Neck Dissection
definition
Neck dissection is a radical surgical procedure to remove the cervical lymph nodes and surrounding structures in the context of tumor diseases. The aim of the operation is to remove infected or endangered lymph nodes and thereby limit the cancer. A distinction is made in medicine between an elective and a therapeutic neck dissection.
In elective dissection, lymph nodes that have not yet been affected are resected (operated on) as a precautionary measure to prevent spreading, to remove any micrometastases and to guarantee an optimal diagnosis. In the more radical, therapeutic neck dissection, settlements (metastases) in lymph nodes are already known and surrounding structures such as nerves, vessels and muscles are also removed.

Indications
A neck dissection is carried out in the context of tumor diseases. The reason is that tumor cells can separate themselves from their actual growth site and thus get into the lymphatic system. Lymph nodes form a kind of intermediate station in the lymph system and filter conspicuous inflammatory cells or tumor cells from the lymph so that they can accumulate within the nodes. The tumor cells form clusters of cells and grow, resulting in a lymph node metastasis.
In the course of the process, one lymph node after the other is affected and the cells spread along the lymphatic pathway. It is therefore important in the context of a tumor to prevent this process and stop the spread. Tumors that cause cells to settle in cervical lymph nodes are primarily cancers of the head and neck, such as larynx cancer, throat cancer, salivary gland cancer, oral cavity cancer, thyroid cancer or cancer of the nose and paranasal sinuses. Neck dissection may also be necessary in the context of lung cancer.
consequences
Neck dissection can vary widely depending on the type and stage of cancer. Depending on how radical the neck dissection is, the more likely complications and side effects of the procedure are. How big the operation will ultimately be depends primarily on whether it is an elective (preventive) or therapeutic dissection. Depending on how much surrounding tissue and muscles have to be removed, there can be a significant loss of tissue, which may have cosmetic consequences.
In addition, excessive scarring is possible, which can cause problems over time. Resection of muscles and nerves can cause restricted mobility, paralysis, sensory disturbances and tingling. In a therapeutic neck dissection, a large jugular vein (internal jugular vein) is often removed, which can lead to drainage disorders and swelling, especially in the case of bilateral resection. The removal of lymph nodes and lymph vessels can also be associated with swelling, in the form of lymphedema, or with a weakened immune system. In addition to the specific side effects, the general surgical risks, which can also have long-term consequences, should also be taken into account.
procedure
Neck dissection is performed under general anesthesia. The incision can vary, depending on the goal of the operation, and is selected by the surgeon. In neck dissection, important anatomical structures are first sought out in order to create an overview and not to injure any important organs or vessels. Then begin with the lymph nodes that are closest to the actual tumor.
The resected lymph nodes are usually sent to the pathology department during the operation to examine them under a microscope. This process is also called quick cut. The pathologists examine whether there are tumor cells in the lymph node and, if so, how far they are on the incision edge. The quick cut has diagnostic reasons on the one hand and is decisive for the further course of the operation on the other. If all the endangered or suspicious lymph nodes and surrounding structures have been successfully removed, the operation can be ended. Unfortunately, it also happens that the affected lymph nodes or vessels could not be removed for surgical reasons and the operation has to be ended prematurely.
Complications
Complications with a neck dissection are, on the one hand, the general surgical risks and the specific complications of a neck dissection. The general risks include general anesthesia and the risk of injuries to important organs, nerves and vessels, as well as bleeding, inflammation, excessive scarring, impaired wound healing and secondary bleeding.
The specific complications of neck dissection depend on the radical nature of the procedure. A therapeutic neck dissection is associated with a significantly higher rate of complications than an elective or selective neck dissection. Whether it is a unilateral or bilateral resection also plays a major role in the surgical risk and side effects. In particular, the removal of significant structures such as larger nerves, muscles and blood vessels increases the risk of complications. This particularly affects the therapeutic dissection, since in this case the large jugular vein (internal jugular vein), a large cranial nerve (accessory nerve) and the nodding muscle (sternocleidomastoid muscle) must be removed.
Do scars remain?
Whether or not scars remain depends on the surgeon's incision. This can vary greatly depending on the goal of the procedure. The surgeon will usually orientate himself on anatomical structures and skin folds so that a good cosmetic result is possible later. In addition, a special suture technique (intracutaneous suture) is usually used for operations on the neck in order to make the scar as inconspicuous as possible. This will appear very slit-shaped. In order to achieve the best possible aesthetic result, the scar should be cared for with creams after it has healed. Moving the neck early and frequently can enlarge the scar.
Lymphatic drainage
The lymphatic system extends all over the body and absorbs fluid from the tissue in order to drain it back into the blood via lymph vessels. Lymph nodes represent a kind of intermediate station, which filter the lymph and stop harmful cells. They are therefore part of the immune system. When resecting lymphatic vessels and nodes (Lymphadenectomy) it can lead to lymph drainage disorders and an accumulation of these in the tissue. This event is also called lymphedema. A therapeutic massage or manual lymphatic drainage can be used as a supportive measure, promoting removal and counteracting swelling.
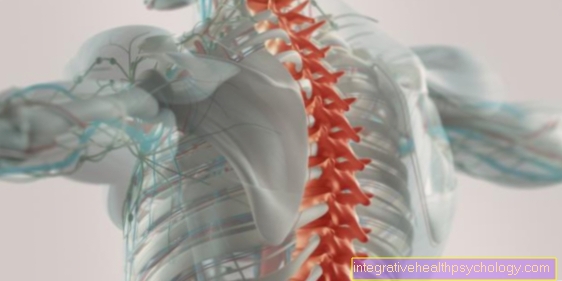
Lymph node level
The lymph nodes of the neck are divided into six different levels and six other sub-levels according to their location and affiliation. The reason for this is that certain tumors specifically spread into certain groups of lymph nodes. In some cases this offers the possibility of selective neck dissection. Only the most vulnerable levels of lymph nodes are removed to allow for a minor procedure and fewer complications. The first level is the submental / submandibular level and is divided into the submental and submandibular sublevel. Submental refers to the area that is centrally located below the chin. Submandibular lies directly to the side of the submental sublevel and describes the area below the jawbone.
The second, third and fourth levels relate to the large jugular vein, the internal jugular vein, which runs diagonally from the top to the inside below the neck parallel to the carotid artery. The second level (craniojugular lymph node group) describes the uppermost area of the vein on the neck and is divided into the medial (central) and the lateral (lateral) sublevel. The third level covers the medium-high area of the vein on the neck and is also known as the mediojugular lymph node group. The lowest part of the jugular vein Interna on the neck is represented by the fourth level and is also called the caudojugular level. The fifth level is the posterior (rear) neck triangle and represents the area to the side or behind the great vena. It is divided into the cranial (upper) and caudal (lower) neck triangle and thus represents the last two sub-levels.
The lymph nodes of the posterior cervical triangle are also known as the accessorius group, as they represent one of the large cranial nerves (accessory nerve) surround. In contrast to the fifth level, the sixth and last level covers the front part of the neck, which is located in the middle in relation to the large vein. The sixth level is also called the anterior compartment and contains the lymph nodes belonging to the throat (para- and retropharyngeal lymph node group).











.jpg)