Physiotherapeutic treatment of chronic neck pain
Synonyms in a broader sense
Cervical spine syndrome, cervical spine syndrome, cervical syndrome, cervical syndrome, chronic cervical spine complaints, cervical spine pain, neck pain
In this topic I would like to convey background knowledge on the development of chronic neck complaints and "Helping people help themselves" to offer.
frequency
About 50% of all adults suffer from back pain, 30% of which are affected by recurrent (recurring) neck pain, about 15% become chronic.
Chronic neck pain with or without radiating pain are the third largest group of chronic pain pictures, in relation to chronic back pain they are in second place of the musculoskeletal pain pictures. Women are affected more often than men.

Appointment with a back specialist?

I would be happy to advise you!
Who am I?
My name is I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
The spine is difficult to treat. On the one hand it is exposed to high mechanical loads, on the other hand it has great mobility.
The treatment of the spine (e.g. herniated disc, facet syndrome, foramen stenosis, etc.) therefore requires a lot of experience.
I focus on a wide variety of diseases of the spine.
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You can find me in:
- - your orthopedic surgeon
14
Directly to the online appointment arrangement
Unfortunately, it is currently only possible to make an appointment with private health insurers. I hope for your understanding!
Further information about myself can be found at
causes
- Inadequately medically treated acute pain symptoms such as "Blockages" or intervertebral disc problems in the cervical spine
- Unhealed injuries such as the Whiplash
- Too long periods of rest after an acute incident
- Muscle imbalances, chronic muscle tension, description follows
- Psychosocial factors such as dissatisfaction at work or family, tendency to catastrophize, gain in attention through pain (no orthopedic background, secondary gain from illness)
- Cervical spine instabilitye arose e.g. through injury, muscle weakness, "weak" supporting tissue, herniated disc, congenital
- Persistent Bad posture in the workplace
- Chronic wear problems of the cervical joints
- Inflammation, basic rheumatic diseases
- tumor
- Eye problems
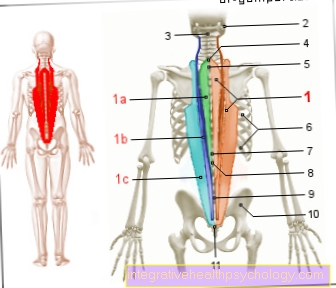
Muscle imbalance
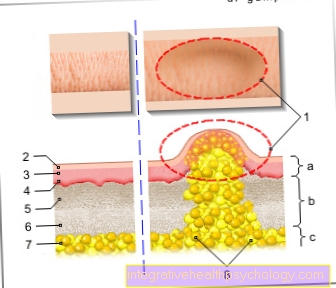
Muscular imbalance is not only caused by strength, stamina or stretching deficits, but often has its origin in a lack of muscular coordination (this means that the cooperation of the neck muscles with regard to the use of force and timing is disturbed) and in malfunctions of the neurological control mechanisms. The impairment in the deep, stabilizing muscle system and the rapid fatigue of the superficial neck muscles lead to overloading of certain muscle groups with strong tension and muscle trigger points (local hardening within a tense muscle strand) and the passive support system of the cervical spine. The result is pain and the feeling that the head is no longer supported by the neck.
Symptoms
One speaks of chronic neck pain if the symptoms persist for more than 3 months. Typical for chronic pain are changing symptoms, that is, there is constant pain that changes in intensity. Pain peaks are often in the morning after getting up and in the evening after the day's exercise, when those affected come to rest. In addition to the pain, there are often additional permanent restrictions of movement through the protection of the neck, so that the turning, bending and stretching movements of the cervical spine are reduced.
Chronic neck pain can be present as isolated symptoms, but they often occur in combination with shoulder and arm complaints, tension headaches or chronic back pain.
Acute pain / chronic pain
Chronic and acute: sometimes both come together
An acute neck pain can develop into a chronic pain event, but a chronic pain event can also be followed by an acute problem of the cervical spine.
Example: chronic neck pain and possibly headache are already present, the patient wakes up in the morning with an acutely painful dysfunction and cannot turn his head to the side.
Pain enhancer:
- Overhead work / overhead sports (e.g. tennis or handball)
- Exhausting activities with the Shoulder girdle
- Cold draft on the neck, damp, cold weather
- Acute pain symptoms acquired through blockages, accidents, etc.
- Increased "stress" in everyday life and at work
Pain memory:
The cause of the development and treatment of chronic pain has been intensively investigated in pain research for years, since chronic pain is an increasing problem on the one hand for the sick and on the other hand for the health care system.
PROTECTIVE FUNCTION OF THE BODY
ACUTE PAIN = BIOLOGICAL WARNING SIGNAL = PROTECTIVE FUNCTION of the BODY
In the event of acute pain (e.g. a disc problem or severe blockage due to "relocating the neck at night"), it is absolutely necessary and sensible to relieve irritated, extremely painful tissue. The Pain quality is described as sharp, piercing, cutting or pointed. At this stage, depending on the cause, a drug (pain reliever and anti-inflammatory), Manual therapy , physical measures such as heat, Electrotherapy, Tape and possibly careful active physiotherapeutic treatment for mobilization is indicated.
But even in the case of acute pain in the neck, the rest phase should be kept as short as possible in order to keep the risk of chronification as low as possible. The prerequisite for this is a consistent and sufficient Treatment of pain in the acute phase of pain.
