Retina of the eye
Synonyms
Medical: retina
English: retina
introduction
The retina is a part of the eye and consists of several layers that contain cells that receive, convert and pass on light stimuli. It is responsible for color and brightness vision and ultimately forms the optic nerve, which forwards the impulses to the brain. The retina contains different cells for different colors and light intensities, which convert the light stimuli into electrochemical stimuli.

anatomy
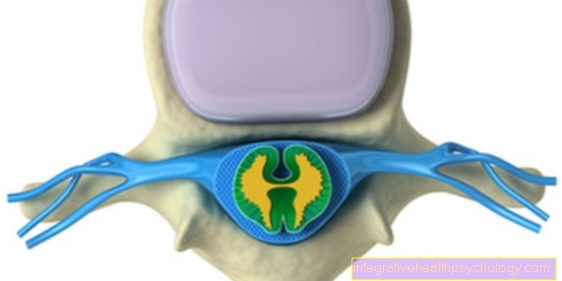
The retina is made up of three layers. The outermost layer is adjacent to the choroid. This outer granular layer contains the sensory cells that receive the light stimuli (Photoreceptors). In the case of photoreceptors, a distinction is made between the rods, which are responsible for night and twilight vision, and the cones, which ensure day and color vision.
The cones are mainly located in the center of the retina, the rods more in the outer areas (Periphery). The inner granular layer adjoins the outer granular layer.
This consists of bipolar cells, horizontal cells and amacrine cells. These cells receive the light pulses detected and processed by the photoreceptors and pass them on to the cells in the innermost layer. The innermost layer is adjacent to the vitreous and consists of the ganglion cells.
The ganglion cells have long cell extensions and move to a common point on the fundus (see also fundus mirroring), the papilla, where they then together form the optic nerve.
The papilla itself does not contain any photoreceptors. So no light stimuli can be perceived there. This is why the papilla is also known as the blind spot. On the side of the blind spot towards the temple is the yellow spot, which is also known as Macula lutea referred to as. There is a depression in the middle. There are sensory cells that only consist of cones. This is why this deepening is also known as the point of sharpest vision. From an evolutionary point of view, the retina is an upstream part of the diencephalon (Diencephalon) and has approx. 120 - 130 million photoreceptors.

- Cornea - Cornea
- Dermis - Sclera
- Iris - iris
- Radiant Bodies - Corpus ciliary
- Choroid - Choroid
- Retina - retina
- Anterior chamber of the eye -
Camera anterior - Chamber angle -
Angulus irodocomealis - Posterior chamber of the eye -
Camera posterior - Eye lens - Lens
- Vitreous - Corpus vitreum
- Yellow spot - Macula lutea
- Blind spot -
Discus nervi optici - Optic nerve (2nd cranial nerve) -
Optic nerve - line of sight - Axis opticus
- Axis of the eyeball - Axis bulbi
- Lateral rectus eye muscle -
Lateral rectus muscle - Inner rectus eye muscle -
Medial rectus muscle
You can find an overview of all Dr-Gumpert images at: medical illustrations
Blood supply to the retina
The inner two layers of the retina are connected by the central retinal artery (A. centralis retinae ), which with the optic nerve through a common opening in the skull bone (Optic foramen) pulls into the eye socket from behind. This comes from the flow area of the artery of the eye (A. ophthalmica), which in turn arises from the flow area of the inner main artery on the neck and head (Internal carotid artery). The outer layer of the retina is supplied by blood vessels in the choroid. The venous blood is disposed of via the eye veins (Vv. Ophthalmicae).
Tasks of the retina
The retina of the eye, also called the retina, takes on the task of transmitting stimuli to the brain when seeing. It is therefore responsible for ensuring that what we see is perceived as an image.
The light first has to pass through the cornea, the lens and the vitreous humor of the eye apparatus before it hits the retina inside the eye.
The retina is made up of millions of sensory cells. The reflected light information of the seen object is picked up by the cells of the retina, sorted, bundled and finally sent as an impulse to the brain via the optic nerve. These tasks are performed by the various cell types that are interconnected in the retina.
Furthermore, the retina takes on tasks in the vitamin A metabolism and represents a kind of boundary between it and the blood vessels lying directly next to it in the choroid. These supply the retina. The barrier ensures that no harmful substances can get into the retina from the blood. The point of sharpest vision, the so-called point of view, is also located in the retina Macula or Fovea centralis. There are only tenons here.
Read more about this under How does seeing work?
Retinal physiology
If a light stimulus hits the eye, it must first penetrate through several different structures of the eye to the photoreceptors. First, the light pulse hits the cornea in the anterior chamber, passes through the pupil, posterior chamber, lens and vitreous humor.
In order to get to the photoreceptors, the light pulse has to pass through the two inner layers of the retina. Once the light stimulus has reached the sensory cells, this light stimulus is converted into electrochemical stimuli and passed on to the two inner layers of the retina. The cells of the inner layer form the optic nerve, which conducts the stimuli into the brain, where they are then processed and perceived.
Colors and twilight vision
There are three types of cones for color and brightness vision, consisting of red, green and blue cones. The rods responsible for twilight vision are virtually switched off when it is bright and cannot perceive any colors. Only rods are active in the dark, which is why it is difficult to see colors in twilight and in the dark.
More information can be found here: Rods and cones in the eye
The photoreceptors and bipolar cells have a certain resting activity (potential). In the event of a stimulus, they pass this information on via an increase or decrease in potential. The ganglion cells in turn pass on their information via electrical signals (action potentials), so they are frequency-coded. Brightness and color have different frequencies, the frequency code of which is decoded in the brain and translated into an image.
