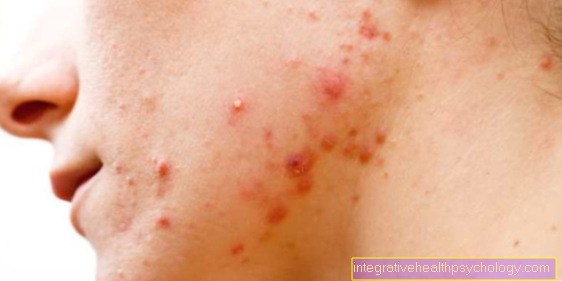
Nerve pain
definition
About 6% of the German population reports nerve pain. Nerve pain or, expertly, neuralgia represents pain that is in the innervated area manifest and be caused by one or more nerves.
This distinguishes nerve pain from other types of pain such as back pain. These can also be due to muscle cramps, for example.
However, nerve pain is the direct result of damage to a tissue belonging to the nervous system. This activates the pain-sensing and -conducting nerve endings that lead to sensory peripheral nerves, but also to the spinal cord and brain.
Also read this article on the topic: Pain

root cause
Damage to a nerve or a structure belonging to the nervous system can have various causes.
Nerves can be damaged by external influences through mechanical effects in the form of cuts or pressure, for example in the case of a herniated disc, and through toxic chemical burns or radiation. The so-called neurotoxins include heavy metals such as lead, cyclic hydrocarbons, alcohol, but also some drugs.
Other causes are inflammatory processes, as in shingles (herpes zoster), or metabolic Processes such as the metabolic disorder diabetes mellitus.
Infections are usually responsible for inflammatory processes. Varicella (Chickenpox pathogen), Borrelia and others also attack the peripheral nerves or the nerve cells themselves when infected.
But inflammation can also go through autoimmunological Processes arise, that is, in diseases in which the body's own immune system attacks cells and structures in its own body. These diseases, which can also cause nerve pain, include multiple sclerosis and Guillain-Barre syndrome.
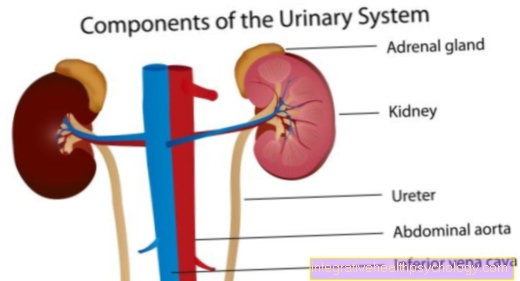
Disorders of the metabolism of the nerve cells or the myelin sheaths can be caused not only by diabetes mellitus but also by diseases of the intestine and the resulting poor recordingsMal absorption) are triggered by vitamins like thiamine. Diseases of the liver or kidneys can also be the cause of a metabolic disorder.
In addition, the exact severity of the nerve pain is influenced by the pattern of damage.
If the medullary sheath of a nerve is damaged, it will "Demyelinated", the nerve loses its protective insulating layer. Without this layer, electrical signals from sensitive nerves that respond to touch can jump to pain-conducting fibers. Causal diseases such as multiple sclerosis and viral infectious diseases such as shingles (Herpes zoster) underlie. Metabolic diseases such as diabetes mellitus can also be responsible for this type of damage.
If not only the protective medullary sheath but also the entire nerve fiber is damaged, the flow of information can be completely blocked, a so-called Deafferentation, come. The blockage creates a lack of information in the central nervous system, so that the inhibitory effects controlled by the central nervous system are no longer activated due to the lack of ascending stimuli. These so-called Deafferentation pain occur, for example, after amputations or paraplegia.
You may also be interested in this topic: Pinched nerve
To Severing of large nerves it is especially important Amputations, what to Deafferentation- and / or phantom pain. As already mentioned, deafferentation pain results from the elimination of inhibitory pains A -? - fibersthat react to pressure and touch. These fibers normally block the transmission of pain impulses in the spinal cord via interneurons. If this inhibition fails, it can lead to one excessive activity the no longer inhibited neurons and consequently pain.
The exact cause for phantom pain is still not adequately clarified. It is known that every part of the body is represented at a specific point on the cortex of the brain.
One explanation is that the Severing a limb in the cortex a reorganization of these representations takes place. The pain felt can then be caused by a Conflict situation between the new and old pattern of the respective representation.
That leaves the expected answer of the missing limb to one Signal of the representation in the cortex, the Signal intensity the representation as a compensation mechanism reinforcedwhat from the patient as pain can be felt.
In addition to the im peripheral nervous system emerging Nerve pain there is still that central pain.
Central nerve pain occurs in the CNS, i.e. directly in the brain or in the spinal cord, through damage to the neurons located there.