Otherwise, there is a risk that, with persistent protective behavior and fear of pain, a process of unfavorable posture and movement patterns will develop in everyday life (e.g. the constant tilted position of the head), which the affected person no longer perceives as changed behavior after some time and therefore does not can correct. The consequence of the pain-related rest is a increasing decrease of the load limit and decreasing resilience in everyday life and at work.
But there are also those affected who do not take the path of sparing, but rather have developed perseverance strategies (“the happy bite-through”) for their everyday lives. Since you have no regard for your complaints, you constantly go over your limits. This group looks happy and carefree on the outside, so that the therapists, relatives and friends get the impression that those affected are symptom-free and easy to deal with. This behavior also acts as a so-called "pain trigger".
CHRONIC PAIN = NON-FUNCTIONAL PAIN = INDEPENDENT DISEASE PICTURE WITHOUT FUNCTION
The mechanisms of pain chronification are based on the ability of nerve cells to adapt to different stimuli. There is no precisely defined period of time between acute damage and the point in time when chronification occurs. Multiple tissue damage and inflammation lead to increased excitability of pain-conducting nerve cells in the brain if these injuries (medical trauma) have not been consistently and adequately treated with pain medicine. In addition, there are psychosocial aspects that significantly influence the individual perception of pain. The result of the increased excitability of nerve cells (the pain is "quasi stored in the cells" = Pain memory) is the excessive perception of pain stimuli or pain sensation in the case of stimuli that are not actually pain-releasing. The Pain quality is described as dull, boring, pulling, burning or tearing.
It has become a independent clinical picture developed.
THE PAIN THRESHOLD FALLS!
Those affected do not react appropriately to cold stimuli, low physical stress or stress (triggers), but they cannot be deliberately influenced with an increase in the pain of the familiar neck and / or headaches. This “oversensitivity” is difficult to understand for the patients themselves, but also for employers and people close to them. The lack of understanding and acceptance of the environment increases the emotional and psychological stress and thus in turn increases pain sensitivity.
The vicious circle
REPEATED TISSUE INJURY - ACUTE PAIN - INSUFFICIENT PAIN THERAPY - CARE - CHRONIFICATION - OVER-SENSITIVITY TO PAIN IRRITATIONS - REDUCTION OF EXERCISE LIMIT - INCREASED SENSITIVITY TO NEW ACUTE TRAUMATA
Read more on the topic: Duration of a cervical spine syndrome
Multimodal pain therapy
The consequence of the knowledge about the manifold development mechanisms of chronic neck pain should be a comprehensive treatment concept be.
The Multimodal pain therapy (Therapy that includes different treatment approaches) is only interdisciplinary in a team Doctor, psycho- and physiotherapist and has already proven itself in the treatment of chronic back pain.
Be proven by this multimodal treatment concepts achieved the best results. Unfortunately, however, in reality they are often not consistently or only partially feasible for reasons of cost or time.
Medication
To drug treatment so-called centrally acting painkillers are used for chronic pain, which reduce the increased excitability of the pain-processing nerve cells. Depending on the daily form or daily stress, short-term painkillers are combined with long-term medication.
Another possible application is the direct infiltration of local anesthetics and / or cortisone into limited, highly sensitive muscle hardening = muscle trigger points.
acupuncture
Although not included in the catalog of services of the statutory health insurance companies, the acupuncture also with chronic neck pain (Cervical spine syndrome) and Headache Experience has shown that it has a good analgesic effect.
You can find further information under our topic: acupuncture
TENS device
The abbreviation TENS stands for Transkutane E.electrical NErven stimulation, in which chronic pain can be positively influenced with the help of weak, low-frequency stimulation currents.
The great advantage of this method is that the patient can self-treat using small, easy-to-use devices at home.
psychotherapy
In psychotherapeutic treatment, the psychosocial causes as the mechanism behind chronic pain are examined and treated. With the help of pain management strategies, behavior changes in the sense of Active against the pain, permanent pain reduction and increased resilience can be achieved.
- Relaxation procedure
- Biofeedback
- Body therapy such as Feldenkrais, Tai Chi, Qi Gong
- Pain management training
- Cognitive behavioral therapy
- Psychotherapy based on depth psychology
- hypnosis
- Possibly inpatient multimodal therapy offer
Development and summary
Development:
Due to the demographic development, an increased proportion of older people in employment can be expected. In particular, activities that stress the neck and shoulders and the generally increased stress in family and at work will lead to increased pain in the postural and musculoskeletal system. So in the future the need for treatment in the area of “chronic neck and back pain” will continue to increase.
In view of the skyrocketing health care costs, which are largely caused by patients with chronic pain disorders, more attention should be paid to prevention programs and treatment concepts in the group. With the rehabilitation sport program of the health insurance companies, a step in the right direction is definitely taken in the case of existing complaints.
Summary :
For the treatment of patients with chronic neck pain, the active group programs with the concept of the neck school are more successful than the individual treatment. Precondition for the therapy success is an exact previous diagnosis, a possible pre-treatment and a consequent active participation of the participants also beyond the group program. In connection with a multimodal treatment concept (medication, behavior change in dealing with pain, consideration of psychosocial aspects), specific strength training of the shoulder and neck muscles in physiotherapy is particularly suitable as a very effective and inexpensive treatment method. In view of the rising costs in the treatment of chronic pain patients, the multimodal concepts are primarily more expensive, but secondarily cheaper, more sustainable and more effective.
<- Back to the main topic of the cervical spine syndrome