Tendinosis calcarea of the shoulder
Synonyms
Shoulder calcification, calcium deposits in the shoulder joint, shoulder calcification, calcified shoulder
introduction
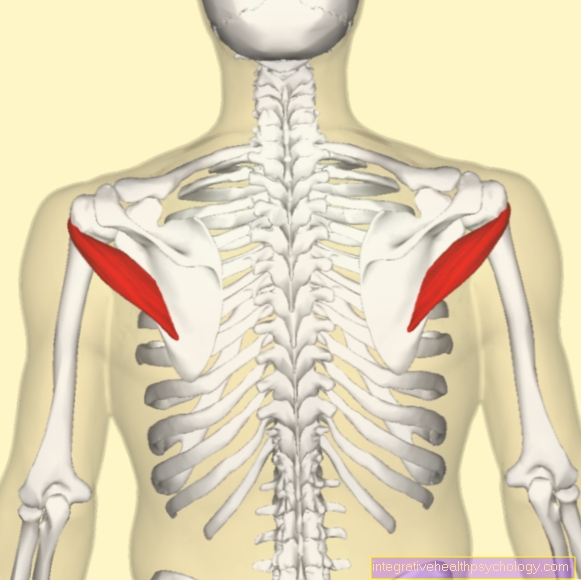
Tendinosis calcarea is the term for the calcification of various tendons in the human body, which is caused by the deposition of calcium crystals. In principle, the tendinosis calcarea can affect any tendon, but particularly often affects the tendons of the shoulder joint (especially the tendon of the supraspinatus muscle). This constellation is also known as the calcareous shoulder. The patellar and Achilles tendons are also relatively often affected by the tendinosis calcarea, but occasionally attachments of the other tendons of the rotator cuff are also affected.

The term rotator cuff is a common name for the muscles of the shoulder involved in arm rotation. In the context of tendinosis calcarea, also known as tendinitis calcarea in the case of very acute, inflammatory complaints, reactive calcium deposits occur at the tendon attachments due to insufficient blood supply to the rotator cuff. These limescale deposits can be recognized by means of an X-ray image and thus diagnosed relatively easily.
In addition to the shoulder, the Achilles tendon, kneecap and hip can also be affected in rare cases. Tendinosis calcarea occurs most frequently in patients between the ages of 40 and 50. Overall, women are affected somewhat more often than men.
Symptoms
The symptoms of tendinosis calcarea depend on which tendon is affected by the condition. If tendons in the shoulder area are diseased, patients usually feel pain when they try to lift their arm (overhead work). Pain in the side position can also occur and, in severe cases, complete immobility of the arm (pseudoparalysis).
As the disease progresses, symptoms also worsen. In the later stage, the calcifications can break into the shoulder joint, causing bursitis with severe pain, overheating and redness in the joint area. Often times, patients can only spread the affected arm away from the body by rotating it outward or inward. As a result of the rotation, the tendon with the embedded crystals is no longer pinched in the shoulder roof, so that the arm can then be raised more easily.
Secondarily, a lime shoulder can also lead to tension in the head and neck area. Because the patients can only lift their arm with pain, they perform more awkward movements that use the mobility of the shoulder blade in particular. This can overload the neck muscles and react with tension, which can often radiate painfully into the head area.
In many cases, the patients then see their problem in the neck area and no longer notice the original problem, namely the calcification of the shoulder tendons.
Appointment with a shoulder specialist

I would be happy to advise you!
Who am I?
My name is Carmen Heinz. I am a specialist in orthopedics and trauma surgery in the specialist team of .
The shoulder joint is one of the most complicated joints in the human body.
The treatment of the shoulder (rotator cuff, impingement syndrome, calcified shoulder (tendinosis calcarea, biceps tendon, etc.) therefore requires a lot of experience.
I treat a wide variety of shoulder diseases in a conservative way.
The aim of any therapy is treatment with full recovery without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You can find me in:
- - your orthopedic surgeon
14
Directly to the online appointment arrangement
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
You can find more information about myself at Carmen Heinz.
therapy
It is not possible to make a general assessment of the individual course of the disease. While some patients “sit out” the disease in the course of the body's own self-healing process, other patients, especially those who suffer from severe pain, whose calcifications are larger than 1 cm and indicate a hard consistency, may require surgical treatment. As this disease has a high tendency to heal spontaneously, surgery is usually very rare.