There is a division into thalamic paincaused by damage to nerve cells in the thalamus, and pseudothalamic painpointing to damage in other regions of the CNS are due. The Spinothalamic tract in the Spinal cord and the Nucleus ventralis posterolateralis of Thalamus name as frequent sites of damage.
This one Lesions (Damage) are often caused by causal diseases. In diseases such as multiple sclerosis or syringomyelia, degenerative processes take place that affect both Failure of obstructive structures in the CNS as well as for Irritation of the sensitive web can lead to pain and temperature.
If peripheral nerve pain persists, a kind of learning process can lead to an adaptation of the nerve cells in the CNS. This means that nerve pain can become chronic in the center, although the actual peripheral cause has long since healed, for example in postherpetic neuralgia.
Symptoms
Depending on the location of the damage and its cause, different forms of nerve pain can occur.
If, for example, a motor nerve is damaged, in addition to nerve pain, symptoms such as paralysis can also occur, which are caused by the functional failure of the affected nerve.
For neuropathic pain, between neuralgiforms and causalgiforms Differentiated pain. Neuralgiform pains are of a short, violent shooting character that may appear in some sort of seizure. Causalgiform pain manifests itself in a persistent dull burning or tingling sensation. Especially with this type of pain, it can become chronic.
Read about this too: Burning in the fingers
Another symptom is that evoked pain. Here, stimuli that would not cause pain under normal circumstances can also trigger pain (a so-called Allodynia).
Even wearing clothes on the skin is perceived as uncomfortable. The perception of heat, cold or pressure can also be excessively increased, so that these stimuli are also perceived as painful (here one speaks of a Hyperalgesia).
Deafferentation pain is often associated with an initial feeling of numbness, which in the course of the process changes into the neuropathic pain symptoms described above.
In phantom pain, the pain sensation usually occurs at the point where the amputated limb was previously located. The pain that occurs can express itself in different ways.
A burning sensation that does not occur consistently from time to time is possible. Abnormal sensations such as warmth, cold or a tingling sensation are also possible. Sometimes the nerve pain is felt like itching or bruising.
The sensations that occur can also be intensified by external influences such as stress, weather and temperature changes or by fear.
Central nerve pain can also express itself in different ways. If the location of the damage is in the thalamus, brain stem or spinal cord, it is often burning and accompanied by abnormal sensations, especially in the arms and legs. However, drilling or tearing can also occur.
In addition, overactivity of the sympathetic nervous system can often be observed where the nerve pain manifests itself. This can lead to excessive sweating and reddening of the skin. The pain often occurs in a large area and can be felt both superficially and in depth.
therapy

The treatment of nerve pain is mostly directed according to their causeas far as this is known.
Is the pain one infection are based, depending on the causative agent Antibiotics or antivirals first choice. Is a Vitamin deficiency the reason for the Nerve pain, even supplementation can help alleviate symptoms. At through diabetes evoked Nerve pain can correct setting of the Blood sugar level already cause the nerve pain to subside.
Are the nerve pain caused by a Intoxication (poisoning) causes, often already introduces Omission of the harmful substance to an improvement of the symptoms.
Is the cause mechanical origin, for example one triggered by pressure Circulatory disorder as a result of an injury or as with one disc prolapse a Narrowing of the spinal canal, this will mostly operational treated. This generally provides rapid relief, taking into account the individual risks of surgery.
Even with others Nerve painwhose cause in a disrupted processing and forwarding of stimuli in Nervous system the symptoms can be improved by surgical measures. These include blockages of the Sympathetic, for example at Thalamic pain, or directly the Pain pathwaysif the actual place of origin of the nerve pain cannot be clearly identified.
Is the cause of that Nerve pain not known, may be through a symptomatic therapy Mitigation can be provided. Above all, this includes one medication, but also alternative healing methods to analgesia (Pain relief) like acupuncture or psychotherapy.
Here the patient is taught through specific training how to handle their own Pain perception bypass and for example through targeted distraction can displace to a large extent. This method is mainly used for long-lasting Nerve pain like that Phantom pain applied.
In the drug therapy there are a number of possible substances. Morphinewhich are otherwise the most effective Painkiller pose are for nerve pain, however fewer Means of choice. As with central pain or attack-like nerve pain like with a Multiple sclerosis direct structures of the central nervous system are affected, drugs that act on these structures are preferred.
These include Anticonvulsants for attack-like, shooting nerve pain and antidepressants for persistent pain.
Anticonvulsants are antispasmodic substances and above all drugs for the treatment of epilepsy, but which are also used in pain therapy. The active ingredients regulate the conduction and transmission of impulses by binding to structures that act both Epilepsies and are overexcited when there is nerve pain. These include gabapentin and carbamazepine, for example.
