Water in the pericardium - dangerous?
What is it and how dangerous is it?
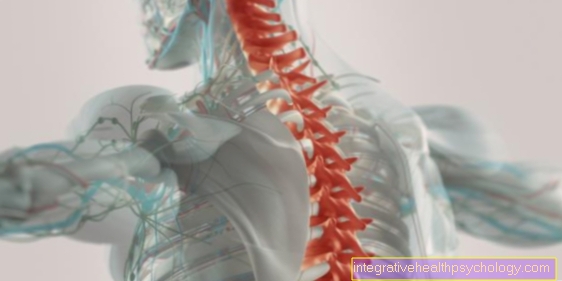
An accumulation of water in the pericardium - also called pericardial effusion - denotes the presence of fluid between the two connective tissue membranes that surround the heart (Pericardial cavity). This accumulation of water can occur both acutely and chronically. In healthy people there is about 20 ml of fluid in the pericardium, which is quite normal and supports the heart in its pumping movement within the pericardium.

The danger posed by water in the pericardium depends largely on the cause and the amount of the effusion. The spectrum of risks with water in the pericardium ranges from the absence of symptoms without the need for treatment to life-threatening emergency situations.
In many cases, especially if the effusion is triggered by pathogens, only a small amount of water collects in the pericardium, which only slightly exceeds the normal fluid level of around 20ml. Most of the time, the water gathers at the apex of the heart along the force of gravity and does not affect the function of the heart.
The development of the amount of water must be constantly monitored in order to be able to assess the course. In these cases, however, drug therapy is sufficient and naturopathic approaches can also be considered. The water itself does not have to be treated, only the underlying disease.
With larger amounts of water in the pericardium, there is a higher acute risk, which is why a puncture and discharge of the pericardium is often necessary. For example, with bacterial infections, new fluids are constantly produced. As long as the infection and thus the underlying disease has not healed, the amount of water in the pericardium will increase. With higher amounts, the pericardium fills up and puts pressure on the heart.
Since the heart muscle is constantly tensing and relaxing again when it beats, its function is restricted when pressure is exerted on the heart from outside, as is the case for example. B. is the case with larger amounts of water in the pericardium. The external pressure prevents the heart from fully relaxing and being able to take up blood volume, resulting in heart failure. As a result, the body is no longer supplied with sufficient blood. In an acute emergency, this condition is also referred to as "cardiac tamponade".
As a result of the restricted heart capacity, palpitations, shortness of breath, dizziness and sweating develop. In the worst case, cardiovascular arrest occurs. In these cases, the patient must be transferred to the intensive care unit and, if necessary, the pericardium punctured to drain the fluid. As long as the underlying disease is acute and not resolved, a drain can also be inserted into the pericardium for a few days so that any newly created fluid can drain away.
Symptoms
Are only small amounts There is water in the pericardium, only kick few to none Symptoms on.
However, if there is a lot of fluids, a variety of complaints occur due to the fact that the Heart constricted in its pericardium and cannot properly expand during contraction or pumping. This allows the Heart chambers no longer filled with sufficient blood and the volume of blood ejected will decrease. This leads to symptoms similar to those of one Heart failure correspond: blue lips, shortness of breath, increased breathing rate, low physical endurance, congested neck veins and possibly also to cough, Loss of appetite and restlessness.
water in the lungs
Often, when there is water in the pericardium, water accumulates in the lungs. The doctor then speaks of a pleural effusion.
Strictly speaking, the water is not found in the lungs themselves, but between the leaves of the lung membrane and lies on the outside of the lungs. A watery effusion in the lungs is much more common than water in the pericardium. However, the lungs can hold significantly more fluid than the pericardium without restricting the breathing function of the lungs. Therefore, pleural effusions do not lead to a life-threatening emergency situation so quickly.
Even with a pleural effusion, the water collects at the lowest point due to gravity. However, the amount of fluid can quickly increase and press on the lungs from the outside. This hinders the expansion of the lungs and limits their function. In these cases, the effusion must be punctured and drained to the outside using a needle. This is usually done under local anesthesia; anesthesia is usually not necessary.