As part of the operation, the calcium deposits are removed and the roof area (subacromial space) for the shoulder tendons is expanded.
Conservative therapy
In the context of acute bursitis (subacromial bursitis) and therefore severe pain, the arm can be briefly relieved with a shoulder orthosis (a type of bandage). The administration of analgesics (= pain relievers) and NSAIDs (= non-steroidal anti-rheumatics), which have a strong anti-inflammatory effect, relieve the pain. Cooling the shoulder (cryotherapy) also relieves pain and slows down inflammation.
Rapid pain relief can be achieved through the injection / syringe of a light anesthetic, possibly with the addition of cortisone. The mixture is injected from the side or from the back under the shoulder roof (subacromial infiltration). The local anesthetic provides an immediate analgesic effect, while the cortisone, as the strongest anti-inflammatory drug ever, provides pain relief even after the anesthetic is broken down. Since cortisone causes the blood sugar level to rise sharply, sugar patients (diabetes mellitus) have to adjust their insulin requirements and check the blood sugar level more frequently.
As soon as the pain subsides, physiotherapy (physical therapy) can be started. The goals of physiotherapy are to relieve the shoulder tendons under the shoulder roof and to preserve the mobility of the shoulder joints. The shoulder joint is the joint of the body that tends to become partially rigid in the event of pain-related restriction of movement or other sustained immobilization due to capsule shrinkage.
At the ESWT (Extracorporeal shock wave therapy) the calcifications in the tendon are deliberately exposed to shock waves, which should lead to the dissolution of the foci. Shock waves are very high-energy pressure waves that can shatter the calcifications. What remains are fine lime particles, which the body can break down and remove more easily. Several sessions are necessary for this. Possible side effects of this treatment are local swelling of the treated tissue, as well as bleeding and reddening of the skin. Some patients also find ESWT painful, but this differs from patient to patient. In some circumstances, the surrounding bones, nerves, tendons and vessels can also be injured.
ESWT does not achieve the desired effect in every patient. In some cases the symptoms can even worsen, but so far very good results have been achieved overall with ESWT in the treatment of tendinosis calcarea. Good to very good results (patient satisfaction) can be achieved in 60-90% of cases.
Further information is also available under our topic: X-ray stimulation
Shock wave therapy for a tendinosis calcarea
The Lime shoulder (Tendinosis calcarea) is one of the classic areas of application for shock wave therapy. The mode of action can be explained more biologically than mechanically. The lime deposit in the shoulder is not smashed but a biological tissue reaction is triggered, the result of which is the dissolution of the calcium deposit and a local reduction in inflammation. The success of therapy should be measured less by whether that Lime deposit in the X-ray control has completely disappeared, rather than the pain reduction of the patient.
Many people have calcium deposits in the shoulder vision without this symptomatic (painful) would have to be. In this respect, a calcareous shoulder is sometimes a chance diagnosis without therapeutic relevance. With painful calcified shoulder (Tendinosis calcarea)is the Shock wave therapy (ESWT) However, it is a promising therapeutic option that should be seriously considered before an operative intervention.
The shock wave should take effect within the first 3 months after treatment. Much later, therapy success (pain relief / dissolution of the calcium deposit) can no longer be expected. Therapy should start with a high energy shock wave be performed.
You can find further information under our topic: Shock wave therapy
Operative therapy

Surgical treatment may be necessary in patients who persistently suffer from severe pain, whose foci of calcium are larger than 1 cm and have a hard consistency. However, since the tendinosis calcarea has a high tendency to spontaneously heal, the indication for surgery is rather cautious.
If conservative procedures have failed, the calcareous shoulder should be surgically removed.
During the operation, the calcium deposits are removed and the subacromial space is expanded.
The procedure is usually minimally invasive, i.e. arthroscopically. An arthroscopy describes the observation (reflection) of a joint by introducing a rod camera over very small incisions (0.5-1 cm). Special instruments can be used during such a mirroring (Arthroscopy) treatment of damaged joint structures can also take place.
After the shoulder joint has been mirrored, through which in particular any additional damage (shoulder arthrosis, rotator cuff tear) can be diagnosed, the shoulder roof space is usually enlarged by sparingly removing bone from the lower surface of the acromion (subacromial decompression). The shoulder bag is also removed. As soon as the limestone focus has been located, it can be removed.
The limescale center can also be removed with a normal, open (not minimally invasive) operation. The operation is then carried out through a small skin incision about 3 cm.
