Stye
Synonyms
Medical: hordeolum
English: hordeolum, sty
definition
A hordeolum (stye) is an acute bacterial inflammation of a lid gland. If several glands are affected at the same time, one speaks of a hordeolosis (several grains of barley).
For general information on the subject of "inflammation of the eye" please also read: Inflammation of the eye

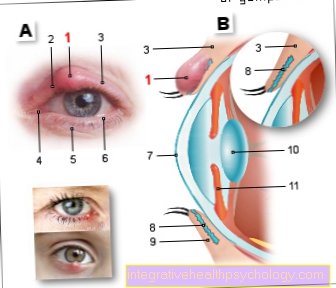
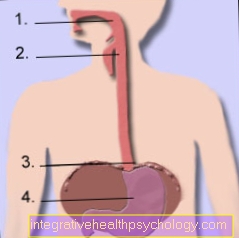
Stye
(Suppuration of a
Eyelash gland)
- Stye -
Hordeolum - Eyelashes (cilia) -
Cilia - Upper eyelid -
Palpebrae superior - Tears -
Caruncula lacrimalis - Lower eyelid -
Inferior palpebrae - Conjunctiva -
Tunica conjunctiva - Cornea -
Cornea - Eyelash gland -
Glandulae sudoriferae
palpebrales - Eye lens -
Lens - Iris -
iris
You can find an overview of all images from Dr-Gumpert under: medical images

Detecting a stye
What are the symptoms of a stye?
The barley grain (hordeolum) is characterized by:
- severe pain in the affected area
- Swelling and
- a strong redness.
- Pus in the eye
Usually there is a central point of pus. The inner stye usually shows more severe accompanying symptoms (e.g. conjunctivitis) than the hordeolum externum.
Read more on the topic: Eye pain
How is a stye diagnosed?
A hordeolum externum (external stye) can usually be diagnosed very quickly due to its location on the outer edge of the eyelid.
The stye is usually diagnosed by what is known as a visual diagnosis, so the doctor knows what problem he is dealing with just by looking at it once.
The hordeolum internum (inner stye), however, is only discovered when ectropioning (folding the song outwards so that the inner conjunctiva becomes visible).
The hailstone (chalazion), which is insensitive to pressure pain (pressure indolent), is the differential diagnosis (which disease is still in question?). For more information on this topic, see: Hailstone.
Inflammation of the lacrimal gland must also be ruled out.
Treating a stye
How is a stye treated?
As a rule, a stye heals spontaneously and without problems.
Various measures can be taken to support the healing process.
Further information is available from: How do you treat a stye?
Is a stye treated conservatively?
In the acute stage, dry warmth (e.g. Red light exposure) cause a breakthrough of the pus or a more rapid encapsulation, and thus a faster healing of the stye. In general, care should be taken not to use your hands to transport the bacteria from the diseased to the healthy eye.
- Red light therapy
Red light or infrared light is also referred to as thermal radiation. In contrast to conventional white light, the long-wave red light rays penetrate deeper into the skin. They gently heat the underlying tissue without damaging the surface of the skin. The local metabolism is stimulated by the slowly rising temperatures in the irradiated region. The blood flow increases and the body's defense cells reach the inflammation faster.
It is not uncommon for the stye to break through the pus and the duration of the illness to be shortened! It is essential to keep your eyes closed during red light therapy. The resulting heat should be pleasant. As soon as a feeling of heat or even pain occurs, the treatment must be stopped immediately! In addition, the minimum distance of about 30 cm to the lamp must not be exceeded.
Precise information on operation and handling can be found in the manufacturer's instructions.
Red light lamps are offered for sale in pharmacies or medical supply stores.
- Compresses
Warm, dry compresses can also help.
However, it is important that no damp envelopes (e.g. Chamomile tea envelopes) be used.
Because the moist warmth would create an optimal breeding ground for the pathogens of the stye: the bacteria spread and further stye develop.
- Lid margin hygiene
The tear film of the human eye has a high fat content. In the case of a stye, the composition of the tear fluid is often disturbed because the fat-producing glands are inflamed. In order to restore the natural balance, eyelid hygiene after the stye has subsided can be helpful. One counts e.g. Lid rim massages, moisturizing eye drops or lid rim cleaning are among the possible measures.
Can a stye be treated surgically?
In the case of massive swelling of the eyelid and great pain caused by the pus in the stye, there is the possibility of a small operation to remedy the situation. To do this, the ophthalmologist opens the stye through a small incision (Incision) and the pus can drain away. Note: This incision, no matter how small, should definitely only be carried out by a doctor! Incorrect scarring can result in permanent disorders of the edge of the eyelid such as an ectropion.
Under no circumstances may the person concerned himself "Lend a handWhen trying to express the stye, similar to a pimple, germs get into the eye. Conjunctivitis and other stye can develop. The hands also come into contact with the pus and transport germs into the unaffected eye.
What drugs help with a stye?
In very rare individual cases it may be necessary to take antibiotics in tablet form. One then speaks of a so-called "systemic antibiosis": The drug does not have a purely local effect on the stye, such as eye ointments, but rather throughout the body. Floxal or Refobacin® are suitable for local antibiotic therapy.
