Myositis
overview
Myositis is one inflammatory disease of the muscle tissue. It can be triggered by a wide variety of causes, but is usually the result of one Autoimmune disease. Myositides occur mainly in association with other diseases, but are overall a relative rare clinical picture There are only 10 cases of illness among a million inhabitants recorded per year. The most common forms of illness are Polymyositis, the Dermatomyositis and the Inclusion body myositis. Often there is one inflammation of Muscle tissue with a Connective tissue inflammation socialized.
Read more about the sub-forms under our special topics:
- Polymyositis
- Dermatomyositis
root cause
The cause of an existing myositis can often not be precisely identified. In this case one speaks of one idiopathic Myositis. In the Polymyositis and the Dermatomyositis, the two most common clinical pictures in this area, are autoimmune-mediated disease processes, so-called Autoimmune diseases. The immune system attacks the body's own cells with its defense cells and thus leads to their destruction. As a result, the affected tissue becomes inflamed.
The muscles can be involved in general systemic infections or inflammations, as well as in inflammatory processes in the connective tissue. If the myositis is triggered from the outside, this happens by bacteria, viruses or Parasites. A disease, for example, is particularly predestined for the development of myositis leprosy, Gonorrhea (syphilis) and tetanus or parasitic infestation with Schistosomes and Trichinellawhich are both worms. Overall, however, the infections mentioned occur less often in European latitudes. Bornholm disease however, it can also occur here, as the triggering Cocksacki B viruses can be found worldwide. Myositis can also hereditary Be origin like that Münchmeyer syndrome. But also this special form of an inflammatory muscle disease is to be regarded as extremely rare due to its slight spread.
Symptoms
The Symptoms a myositis can develop depending on the clinical picture symmetrical or just one-sided represent. However, it goes along with all forms increasing loss of strength and muscle weakness as well Muscle aches hand in hand. The intensity of the symptoms depends on the degree of inflammation. Without anti-inflammatory treatment, it can too muscle degenerative processes come out in the visible muscular dystrophy represent. Since all muscles in the entire body can be affected, localization in the throat and pharynx muscles can cause it to become too Difficulty swallowing and hoarseness come.
If the underlying disease is degenerative, as in Münchmeyer syndrome, the cells can be remodeled. In this rare case it will be Calcium salts stored in the affected cells and lead to Ossification of the muscles (Myositis ossificans). Such Cell calcification can develop to a lesser extent in other forms of myositis. Basically, inflammatory processes put stress on the cells of the affected tissue. Due to the constant breakdown and build-up of cells, it can Metaplasias, that is, changes in the cell structure occur. These can ultimately lead to a degeneration of the tissue - a malignant tumor.
Diagnosis
The diagnosis of myositis is usually complicated because it is difficult to differentiate between different clinical pictures. The clinical symptoms should be the guide, as these can provide an indication of the type and localization of the inflammation. However, the majority of myositis are creeping illnesswhich is only noticed late. This increases the risk of developing permanent consequential damage. In principle, the examining doctor three diagnostic toolswhich can be used: a Laboratory examination, an electromyography (EMG; Tension measurement in the muscles) and a Muscle biopsy (invasive procedure in which muscle tissue is removed.
Laboratory examination: When examining the laboratory parameters in the patient's blood, the main focus is on enzymes that accumulate in muscle cells and are released when the cells are damaged. The most important enzyme is the Creatine kinase (CK). In addition, other parameters such as the activity of lactate dehydrogenase, of the Aldolase and aspartate aminotransferase in the blood. General signs of inflammation how increased C-reactive protein, increased white blood cell count or one extended BSG are also recorded, but only prove the presence of inflammation. The amount of Myoglobin, a specific protein of the skeletal muscles, can also be determined and included in the diagnosis. However, the value says nothing about the location of the damage, only that muscle cells have perished. If there is a suspicion of an infection with pathogens, it is possible to detect antibodies formed by the body against the pathogen and thus indicate an existing infection or use a PCR (Polymerase chain reaction) to duplicate the DNA of the pathogen and to display it in such a way that a computer-controlled precise identification is possible. Myositis-specific antibodies, which are formed in the course of the disease in some patients, in most cases have no conclusive significance, as they are also used in other diseases, such as inflammation of the alveoli (Alveolitis) or inflammation of the joints (arthritis).
