Ovariectomy - removal of the ovaries
introduction
One or both ovaries (ovaries) can be surgically removed. After the ovaries have been removed, a woman can no longer have children and is therefore sterile. An oophorectomy can be necessary due to diseases such as tumors or ovarian cysts. For example, if one or more large ovarian cysts are present, it may be necessary to remove the ovary if it is not possible to simply remove the cyst. An oophorectomy can also be performed to reduce hormone production. This plays a role, for example, in the treatment of breast cancer (Breast cancer) play a role if it is a type of tumor that grows depending on the estrogens produced in the ovaries. In addition, a twisting of one ovary (Ovarian torisone) is an indication for oophorectomy.

The twisting can lead to a blockage of the blood supply and a very painful ovarian infarction can lead to the death of the ovary. In some cases, an egg cell within the ovary is fertilized (ovarian pregnancy), which may also require removal of the ovary.
However, other causes can lead to ovarian pain during pregnancy, which may not lead to an oophorectomy. You can read more about this in the article Ovarian Pain During Pregnancy.
Usually the entire ovary is removed. If the tumor is benign, partial removal may also be an option. One speaks of an ovariohysterectomy if the ovaries and at the same time also the uterus (uterus) must be removed.
This is very controversial among medical professionals and in society prophylactic removal the ovaries. This is understood to be an oophorectomy, although no disease has occurred yet. Such a prophylactic intervention may only be carried out if there is an increased risk of developing a gynecological tumor, which should be reduced by removing the ovaries. However, removing the ovaries leads to significant side effects, which is why such an intervention should only be carried out under strict indications.
Ovary anatomy (ovaries)
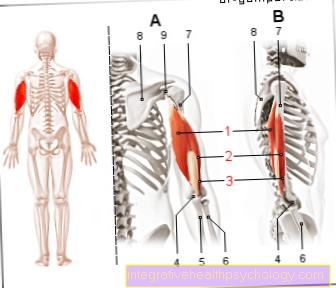
The two Ovaries are among the primary, female genital organs (corresponding to the male Testicles). You are in small pelvis side of the uterus and have a size of about 3x3x5 centimeters.
In the ovaries the ova and female sex hormones (estrogen and progesterone) educated. At childbearing age, the fallopian tube transports (tube) the egg cell from the ovary into the uterus. A Inflammation of an ovary will also be Oopheritis and occurs in most cases in combination with a Inflammation of the fallopian tube on (Adnexitis).
There are a number of benign (e.g. struma ovarii) and malignant (e.g. Ovarian cancer) Tumors that may appear in the ovaries. Other functional disorders of the ovaries represent polycystic ovarian syndrome, the Ovarian failure and Ovarian cysts The size and function of the ovaries decrease with age menopause the ovarian cycle comes to a standstill.
Illustration of the ovaries

- Ovary -
Ovary - Basic tissue of the ovary -
Stroma ovarii - Mature vesicle follicles -
Folliculus ovaricus tertiarius - Corpus luteum -
Corpus luteum - Uterine cavity -
Cavitas uteri - Cervix -
Ostium uteri - Ovarian ligament -
Ligamentum ovarii proprium - Fringed funnel of the fallopian tube -
Infundibulum tubae uterinae - Fallopian tubes -
Tuba uterina - Ovarian artery -
Ovarian artery
You can find an overview of all Dr-Gumpert images at: medical illustrations
Consequences of an ovarian removal

Becomes just one ovary removed, so the ovary on the opposite side takes over the hormone production, which mostly no symptoms occur. But when both ovaries be removed, so is afterwards no fertility more given that Woman is sterilized. But not only the ability to reproduce is affected by the removal of the ovaries, but also the production of important sex hormones. In the ovaries are among other things estrogen, progesterone and Androgen educated. These hormones control a variety of things important physical and mental functions in the body. Through the Oophorectomy the balance of the female hormonal balance is disrupted and the Menopause begins suddenly. Because of the Hormone deficiency by removing both ovaries it can become too dizziness, migraine, nausea, but also psychological complaints like changed sensory perceptions and perceptions up to one depression come. Also Bone density and Muscle mass decrease. Due to the hormone deficiency, it also occurs in many cases sexual problems, are often one Decrease in sexual desire and sexual motivation and enjoyment of intercourse are often completely absent. Typical symptoms of so-called menopausal symptoms such as Sweats, dry mucous membranes, Mood swings and insomnia can occur. The physical and mental complaints triggered by the hormone deficiency can be caused by a Hormone replacement therapy be counteracted. Usually the removal of the ovaries is followed by treatment with artificial estrogens and gestagens.
