Periosteum inflammation on the shin
introduction
The Clinical picture The periosteum of the tibia is mainly due to sudden, pressing pain marked in the area of the shin. These can radiate or be felt localized when moving in adjacent regions. Since it is mostly in addition to the Inflammation of the surrounding soft tissues comes, there is also often one swelling or Redness of the surrounding skin areas.

definition
Periosteum inflammation of the tibia is an acute or chronic inflammatory change in the periosteum (Periosteum). This spans the bone and is sensitive to pain. Their function is to protect and nourish the bones. The periostitis is also known as periostitis.
Periosteum inflammation occurs mainly in childhood and can have different causes. In principle, the periosteum of any bone can be affected by inflammation, with the tibia being affected relatively often. Periosteum inflammation of the tibia should be treated promptly to prevent the inflammation from spreading to the rest of the body. Numerous conservative as well as surgical measures are available for treatment.
Read more about this on our main page:
- Periosteum inflammation
Appointment with ?

I would be happy to advise you!
Who am I?
My name is I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
In order to be able to treat successfully in orthopedics, a thorough examination, diagnosis and a medical history are required.
In our very economic world in particular, there is too little time to thoroughly grasp the complex diseases of orthopedics and thus initiate targeted treatment.
I don't want to join the ranks of "quick knife pullers".
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You will find me:
- - orthopedic surgeons
14
You can make an appointment here.
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
For more information about myself, see - Orthopedists.
Causes of periosteum inflammation
The main cause of periosteum inflammation of the tibia is due to mechanical irritation and excessive stress. In young athletes in particular, inflammatory changes in the periosteum, which are mostly localized in the area of the shin, occur.
In the area around the shin there are a multitude of muscles, some of which are heavily used during sporting activities and so cause friction on the surface of the Periostes being able to lead. As a rule, the person concerned does not notice these friction processes. In the case of high or excessive physical exertion, this can lead to the development of an inflammatory reaction in the area of the periosteum of the tibia.
If you analyze the inflamed periosteum after taking a sample (biopsy) histologically with the aid of a microscope, edematous thickenings caused by the accumulation of tissue fluid can be determined in the area of the periosteum, which are based on the permanent mechanical stress. In addition to the inflammatory thickening, there is also an increased amount of connective tissue that was formed by the body to protect the mechanically stressed bone. Sometimes ossification occurs at an early stage, especially in the area of the muscle tendon attachments, which can also be seen as a protective measure for the body. On the other hand, these processes promote an increased inflammatory reaction in the area of the periosteum.
Periosteum inflammation can also be caused by bacteria. Most of the time, bacterial infection of the periosteum occurs due to the invasion of germs, such as Staphylococciwhich normally live on the skin without causing any pathological change. In the case of bacterial inflammation of the periosteum, the bacteria usually enter the skin area, for example via a small wound.
You might also be interested in these topics:
- Periosteum inflammation on the coccyx
- Periosteum inflammation on the knee
to jog
Jogging is one of the common causes of shin splint syndrome.
Too hard a floor covering when jogging plays an important role in the development of periosteum inflammation on the shin. Movement on the hard road surface stresses the muscles, tendons and muscle sheaths (fasciae). This can irritate the periosteum and become inflamed. Incorrect footwear and excessive strain promote the development of periosteum inflammation when jogging.
To ski
In addition to jogging, skiing can also lead to periosteum inflammation on the shin.
Skiing puts an enormous strain on the muscles. Those affected often carry out too one-sided and too intensive training, with which they overload their muscles. Risk factors for tibial splint syndrome are, in addition to overstrain, overtired muscles, a change in technique during movements and a change in the flooring.
Incorrect footwear and foot deformities can also promote the occurrence of periostitis. Skiers often train very diligently and for a long time. Inflammation of the periosteum on the shin bone can be a reaction of the periosteum to the increased pulling force of the muscles, tendons and fasciae. The periosteum is stressed so much by overloading and changes in movement sequences that it can become inflamed.
Symptoms
The most common symptoms of acute periosteum inflammation are sudden pain in the tibia. These are perceived and described as pressing and extremely uncomfortable, whereby the pain radiates and can consequently also be felt in adjacent anatomical areas such as the knee, the ankle or the foot. When moving, their localization can shift and they are often reported as increased by the patient, which leads to a subjective restriction of movement. Stinging or burning pain is rarely found in periosteum inflammation. Furthermore, the bone in the area of the tibia is tender on pressure, which manifests itself in a particularly strong sensation of pain as soon as one presses on an affected area of the tibia with a blunt object or with the hand.
Furthermore, swellings in the area of the shinbone occur relatively frequently, as there are also inflammatory changes in the soft tissues of the leg. Redness on the skin above the shin is also observed at times. As the tibia becomes warm, the five cardinal symptoms (redness, swelling, pain, overheating and functional impairment), which are characteristic of the presence of inflammation, are completed.
