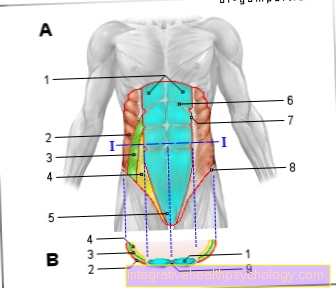
Jawbone structure
synonym
Jawbone augmentation
introduction
The so-called jawbone structure (technical term: Jawbone augmentation) primarily serves to restore lost bone substance.
An intact and break-proof jawbone is essential for the chewing process as well as for the overall aesthetics of the face.
Read more on the topic: Jawbone

Bone decline in the area of the chewing organ can have serious consequences, because in the worst case, perfectly healthy teeth can lose their anchorage and fall out. In addition, extensive bone loss can lead to visible deformations of the face and severe functional losses in the jaw.
Causes of jawbone decline
There can be various causes for the receding of the bony jaw. In a large number of cases, the bone regression is based on inflammatory processes in the oral cavity. An irregular or simply incorrectly performed oral hygiene forms the basis of this inflammation.
Read more on the subject: Oral hygiene
Plaque deposits on the tooth surface that are not removed can after a while penetrate under the gumline and attack the tissue located there. The first consequence is the formation of deep gum pockets in which bacteria can settle and multiply. In these areas, so-called gingivitis (Latin: gingivitis) usually develops first.
Read more on the subject: Inflammation of the gums
Inflammation of the gums, on the other hand, can spread to other parts of the tooth support system (lat. Periodontium), especially on the jawbone, and cause enormous damage. Dentists refer to this type of disease as an inflammation of the periodontium (lat. Periodontitis).
Read more on the topic: Periodontal disease
If no suitable therapy is carried out at this stage either, in almost all cases an inflammation-related regression of the jawbone follows. Removable dentures that put strong pressure on the jaw can also cause bone loss. Even after the removal of destroyed teeth, the jawbone usually reacts by breaking down the bone substance.
However, this bone decline is by far not as pronounced as the breakdown in the course of pressure load and / or inflammatory processes.
Materials for a jawbone structure
Jawbone augmentation can be considered for a variety of reasons. On the one hand, this procedure can be used to restore the aesthetics of the face; on the other hand, a planned implantation can make a jawbone augmentation necessary. This fact is due to the fact that implants can generally only be used in intact bones. In the event of tooth loss in the course of acute bone decline, the underlying cause must therefore be treated first.
The jawbone augmentation is then carried out. The actual implant can be inserted around four to six months after the jawbone has been built up. Various bone substitute materials can be used to build up the bone. So-called alloplastic bone (artificial bone substitute) usually comes from a human donor or from beef. This material is completely broken down by the organism within a few months after it has been introduced and replaced by the body's own bone material.
Autologous bone is bone material from the patient himself, which must be removed from another location beforehand. The most common sampling points are the ascending part of the lower jaw, the angle of the jaw, the chin and the iliac crest. The advantage of using this bone material is the lower risk of rejection reactions occurring.
The disadvantage is the fact that inflammatory processes and / or wound healing disorders can occur in the area of the removal site. In addition, so-called "Bone chips“Can be used to build up the jawbone. It is a biotechnologically produced bone substance that is implanted in the patient.
Performing a jawbone augmentation
There are various methods available to the oral surgeon to build up the jawbone. The bone material can be introduced by means of a horizontal / vertical augmentation using a bone block. Another possibility is what is known as bone splitting (Alveolar process splitting). Bone spreading (Alveolar process spreading) and distraction osteogenesis (Pulling the bone apart) are other options.
The socket preservation technique and the internal (or external) sinus lift are also used in a large number of patients. The jawbone augmentation through horizontal or vertical augmentation, medium jaw block, is the most frequently performed procedure.
It is particularly suitable for those patients in whom bone decline is particularly advanced. In the course of this procedure, the body's own (more autogenic) and donor bones (allogeneic bones) can be used.After opening the gums and preparing the remaining bone, the selected material is introduced into the areas to be treated and fixed with the help of small titanium nails or screws.