The ingestion is indicated as soon as the inflammation threatens the eye socket (Orbit) to hike over.
Which eye ointments help with a stye?
For stye, eye ointment can aid the healing process. A distinction is made between antibiotic, disinfecting and homeopathic eye ointments. Without an ophthalmologist's advice, the over-the-counter ointments should only be used cautiously.
General application: Before using eye ointment, those affected should wash and dry their hands thoroughly. Contact lens wearers must remove their lenses! Then the cover of the tube is unscrewed and stored safely. Now it makes sense to put your head back slightly. With one hand, pull the lower lid of the affected eye down slightly. A cotton pad or handkerchief can be used to protect the sensitive skin around the eyes. The other hand exerts gentle pressure on the tube of ointment and thus applies a strand of ointment into the conjunctival sac. For reasons of hygiene, it is essential to ensure that the tip of the tube does not come into contact with the eye! After the end, those affected can slowly close and open their eyes.
Caution: Immediately after applying the ointment, eyesight is impaired: Therefore, may in the first few minutes no heavy machinery is operated or taken on the road! After a short time, however, the blurred vision disappears and visual acuity is restored.
- Antibiotic eye ointment
Antibiotic eye ointment kills stye pathogens due to its bactericidal properties.
This speeds up healing and prevents the bacteria from spreading. Most often the ointment will several times a day into the conjunctival sac (Lower eyelid) given. Gentamycin is one of the most common active ingredients and is often combined with the anti-inflammatory dexamethasone. As a rule, those affected should two to three times a day, an approx. 1 cm long strand of ointment into the conjunctival sac (Lower eyelid) give.Antibiotic eye ointment is a prescription drug and can therefore only be used on medical advice.
Another commonly prescribed antibiotic eye ointment is Floxal eye ointment; Floxal eye drops are also available.
- Disinfectant eye ointment
Disinfecting eye ointment, on the other hand, is freely available in pharmacies and has a cleansing effect on the stye thanks to the active ingredient bibrocathol. In addition to the antiseptic effect, it often has so-called secretion-inhibiting ingredients that loosen the adhesions in the affected eye. There are numerous disinfecting eye ointments available in pharmacies, including:
- Posiformin® 2% eye ointment
- Noviform 2% eye ointment
Those affected should take one several times a day about 0.5cm Put a long line of ointment in the conjunctival sac or on the affected lid edge.
- Homeopathic eye ointment
Apart from the conventional medical eye ointments, homeopathic treatment with herbal, over-the-counter ointments can also provide relief. A proven ingredient of such eye ointment is an extract from the Echinacea plant, also called coneflower. If after 2-3 days of treatment with Echinacea eye ointment (e.g. Euphrasia eye ointment) there is no noticeable improvement or the symptoms get worse, those affected should nevertheless consult an ophthalmologist.
Which homeopathic remedies help with a stye?
There are several homeopathic remedies that can be used to treat stye in both children and adults.
Most are in the form of globules (Globules) taken. Depending on the course and stage of the disease, different preparations are used.
In the beginning, if no pus has collected, Belladonna and Arnica can help suppress the development of pus and thus positively influence the course of the disease. These two preparations should be taken when the first swelling and reddening of the eyelid is noticeable.
Other helpful substances are:
- Hepar Sulfuris - for pus formation
- Pulsatilla pratensis - for sticky, inflamed eyelids
- Staphisagria, Sulfur - if the stye keeps reappearing
- Lycopodium clavatum - stye near the inner corner of the eye
- Graphites - stye on the lower eyelid
If the symptoms do not get better after about 2 days and may even get worse, a doctor should be consulted immediately.
Read more on the subject at: Homeopathy for stye.
Preventing a stye
What are the causes of a stye?
Most stye is an infection with the bacterium Staphylococcus aureus. This pathogen occurs naturally in different parts of the body.
For example, it can be found in the armpit, the nasal vestibule or the hairline on the forehead.
The eyelid has several different glands. The so-called Meibomian glands are more on the inside of the eyelid, while the so-called Moll and Zeis glands are located next to the eyelashes, i.e. more on the outside of the eyelid.
If a meibomian gland is affected by the inflammation, one speaks of an inner stye (Hordeolum internum).
To get an outer stye (External hordeolum) it is when Moll or Zeis glands are infected.
Pus develops in the eyelid, painful thickening and reddening. As a rule, the "pimple" bursts after about a week and the pus drains.
Barley is often associated with diabetes mellitus.
Frequent recurrences (recurrences) also occur with acne (Acne vulgaris) or gastrointestinal diseases.
They are particularly popular with frequent eyelid inflammation or dry eyes.
What are the risk factors for a stye?
If barley grains occur frequently, or patients sometimes suffer from multiple inflammations at the same time, this is known as hordeolosis.
People with a weakened immune system are particularly at risk:
These include above all patients with diabetes mellitus (Diabetes)!
But even with high psychological stress (e.g. stress) the clinical picture can occur more frequently.
