can often be found, we can only advise against them at this point. They can additionally irritate the vaginal flora and, in the worst case, lead to inflammation or allergic reactions. If you have a vaginal infection, only medical treatment can help. In addition, one should pay attention to the correct intimate hygiene in order not to delay the healing.
Medication for a vaginal infection
Various medications are available to treat a vaginal infection. Fungal infections of the vagina are treated with something called an antifungal drug. Antimycotics are active ingredients that target fungi and either disrupt or kill their growth. A common antifungal agent used to treat vaginal thrush is clotrimazole. As a vaginal ointment or vaginal suppository, it is used for local treatment. For stubborn vaginal fungus, antifungal drugs are also swallowed in the form of tablets. The active ingredients fluconazole and itraconazole are suitable for such a systemic therapy.
Bacterial vaginosis, on the other hand, is treated with antibiotics. The active ingredients metronidazole and clindamycin are preferably used. Other bacterial infections, such as gonorrhea, trichomonas or chlamydial infections, are also treated with antibiotic agents. The active ingredient metronidazole is also suitable for the treatment of trichomonads. Gonorrhea is treated with a single syringe containing the active ingredient ceftriaxone. The infection with chlamydia is treated with the active ingredient doxycycline.
Viral vaginal infections are also less common. Genital herpes in particular plays an important role here. Since genital herpes can be very painful, pain relievers such as ibuprofen and paracetamol are used to treat it. To fight the herpes viruses, you still need an antiviral agent. This is usually the active ingredient acyclovir. The active ingredients famciclovir and valaciclovir are an alternative.
Homeopathy for a vaginal infection
In homeopathy, too, there are various, but not uniform, recommendations for the treatment of a vaginal infection. However, the recommendations usually only apply to non-contagious infections, such as bacterial vaginosis or vaginal thrush. Infectious infections such as gonorrhea, chlamydia or trichomoniasis should be treated immediately by a doctor, otherwise they can be passed on to sexual partners. However, nothing speaks against supportive treatment with homeopathic remedies for bacterial vaginosis or vaginal thrush.
Nevertheless, the treatment should be clarified by a doctor, as recurring infections can also hide other diseases that require treatment. In particular, the agents sodium muriaticum 15C, Carbonicum acidum 15C or Kreosotum 15C are often recommended. The remedy sodium muciaticum is, according to recommendations, suitable for a strongly burning discharge. Carbonicum acidum is recommended for discharge with a fishy odor and back pain. A yellowish, unpleasant smelling discharge with itching, on the other hand, should be treated with Kreosotum. Other homeopathic remedies that are also used in the treatment of vaginal infections are Sepia, Graphites, Pulsatilla, Nitricum acidum, Mercurius solubilis, Hydrastis, Lilium tigrinum and Arsenicum album.
Duration
The duration of a vaginal infection depends on a number of factors. Many vaginal infections can be treated very quickly and easily. Vaginal thrush are usually symptom-free within a few days under treatment. Without treatment, however, the symptoms can last for weeks or even months. It is similar with bacterial vaginosis. This can take several months without treatment and go unnoticed as it does not always cause symptoms. Bacterial infections such as gonorrhea or chlamydia must also be treated in order to heal. An infection with chlamydia requires a relatively long antibiotic therapy. Therapy can last between 7 and 20 days. However, the symptoms subside within a few days of therapy.
How can you prevent a vaginal infection?
There are a few things you can do yourself to prevent a vaginal infection. Important aspects of prevention primarily concern the vaginal flora. The most common vaginal infections are not caused by a transmissible germ, but by an imbalance in the healthy vaginal flora. Excessive intimate hygiene is a common problem in this regard. Aggressive washing lotions and shower gels attack the acidic pH value of the vagina and promote infections. The intimate area should therefore be cared for with clear water or a special intimate lotion that has an acidic pH value. However, clear water is absolutely sufficient for the care of the intimate area. The vagina should only be washed by hand and not with a washcloth, as this forms the perfect breeding ground for germs.
The use of intimate deodorants, intimate powders or similar care products should be avoided as they unbalance the vaginal flora. To clean the intimate area, you should use fresh towels and wash them at 60 ° C to kill germs. The vaginal flora can also be accommodated when choosing underwear. Cotton underwear is preferable to synthetic underwear, as it can be washed at higher temperatures. After an infection, it is advisable to restore the vaginal flora with a lactic acid treatment. Sexually transmitted germs can be prevented by using condoms.
Vaginal Infection During Pregnancy - How Dangerous Is It?
Infections of all kinds are particularly feared during pregnancy, as some can endanger the integrity of the child. Some vaginal infections can also negatively affect pregnancy and should therefore be treated. The common fungal infection is not one of them. It is harmless in nature and does not endanger pregnancy. Nevertheless, it should be treated as it is extremely bothersome and attacks the vaginal flora. Bacterial vaginosis, on the other hand, must be treated in any case, as it has been shown to be associated with premature birth.
Untreated gonorrhea can lead to a conjunctival infection in the newborn known as gonococcal conjunctivitis. Chlamydia or herpes viruses can also cause such inflammation in the eyes. However, these infections only pose a problem at birth, as the pathogen can then be transmitted to the child. The infections are treated as part of the preventive check-ups so that such a course can be prevented. A vaginal infection does not pose a direct risk to pregnancy or early pregnancy in the sense of a miscarriage or developmental disorder of the child.
How contagious is a vaginal infection?
A vaginal infection is usually based on an imbalance in the natural vaginal flora. This allows germs to multiply that would otherwise colonize the vagina in lower numbers. Such infections are usually not contagious. However, if you have repeated vaginal thrush or bacterial vaginosis, your partner should also be examined. If necessary, there are also germs in the partner that must be treated as well. Infections with other germs, such as genital herpes, chlamydia, gonorrhea or trichomonads, on the other hand, can be transmitted through sexual intercourse. Only the use of condoms can prevent transmission.
Can you vaccinate against a vaginal infection?
You cannot vaccinate against vaginal infections in general. For several years there has been a vaccination against various strains of the human papilloma virus - HPV virus for short. This vaccination, often called the cervical cancer vaccination, protects against infection with different strains of the HPV virus. A vaccination effectively prevents the development of cervical cancer in women who are not yet infected and is therefore recommended by the Standing Vaccination Commission (STIKO). It should be completed before the first sexual intercourse, as the likelihood of an infection increases afterwards.