With severe inflammation of the periosteum, the entire body can increasingly be affected, which the person concerned notices through a general feeling of fatigue and even through a fever. Sometimes there is also the formation of pus and the development of visible small boils, which empty when pressure is applied. In the context of the maximum form of periosteum inflammation, purulent skin inflammation represents the full picture of periosteum inflammation that must be treated immediately.
For more information on causes of shin pain, visit:
- Shin pain
- Fatigue fracture on the shin
- Shin splints
therapy
Before treatment for periosteum inflammation can be started, it is important to find out what caused the inflammation, as the further course of action can differ fundamentally as a result.
In the event of chronic overload through sport, the leg should first be cooled and protected and appropriate sporting activities should be avoided in the near future. Symptomatic therapy using drugs such as ibuprofen or Voltaren makes sense, as these help the inflammation subside faster and reduce the existing pain.
If the periosteum has been triggered by the invasion of bacteria, antibiotic treatment must be started. There are numerous antibiotics available for this purpose, including those that are particularly well absorbed by the tissue. A parallel application of cooling and anti-inflammatory measures is advisable in order to quickly achieve a subjective improvement in the symptoms.
Read more on the topic:
- This is how long periosteum inflammation lasts
Use of medication
In the treatment of periosteum inflammation of the shin, anti-inflammatory painkillers are primarily used, such as from the group of non-steroidal anti-inflammatory drugs ibuprofen or diclofenac.
Furthermore, an inflammation of the periosteum of the tibia must be treated with antibiotics if it is caused by bacteria. Most often penicillins or the tissue-absorbing clindamycin are used, which should be used within a period of about one week. In exceptional cases, however, it may be that the specific pathogen does not respond to therapy with the usual broad spectrum antibiotics and can be adequately eliminated. As a result, a special analysis of potentially effective drugs, an antibiogram, must be carried out. This means that material containing the pathogen must first be obtained, for example, by a smear, and this must be analyzed in order to then begin a targeted antibiotic therapy. Depending on the pathogen, this can take up to several weeks and consequently lengthen the period of time until healing.
Anoint
Cool and anti-inflammatory ointments can help relieve symptoms of periosteum inflammation on the shin.
The active ingredient diclofenac has an analgesic and anti-inflammatory effect. It is ideal for external application to the shin. Diclofenac is contained in Voltaren® and Diclo-Pain Gel®, for example.
The well-known active ingredient ibuprofen also has a pain reliever and anti-inflammatory effect. The doc® ibuprofen pain gel also has a beneficial effect on periosteum inflammation on the shin. When buying other ointments, one should make sure that the products are anti-inflammatory and effective against pain.
Home remedies
In addition to protecting the affected leg, there are home remedies that can alleviate the symptoms.
Quark wraps that are wrapped around the affected shin are ideal. The compresses cool, relieve pain, have anti-inflammatory and decongestant effects. It is a tried and tested home remedy that is cheap and well tolerated. In addition, all other coolants, such as cooling pads or moist compresses with cold water, are suitable to cool the tissue and reduce swelling. In the further course, cold-warm alternating images can be effective.
Use of kinesio tapes
Another, mostly complementary measure in the treatment of periosteum inflammation of the shin is the application of a kinesio tape. An acute and severe periosteum inflammation cannot be adequately treated with a kinesio tape; however, it can lead to an improvement in the subjective complaints.
The kinesio tape - an elastic adhesive tape - is attached along the shin and ensures that the muscles that run along or on the edge of the shin are relieved of the tensile forces that are applied.
The duration of the kinesio tape application varies according to the severity of the periostitis. If, contrary to expectations, deterioration occurs during use, the treatment must be stopped immediately.
Read more on this topic at:
- Applying a tape bandage
Operative therapy
Occasionally, conservative treatment of the periosteum inflammation alone is not enough to improve the symptoms. On the one hand, this can be the case if the periosteum inflammation has passed into a chronic stage due to overload, so that a cooling or gentle treatment no longer has a positive effect.
Furthermore, conservative therapy is usually futile if a bacterial periosteum inflammation cannot be treated effectively enough with antibiotics and is very difficult. In this case, there is reasonable concern that the inflammation could spread to other areas and cause systemic harm to the patient. In some very rare cases, inflammation in the periosteum can spread to such an extent that amputation of the leg would have to be considered without rapid surgical treatment of the affected area.
Surgical rehabilitation of periosteum inflammation is one of the last ways to remove the inflammatory process and any causative pathogens from the body.
The surgical procedure takes place in a special clinic for septic diseases and is usually carried out under general anesthesia. First, there is sufficient disinfection and covering, followed by layer-by-layer removal of the soft tissues in the direction of the affected tibia. Here, dead and severely inflamed parts are removed. The severely inflamed periosteum must be partially removed and the area of the tibia must be rinsed with a special disinfecting solution. Finally, the severed soft tissues are adapted again in layers and finally the skin is closed.
The patient then receives an oral antibiotic which is supposed to ensure that germs that may have penetrated the normally highly sterile region of the bone are killed. In rare cases, an antibiotic chain is also applied to the periosteum. This is a small chain that is linked to an antibiotic such as B. Gentamicin is coated. This is delivered directly to the surrounding area over about two weeks and can have a local effect there. Thus, the severely inflamed area will be treated with antibiotics in high doses, which the administration of a tablet would not be possible without side effects. The antibiotic chain is then removed again.