After an operation, the shoulder should be spared for about 3 weeks. As a rule, postoperative follow-up care is carried out in conjunction with anti-inflammatory and pain reliever medication. Physiotherapy exercise treatments are intended to preserve the mobility of the shoulder joints.
You can also find more information on this topic at: OP of a calcareous shoulder
Physiotherapy for a tendinosis calcarea
Physiotherapy is an important pillar of therapy for the calcified shoulder.
A tendinosis calcarea harbors the risk of chronic pain and the development of a stiff shoulder, which should be averted with the help of physiotherapy. It is important to keep the shoulder in motion with the right exercises, since relieving postures can otherwise lead to permanent bad postures.
Physiotherapy is used not only as part of the conservative therapy of tendinosis calcarea, but also after surgical calcium removal. Physiotherapy is often combined with what is known as cryotherapy (Cold therapy) combined. Physiotherapy expands the space in the shoulder joint so that less pressure is exerted on the tendons of the shoulder joint and the pain is alleviated.
Exercises for a tendinosis calcarea
Exercises should not only be carried out together with the treating physiotherapist, but also independently at home. This allows the healing to progress faster. The exercises are best shown by the treating physiotherapist so that you know exactly what to look out for.
Exercises that are recommended for a calcareous shoulder are stretching exercises.
Stretching exercises ensure that tendons and muscles become more elastic and blood circulation is increased. A simple but good exercise for the shoulder is the pendulum movement in the shoulder joint. The arm dangles back and forth very loosely on the body.
In another exercise, the arm can be stretched out horizontally and the forearm bent 90 degrees upwards. The weight of your forearm is carefully pressed against a wall until you feel tight at some point.
For another exercise, stand in a door frame: the upper arms are against the body and the forearms are angled forward at 90 degrees and now both press against the respective door frame. In a last recommended exercise, you put your hand behind your head as if you wanted to tie an apron or something similar around your neck. With the other hand a pull is made on the upright and bent elbow towards the top and outside. During these exercises you should only feel a slight feeling of tension; if you experience pain, you should stop the exercise.
Read more on this topic: Which exercises help with a calcified shoulder?
Can Exercise Help?
In the long term, exercises can help with a tendinosis calcarea. Planned and targeted exercises should always be carried out, in which incorrect loading or overloading of the shoulder is avoided. Training or supervision by a physiotherapist is very useful. In this way, misalignments and incorrect training can be avoided and further damage to the affected area is prevented. It is also very important to protect the area in question in the event of sudden and acute severe pain.
Kinesio tape for the treatment of a tendinosis calcarea
Kinesio taping is a relatively newer treatment method. It can be used in various clinical pictures, such as the tendinosis calcarea. With kinesio taping, elastic strips are stuck to the skin in certain directions of pull.
This treatment can correct bad posture, alleviate pain and support certain encouraging movements. Many patients respond positively to this method of treatment. Kinesio taping should not be used as the only therapy, but only as a support.
Read more on the topic: Kinesio tape
Homeopathy for a tendinosis calcarea
As with many other diseases, homeopathy can also be used for the calcified shoulder.
In particular, remedies such as Solanum malacoxylon, vermiculite, Lyopodium, Calcium phosphoricum and apple cider vinegar are used. The preparations are said to have effects that are supposed to work against calcifications. Apple cider vinegar, for example, can be used both externally in the form of a soaked compress and internally for drinking in the form of a water-apple cider vinegar mixture (about two spoons of apple cider vinegar). Apple cider vinegar should be able to dissolve the lime. However, the effect of these preparations has not been scientifically proven.
causes
The exact causes of the tendinosis calcarea have not been conclusively clarified. It is assumed that due to degenerative changes in the tendons, i.e. due to signs of wear and tear during the aging process, the blood circulation in the tendons deteriorates and the pressure on the tendons increases.
This ultimately leads to the reactive deposits of calcium crystals in the tissue, which cause pain when moving. Using the example of the shoulder joint, the crystals lead to a relative thickening of the tendon, so that it is pinched between the shoulder joint and the shoulder roof when the arm is raised. This causes the typical complaints.
