Endocrine orbitopathy
synonym
Endocrine ophthalmopathy
introduction
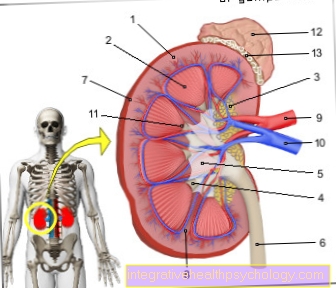
Endocrine orbitopathy is a condition that affects the eyes and their sockets (called the orbit). It belongs to the group of organ-specific autoimmune diseases. This includes all diseases that attack the body and its organs through misdirected processes and functions of the body's own immune system. This attack can either take place on the entire body (this is called organ-unspecific) or it can be restricted to individual organs or organ systems (i.e. organ-specific), as is the case with endocrine orbitopathy. The majority of patients with endocrine orbitopathy develop this symptom as part of a thyroid dysfunction.
In general, it can be said that thyroid disorders affect women much more often than men.

Detecting endocrine orbitopathy
What are the symptoms of endocrine orbitopathy?
Endocrine orbitopathy is relatively easy and quick to recognize even for the medical layperson: the eyes of the affected patient protrude from their eye socket (in technical jargon this is called exophthalmos) and the upper eyelids appear pulled up (also called eyelid retraction), so that the eyes appear unnaturally large and wide open. However, the size and volume of the eyes themselves do not change with endocrine orbitopathy. The changes described can be traced back to a structural as well as volume change in the muscle tissue, the connective tissue and the adipose tissue that is located behind the eyes in each of us. As it increases and swells, the eyeballs are pushed out forwards, so to speak, giving the impression of being swollen themselves. Endocrine orbitopathy almost always occurs in combination with other symptoms. Mostly these are an enlarged thyroid gland (a so-called thyroid goiter) and a racing heart (a Tachycardia). These three symptoms are commonly referred to as so-called "Merseburg Triassic“Together and they classically occur in Graves' disease. The name of this triad of symptoms is derived from the person who first described it, the doctor Carl Adolph von Basedow from Merseburg, who published it scientifically in 1840 under this name.
Endocrine orbitopathy usually occurs on both sides, but in principle can only occur in one eye. In most cases, both eyes are not equally severely affected (however, the specialist literature disagrees here about the study situation).
How is endocrine orbitopathy diagnosed?
The diagnosis of endocrine orbitopathy is primarily made clinically by the examining doctor, which means that the patient's appearance is such a clear indication of the disease that the laboratory tests basically only serve to confirm. Exophthalmos (protrusion of the eyeball), typically in combination with a racing heart and an enlarged thyroid gland, is typical for Graves' disease.
Further diagnostics such as blood tests and imaging methods are used to determine the severity of the disease and to assess the course. Nuclear magnetic resonance spectroscopy (NMR) has proven to be particularly suitable. In any case, it must be ruled out that a tumor located behind the eye is responsible for the exophthalmos.
If no hormonal involvement can be found in the blood analysis, it is not an endocrine orbitopathy. In order to be able to document the course of the endocrine orbitopathy uniformly, it is divided into six different stages:
- Stage 1: the retraction of the upper eyelids
- Stage 2: the eyelids swell and the conjunctiva of the eyes becomes inflamed
- Stage 3: exophthalmos
- Stage 4: the eye muscles are restricted in their mobility, double vision occurs
- Stage 5: the cornea shows initial damage
- Stage 6: compression of the optic nerves leads to a deterioration in vision, possibly glaucoma (glaucoma)
Treat endocrine orbitopathy
How is endocrine orbitopathy treated?
Unfortunately, a causal therapy has not yet been developed. However, it is possible to treat the symptoms and thus help the patient. Cortisone is the first choice here. If the effect is not yet sufficient, other preparations are available. In order to maximize the effectiveness of the therapy, it is important that there is interdisciplinary collaboration, especially between the departments of internal medicine, radiation therapy, ophthalmology and specialist surgeons.
Visiting a psychologist is also described by the patient in many cases as being very relieving and relieving.