Antidepressants are primarily used in the treatment of depression, however, depending on their mechanism of action, they also have pain-relieving effects. By using signal substances that conduct pain inhibit or the breakdown of pain-relieving messenger substances prevent, the transfer of Pain impulses disturbed. Common remedies are here Amitriptyline, Clomipramine, Imipramine and doxepin.
Another way of treating nerve pain is electrical stimulation, the so-called transcutaneous electrical nerve stimulation (TENS), which among other things for phantom pain and as deep brain stimulation central pain Is used. This is done with electrodes slight stimuli in the form of Current pulses generated and transferred to nerve fibers. This stops the forwarding and thus also the perception of pain suppressed.
Nerve pain after an operation
Nerve pain can occur after an operation. It is essential to treat this as quickly as possible, as pain can have a negative effect on the healing process. Post-operative pain can either by direct damage to the nerve or caused by a cause stressing the nerve. The operation does not necessarily have to be an operation close to the nerve, such as an intervertebral disc operation. However, nerve pain naturally occurs more frequently after such procedures.
If the nerve is irritated, cut, torn, or completely severed during the operation, there is a high probability of nerve pain. One is particularly critical Severing the nerve - Not only are all the functions that were mediated by the nerve lost; there is also a risk of the patient becoming resistant to therapy Phantom pain developed. In addition to the direct influence on the nerve, external influences are important in the development of postoperative pain. On the one hand, the operation may not have been expedient. The pathological change, for example the herniated disc, still exists and affects the nerve. On the other hand, the consequences of the procedure can affect a nerve. By Bleeding or swelling in the surgical area or infections can recur.
When treating nerve pain after surgery, normal post-operative pain relievers are used, as the pain often recedes. Other treatment measures should also be taken to promote the healing process and the recovery of the nerve tissue. Physiotherapy is used successfully in many cases for nerve pain. Heat compressions, electrotherapy (TENS) and acupuncture have proven to be pain relievers in the past.
Nerve pain in certain parts of the body
Nerve pain in the back
Nerve pain in the back differs significantly from back pain of other origins, which can have various causes. The nerve pain is usually one-sided. Since nerve cords emerge from the spine on the left as well as on the right, only one side is usually damaged and then causes more or less problems.
In one out of 10 cases, the back pain is caused by pathological changes to the intervertebral discs or damage to the surrounding region. Not just the classic herniated disc (Prolapse) plays an important role here, but also injuries. In the case of a herniated disc, after lengthy changes, a disc bulges out into the space of the spinal cord. This compresses it and the nerve roots can be compressed (Radiculopathy) that emerge laterally from the spinal cord. If the corresponding nerve root supplies parts of the back, massive pain can occur.
Lumboischialgia is a special clinical picture. In this, two syndromes come together: sciatica and lumbago (lumbago). The disease is usually associated with a very deep herniated disc (or some other deep-seated impairment of the spinal cord). The strong compression of the lower nerve roots not only results in massive back pain, but also a radiation of the pain into the patient's legs. A simple lumbago, on the other hand, is often based on a vertebral blockage that can be resolved through manual therapy.
Injuries to the spine are also based on a similar disease process - if a vertebral body breaks, there is a possibility of compression. An accident does not necessarily have to be responsible for the injury. Changes in the bones caused by the disease osteoporosis can also make the bones so brittle that they break under low stress. Older women are particularly often affected. After the menopause there is a change in the hormonal balance (especially the estrogen level) in women, which affects the structure of bones. Other space-occupying processes can be tumors or abscesses.
Shingles and its virus, herpes zoster, can also cause nerve pain. After the virus causes chickenpox when it first becomes infected, which usually takes place in childhood, it remains in the body of every patient until the end of their life. The pathogen attaches itself to nerve nodes and can break out again at times. This can be brought about by a weakened immune system, stressful situations or various other circumstances. When it breaks out, herpes zoster triggers an inflammation of the nerves, which in addition to a rash in the innervation area (area supplied by the nerve) can also lead to severe pain. The nerve pain can last longer than the actual infection lasts. This is called postherpetic neuralgia.
Read more on the subject at: Shingles pain
Nerve pain in the leg
Nerve pain in the leg is not only stressful because of the pain, but is also often associated with severe restrictions for the patient. Movement and prolonged standing are usually difficult and can lead to a reduction in the patient's quality of life - both socially and professionally.
Most commonly, nerve pain in the leg is caused by sciatica. The pain radiates through the buttocks into the leg and is caused by the sciatic nerve. The impairment of the nerve, which usually results from an existing pressure load, can be triggered by various circumstances. Muscle tension is the most harmless cause of sciatica, but in many cases vertebral blockages, protruding discs or herniated discs also play a role. Operations that affect the hip joint or surrounding structures can damage the sciatic nerve. Sciatica with associated nerve pain in the leg can also be triggered by inflammation or tumors, but this is less common.
Read more on the topic: Duration of an inflammation of the nerves - what you should be aware of!