In the course of the disease, the immune system also reacts to the stored crystals in that certain immune cells, the macrophages, try to break down the crystals. Ultimately, this results in scarring of the tissue and, under certain circumstances, a persistent thickening of the tendons.
course
Tendinosis calcarea is often diagnosed by chance, as it is usually relatively painless. Many patients may have a "calcareous shoulder" without this ever having to lead to symptoms. The course of the disease and the development of the tendinosis calcarea / calcareous shoulder can be divided into individual phases.Due to the phased course, acute pain usually occurs relapses. Lingering in a phase of illness differs from patient to patient and cannot be predicted. Phases of inflammatory shoulder pain change to phases of almost complete freedom from pain. There are four phases of tendinitis calcarea:
- Phase: Cell transformation phase:
During the first phase, there is a cell transformation. The tendon tissue is converted into fiber cartilage. The patient usually has no or very little pain. This phase cannot yet be diagnosed with an X-ray, as calcification has not yet taken place. - Phase: Calcification phase:
In the course of the second phase, the cartilage tissue partially dies and lime is deposited. This phase can be diagnosed on the one hand by means of ultrasound, but also by means of X-ray examinations. If the shoulder tendon is very thrown up by the calcium deposit, a tight shoulder can result when the arm is raised. This in turn leads to irritation of the tendons that slide under the roof of the shoulder, here especially the supraspinatus tendon, as well as of the roof of the shoulder bag (Subacromial bursa). The painful clinical picture of an impingement syndrome can develop in this way. - Phase: Phase of resorption:
In this phase, the limescale dissolves spontaneously. Frequently, calcium is carried away into the adjacent bursa, which can cause massive inflammation. The third phase is therefore often characterized by extreme pain, which can be traced back to the severe bursitis. Patients have great difficulty moving their arm because of the pain. Within a few weeks, however, the calcifications eventually recede. - Phase: Repair phase:
In the last phase, the calcification has receded to such an extent that new scar tissue can fill the remaining tendon injury. Under certain circumstances, this can result in a thickened tendon that can continue to cause problems. In the best case scenario, however, the tendon can also take on its original shape and thickness. Not every Tendinosis calcarea disease goes through this cycle completely. Tendinosis calcarea can persist in any stage of the disease and may not even reach the next phase.
Complications of a tendinosis calcarea
If the supraspinatus tendon is damaged, various complications can result. The supraspinatus tendon can be damaged by wear and tear or, as part of a tendinosis calcarea, be permeated with calcium deposits. The tendon fibers are converted into stronger material. However, this is less elastic and so there is a risk of torn or torn vision. Such a crack is usually accompanied by severe pain and an inflammatory reaction. In addition, the muscles can no longer be held properly by the tendon. For this reason, the function of the muscle, which in the supraspinatus corresponds to the splaying of the arm, can no longer be carried out properly. Another complication of damage to the supraspinatus tendon is inflammation of the bursae in the shoulder. If the tendon has stored calcium in the tendinosis calcarea, some of it can peel off. If these lime particles get into the bursa, it becomes very irritated and inflamed. In addition, the increased pressure during remodeling processes of the supraspinatus tendon can also cause irritation of the bursa, which is accompanied by bursitis. This manifests itself primarily in warming, redness and swelling of the shoulder joint and can be very painful as a complication of damage to the supraspinatus tendon.
More on this: Bursitis of the shoulder
Does the diet have an influence on the development of a tendinosis calcarea?
When it comes to the question of the extent to which diet plays a role in the development or also in the prevention of tendinosis calcarea, opinions differ. Most take the position that diet is not an influencing factor for the development of a calcareous shoulder. However, obesity is a decisive risk factor for all illnesses that have to do with wear processes.
Even with tendinosis calcarea, high weight places an additional burden on the affected tendon and therefore worsens the prognosis of the disease. In addition, a balanced diet is not only important for an appropriate weight, but also to provide the body with sufficient minerals and nutrients that are necessary for the repair processes of the damaged tendon. Furthermore, a basic diet that deacidifies the body can have a positive influence on tendinosis.
In other sources you can read that a diet rich in magnesium should be helpful to prevent a calcareous shoulder. Whole grain products or nuts, for example, are rich in magnesium.
Where else does a tendinosis calcarea occur?
Tendinosis calcarea is most common in the shoulder area. The tendon of the supraspinatus muscle is usually affected. However, it can occur on all tendons in the body. For example, the other tendons that hold the different muscles of the shoulder can also be affected. In addition, the tendinosis calcarea occurs in the knee region. The kneecap is held in place by various tendons and ligaments. These are often exposed to heavy loads in daily life and are therefore susceptible to diseases that are associated with wear and tear. Tendinosis calcarea can also affect the tendons of the kneecap.
