Ligament stretch at the ankle
Synonyms
Supination trauma, pronation trauma, ligament stretching, ligament tear, ligament lesion, distortion trauma
definition
Injury to the upper ankle joint (ankle joint) often occurs during sporting activities, but also in everyday life. Most events do not lead to serious structural damage, i.e. injury with permanent consequences. Nevertheless, it can lead to a torn ligament, especially come in the area of the outer ankle. When the doctor examines the ankle, they can hardly be distinguished from stretched ligaments or partial ligament tears or complete ligament tears. The transition is fluid.

introduction
An ankle injury is common and usually harmless. In some cases, however, a supposedly harmless ligament stretch can have permanent consequences with pain and restricted mobility of the injured ankle.
Magnetic resonance imaging (MRI) is only performed on very few ankle injuries to determine the extent of the ligament damage.
A magnetic resonance tomography is a magnetic examination - i.e. free of X-rays - which shows layer images of the ankle.
The treatment concept usually provides for conservative therapy. Even if most ligament injuries heal without consequences, it happens again and again that patients complain of persistent pain and restricted mobility or of permanent instability of the ankle. In order to avoid the consequences of such injuries, physiotherapeutic treatment is of great importance.
The most common injury mechanisms in the ankle area include twisting ankle while running or landing after a jump.
In the vast majority of cases, the foot is twisted to the outside, resulting in what is known as "supination trauma".
The much rarer ankle twisting to the inside is called "pronation trauma".
However, this description of the type of injury does not say anything about which structures of the ankle were injured.
The most common consequence of injury is damage to the capsule and ligaments (capsule-ligament apparatus) of the ankle. A thorough examination immediately after the occurrence of the injury often provides an initial indication of the severity of the injury. However, a final diagnosis is often only possible through the use of imaging methods (x-ray, magnetic resonance imaging).
In principle, every twisting injury with development of a significant swelling should be x-rayed to rule out a break. Depending on the exact mechanism of the accident, the following fractures can occur:
- Outer ankle fracture
- Medial malleolus fracture
- Fracture of the lower leg
- High fibula fracture (Maissoneuve fracture)
- Fracture of the 5th metatarsal
Please also read our page Ligament Stretching - An Overview
Appointment with ?

I would be happy to advise you!
Who am I?
My name is I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
Athletes (joggers, soccer players, etc.) are particularly often affected by diseases of the foot. In some cases, the cause of the foot discomfort cannot be identified at first.
Therefore, the treatment of the foot (e.g. Achilles tendonitis, heel spurs, etc.) requires a lot of experience.
I focus on a wide variety of foot diseases.
The aim of every treatment is treatment without surgery with a complete recovery of performance.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You can find me in:
- - your orthopedic surgeon
14
Directly to the online appointment arrangement
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
Further information about myself can be found at
therapy
The therapy for ligament stretching is often very simple.
Here the patient should proceed according to the so-called PECH scheme:
- In this case, the P stands for a pause that the patient should absolutely keep. It is important that the therapy in the case of ligament stretching can only lead to an improvement in the symptoms if the patient does not repeatedly overload the ligament. You should definitely take a break from exercising, and the tape should be spared as much as possible for the first 2 days.
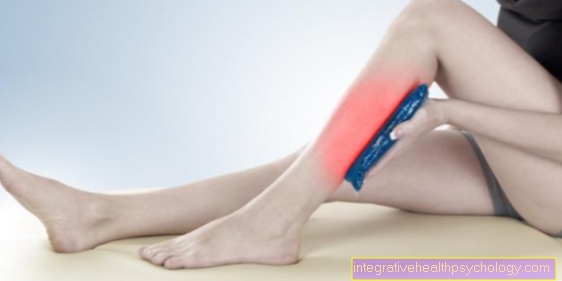
- The E stands for ice, whereby it is mainly about the cooling of the pulled ligament. If a patient notices that he has torn the ligament, he should place an ice pack on the affected area as soon as possible in order to relieve swelling and pain. An actual therapy for ligament stretching is not based on the cooling, but the cooling leads to a relief of the symptoms.
- The C in the PECH scheme stands for compression. Although it is not always possible to wrap the affected joint with a pressure bandage, it is possible, so the patient should try to relieve the strained ligament with the pressure bandage.
- The H indicates that the affected joint should be raised high. Elevation is not always possible, especially in the shoulder area, but if the knee or ankle is affected, the affected leg should be elevated.
Another possibility of therapy for ligament stretching with severe pain is drug treatment. For example, gels that relieve pain and swelling can be applied to the affected area. The patient can also take pain relievers to reduce pain. It is important to mention, however, that pain medication is not actually a therapy for ligament stretching but can only alleviate the pain and swelling associated with it.