Post-oophorectomy hormones
Become both ovaries removed, there is a sudden Cessation of hormone production. Menopause is brought about artificially.
During the Menopause hormone production is also reduced, but it is a significantly longer period of several years. After surgery, a Hormone replacement therapy (Hormonal drugs) take over the slow adaptation of the body to the hormonal situation.
That way you just don't get strong menopausal symptoms intercepted, but also reduces the risk of cardiovascular diseases and osteoporosis.
Are part of Estrogens and or Progestins.
If female hormones are taken over a long period of time, this in turn increases the likelihood of breast cancer, thrombosis and strokes, and heart attacks.
Hormone replacement therapy is particularly useful Recommended for womenwho are still before the procedure not in menopause are located. In this way, sudden discomforts as a result of the procedure are reduced.
After the oophorectomy, it can take some time to find the right dosage and preparation. The duration of the therapy depends on the natural occurrence of menopause.
Operational sequence
The ovaries can be removed in a number of ways. The surgery takes place in general anesthetic. Before doing this, you may have to stop taking drugs that reduce blood clotting (e.g. Marcumar® or aspirin®).
As minimally invasive surgical procedure will the Laparoscopy (laparoscopy) viewed. At a laparoscopy there is only a small one Incision on the abdominal wallthrough which a laparoscope (a special endoscope) is inserted into the abdomen. The device is connected to a video camera and a light source so that the entire abdominal cavity can be seen. An instrument to remove the ovaries can now be inserted through another small skin incision. This Method is very gentle and the risk of complications is very low.
A further surgical procedure represents the so-called Colpotomy where an incision is made in the vagina to gain access to the ovaries.
The classic surgical method for removing the ovaries is the laparotomy represents. The Abdominal wall through a larger abdominal incision opened and the ovaries removed under the surgeon's direct line of sight. With this method, that is Risk of complications higher than the other methods. At the end of the operation, a drain is often inserted into the abdominal cavity so that wound secretion can be drained away. This drainage can be removed after a few days.
After the operation, excessive physical activity should not be exercised for a while; particularly heavy loads should not be lifted or carried. Likewise, sexual intercourse should be avoided for a while and medical checks should be carried out regularly.
Outpatient procedure
The bilateral oophorectomy or Removal of the ovaries is also in outpatient area possible. The minimally invasive procedure is performed laparoscopically (laparoscopy) carried out. This means that three small incisions are usually made under general anesthesia and the instruments inserted into the abdomen. In addition to the laparoscope, which functions as a small video camera, one or two other surgical instruments are required. The abdominal cavity is stretched with carbon dioxide for a better view in the operating field.
The Removal of the ovaries takes on average between 60 and 120 minutes. The surgical wounds are sutured from the inside with a self-dissolving thread.
After the operation without complications, the patient can go home on the same day.
Side effects
With the operation itself there can be some Complications come. For example, neighboring organs or anatomical structures (e.g. a ureter) get hurt. As with any surgical procedure, it can be too Bleeding or secondary bleeding come. In rare cases it occurs Nerve damagethat to Signs of paralysis, Numbness or mostly not permanent Urinary bladder dysfunction to lead.
Surgery can cause it to Adhesions in the abdomen come. Very rarely, there are serious complications like one Intestinal obstruction or a life threatening one Peritonitis. In the further course of the operation you can inflammatory communication channels (Fistulas) for example between vagina and rectum develop. The anesthesia harbors further risks as well as excessive ones Scarring, Pain and allergic reaction can occur.