The Achilles tendon, which is located above the heel, is also used with every step. Wear processes occur at this point, especially if the feet or legs are misaligned, poor footwear or incorrect gait habits. Tensile and compressive loads can also damage the Achilles tendon and, in turn, lead to tendinosis calcarea. Tendons that extend from the outer side of the thigh bone to the hip can also be affected. In rare cases, calcar tendinosis occurs on tendons that extend along the side or behind the elbow.
forecast
In principle, the tendinosis calcarea often heals spontaneously after the phases mentioned above, even without treatment. Nevertheless, there are often very severe symptoms, especially due to accompanying bursitis, so that supportive therapy is advisable in any case.
The exact course of the disease cannot be predicted, so it can be difficult to decide which therapy to use. Since the individual phases of the disease can last for several years and repeatedly lead to more or less severe pain, many patients do not want to wait until the calcifications resolve on their own. The therapy should be adapted to the patient's stage of the disease through targeted advice and adequate imaging.
diagnosis
Ultrasonic
As soon as calcification has occurred, it can be detected using ultrasound. The calcium focus leads to a sound extinction behind it, which can be recognized. An advantage of the ultrasound examination is the determination of the exact calcium deposit, which can make it easier to find the calcium focus when planning the operation. It is typical of the tendinosis calcarea that the calcification is in the middle of the tendon and not above or below it. This is important to know in order not to confuse the tendinosis calcarea with other possible diseases.
roentgen
As soon as calcification has occurred, it can be detected on the X-ray. The calcifications are usually very easy to see. However, there are restrictions with regard to the exact location of the limestone hearth, because images must be available from different angles in order to be able to reliably locate all limestone hearths.
Magnetic resonance examination (MRI of the shoulder)
For the diagnosis of the tendinosis calcarea, MRI does not play a role. The calcium deposit is poorly presented, which means that it can easily be mistaken for a rotator cuff lesion (rotator cuff tear / degneration of the rotator cuff tendons).
Read more on this topic at: MRI of the shoulder
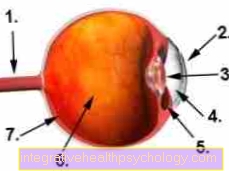
X-ray image of a tendnosis calcarea of the shoulder

- Shoulder roof (acromion)
- Lime hearth
- Humerus head
- Shoulder socket (glenoid cavity)
Summary
Tendinosis calcarea is the term for the calcification of various tendons in the human body, which is caused by the deposition of calcium crystals. In most cases the tendon of the supraspinatus muscle, which is part of the rotator cuff of the shoulder joint, is affected. One then speaks of a calcareous shoulder with complaints of arm movement.
The symptoms of a patient with tendinosis calcarea can vary considerably. This mainly depends on the size of the calcium deposit and the stage of the disease.
Large calcium deposits can lead to the affected tendon, especially when the arm is lifted sideways (Abduction) irritates under the shoulder roof.
The symptoms can include:
- Pain when lying on the affected shoulder
- Stress pain in the shoulder
- Pain after working overhead
- Sudden shoulder pain arising out of nowhere (not an accident)
- Inability to move the arm (pseudo paralysis / pseudoparalysis)
Imaging by means of ultrasound can be used for a clear diagnosis of the tendinosis calcarea, whereby the somewhat difficult diagnosis by means of x-rays is also possible. An MRI image is not suitable.
Shock wave therapy (ESWT) or surgery are particularly suitable for treatment. In ESWT, the calcium crystals are shattered by means of high-energy pressure waves so that they can be broken down by the body.
Another alternative to treating the tendinosis calcarea is surgical treatment of the calcified tendons. This is usually only carried out if the patient continues to suffer from severe pain despite conservative measures, the calcifications are very large and there is no evidence of a spontaneous regression of the calcifications. Since the calcifications very often recede spontaneously, surgical rehabilitation of the tissue is waited as long as possible.
If the operation is indicated, however, it is usually performed as part of an arthroscopy (Jointoscopy) performed. This approach is minimally invasive and poses the lowest risk. During the procedure, the calcified foci are removed from the tendon tissue. Then the joint must first be immobilized. In order to maintain the function and mobility of the joint, physiotherapy is usually carried out afterwards.