Children in particular often suffer from stye due to poor hand hygiene.
Contact lens wearers represent a special risk group.
Inserting the lenses can easily get bacteria into the eye and cause an infection.
Only strict hygienic handling will reduce the risk!
Eye makeup should also be viewed critically, as e.g. by washing the eyelashes, pathogens can reach the edge of the eyelid
Hence, it is best to use the mascara every 3-6 months to exchange.
Is a stye contagious?
In most cases, stye is triggered by an infection with bacteria.
In principle, it is therefore one of the contagious diseases, like all clinical pictures with a bacterial basis!
Nevertheless, the risk of infection is rather low, e.g. in contrast to conjunctivitis.
The most common pathogen in stye is Staphylococcus aureus, a widespread bacterium.
It can be found on many natural surfaces or materials, not infrequently on human skin or mucous membrane.
Typically e.g. Infect children with the germs while playing in the sandpit.
Usually the pathogen is harmless and does not cause any symptoms.
However, if the bacterial density is increased by favorable conditions, e.g. a weakened immune system or minor injuries, which increases rapidly, upset the sensitive balance: formerly harmless staphylococci gain in disease value and cause complaints such as stye.
transmission
The transmission of bacteria can take place in different ways. A distinction is made between the so-called direct and indirect infection.
In the case of a direct infection, the person concerned comes into direct contact with the pathogens: by sneezing, coughing or blowing their nose numerous tiny droplets are sprayed into the air.
People nearby breathe them in and the pathogens enter the body.
Contact infection is also one of the direct ways of infection.
Here germs are caused by direct contact, e.g. Shake hands, stripped off.
The so-called smear infection plays a role in the infection with a stye.
Here the infection occurs indirectly by touching a contaminated (contaminated) Subject: Sufferers wash their face and rub the affected eye with the towel.
The bacteria get to the surface and settle.
Then other family members dry their faces with the same towel and thus carry pathogens into their eyes.
There they multiply and lead to a stye.
In general, hand-eye contact should be strictly avoided in the event of illness.
It takes some discipline not to touch the itchy and burning stye. It is especially difficult for children!
This is the only way to prevent pathogens from getting through body contact (e.g. Shaking hands) be transmitted.
It is not to be expected that the bacteria will pass eye to eye "leap'.
As long as the following rules of conduct are followed, the risk of infection can be almost completely reduced:
-
Avoid eye-hand contact.
-
Frequent and careful hand washing: hold hands under running water, 20-30 seconds rub with soap, rinse thoroughly.
Especially before and after touching the eyes! -
Strict separation of towels, washcloths etc.
-
Eye ointments and drops may only be used by one person.
-
No eye makeup (mascara, kohl pencil, etc.).
- Avoid contact lenses.
Course of a stye
What is the course of a stye?
After the pus has broken through and the stye (hordeolum) has completely emptied, the symptoms in most cases go away very quickly.
How long is the duration of a stye?
The stye (hordeolum) is usually a fairly harmless bacterial infection. If there are no complications and the pathogen does not spread further, it usually heals on its own.
As the disease progresses, the eyelids are initially swollen and reddened. This can develop within a few days. In most cases, the accumulation of pus then opens up on its own. Usually this happens after about 3 to 6 days.
If strict hygiene is observed and the avoidance of further spread of the pathogens located in the pus, the stye heals without complications. If the bacteria are transferred to the eyeball or the conjunctiva, however, more extensive inflammation can occur and the course of the disease is much more protracted. In addition, with a weakened immune system, several grains of barley can develop in a row, which can also delay the healing process.
What is the prognosis for a stye?
Usually, a stye will heal completely without any problem.
However, if left untreated, chronic inflammation of the affected glands can develop over time.
In such cases a so-called hailstone (Chalazion) visible in the upper or lower eyelid.
As a rule, the hailstone cannot be moved, is very firm and, in contrast to the stye, is completely painless!
Most of the hailstones have to be removed surgically.
In some disease courses, the infection attacks surrounding regions, such as the conjunctiva (conjunctivitis: conjunctivitis) or, very rarely, the eye socket (orbit).
If the disease recurs frequently, an underlying disease (e.g. diabetes mellitus) should be excluded.
Further questions about stye
Why do children have stye more often?
In children it comes to the development of a stye much more often than in adults. This is due to the child's immune system, which is not yet fully developed. The bacteria can settle on the eyelid more easily and cause a purulent inflammation.
The risk of infection and the spread of the pathogen is also increased in children, as they often rub their eyes with their hands and the bacteria can be passed on. In these cases it is particularly important to pay close attention to hygiene and to use your own towels and washcloths within a family. In no case should the stye itself be opened.
Since a stye is contagious, care should be taken in kindergarten or school to ensure that hands are washed regularly and that the pathogen is prevented from spreading. The child should be presented to a pediatrician who will decide whether the child can visit public institutions and whether an antibiotic may be necessary to fight the bacteria. Antibiotics are used in the form of eye drops or eye ointments. Irradiation with red light can also help to positively influence the course of the disease, since it accelerates the self-opening of the stye.