Sciatica can be recognized by the relatively characteristic pain symptoms. Suddenly, extremely severe pain occurs, moving from the lower back over the lumbar spine, then over the buttocks into the legs - primarily into the back of the thighs. The pain can continue into the foot region. In addition to the pain, there are sensory disorders that patients describe as numbness or tingling.
Strong movements such as uncontrolled coughing or sneezing make the pain worse, as this builds up pressure in the abdomen. The movement of the upper body as well as the hips and legs are extremely restricted. Usually, only one leg is affected by the pain symptoms in sciatica. A relieving posture can typically be observed in many patients: the upper body is tilted towards the healthy side in order to take pressure off the stressed nerve root. The nerve roots that emerge from the spinal cord at the end of the spine are responsible for controlling continence. Severe sciatica can lead to problems with bowel movements, but also with urination.
Read more on the subject at: Sciatica
Nerve pain in the foot
In the foot, pain is usually caused by injuries to the joint or ligamentous apparatus. But nerve pain can also be responsible for sharp pain, for which normal pain reliever medication is not sufficient. The treatment of the painful foot is urgently necessary, as the constant strain increases pain and the patient's suffering is very high.
Even with nerve pain in the foot, the cause usually lies with the Entrapment of the affected nerve. This can go through Misaligned feet or shoes that are too tight. Women are particularly often affected by such pain, as they tend to wear narrow shoes with heels. A Tarsal tunnel syndrome can also lead to nerve entrapment. The development of this clinical picture is the same as with carpal tunnel syndrome - only on the leg instead of the wrist.
Are rare Infections, tumors or drugs to blame for pain in the foot. Much more often occur so-called neuropathic pain with existing diabetes mellitus on. The high blood sugar level damages the vessels and nerves and thus leads to abnormal sensations and pain.A wide range of pain medication should be tried during treatment, as few medications provide relief from nerve pain. If the case is resistant to therapy, the nerve can be surgically exposed and desensitized (made insensitive). In the case of diabetic nerve pain, a good control of blood sugar and the administration of alpha lipoic acid and vitamin B supplements usually promise an improvement.
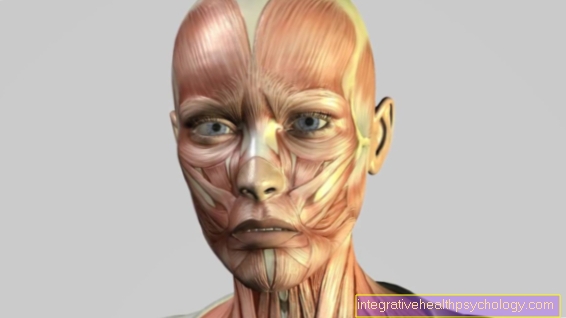
Nerve pain in the face
Nerve pain in the face is extremely uncomfortable. Patients find touch and movements that are carried out throughout the day painful. It can even a draft of air that brushes the skin can trigger pain. The intensity of the pain is hardly comparable - those affected often indicate the highest possible pain level in the classification, which is why this is also called "Annihilation pain" referred to as.
The most common disease associated with facial nerve pain is Trigeminal neuralgia. The fifth cranial nerve, the trigeminal nerve, is usually damaged or inflamed. It supplies the face with pain-sensitive nerve fibers on all levels. The pain symptoms are characterized by their enormous intensity and you seizure-like occurrence. Trigeminal neuralgia can be triggered by many different underlying diseases. The therapy uses carbamazepine, which is actually a drug used to treat epilepsy. In this area of application, it has a pain-preventing effect, since normal painkillers have no effect on classic trigeminal neuralgia. During surgical interventions, extreme care must be taken, as otherwise lifelong sensory disorders can remain in the face.
Nerve pain in the arm
Any part of the arm can be affected by predominant nerve pain. Starting with the hand, the pain can spread over the forearm and upper arm to the shoulder region. The problems are often noticed in everyday movements that are suddenly associated with pain. Raising your arms above your head, hygiene in the morning or getting dressed can be the trigger for the first pain symptoms.
The damage that the nerve must be subject to is not infrequently due to repeated incorrect loading. The same course of action at work as well as general bad posture always play an important role. If muscles are repeatedly stressed incorrectly, the muscle strands harden. This can affect not just one muscle, but groups of muscles that work together. The hardened muscle area presses on the nerve and, among other causes, can lead to nerve inflammation (neuritis) with the following nerve pain. The symptoms are specific to the supply area of the affected nerve.
In addition to pain, abnormal sensations and even movement disorders can occur. Since nerve pain in the arm is very painful, pain prevention therapy is the method of choice. Medicines that are actually used to treat depression or epilepsy are prescribed.
Read more about the topic here: Nerve inflammation on the arm.


.jpg)