Nevertheless, taking a break from exercising and relieving the stress on the affected joint has absolute priority, as this is the best therapy for ligament stretching. The affected ligament can only regenerate by taking a break from exercising without being torn again when the stress is repeated.
If a ligament strain is not treated with a sufficient break, a ligament rupture can occur more quickly with renewed exercise. That is why a break in sports for a few days is absolutely essential. If the ligament is severely pulled, an orthopedic surgeon or trauma surgeon can also prescribe stabilizing splints (for example for the knee or ankle joint). These help the patient not to expose the pulled ligament to the full body load but distribute the load adequately. This therapy of ligament stretching is mainly used for severe strains or if the patient is very prone to ligament strains. The splints are usually worn for a week.
Physiotherapy for ligament stretching
Early functional treatment phase
The early functional follow-up treatment of a ligament stretch / torn ligament begins in the first few days after the injury and is important for the fastest and optimal healing possible. Ankle injuries cause pain and swellings in the ankle, which limit the mobility of the ankle.
The early functional treatment is usually carried out as part of physiotherapy.
The main goal of early functional treatment is to restore full mobility in the affected ankle as early as possible.
In physiotherapy, this can be done, for example, through exercise therapy in the sense of PNF treatment (proprioceptive neuromuscular facilitation). The intensity and type of load can be easily adapted to the current performance capacity.
You can find more information on physiotherapy on the following page: Physiotherapy
Coordination and proprioception training
A very essential, if not the most important aspect of the follow-up treatment of an ankle joint injury, however, is the training of coordinative and proprioceptive skills.
If, after the first two phases of treatment, good mobility of the ankle joint and minimal pain can be achieved, training these two skills has top priority.
Coordination training means improving the interaction of the muscles that are responsible for the stability and movement of the ankle.
Proprioception means the ability to safely ensure the perception and control of one's own body in space. The word "sense of balance" is probably an acceptable translation of the term "proprioception".
Training these two skills is difficult to differentiate and is hardly possible in isolation, since almost every coordinative action also requires a high level of proprioceptive skills. The reverse is also true.
In practice, proprioceptor or coordination training for the ankle joints should be carried out barefoot, if possible, since wearing socks can prevent important training stimuli.
The structure of the exercises or the sequence of exercises depends on the patient's ability to perform as well as his or her individual demands on everyday life.
Exercises that seem simple at first glance already demand a considerable amount from ankle patients coordinative skills.
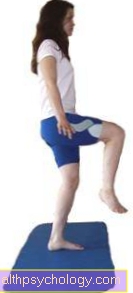
For example, standing on one leg on an exercise mat is one of the tasks that require a high level of body awareness and balance.
At the end of this therapy phase, it is essential to develop dynamic stability during movement.
This can be trained very well, for example, by running exercises on a mat or on a mini trampoline.
The coordination and proprioception training is primarily geared towards the demands that everyday life places on the respective patient. A professional footballer certainly needs a different form of rehabilitation than a person who mainly performs sedentary activities and is not very active in sports. The muscular and coordinative starting conditions are completely different here.
Nevertheless, sufficient stability and mobility in the ankle are important for every ankle injured. For younger patients or those who are physically active, a so-called "Run ABC " or one “Jump school" on.
At the "Run ABC“Different forms of running, such as hopping, deliberately rolling over the ankle joints, or skipping (pulling the knees up to about hip height) are developed.
In the "Jump school“The most varied types of jump (two-legged jumps, one-leg jumps, jumps over hurdles, etc.) are trained with the patient according to methodically coordinated aspects.
Follow-up treatment for an ankle injuries is offered by any physical therapy practice.
More sporty ambitious patients who want a running school or a sports doctor-specific advanced training are with a specially trained one Sports Physiotherapists better off.
A look at the websites of the local physiotherapy practices will help you to get an overview of which practice offers appropriate sports physiotherapy.
Conservative therapy options for ligament stretching
Taping when the ligament is stretched
Stabilization of the ligament apparatus and the entire joint is essential for the healing of a ligament stretch.
The advantage of taping is that the functionality of the joint is still retained.
Sports tapes are now available in every pharmacy, but improper use can even worsen the injury. For this reason, the person concerned should always have a doctor, physiotherapist or other specialist demonstrate how to affix it correctly. The function of a tape bandage is that the tape strips on the skin transfer the forces that occur in such a way that the ligament apparatus and thus the stability of the entire joint are supported. The tissue swelling associated with the injury can also be reduced.
Read more on the topic: Knee tape
Ointment for a ligament stretch
Symptoms of ligament stretch can often be treated with nonprescription drugs.