Electromyography (EMG): With an EMG, two tiny needles are inserted into the muscle to be examined. The needles conduct electricity and measure Changes in tension in muscle tissue. The changes are in Recorded and evaluated rest and tension. Most patients with myositis show conspicuous patterns, which are not automatically proof of the disease. Nevertheless, the EMG is an uncomplicated examination through which the indication for further diagnostics can arise. In addition, an electroneurography can be performed in which the Nerve conduction velocity and the Muscle reaction time is measured. Here a nerve is excited with the help of applied electrodes and attention is paid to the muscle twitching that can be triggered. Concomitant nerve damage or other diseases can be proven or excluded, which plays an important role in differential diagnosis (other diseases with matching symptoms).
Muscle biopsy: Since the muscle biopsy is a invasive examination the location of the intervention should be planned. This is usually done through an MRI (magnetic resonance imaging). The biopsy should not be done at a site that has previously had an EMG. The punctures by the needles lead to local cell death, which in retrospect can no longer be differentiated from myositis. Once the right place for the biopsy has been found, the Biopsy (biopsied tissue) light microscopic examination general features of myositis have been demonstrated, but tissue changes specific to various forms can also be observed. You can see both in a characteristic way Muscle fiber losses (dead / necrotic muscle fibers), as well as regenerated sections of muscle fibers and typical signs of inflammation - Tissue infiltration (Immigration) through inflammatory cells. If the disease activity is low, the diagnosis can be made more difficult by missing or difficult to find cell signs.
Myositis antibodies
Since the Myositis one of the inflammatory skeletal muscle diseases that can be caused by an autoimmune reaction, i.e. a false reaction of the body's own defense system against the body's own structures, it is therefore possible to detect certain antibodies in the blood of the affected patient.
These antibodies are part of the immune system and are called B lymphocytes in the context of an autoimmune disease - here in the case of myositis - structures of the skeletal muscle culture, so-called antigens. In myositis, a distinction is made between myositis-specific and myositis-associated antibodies.
The former are found in about 15-50% of patients in the blood serum and can be measured by taking a blood sample.
The myositis-specific antibodies primarily include antibodies against tRNA synthetases, such as Jo-1 antibodies, PL-7 antibodies, EJ antibodies, or KS antibodies. The myositis-associated antibodies include i.a. anti-Mi-2, anti-SRP and anti-Pm-Scl.
The most common clinical pictures
Polymyositis
The polymyositis is that rarest form the common inflammatory muscle diseases. It occurs more frequently in two phases of the patient's life: in childhood and adolescence from 5 to 14 years and in advanced adulthood from 45 to 65 years. On average, twice as many women as men are affected by polymyositis. Clinically the disease shows itself through mostly symmetrical muscle weakness in the area of Shoulder-neck belt and the hip - the muscles close to the torso. The weaknesses develop in comparison to inclusion body myositis quite fast, over weeks to months. The lack of muscle strength can cause it to painful bad posture come through Scarring from inflamed muscle sections to Misalignment of joints. The tissue sample taken through a biopsy points between the muscle fibers Immigrated inflammatory cells on. The disease process of polymyositis is not yet fully understood. However, it is assumed to be a Autoimmune disease acts. In contrast to dermatomyositis, however, this is mediated by a direct cell response of the body and not via corresponding proteins.