Diseases of the retina
Retinal detachment / retina detaches
In general, diseases of the retina take place painlessbecause there are no pain fibers there.
At a Retinal detachment it comes to one Separation of the retina from the vascularized choroid. It imagines Space, in which Fluid accumulates. As a result, the retina can no longer be supplied by the choroid and visual disturbances occur.
Causes of retinal detachment can be Inflammation, Degenerations, Formation of holes or cracks be. The latter are caused by weak spots or, for example, by bruises in the eyeball. Fluid passes through the hole and the retina becomes detached. Since in most cases no pain is felt, a retinal detachment can usually be managed blurred vision determine. If the cracks caused by degeneration are in the area of a blood vessel, it can lead to small visible hemorrhages in the eye. If the retina has become detached in the area of the central fovea, sharp vision is no longer possible. Furthermore, there is reduced light perception in the area of the detached point. this will often perceived as a kind of veil in front of the eye. In the most common cases, retinal detachment is caused by age-related cracks or holes. The cause of these cracks is the increasing shrinkage of the so-called vitreous body inside the eye with age. Since this is connected to the retina in some places, its shrinkage causes tension on the retina. This results in cracks.
People who at Diabetes mellitus are sick who nearsighted are or due to a cataracts have had an operation higher risk experience retinal detachment. If the retina is torn, this can be remedied with laser therapy. If the retina is detached, surgery must be performed. Unfortunately, holes in the retina or retinal detachment cannot be treated with medication. The retinal detachment can be divided into a rhegmatogenic detachment based on crack formation, an exudative detachment in which fluid from the vessels of the choroid penetrates into the retina and a tractive retinal detachment. The latter creates scar tissue. At the point of scarring, the tissue contracts and a tension is created. Because of this, the retina can become detached.
- Symptoms of retinal detachment
- Retinal detachment surgery
Circulatory disorder of the retina
In order to always function properly and to enable seeing as a process, the retina must constant from the blood vessels from the adjacent choroid provided become. With a circulatory disorder it comes to Loss of vision leading to blindness because the retina can no longer be adequately supplied. Both arteries and veins can be affected.
Primary diseases that can lead to a blockage of a vessel and thus to a circulatory disorder are above all Diabetes mellitus, high blood pressure and arteriosclerosis. It is therefore important the parameters of these diseases always check allow.
Arterial Disturbances turn into one spontaneous, painless and direct loss of vision noticeable in the affected area. Should symptoms occur an ophthalmologist immediately within 24 hours be sought out so that there is a chance of recovery.
Venous-related Failures express themselves not so strong and abrupt compared to the arterial occlusions. The symptoms here are mostly considered one Kind of dark shadow or curtain perceived. A common consequence of venous circulatory disorders is swelling in the area of sharpest vision (Macular edema) due to which the visual acuity is greatly reduced.
- Circulatory disorders of the eye
- Diabetic retinopathy
- Thrombosis in the eye
Retina torn / retinal tear
Often the retina tears in the peripheral areas for no apparent reason one and there is a hole. Normally, the retina lies against the inside of the eye wall. It is held in position by a suction created by liquid. If a tear has now appeared in the retina, the suction is lost. The water from inside the eye gets into the space in between. This increasingly fills with liquid and the Retina peels off. The retina can peel off completely within a few days.
The original cracks in the retina mostly make up as fast and bright flashes or as many small black dotsthat seem to swim around in front of the eye of the person concerned are noticeable. If the retina has become detached, severe visual field defects occur.
If you notice symptoms, you should see an ophthalmologist as soon as possible. If the retina has not yet detached at this point, laser therapy is sufficient in most cases. In this case, an inflammatory reaction is triggered at the affected area by a laser beam, which causes the tissue at the location of the hole to scar and thus closes it. If the retina is already lifted, one will help Laser therapy no more and it must be operated on.
Retinal inflammation
A pure inflammation of the retina is referred to as Retinitis. Since the retina and choroid are closely connected, the choroid directly next to it is usually also affected. Therefore, the inflammation of the fundus is also known as Chorioretinitis.
The retinal inflammation runs painless. At the start it also runs symptomless. Only in later stage inflammation often occurs in those affected Fogging in front of the eyes or Opacities in the field of vision. The extent of the symptoms depends on the location of the inflammation on the retina. The closer this is to the point of sharpest vision, the more severe the visual impairment.
root cause for retinal inflammation mostly bacteria, Viruses or Mushroomsthat penetrate the retina. Furthermore, diseases like rubella, Herpes, syphilis or Autoimmune diseases be the cause of retinal inflammation. To combat inflammation are mostly used Antibiotics using eye drops administered. Due to its anti-inflammatory effect, cortisone is also often used. In severe cases, the antibiotic must be injected using a syringe.
- Retinitis pigmentosa
- Eye drops containing antibiotics
Retinal examination
After you've described the symptoms of inflammation, cracking, or detachment of the retina to your eye doctor, they will first of all one Eye test carry out. In this way, the ophthalmologist can assess the extent of the damage in relation to the eyesight.
In the following, the posterior wall of the eye, including the retina and choroid, must be Ophthalmoscope to be viewed as. With this procedure, the fundus of the eye can be viewed enlarged so that it can be determined what the damage is.
Fast treatment is always very important to avoid consequential damage. If, for example, the retina has been inflamed for a long time, it is possible that scars form on the retina, which severely impair vision.
As general examinations, the fundus of the eye can be mirrored in the case of the symptoms described, circulatory disorders can be made photographically visible with the aid of fluorescence angiography, and degrees of swelling can be determined using optical coherence tomography (OCT).
- Fundus examination
- Intraocular pressure measurement
- Examination of the retina