Hepatitis C.
causes
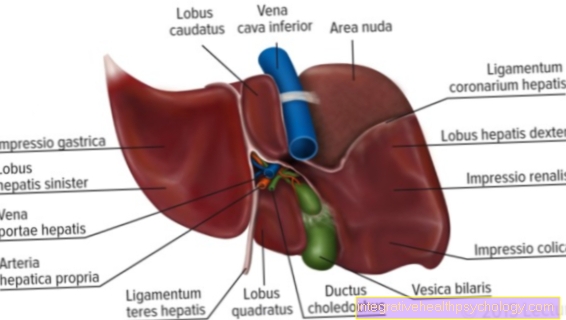
Hepatitis C is an inflammatory disease of the liver caused by the hepatitis C virus (HCV). The virus belongs to the group of flaviviruses and is an enveloped, single-stranded RNA virus.
Based on its genetic information, this virus can be divided into 6 groups (so-called genotypes), which are further subdivided into a total of 30 main types.

The genotypes differ in terms of where they occur more frequently (1-3 are found mainly in Europe, 4 almost exclusively in Africa) and how they respond to the various therapeutic options for hepatitis C.
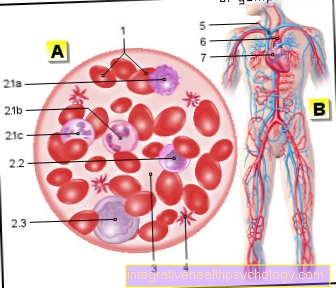
The hepatitis C virus is transmitted parenterally (literally translated: past the intestine) i.e. via blood and other body fluids. Infections are therefore particularly common in certain risk groups: Medical staff or nursing staff who deal with infected people, for example, have the risk of coming into contact with the blood of sick people via needlestick injuries and thus becoming infected.
Drug addicts who consume drugs such as heroin, who have to be injected into the blood, who share syringes, run a high risk of infection. Infections are also conceivable through other contaminated sharp objects such as piercing devices or tattoo needles.
In the past, there was also more frequent hepatitis C due to infected blood, but thanks to reliable test procedures for donated blood, this is almost impossible to record today. The same applies to the transplantation of liver (parts). The viral load in other body fluids besides blood (for example sperm, vaginal secretions, breast milk or saliva) is so low that the risk of infection is almost zero, although it is in principle possible. This is why sexual transmission is not as common as generally assumed (in contrast to hepatitis B!) And occurs almost only when special sexual practices are used in which there is an increased risk of bleeding due to injuries to the mucous membrane, such as anal intercourse .
Transmission from an infected mother to her child is also possible both during pregnancy and during delivery; the rate here is around 4 percent.
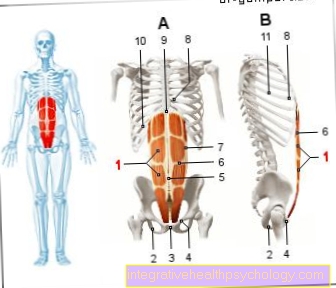
If the virus gets into the bloodstream, it works its way through the body and only affects liver cells. The exact mechanism that leads to the inflammatory reaction in the liver has not yet been fully clarified, but it is assumed that certain cytotoxic (thus causing cell death) Defense cells (Lymphocytes) are formed, which ultimately ensure that more liver cells die. This then ensures the typical symptoms of hepatitis, which result from the impaired functionality of the liver, in later stages especially jaundice (Jaundice).
The sexual transmission route in hepatitis C.
The sexual transmission route plays a subordinate role in hepatitis C compared to hepatitis B and HIV. This transmission route is very rare, but is favored by open wounds on the external or internal genitalia, such as hemorrhoids and genital warts. The risk of injury and infection is further increased by anal intercourse, “fisting” and shared sex toys. When kissing and having oral sex with healthy skin and mucous membranes, there is a very low risk of the transmission of the hepatitis C virus.
For more information, see: sexual transmission route in hepatitis C.
Can it be transmitted by kissing or exchanging saliva?
The hepatitis C virus is very rarely transmitted through sexual contact and usually only when there are open wounds.
In contrast, an exchange of saliva during kissing and oral sex with healthy skin and mucous membranes carries an even lower risk of virus transmission and is therefore almost negligible. In general, sexual acts are a rather disorderly risk of transmission of hepatitis C infection. Kissing and other oral sex practices are even less dangerous ways of transmission in this group. It plays almost no relevance.
Read more at: Transmission through saliva
Risk of infection through blood contact and blood transfusions?
The transmission of hepatitis C via blood contact poses a great risk of virus transmission. Most of the hepatitis C transmission routes take place via blood contact. Shared needles among drug addicts or contaminated tattoo needles are very often primarily responsible for an infection.
Needlestick injuries to hospital staff, for example, or blood transfusions are less dangerous in this group. The likelihood of infection from a contaminated needle in the hospital is less than one percent and the likelihood of infection via a blood transfusion has been 1: 5 million in Germany since testing from 1992.
Read more at: Transmission of hepatitis C through blood transfusions
Drug addiction
Drug addiction and the common use of a needle that goes with it are by far the greatest risk of hepatitis C infection. This so-called “needle sharing” ensures a relatively high level of contamination. About 90% of drug addicts who consume substances through the vein become infected with the virus. Infection with hepatitis C occurs because there is still infected blood from the previous user on the needle and can thus penetrate the body of the new user.
Further information can be found at: Transmission in drug addiction
Tattoo needles
Needles that are used for tattooing or piercing are at high risk of infection. If a high level of hygiene is not observed in this context, for example by not sterilizing the needles after use, there is a considerable risk of infection from contaminated tattoo needles. If there is a desire for a tattoo, care should be taken to select a studio that is clean and adheres to a high level of hygiene.
Dialysis as a possibility of infection
The risk of hepatitis infection due to virus transmission via dialysis is comparatively high. Modern equipment sterilization and patient blood tests have significantly reduced the risk of hepatitis C transmission. However, 10 percent of dialysis patients still have hepatitis C. Together with the drug addicts who take their drugs via the vein and are 90% infected, they belong to the patient group with the highest risk of infection.
Read more on this topic at: Transmission through dialysis
Contagion through breast milk?
Whether breast milk can be responsible for virus transmission remains a matter of dispute among researchers. Some studies have shown that breast milk can contain viruses while others have failed to make this observation. Unfortunately, it is still uncertain whether this creates a risk of infection for the child. However, the researchers agree on the issue that infection can occur during childbirth and that a high viral load in the mother's blood increases this risk. A caesarean section helps to keep this risk as small as possible.



.jpg)