In addition to infections, many internal diseases can also lead to an effusion of water in the lungs. A common cause is e.g. the heart failure. The heart, which is no longer able to pump the blood volume adjusted to the needs of the body in the case of heart failure, prevents the flow of liquid blood. The blood in the blood vessels congests until the blood is forced out of the blood vessels by the high pressure and accumulates in the lungs. Infections and heart diseases in particular can lead to joint effusions of water in the pericardium and the lungs.
diagnosis
The method of choice for diagnosing pericardial effusion is Ultrasound diagnostics (Sonography), in which the water in the pericardium can be represented graphically.
Also one Computed tomography (CT) can be used to visualize fluid between the two membranes of the heart. After pictorial confirmation of the water accumulation, a Fluid withdrawal undertaken from the pericardial cavity (Puncture) to this on possible pathogens or cancer cells to investigate.
Also in EKG The accumulation of fluid can be noticeable; those affected often show one decreased rash in the ECG recording.
Complications
The dreaded complication of the accumulation of water in the pericardium is the so-called pericardial tamponade. This is a massive dysfunction of the heart, which is caused by a very strong accumulation of fluid in the pericardium. The heart is then barely able to pump properly, the heart chambers are barely filled with blood and the compression barely ensures blood flow to the heart. In extreme cases, this can even lead to life-threatening circumstances if enough blood can no longer be ejected from the heart to supply the body.
Read more at: Pericardial tamponade and Pericardial effusion
therapy
The therapy for pericardial effusion can be very variable and depends largely on the underlying cause. Small accumulations of fluid in the pericardium usually need no therapy, bigger should relieved by punctures to avoid complications.
The attending physician will issue a Needle inserted into chest under ECG control and advanced into the pericardium in order to then withdraw the fluid from the pericardium via a cannula. However, if the amount of fluid is so large that it can no longer be removed by a simple puncture, that is too Place a pericardial drainage into the pericardium, which then drains the fluid continuously through a kind of catheter.
Is the pericardial effusion infectious, is often also the Administration of antibiotics, anti-inflammatory Painkillers indexed. However, no conservative therapy addresses or occurs recurring effusions, can often only have one surgical intervention Remedy: Here a kind of small hole or window is cut in the pericardium (Pericardial fenestration), through which the accumulated liquid can escape. Only in the rarest of cases can a complete removal of the pericardium (Pericardectomy) to be necessary.
How to puncture water in the pericardium
If you have water in your pericardium, this can very quickly lead to serious complications. For example, a constriction of the heart leads to a loss of function with a significantly reduced amount of blood which is pumped into the circulation. Occasionally, conservative (wait-and-see) therapy is sufficient by treating the cause of the water retention.
However, a puncture is often required. The water can be drained from the pericardium. Usually, the fluid from the pericardium is also used for further examinations. The puncture is usually performed ultrasonically with a long needle or syringe. The liquid can be collected directly using the syringe so that it can be used for further diagnostic purposes.
Also read: Puncture
Duration
The duration of the accumulation of water in the pericardium depends on many factors. Most of the time, the accumulation of fluid recedes once the cause has been eliminated. Acute accumulations of large amounts of water or a lot of blood in the pericardium usually have to be emptied very quickly, otherwise serious consequential damage can occur. If the water arises as part of a chronic illness, such as chronic kidney disease, heart failure or chronic heart failure, it can also remain permanently.
causes
The most common causes of water retention in the pericardium include a wide variety Infectious diseases, such as tuberculosis, diphtheria, Coxsackie viruses, HIV or Herpes. Existing ones can also be used in the same way Autoimmune diseases, as the Rheumatoid arthritis or the Lupus erythematosus cause pericardial effusion.
Other triggers can be Metabolic diseases (e.g. uremia), malignant tumors or metastases, trauma, or a Heart attack be. Less often can too medical interventions lead to water in the pericardium at the heart, e.g. after operations, Pacemaker implantations or after radiotherapy in the chest area.
Water in the pericardium after a heart attack
Up to 30% of people have water in their pericardium following a heart attack. If this does not cause any additional symptoms, it does not affect the healing process and does not need to be treated. However, the water can also arise with an autoimmune inflammation of the pericardium. In addition to the build-up of fluid, there may be fever and chest pain. This clinical picture is called Dressler's syndrome. The inflammation usually develops in the second to third week after the heart attack, but can also occur days to weeks after the heart attack. In very rare cases, the water in the pericardium can prevent the heart from expanding, thereby disrupting its pumping function. In such a case it is necessary to drain the liquid.