With so-called bone splitting (Alveolar process splitting) the remaining bone is split in the middle using a cutting disc. The two halves are then completely separated from each other with a hammer and chisel. In most cases, the surgical site has to be temporarily closed and the bone substitute material inserted a few days later, but in some cases the jawbone can be built up immediately.
The surgeon brings the selected replacement material into the cavities created by the bone division and mixes it with the body's own blood. The treated area can then be closed again with a gum suture. A jawbone augmentation is usually performed under local anesthesia. In exceptional cases, anesthesia can also be considered.
Is there a difference between upper jaw and lower jaw bone structure?
Not all bone structures are created equal and are strongly dependent on the side of the jaw. The anatomical bone structure means that the upper and lower jaw have very different structures. In the lower jaw, the bone substance is rather dense and hard, while in the upper jaw the bone substance is more honeycomb, porous and softer. The bone in the upper jaw is often weaker as a result. In addition, the bone in the lower jaw usually loses height when bone is broken down, while in the upper jaw it first loses width and then height. For this reason, a higher bone level often has to be restored in the upper jaw than in the lower jaw.
Furthermore, the inferior alveolar nerve in the lower jaw is anchored in the nerve canal within the bone. This is potentially at risk in the event of a surgical procedure, making it even more difficult. It is also decisive whether the bone width, density or height is to be restored or expanded, because the bone width is largely less problematic to restore than the bone height.
Risks of jawbone augmentation
In most cases, jawbone augmentation (jawbone augmentation) is tolerated by the patient without any problems. Risks are rather rare with this type of operation and can usually be treated easily if they occur. However, as with any surgical procedure, the dentist cannot guarantee absolute freedom from risk when augmenting the jawbone. Risks in the medical sense are divided into two groups. One speaks of so-called general risks (risks that exist equally in every operation) and special risks (risks that are specifically based on the respective type of surgical intervention).
The general risks also include infections, secondary bleeding and wound healing disorders when building up the jawbone. In general, these problems occur comparatively rarely and, if they occur, can be successfully treated by using an antibiotic or applying local coagulants. An opening of the maxillary sinus can represent a special risk of bone formation in the upper jaw. This, too, can be treated with antibiotic therapy if it occurs, without reducing the probability of healing or the bone material being less well accepted by the organism.
The structure of the jawbone in the lower jaw harbors various risks, such as injury to the large mandibular nerve (nervus mandibularis). The tongue nerve (nervus lingualis) is also potentially at risk during the jawbone development. Temporary loss of sensitivity in the supply area of these nerves are often the result. Permanent numbness or permanent loss of mobility of the tongue is rare. Depending on the material chosen (especially foreign material), allergic reactions or rejection reactions can occur in the course of the jawbone structure.
In very rare cases, cysts form in the area of the inserted bone.
It must also be noted that the operation is usually carried out with the application of a local anesthetic, and for this reason allergic reactions to this local anesthetic are also possible.
Read more on the topic: Local anesthesia at the dentist
Duration of jaw augmentation / duration of healing
Surgical procedures to reconstruct the level of the jaw can be a lengthy therapeutic process. The purpose of this intervention is either to produce sufficient bone for a subsequent implantation or, for example, to create a prosthesis bed for a full prosthesis. The duration of the jaw build-up depends on the complexity of the procedure.
Read more on the topic: Full denture
A bone build-up that takes place with bone chips and which is supposed to produce a bone build-up of 2-3mm takes much less time than a reconstruction with an iliac crest transplant, which is a major surgical procedure. The complexity is also decisive for the healing time. The healing time for smaller operations is about 6 months, but it can also be up to 12 months for large transplants.
The patient's general medical history plays a major role in this. With good healing and an intact immune system, the risk of infection or the rejection of the implant is low. If the transplant becomes infected by bacteria or viruses, the healing time may be greatly extended or a new intervention may be necessary because the body does not accept the transplant or it atrophies again immediately. Atrophy, the breakdown of the new bone, is always a complication that occurs less often with good general health.