These include, above all, ointments that are applied locally to the affected area. This eliminates side effects such as stomach pain, which can occur, for example, when taking painkillers in tablet form.
Pain relief ointments such as the well-known Voltarengel contain nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen or diclofenac, which have an analgesic and anti-inflammatory effect. Applied regularly and early, they help relieve the symptoms of ligament stretching. Special sports ointments are also available.
These often contain natural ingredients such as menthol, which are said to have a cooling and decongestant effect. The application of a cooling ointment bandage is particularly recommended.
To do this, the ointment can be stored in the refrigerator beforehand and the foot can then be wrapped with a bandage after the ointment has been applied. Certain ointments can also be applied to counteract the bluish discoloration that occurs when small blood vessels bleed into the tissue. Creams with natural ingredients or heparin ointment can be used for this.
More information on the topic: Treatment of a ligament stretch
Duration of a ligament stretch
Ligament stretching or ligament strain is one of the lighter ligament injuries.
Ligament stretching is usually only associated with temporary functional impairments and symptoms.
Nevertheless, if you suspect a ligament injury, it is advisable to consult an orthopedic surgeon to be on the safe side. This can rule out more serious injuries such as torn ligaments or even broken bones.
Complications rarely arise, so that the ligament stretch usually heals without problems. The pain and swelling should subside after a few days.
During this time, excessive exertion and exercise should be avoided, but absolute rest is not necessary. The pain and swelling that typically occurs immediately after the injury, as well as the often associated bruise, should subside significantly after 1 to 2 weeks. If this is not the case, a doctor should be consulted (again). As soon as the symptoms have completely subsided, the foot can be put back under load as usual.
Duration of healing of a ligament stretch? Read here.
Bruising from a stretched ligament
In addition to severe pain and swelling, a stretched ligament often leads to a bruise after a few hours (Hematoma).
Contrary to popular opinion, this is also the case if only individual fibers of the tape have torn and the tape as a whole is merely overstretched and not torn.
The cause is the rupture of small vessels, which subsequently bleed into the surrounding tissue and are thus externally visible as a bruise. Since the injury here is close to the skin surface, the bruise occurs relatively quickly after the injury and takes on different dimensions depending on the location and severity of the injury.
One often provides relief Immobilize and Elevate of the affected foot, as well as the cooling or creating one Compression bandage.
In addition, pain relief ointments or cooling gels can be applied. Heparin ointment can help by preventing blood clotting (class of anticoagulants). Applied 2 to 3 times a day, it reduces the swelling and ensures that the blood clots in the vessels under the skin dissolve more quickly, making the bruise increasingly faded.
Causes of ligament stretch
Ligament stretching or straining can have various reasons.
The most common cause of ligament stretching is distortion or incorrect movement while exercising. Especially if a patient has not warmed up sufficiently before training, it can with Overuse of the ligaments (Ligaments) or ligaments can quickly stretch if the movement is incorrectly performed.
But it is not only in sports that a ligament can be pulled. Another cause of ligament stretch is when a patient is with her Highheel twisted or if a patient makes a generally awkward movement.
Violent trauma, such as a fall or a blow to the knee, can also be the cause of ligament stretching. Here it is especially important to differentiate whether the patient has the tape "just"Has overstretched or whether there is a tear in the band (please refer: Torn ligament) came. This is very painful and leads to an unusual (pathological) Mobility of the affected joint, sometimes also to misalignments (Dislocations) of the joint. However, the most common cause of ligament stretching or even tearing remains sport.
Especially sports that involve an abrupt stop or change of direction are predestined for ligament strains. Thus, sports are like Soccer, tennis, basketball or Handball a particularly common cause of ligament stretching.
Symptoms of a ligament stretch
The symptoms of a ligament stretch can vary widely and depend, among other things, on how often the patient has already pulled the ligament and how severe the strain is.
After a while, many athletes hardly notice any tension in the ligaments at all, as they become more flexible after a while. This phenomenon can be observed especially in a ballerina or a figure skater.
If they still have symptoms of ligament stretching at the beginning, such as pain or slight swelling, after some time with a little practice they can manage the splits without pain.
The reason for this is that the ligaments are elastic and become even more elastic after a while due to permanent overstretching.
However, if there is an acute ligament stretch, symptoms are completely normal.
Typical symptoms of ligament stretching include pain and swelling in the affected joint. For example, has a footballer pulled a ligament (Ligament) is drawn in the knee, acute pain and swelling in the knee area occur. Pain and swelling are usually caused by:
- cooling
- Elevation and
- Immobilization of the knee
better.
The symptoms of ligament stretching, on the other hand, worsen if the patient tries to put pressure on the affected joint and continues to exercise. The joint often hurts even with small loads, such as simple walking. However, it is important to differentiate between a torn ligament and a stretched ligament.