You might also be interested in this topic: Consequences of a heart attack
Water in the pericardium after an operation
The accumulation of fluid, especially blood, in the pericardium is a common side effect of the operation after cardiac operations, especially after bypass operations. This is usually harmless and in the majority of cases disappears by itself. Tamponade (a disturbance of the heart function as a result of pressure) occurs less frequently and the doctor must then empty it as quickly as possible
In very rare cases, fluid may accumulate in the pericardium after a pacemaker or stenting. The procedure could have damaged the coronary arteries and lead to permanent bleeding. The heart muscle itself can also be injured. In the case of elderly patients in particular, the surgical tool can damage the heart wall in such a way that it tears or becomes permeable. In any case, it is an acute emergency, as it can lead to pericardial tamponade.
Postcardiotomy syndrome can rarely occur after heart surgery. The cover of the heart becomes inflamed due to the physical irritation during the heart operation. No pathogens are involved in this inflammation. Nevertheless, in addition to the water in the pericardium, a fever can occur.
Read more on the topic: Cardiac bypass
Water in the pericardium after pneumonia
In pneumonia, the body's immune reaction causes inflammatory cells to flood in along with fluid. This usually accumulates in the lungs. In the case of pronounced findings, however, fluid can also enter the pericardium (heart sac), so that water accumulates in the heart sac. The most serious complication is the pericardial tamponade, in which the pericardium is so bulging with fluid that the heart does not have enough space. There is a deterioration in pumping performance and as a result, heart failure can occur.
Read more here: lung infection
Water in the pericardium in cancer
In the context of cancer, fluid can accumulate in various cavities in the body. These are known as malignant effusions. The causes of fluid development are numerous.
On the one hand, the tumor itself, for example through excessive growth of the lymph nodes, can cause lymphatic congestion and an effusion. Organs such as the heart, kidneys or liver are often damaged by the harmful influence of the tumor.This can lead to imbalances in the blood, which lead to water retention and effusions in many areas of the body, including the pericardium.
It is not uncommon for the accumulations of fluid to arise as a secondary consequence of the destruction of the tumor. Infections with fungi, viruses or bacteria can also develop favorably and lead to water in the pericardium. Cancer types that lead to water retention in the pericardium in particular are breast cancer and lung cancer, but also leukemia.
Water in the pericardium during chemotherapy
Chemotherapy involves drugs that are directed against cancer cells and are intended to hinder and destroy their growth.
The means that are administered differ with each type of cancer and thus cause different side effects. In many cases, chemotherapy can also attack the body's own cells, which leads to the many side effects.
Some cancer drugs are also classified as toxic to the heart, which means that they attack the cells of the heart. The destruction of the heart cells can also cause dangerous water retention in the pericardium. In many cases it cannot be determined exactly whether the cancer itself or the chemotherapy caused an effusion in the pericardium.
Radiation therapy, another pillar of cancer treatment, can damage heart cells and lead to effusions. The heart is particularly at risk in the case of cardiac tumors, lung tumors or tumors of the middle layer in the chest. Long-term effects can occur here even decades after the cancer disease.
Water in the pericardium in anorexia
Anorexia can cause water to accumulate in the pericardium. Serious complications rarely occur. Rather, it is an expression of the severity of anorexia, because the lower the BMI (body mass index), the higher the probability that water will accumulate in the pericardium. When the weight is normalized, however, the water in the pericardium usually also disappears. The accumulation of water is caused by the decrease in the muscle mass of the heart and the fat tissue surrounding it, so that the heart becomes relatively too small for the pericardium.
Another explanation is that anorexics often have too little protein in their blood. The protein usually holds the liquid back in the jar. If there is too little protein, then it is more likely to accumulate fluid in body cavities. This is also what causes hunger edema.
Also read our topic: anorexia
Water in the pericardium of the baby
It is very rare for babies to accumulate water in the pericardium. The main causes are bacterial or viral infections, but also effusions after heart operations. In the fetus, fluid buildup during pregnancy can be a sign of serious medical conditions such as a Hydrops fetalis, a serious childhood heart defect, heart tumors or genetic diseases (trisomy 21, ...).
Read more on this topic at: Hydrops fetalis



















.jpg)