The removal of the chronically inflamed periosteum is often successful. Unfortunately, there are also a few rare cases of chronic periosteum inflammation that do not respond successfully to any therapy. Even operational renovations can be difficult, so that some of them have to be repeated several times.
Diagnosis
In the context of diagnostics, it is particularly important to question the person affected (anamnesis), which should reveal important clues. First of all, the doctor should inquire how long the symptoms have existed and whether excessive sport is practiced or whether the pain occurs when moving or at rest. Furthermore, possible general symptoms such as fever, which could indicate inflammation, should be inquired about.
The next step is to inspect and examine the affected leg. This includes, among other things, feeling the shinbone, which will be painful in the case of periosteum inflammation. The leg is also examined for redness, swelling and, if necessary, water retention (edema). The patient is also asked to perform some movements.
In the case of chronic periosteum inflammation, which is usually more gradual, an X-ray of the tibia can provide further clues. Here the tibia appears inflamed and thickened and small bone attachments, which are signs of a compensatory reaction of the bone, may be visible.
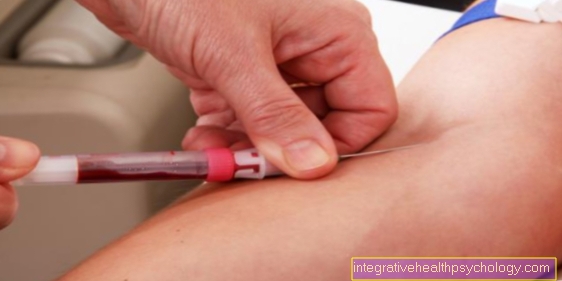
A blood test may also show evidence of periosteum inflammation. In the case of periostitis, the typical signs of inflammation in the blood count (CRP and Leukocytes) be increased.
Preventive measures
There are numerous ways to prevent periosteum inflammation. Overloading should be avoided, especially during sporting activities, and a consistent warm-up program should be observed. Furthermore, orthopedic misalignments, such as knock knees or bow legs, should be compensated for with shoe insoles, as these can otherwise lead to incorrect loads.
To avoid periosteum inflammation caused by an invasion of bacteria, care should be taken to ensure that the skin in the area above the shin is intact and, in the case of wounds, that the wound is adequately disinfected and sterile covered in order to minimize the germ load.
Running analysis
There are risk factors for developing periosteum inflammation on the shin. This includes incorrect footwear, incorrect movement sequences and hard surfaces, such as road surfaces, when jogging. A treadmill analysis with individual adjustment of the jogging shoes can help prevent future periosteum infections in athletes.
- Treadmill analysis
insoles
In addition to adjusting the running shoes, insoles can be a useful measure to prevent shin splints.
Orthopedic insoles should match the athletic shoe that is being worn. In an orthopedic shoe store, insoles are individually adjusted and any foot misalignments can be corrected. Those affected should take their running shoes with them and show them to trained staff.
stretching
In the case of an acute periosteum inflammation, the tissue should be spared.
In the further course and as a future preventive measure, the leg muscles should be thoroughly stretched before and after training. This includes stretching the entire rear leg muscles, especially the calves and front leg muscles.
Fascia therapy
Adhesive fasciae promote the development of periosteum inflammation on the shin. Targeted fascia therapy can help prevent shin splint syndrome.
The aim is to loosen the adhesions in the connective tissue and tension. Fascia treatment with fascia rollers such as the Blackroll® is popular. There are several exercises that can be used to relieve the legs with this form of self-massage.
Also read:
- Fascia training
Duration
The time it takes for periosteum inflammation to heal depends, among other things, on the underlying cause. For example, periosteum inflammation caused by overload should not last longer than two weeks. This is usually achieved through consistent rest, cooling and taking anti-inflammatory and pain-relieving medications such as ibuprofen or diclofenac.
If the periosteum is caused by a bacterial infection, it can take many times longer for the symptoms to subside. As a rule, the inflammation heals quickly under the antibiotic therapy carried out. In addition to drug therapy, the entry portal for the bacteria on the leg may also have to be surgically repaired.
If there are recurring re-infections or systemic involvement of the entire body, it can take months for the periostitis to completely heal. In the case of a complicated course, the treatment would no longer be carried out on an outpatient basis, but rather on an inpatient basis. For this purpose, many orthopedic trauma surgery hospitals have specialized departments which, among other things, deal with the treatment of periosteum infections.
Read more on this topic:
- This is how long periosteum inflammation lasts
Chronic course
Chronic periosteum inflammation almost always occurs when there are permanent mechanical causes in the sense of excessive stress or improper stress. Chronic courses can last from months to years. Here it is particularly important to first make the exact diagnosis and determine the underlying cause. Then a gait analysis should be carried out and the corresponding incorrect loads diagnosed. Sports overload should be avoided.
You may also be interested in this topic: Lump on the shin







.jpg)