Jaw augmentation for an implant - what should be considered?
If a jaw augmentation has to be carried out before an implantation, this represents a lengthy therapy process. After the operation, the bone graft must first grow in for at least six months before the implant can be inserted. The implant has to grow in again for about half a year. If the affected area is in the visible area, the patient may have to bridge this year's waiting period with a temporary solution.
Read more on the topic: Dental implant
Furthermore, it must be noted that some medications and general diseases make jaw augmentation and implantation difficult, if not impossible. One example of this is Parkinson's medication, which has been proven to hinder or even completely prevent the healing of transplants and implants. Immunosuppressants and drugs that affect bone metabolism such as bisphosphonates are also contraindications for surgery. The procedure cannot be carried out if the jaw growth has not yet been completed, in underage patients or in drug-dependent patients.
Pain in the jaw bone structure
During the jawbone augmentation (jawbone augmentation), pain is not to be expected due to the local elimination of pain in the area of the operation.
Most patients report only a slight feeling of pressure while inserting the bone material. After the jawbone has been built up, slight pain may occur, but this can be quickly relieved by careful cooling and the use of a mild pain reliever (analgesic).
Care should be taken here to ensure that no painkillers that have a blood-thinning effect (e.g. Aspirin®; ASA) are taken. Blood-thinning painkillers increase the risk of bleeding many times over. The pain should almost completely go away within the first week after the jawbone is built.
Diet for jawbone development
There are a few things to keep in mind about your diet for the first few days after performing a jawbone augmentation. In order to avoid the occurrence of pain and excessive strain on the operating area, you should refrain from eating too solid foods for the time being. Even meals with hard edges should be deleted from the nutrition plan for the time being.
After performing a jawbone augmentation, the patient does not usually have to go without specific foods. To this day, experts do not agree on whether dairy products such as cheese or yoghurt can be eaten without any problems. Many dentists assume that the bacterial pathogens that exist in this type of food have a negative influence on wound healing or can even provoke infections.
In order to strengthen the jawbone in the long term, patients should pay attention to a bone-friendly diet after a successful operation. This means that certain vitamins and trace elements should be consumed in sufficient quantities. On the one hand, bone substance requires a balanced calcium balance, which can be maintained through a diet with milk and dairy products. In addition, the fat-soluble vitamins (vitamin A and vitamin K) are essential for the jawbone. For the maturation of healthy collagen, a diet rich in vitamin C should also be observed.
Cost of a jawbone reconstruction
The costs of a jawbone augmentation are usually not borne by the statutory health insurance, which forces the patient to pay for all the sums incurred.
The actual amount of these costs depends on the initial state of the bone substance (and thus on the Scope of operation), as well as the chosen procedure. In addition, the prices of a jawbone augmentation differ enormously from doctor to doctor. Some oral surgeons offer jawbone augmentation for around 300-1000 euros, depending on the method chosen, others charge up to 3000 euros for the treatment.
The prices for a jawbone augmentation include all costs for the bone substitute material, the necessary consumables, the operating costs and the fee for the attending physician. When performing general anesthesia, there are usually additional costs for the patient.
Read more on the topic: General anesthesia at the dentist
homeopathy
Many homeopathic preparations promise strong teeth due to an increased ability to absorb calcium. However, naturopathy cannot achieve a specific bone structure on the jaw at a certain point. The preparations can only act as an accompanying therapy in addition to the surgical procedure in order to strengthen wound healing, the immune system and the bones. An individually suitable preparation and the optimal medication must, however, be discussed with the attending physician so that self-medication cannot lead to a diminishing therapeutic success.
Accordingly, the patient receives a potentized, highly diluted active ingredient that optimally suits the patient's therapeutic needs. The drugs of choice are the Globuli Symphytum, Calcium phosphoricum or Silicea terra.