By removing the ovaries it comes abruptly at the onset of menopause, the transition from the reproductive to the postmenopausal phase. Common complaints due to the Lack of estrogen occur Sweats, Hot flashes, Lack of libido and a Atrophy of the vaginal membrane. This leads to a corresponding Vaginal dryness, what to Painful intercourse, to Vaginal infections and Bleeding can lead. Also mental changes, Dizziness, easier fatigue, Listlessness, irritability, nervousness and Mood swings up to depressions are side effects of (bilateral) ovarian removal. It can lead to a Poor concentration, Urinary incontinence, constipation, diarrhea, Weight gain, Hair loss and reinforced Hair growth coming on the face. Most of these side effects go away (as with naturally induced menopause) after about a year to a year and a half.
Disadvantages of an oophorectomy
A bilateral Removal of the ovaries means a serious intervention for the woman concerned. As a result of the operation is a pregnancy naturally not possible anymore.
The hormone production by the ovaries dries up after the procedure and can cause a special Make hormone treatment necessary. Artificially produced combination preparations made from estrogens and progesterone or gestagens are used most frequently.
Among the most common complaints count after oophorectomy dizziness, migraine and nausea. In some cases, depression occurs.
In addition to decreasing Muscle mass and Bone density, the libido reduce. At the same time Removal of the uterus menopause is artificially brought about. As a result, those affected sometimes suffer more Hot flashes, sleep disorders, unbalanced mood and dry mucous membranes.
Tamoxifen instead of an oophorectomy
The drug Tamoxifen inhibits so-called Estrogen receptors and simultaneously stimulates progesterone receptors. It is a selective estrogen receptor modulator that is preferred in the Therapy of hormone-sensitive breast cancer (Breast cancer therapy) is used.
In the ovaries, among other things Hormone estrogen educated. In the case of hormone-sensitive forms of breast cancer, the Binding of estrogen to the tumor is prevented as this can affect growth.
For this can Tamoxifen used become or one Removal of the ovaries respectively. Which of the two procedures is the most suitable should be discussed with the attending physician.
It should be noted that after a bilateral oophorectomy no pregnancy more can come about. In addition, after removal of the ovaries, the onset of Menopausal symptoms.
Oophorectomy after breast cancer
More than half of malignant breast tumors grow dependent on female sex hormones. The estrogen produced in the ovaries in particular is essential for some types of breast cancer. When this link was discovered, many women with breast cancer had their ovaries removed. This slowed or stopped the growth of breast cancer due to the following hormone deficiency. However, the resulting infertility was very problematic, especially for young women, and the menopause that began immediately with its typical symptoms was also viewed critically.
Since the 1970s, oophorectomy after breast cancer has not been performed as a standard, because anti-hormone therapies have been available since then, with which tumor growth can be influenced by drug use. After the treatment, the menstrual period resumes in most cases and fertility is maintained.
Even if certain gene variants are found in a woman with breast cancer, the risk of developing ovarian cancer can also be increased. As part of this increased risk, an oophorectomy may be considered in women who have completed family planning. So far, two hereditary genetic mutations have been identified that lead to breast and often ovarian cancer in a high percentage of those affected. These are the genes BRCA1 and BRCA2 (BRCA = Breast Cancer). These two genes can be reliably detected through complex genetic tests; they are probably responsible for less than half (around 25-50 percent) of hereditary breast cancer cases. However, genome research in hereditary diseases is still in its "infancy". Many questions regarding a possible increase in the risk of the occurrence of certain diseases through the effects of gene variants are still open.
Read more about this: The breast cancer gene.
Postmenopausal oophorectomy
In the Menopause the woman's body goes through a phase of hormonal changein which the ovaries gradually stop working. The Shrink ovaries yourself and to produce always lower levels of hormones. But even after the menopause, hormone production does not stop completely.
When the uterus is removed after menopause, the ovaries are often removed at the same time. This way, one would like to have a potentially increased risk of cancer, especially for Minimize breast and ovarian cancer.
The bilateral oophorectomy is also used when newly occurring Cysts in the ovaries necessary after menopause. They can indicate a malicious event.
According to more recent findings, bilateral oophorectomy seems to be associated with an increased likelihood of diseases of the cardiovascular system. The risk of suffering a stroke or developing coronary heart disease increases by around 15 percent.