Waterhouse Friedrichsen Syndrome
Synonyms
Adrenal apoplexy (failure of the Adrenal glands due to bleeding or vascular occlusion), suprarenal apoplexy
Definition and introduction
The Waterhouse-Friedrichsen Syndrome is one State of shock through toxins (bacterial poisons)that are produced by the bacteria.
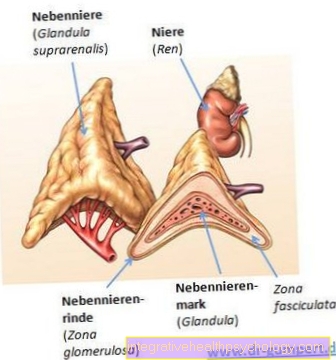
There is an extreme consumption of coagulation factors (consumption coagulopathy) and tissue death (hemorrhagic necrosis) of the adrenal cortex, usually as a result of a bacterial blood poisoning (Meningococcal sepsis).
Frequency distribution
A Waterhouse-Friedrichsen syndrome occurs in around 10 to 20% of patients with meningococcal sepsis.
The Mortality (Lethality) is very high and lies at up to 90%, despite treatment. If left untreated, the Waterhouse-Friedrichsen syndrome is always fatal.
The age peak is currently still in toddler age, but adolescents are now also more often affected, which indicates that the Number of new cases (Incidence) slowly to adulthood shifts towards.
causes
The Waterhouse-Friedrichsen Syndrome is caused by the massive distribution of Toxins from the causative bacteria evoked. These are mostly meningococci. Pneumococci and Haemophilus influenzea can also trigger this serious clinical picture.
The release of toxins leads to a massive activation of the coagulation factors in the blood.
So there are very many Thrombi which lead to the occlusion of the vessels, on the other hand, massive bleeding occurs due to the high consumption of coagulation factors in other areas. These occur in skin, Mucous membrane and internal organs.
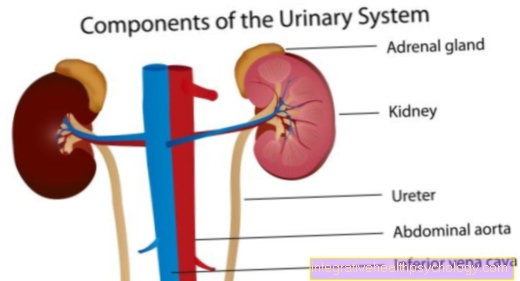
The patients come into one Shock situation and bleed to death. In addition, there is an endotoxin shock, which leads to functional restrictions in the liver, Kidneys and Adrenal glands and the Lungs leads.
Symptoms of Waterhouse Friedrichsen Syndrome
Clinically it comes with Waterhouse Friedrichsen Syndrome to massive bleeding into the skin, so-called. Petechiae.
Also kick Mucosal bleeding and intravital Death spots on. These are cold, livid areas of the skin where the blood has stagnated.
Furthermore, there are various signs of the Waterhouse Friedrichsen Syndrome Shocks. The Kidneys stop working, i.e. there is very little or no urine output. Besides, it comes to Shortness of breath, through the shock of the Lungs, and to one Yellowing of the patient, from shock liver.
Are the cerebral vessels of Thrombi relocated, neurological abnormalities occur. This includes cramps and Somnolence.
Important
Typically, these symptoms develop within a few hours.
diagnosis

The symptoms (clinical picture) are an important indicator, since the Waterhouse-Friedrichsen syndrome must be treated as quickly as possible.
Therefore, a combination of a large number of small bleeds on the skin (Petechiae), fever and diarrhea think of a Waterhouse-Friedrichsen syndrome.
in the blood the various coagulation and fibrinolysis tests are conspicuous, as all coagulation factors are massively consumed.
In addition, the number of white blood cells (leukocytes) and the Platelets.
therapy

The important thing is that antibiotic therapy to start as early as possible.
This is usually done Penicillin G and Cefotaxime utilized.
In addition, the State of shockshock of the patient are fought. This means that fluid must be supplied through the veins in order to compensate for a lack of volume.
In addition, ventilation must be provided, the acid-base balance and the electrolyte balance should be balanced.
If the massive bleeding is in the foreground, you can Platelet concentrates and Fresh plasma administered.
prophylaxis
There are no vaccination against the group of Meningococci, which are the most frequent cause of the Waterhouse-Friedrichsen syndrome and occur with us.
Against Pneumococci and Haemophilus influenzea can on the other hand be vaccinated. These are contained in the 6-fold vaccine, which can be given from the 3rd month of life.
Still be antibody against meningococci naturally formed in the course of life, which then protect against invasion and thus make the disease relatively rare.
Summary
Despite its rarity, the Waterhouse-Friedrichsen syndrome is a very dangerous clinical picture that is very often fatal even under intensive medical therapy.
Most important for the survival of the patient is a diagnosis as early as possible, to which an immediate intensive care unit and antibiotic treatment must connect.



.jpg)