Read more on this topic at: Polymyositis
Dermatomyositis
Disregarding age, dermatomyositis occurs more frequently than polymyositis. As with polymyositis, an age-specific accumulation can be observed. Women are more likely to be affected than men. Among the symptoms that affect the skeletal muscles, changes in the skin appear in dermatomyositis. Lilac-colored rashes (erythema) form on areas of the body exposed to light, which is why the name purple disease came about. The skin becomes flaky, especially in places over joints such as fingers, elbows, and knees. As part of the rash, there may be swelling of the upper eyelids, giving the patient a whiny expression. This can be aggravated by scarring of the scaly skin.
The changes described can appear more or less strongly. If a muscle biopsy is performed, the perivascular inflammatory cells surrounding the vessels can be identified in the specimen. Corresponding cells also collect between the individual muscle fiber bundles (interfascicular). Peripheral muscle fibers become narrower in relation to the rest of the bundle. This is known as perifascicular atrophy. The pathomechanism (disease process) is based on an autoimmune reaction that is directed against the capillaries (smallest vessels) in the muscles. These are attacked and damaged by the body's own inflammatory proteins (e.g. immunoglobulins). As a result, the muscle fibers can no longer be supplied and die.
Local necrosis (cell death) and vascular thrombosis (occlusion of a vessel by a blood clot / thrombus) occur - the muscle fiber bundles decrease in strength and ultimately wither. A malignant tumor is the cause of development in over a quarter of dermatomyositis diseases. Here, too, the body forms substances that are directed against both the tumor and healthy body tissue.
Read more on this topic at: Dermatomyositis
Inclusion body myositis
Inclusion body myositis is a chronic, progressive, inflammatory, degenerative disease. The causal process in the body has not yet been precisely clarified, but an interplay of inflammatory and degenerative factors is suspected. It affects men in 75 percent of cases and occurs mainly after the age of 50. The course is rather gradual - it can sometimes take months or years for the first clinical symptoms to appear. Patients first notice problems climbing stairs or getting up from a sitting position. Difficulties in holding a firm grip or even in the first place are also characteristic. Symptoms are caused by the progressive weakness of the forearm and thigh muscles. 60% of sufferers report difficulty swallowing, as muscles are required for this, too, which can be affected by the inflammation. The preparation made from a biopsy resembles that of a polymyositis. Immigrated inflammatory cells and submerged fiber strands can be seen. In addition, there are inclusions in the tissue, so-called ¨rimmed vacuoles¨ (in English: framed vacuoles; vacuole = cell vesicle). The inclusion bodies contain various protein structures, α-amyloid and tau proteins. These compounds are also used in other degenerative diseases, such as in Alzheimer's disease, to find.
Special clinical pictures
Münchmeyer syndrome (Fibrodysplasia ossificans progressiva): By a inherited genetic defect which influences the development of the skeletal muscles, the so-called Münchmeyer syndrome occurs. It happens over the years Storage of calcium salts in muscle cells and as a result to ossification of the muscles. Starting in the neck area, the disease progresses up down forward, over the shoulder region into the arms and trunk. Since there is currently no proven possibility for therapy, let alone for healing, it comes in Terminal stage the disease for Ossification of the respiratory muscles and thus to difficult breathing, up to Suffocation. Since most patients remain childless and do not pass on the genes, the spread of Münchmeyer syndrome is very limited.
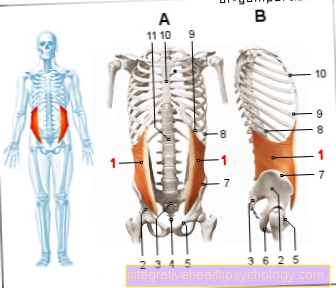
Bornholm disease (Epidemic Pleurodynia): Epidemic Pleurodynia is a inflammatory disease of the pleura (Pleura), the chest and abdominal muscles. It is caused by an infection with the Cocksackie B virus, a member of the enterovirus family. Are symptomatic Painful breathing, light fever and a red throat. The pain is caused by the involvement of the intercostal muscles, the muscles between the ribs, which are part of the respiratory muscles.Bornholm disease can transmitted from person to person and will default to the symptoms with Analgesics treated.