Despite all efforts, an improvement in symptoms can unfortunately only be achieved in about 30 percent of all those affected.In 60 percent, the condition remains unchanged and in 10 percent even a deterioration is recorded. The therapeutic measures are primarily aimed at containing the inflammatory processes in the eye socket and preventing consequential damage to the eyes.
Due to the constant protrusion of the eyes and the sometimes incomplete eyelid closure, it is necessary to keep the eyes artificially moist in order to prevent the cornea from drying out and tearing. Special eye drops and eye ointments can help.
In addition, the thyroid malfunction (if it exists) must be treated. In the long term, however, high-dose cortisone therapy also harbors certain risks and side effects: weight gain and mood swings can occur, or stomach ulcers can form).
Recent studies show that regular intake of selenium can slow the progression of endocrine orbitopathy. However, it is not yet part of the standard therapy in Germany.
Prevention of endocrine orbitopathy
What are the causes of endocrine orbitopathy?
The fact that it is still not possible for doctors to treat endocrine orbitopathy causally is due not least to the fact that the exact causes of the disease have not yet been fully researched.
Most likely an inherited autoimmune disease causes the body's own cells of the immune system to form autoantibodies against the so-called thyrotropin receptors. These receptors are the "docking points" for the body's own hormone thyrotropin (TSH for short), which is released to stimulate the thyroid gland to grow. These special thyrotropin receptors are not only found in the thyroid gland, but also in the tissue of the eye socket, where they can also react with growth to the hormone released.
Endocrine orbitopathy can be seen in about ten percent of all people with some form of thyroid disease. In over 90 percent it occurs in the context of Graves' disease and in around 60 percent in combination with an overactive thyroid (a so-called Hyperthyroidism).
Endocrine orbitopathy does not necessarily have to occur at the same time as a thyroid disease, it can be noticeable years later or much earlier. Scientists therefore assume that endocrine orbitopathy has its causes outside the thyroid gland and is subject to the same autoimmune processes as Graves' disease itself.
It is known that both genetic predisposition and environmental influences are relevant for the disease, which can be described as extremely complex. It has been found that patients receiving radioiodine therapy can sometimes develop endocrine orbitopathy or an already existing one becomes significantly worse in its course.
Endocrine orbitopathy and Hashimoto's thyroiditis (also known as Hashimoto's disease) occur together or entirely without any involvement of the thyroid gland.
Heavy nicotine consumption negatively affects both the severity of the disease and its clinical course.
Course of an endocrine orbitopathy
How does endocrine orbitopathy work?
The clinical characteristics associated with the disease are dynamic in their course and are primarily characterized by increased levels of inflammation and the structural change in the tissue behind the eyes and the eye muscles. In some patients, the eyes protrude so much or the upper eyelids are pulled upwards so much that it is no longer possible to close the eyelid completely. In these cases one speaks of a lagophthalmos. This in turn promotes the development of corneal ulcers.
In general, the course of endocrine orbitopathy is different in each patient and the disease is not always consistently active. Apart from the organic and functional accompanying problems with this disease, the cosmetic aspect should not be neglected either. The patients often feel stigmatized and avoided in everyday life, which leads to a very high psychosocial burden for the individual. In the course of time, science has established several treatment methods that combat the symptoms and clinical problems of endocrine orbitopathy. However, it is not yet possible to remedy the causes of the disease. So there is currently no causal therapy.
The development of an endocrine orbitopathy is the result of extremely complex, pathologically altered immune processes in the body. These are triggered by what are known as B lymphocytes and autoreactive T lymphocytes (white blood cells), which ensure an increased production of antibodies. These autoantibodies are directed against the structures of the thyrotropin receptors.
So-called fibroblasts, a special type of cell located in the tissue behind the eyes, react very strongly to inflammatory stimuli. They cause an increased formation of fat cells and an increase in the volume of the tissue.
Excessive nicotine consumption can have the same effect.
As a result of these inflammatory processes triggered by the body's own immune system, the entire tissue behind the eyes swells more and more and, as there is nowhere else to go, pushes the eyeball further and further forward. An exophthalmos develops (protrusion of the eyeball). Due to the permanent overstretching, the eye muscles also lose strength and stability and the patients suffer from double vision as a result. Another classic symptom is a diffuse growth of fatty tissue in the area of the eyes, also known as lipomatosis.