How can you recognize a herniated disc?
introduction
Persistent back pain is one of the most common complaints that make it necessary to visit a family doctor. Most of the affected patients assume that this back pain is mostly related to a herniated disc.
Contrary to popular belief, a herniated disc is comparatively rarely the cause of back pain.

What are the symptoms of a herniated disc?
The most common symptoms of a ligament hernia include:
- Back pain depending on the severity of the incident
- Paralysis of the arms or legs
- Parasitic sensations in the arms or legs
In order to recognize a herniated disc, the affected patient must look out for other typical symptoms.
Above all, disturbances in sensory perception, such as numbness or tingling, can help to recognize a herniated disc as such.
In addition, prolonged compression of a nerve root can lead to pronounced impairment of motor skills.
Not sure what is causing your back pain? Find out more in our article:
- How do I distinguish a herniated disc from a lumbago?
In general, the earlier it is diagnosed, the better the prognosis for a herniated disc. Short-term nerve root compression usually leads to symptoms that subside completely after successful treatment. On the other hand, pronounced and / or long-term compressions of the nerve roots can lead to permanent complications.
Particularly in the case of a deep herniated disc in the lumbar spine, for example between the 5th lumbar vertebra and the 1st sacral spinal segment, disorders of bowel and bladder emptying are among the most feared complications.
Read more on this topic at:
- Symptoms of a herniated disc
and - Diagnosing a herniated disc.
Sensory disturbances and tingling sensations
Furthermore, a herniated disc can often be recognized during the doctor-patient conversation because the affected patients are pronounced Sensory disturbances specify. These sensory disturbances can take the form of Numbness and / or tingling sensation occur. Their location also allows conclusions to be drawn about the impaired spine segment.
Also one subjective reduction in muscle strength can help the doctor treating you to recognize a herniated disc as such.
- Does a tingling sensation indicate a herniated disc?
or - Is numbness an indication of a herniated disc?
Appointment with a specialist for a herniated disc?

I would be happy to advise you!
Who am I?
My name is I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
A herniated disc is difficult to treat. On the one hand it is exposed to high mechanical loads, on the other hand it has great mobility.
Therefore, treating a herniated disc requires a lot of experience.
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You can find me in:
- - your orthopedic surgeon
14
Directly to the online appointment arrangement
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
Further information about myself can be found at
How can you recognize a herniated disc yourself?
It is often difficult to recognize a herniated disc yourself. Most people assume that persistent back pain is inevitably related to a herniated disc.
In general, however, it can be assumed that the herniated disc is a comparatively rare cause of persistent back pain. Much more often, such complaints are caused by muscular tension.
Affected people cannot recognize a herniated disc by the fact that they are suffering from back pain. Nevertheless, pain in the area of the affected spinal column segment can provide an initial indication of a disease.
However, with a herniated disc, pain is typically not confined to the back. In the case of intervertebral disc prolapse of the cervical spine, the symptoms radiate from the neck to the arms.
Those affected can recognize a herniated disc in the thoracic spine by the fact that the pain radiates from the middle back in a belt-shaped manner along the ribs.
A herniated disc in the lumbar spine, on the other hand, is usually indicated by the radiation of pain into the buttocks and / or legs.
Find out more about the Disc herniation pain.
In addition to the pain, however, other symptoms can help identify a herniated disc for itself. Above all sensory disturbances in the form of numbness and / or tingling are typical signs of a herniated disc. In addition, the sustained compression of the nerve roots can lead to a significant decrease in the muscle strength of the respective key muscles.
Functional tests for a herniated disc
An orientating neurological examination should be carried out after the doctor-patient discussion. During this examination, the specialist can determine whether and which nerve root is being constricted. To check the sensitive nerve pathways, the extremities must be coated. This special examination must always be carried out in side-by-side comparison. If there is a deviation in the sensation on both sides, nerve damage can be assumed.
In the following, muscle strength should be the most important Identification muscles (Muscles that can be assigned to a segment of the spine). A herniated disc in particular, which is already very advanced and / or has existed for a longer period of time, can often be recognized in this way.