Myositis of the eye
The myositis on the eye, too ocular myositis called, is an idiopathic (that is, occurring without a known causeInflammation of the muscles in the eyes.
It is one of the third most common diseases of the eye socket and comes right after eye involvement in Hyperthyroidism and in lymphoproliferative diseases.
The exact cause of myositis in the eye has not yet been fully clarified; it is suspected that an autoimmune reaction, that is, a false reaction of the body's own defense system, which falsely recognizes and combats certain cellular structures as foreign.
Women in young adulthood are most commonly affected (Mean age of onset: 34 years), whereby the symptoms are more often unilateral (only one eye affected) than bilateral:
- protruding eyeball
- Conjunctival swelling and inflammation
- eye movement-dependent pain
- Eye movement restrictions and the resulting visual disturbances (e.g. double vision).
The eye muscle that is most commonly affected is the middle straight muscle (Medial rectus muscle), which usually moves the eyeball towards the nose. Ocular myositis is usually diagnosed with a CT scan, and it is treated by taking glucocorticoids (cortisone), so that the inflammation usually subsides within several days without consequences.
Myositis ossificans
The term "Myositis ossificans"Includes two medical disease patterns.
On the one hand, it is heterotropic ossification This is a disease that occurs in various parts of the body either spontaneously or after trauma and surgery Ossifications comes.
On the other hand, the term "Myositis ossificans“Also a rare hereditary disease - the Myositis ossificans progressiva. This is a congenital genetic defect that causes the skeletal muscles of the body to be converted into bone tissue in stages. Only around 600 people worldwide are affected by this hereditary disease. The cause of the bony remodeling is the inability to repair defective skeletal muscles after trivial injuries or traumas with healthy muscle tissue or scar tissue - bone tissue is used instead.
Over time, the muscular system becomes increasingly inoperable, and the disease becomes life-threatening when organs are impaired by ossification of the muscles (E.g. respiratory dysfunction due to increasing ossification of the intercostal muscles and thus the chest).
therapy
The treatment of dermatomyositis and polymyositis corresponds to the mostly applied therapy for autoimmune diseases. Here is Cortisone administered, which inhibits the immune system in part and in part Flatten the inflammation leads so that the tissue can recover. Relatively high doses are used, which are gradually reduced over a longer period of time. The effect starts depending on the patient after days to weeks, in delayed cases after 1-2 months. Long-term cortisone administration however, is with a wide variety of Side effects connected, such as Muscle breakdown, osteoporosis or mental changes. If the therapy does not have the desired effect or if the dosage has to be reduced due to side effects, additional Cytostatics how methotrexate are used, which also have a fixed place in tumor treatment and additionally compress the immune system. The gift of high-dose immunoglobulins can be helpful in polymyositis and dermatomyositis, but is particularly controversial in the treatment of inclusion body myositis. In addition to drug therapy, you can physiotherapy and Occupational therapy are used to maintain freedom of movement and reduce muscle shortening (Contractions) to prevent. In the case of pronounced muscle weakness, the use of walking aids or wheelchairs, in the case of paralysis, muscle hardening or injuries, further treatment may be necessary.
forecast
Regular therapy can help at half the patient one Polymyositis a complete healing can be effected. Otherwise a standstill with more or less permanent muscle weakness can be achieved. However, in 20% of the cases there is the possibility that no success can be recorded despite complex therapy.
The Dermatomyositis can also be cured or at least limited by appropriate therapy. The treatment of the tumor that is often the cause of the disease can cause permanent improvement in symptoms or the healing of the secondary disease.
Since drug therapy is a Inclusion body myositis is not promising, a constant range of motion must be aimed for through physiotherapy and independent exercises. Light strength exercises and muscle endurance training can also counteract the symptoms. In the case of disturbing impairment of the throat muscles, a visit to a speech therapist can provide relief to improve the swallowing difficulties. Helpful movements or postures are practiced that make the swallowing process easier.