If the ligament is torn, the symptoms are more pronounced than if the ligament is pulled.
A torn ligament, on the other hand, results in unusual mobility, for example the patient can move the lower leg abnormally due to a torn ligament in the knee (pathological) turn inwards or outwards (rotate). The formation of a hematoma is also more likely to indicate a torn ligament.
These symptoms are not all present with ligament stretching. Here the joint remains stable and the patient can step (albeit with pain) and perform normal movements. If the ligament is stretched, symptoms such as bleeding (Hematomas) only extremely rarely. Furthermore, despite the symptoms, the patient can put strain on the affected joint if the ligament is stretched. The joint is also stable.
Read more about: Symptoms of Ligament Stretching
forecast
The prognosis of ligament stretching is, if it has been adequately treated, mostly very good. Especially if it's a first-time ligament stretching acts, it can heal without any further damage. Still, it is very important that the patient look after the ligament strain sufficiently gentle so that there is no consequential damage.
However, if a patient treats his ligament strain adequately and if he takes the sports break prescribed by the doctor, the prognosis of a ligament stretch is generally very good. Nevertheless, it can be the case that patients who repeatedly overstretch their ligaments have to reckon with consequential damage. Due to the recurring (recurrent) Overuse of the ligament (ligament) it can happen that the elastic Tape extends so farthat it no longer finds its way back to its original form.
This is the case, for example, when the Ligaments around the hip again and again by one Balancing act were overloaded. In this case, the long-term healing prognosis is slightly worse. The fact that the tape is becoming more and more elastic and has to keep expanding can mean that the necessary stability is no longer guaranteed.
This can lead to a so-called Dislocation of the femoral head (Femur) come. The head of the thigh slips out of the hip joint socket (Cox) because the ligaments can no longer guarantee sufficient stability.
Even with one Overstretching of the ligaments on the shoulder is this possible (shoulder dislocation). In this case, the prognosis for a cure is worse. In general, however, such consequential damage only occurs when the patient does his Ligaments often or permanently pulled and overstretched.
If a patient spares the ligament strain, consequential damage is rare. Still, an overstretched or Torn ligament is more prone to torn ligament and thus instability in the joint. A Torn ligament, especially a cruciate ligament tear, has one far worse prognosis than ligament stretching. This makes it all the more important to protect the torn ligament as well as an adequate therapy, since in this case a very favorable prognosis for ligament stretching can be expected.
diagnosis
The diagnosis of a ligament stretch can usually be made with the help of an anamnesis, i.e. a conversation with a specialist doctor (Orthopedic surgeon or trauma surgeon).
Based on the description of the mechanism of the accident, the doctor can often conclude that the ligament has been pulled.
In addition, the affected joint should be examined. This is where the diagnosis of ligament stretching can best be distinguished from a ligament tear. During the examination, the affected joint is examined in detail.
The most important thing is whether the patient has pressure pain in the area of the joint, whether swelling or even a bruise (Hematoma) is present as well as whether an abnormal (pathological) There is mobility of the joint.
The examination can then be used to diagnose a ligament stretch. If the doctor notices a pathological mobility of the affected joint, a torn ligament is likely and additional diagnostics, for example an X-ray or an MRI of the foot, may have to be carried out.
More on this topic at: MRI of the ankle
There are specific tests for each joint and ligament to help doctors distinguish a diagnosis of ligament stretching from a ligament tear. For example, there is the front and rear drawer test on the knee joint.
With the help of these simple examinations, the doctor can differentiate between a cruciate ligament tear or an overstretching of the cruciate ligament. If the test results are positive, this means that the knee is pathologically mobile. Thus, the diagnosis is not ligament stretching but rather a ligament tear, in this case a tear of the anterior or posterior cruciate ligament.
In general, most ligaments in the human body have a specific test to confirm the diagnosis of ligament stretching. Nevertheless, it can be the case that a reliable diagnosis cannot be made despite an expert examination.
In this case, an X-ray or an MRI image is indicated in order to assess the structure of the ligaments by imaging.
Figure outer ankle
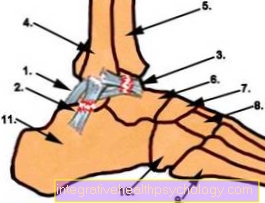
- Ligamentum fibulotalare posterius
- Fibulocalcaneare ligament
- Ligamentum fibulotalare anterius
- Fibula
- Shinbone (tibia)
- Talus bone
- Scaphoid bone (navicular bone)
- Sphenoid bone (os cuniforme)
- Metatarsal bone
- Cuboid bone (Os cuboideum)