In addition, possible nerve root compression can be determined through a simple test. The so-called Lasègue test the patient is placed on his back. The specialist then begins to slowly bend the patient's extended leg in the hip joint. This test must be assessed as positive if the patient experiences pain in the lumbar spine when lifting the extended leg.
The classic tests of nerve root compression must be considered positive if pain is induced during passive movement.
A positive one Lasègue sign does not necessarily have to indicate a herniated disc. The Lasègue test is also typically positive for inflammatory processes in the area of the meninges (so-called meningitis).
However, if the symptoms indicate a herniated disc in the lumbar spine, the Lasègue test can help to identify the prolapse as such.
In addition, if a herniated disc is suspected, the diagnosis includes various exercises. These exercises specifically test the functionality of the Identification muscles of the most important spinal segments. In patients who can easily walk on their toes and heels, paralysis of these key muscles can be excluded.
Read more on this topic at: Functional test for a herniated disc.
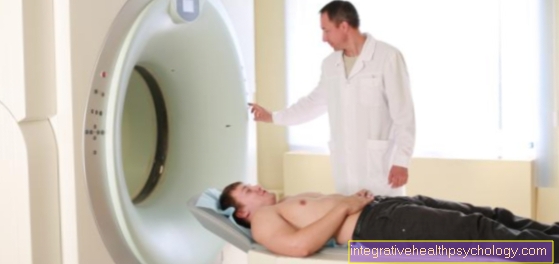
What imaging procedures are there?
If the suspicion of a herniated disc is confirmed during the physical examination, further diagnostic measures must be initiated. Only imaging procedures that are suitable for mapping the spine and the intervertebral discs can help to identify the herniated disc unequivocally as such and thus to substantiate the suspected diagnosis.
However, taking ordinary x-rays is not very helpful in diagnosing a herniated disc. A computer (CT) or magnetic resonance tomography (MRT) scan must therefore be performed to detect a herniated disc. Due to the fact that the intervertebral discs can be better visualized, magnetic resonance tomography is the first choice in the diagnosis of a herniated disc.
In addition, nerve conductivity and muscle strength can be checked using special tests. So-called electromyography (EMG) in particular can help to identify whether there are sensory disorders and signs of paralysis. Electronurography too (CLOSELY) is considered a suitable method in diagnosing a herniated disc.
MRI for a herniated disc
Imaging procedures are considered the only way to unequivocally identify a herniated disc, but they do not necessarily have to be carried out even if a disc prolapse is suspected.
Especially in the case of less pronounced complaints, images of the spine are often not taken. However, imaging procedures cannot be dispensed with in a patient who already suffers from sensitivity disorders and muscle strength limitations.
Conventional X-rays do not play a role in the detection of a herniated disc. The reason for this is the fact that only bony structures can be assessed in an ordinary X-ray. Individual nerve roots and the intervertebral disc cannot be mapped in this way.
For this reason, a herniated disc is recognized primarily by magnetic resonance imaging (MRI). The MRI can show bony structures of the spine as well as nerve roots and intervertebral discs.
Due to the fact that the production of an MRI does not result in any radiation exposure on the patient, the detection of a herniated disc by MRI is the diagnostic method of first choice.
In principle, the relevant structures can also be represented by computed tomography (CT). During this examination process, however, the patient is exposed to comparatively high doses of radiation.
Read more on this topic at: MRI for a herniated disc
X-ray for a herniated disc
A herniated disc as such cannot be diagnosed by X-rays. The detection of a herniated disc only through X-rays is still not possible for several reasons.
Although the spine can be perfectly visualized with conventional X-rays, the ability to assess the individual spine segments is limited to the bony structures.
Neither the nerve roots nor the intervertebral disc itself can be visualized by conventional X-rays.
To recognize a herniated disc, however, all structures of the individual spinal column segments must be assessed. For this reason, magnetic resonance imaging is the first choice in diagnosing a herniated disc. In this context, however, it must be noted that herniated discs in the thoracic spine (thoracic spine) are often related to a previous trauma.
In these cases, the X-ray can at least help to identify whether there is a possible fracture in the area of the bony spinal structures.