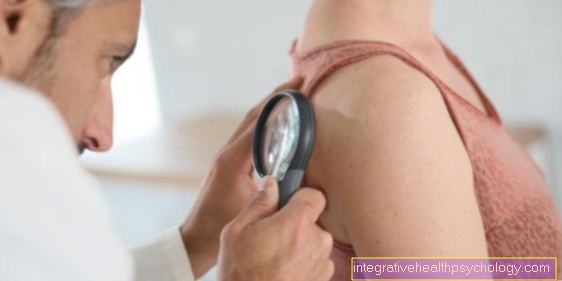
The animal hair allergy
introduction
People who suffer from an animal hair allergy can have it in different forms. For some patients, it is sufficient that the corresponding animal is in the room for the symptoms to occur; for other patients, the allergy only occurs when there is direct contact with the animal.
The trigger of the allergy, however, is not the animal hair itself, but the proteins in the animal excretions that settle in the fur of the animals. These proteins mostly come from the faeces, sweat, sebum or urine of the animals. Frequent animal hair allergies are directed against the proteins (Proteins) in the skins of dogs, cats, rabbits, and horses. The allergy can also occur in animals that do not have hair in this sense, such as parrots and budgies. This is because these animals naturally also have excretions and the proteins adhere to their plumage just as they do in the fur of rodents, for example. According to estimates, every 10th person in Germany is affected by an animal hair allergy.

Emergence
Basically, all allergies arise from an overreaction of the immune system.
Why allergies occur more frequently, especially in industrialized nations, has not yet been conclusively clarified. However, there are various theories about the development of an (animal hair) allergy. For one thing, there are different classes of so-called immunoglobulins in the immune system that mediate the immune system's response. The immunoglobulin E (IgE) not only mediates the immune response to parasite infestation, but also to an allergy. This led to the theory that the decline in parasite infestations in industrialized nations leads to "underemployment" of the immune system and that the immune system is looking for a new type of employment through the development of an allergy.
Also the "Hygiene hypothesis“Considers some kind of underemployment of the immune system. This hypothesis says that a very sterile environment, as is often the case in industrialized nations, promotes the development of an allergy. Since our environment is kept very clean and as free as possible from pathogens of a disease, our immune system seeks another task here too and overreacts when it comes into contact with the substance that causes the allergy (allergen).
As is so often the case, the development of an animal hair allergy is related to genetics, so the probability of developing an animal hair allergy increases sharply as soon as both parents already suffer from an animal hair allergy. It has also been discussed whether vaccinating children can cause allergies, but several studies have already been carried out and no evidence of vaccination-associated allergy has been found.
The human body must first have had contact with the allergen in question before it can develop an allergy. The immune system reacts neutrally to completely unknown substances upon first contact. Only when the immune system has had the opportunity to "train" the immunoglobulins E (IgE) can they react to the allergen. If the instructed immunoglobulins E now encounter an allergen, they activate the phagocytes (mast cells) of our body, these mast cells in turn release histamine and inflammation mediators. So the same path is taken here that the body chooses in the event of inflammation.
Read more about this under Allergic reaction
Symptoms
From the way described above, it can be seen that the symptoms of an animal hair allergy only occur if there is or has recently been in contact with the animal in question.
Symptoms can be from a Skin irritation after contact (Contact eczema) to one allergic shock (anaphylactic shock) pass. The so-called contact eczema usually occurs a few minutes after contact with the animal and can persist for between a few hours and several days. The affected skin area is then reddened and patients usually also complain of severe itching.
It can also become a allergic conjunctivitis (Conjunctivitis) come. The affected patients have very red and itchy eyes, which can also water.
In some patients, it happens severe and sudden onset of shortness of breathas soon as they are in the vicinity of the animal, which is the cause of their animal hair allergy. The symptoms often improve quickly in those affected when they are out of reach of the animal.
In some patients, the bouts of shortness of breath also go into allergen exposure allergic asthma or one chronic sinus infection (chronic rhinosinusitis) over.
In a few people affected, the animal hair allergy manifests itself in the form of a allergic shocks (anaphylactic shock). Should this happen, is Call an emergency doctor immediately, as this is an acutely life-threatening situation.
Throat irritation with an animal hair allergy
Coughing as a symptom of animal hair allergy is less common. This often requires large amounts of animal protein in the air. If these are inhaled in large quantities in the vicinity of the animal, a hypersensitivity reaction can occur.
The immune cells in the airways recognize the protein as foreign and harmful and try to get it out of the body. Coughing fits can be the result. The airways can then swell as an allergy reaction and make the passage of further particles difficult.
Learn more at: Cough if you have an allergy
Difficulty breathing in an animal hair allergy
Just as the cough occurs as a defense reaction against the inhaled animal proteins, shortness of breath can also arise. In contrast to the skin of the body, mucous membranes do not have a horny surface to repel proteins of this kind. Contact with an allergen can cause them to swell, itch and cause problems.
The mucous membranes in the oropharynx swell so much that breathing becomes difficult. Especially in the throat at the transition to the larynx, even slight swellings can cause a significant blockage of the airways.
Asthma can also occur as an allergic reaction. The allergic reactions can even block breathing completely, leading to unconsciousness and an acute medical emergency.
Symptoms on the skin
Symptoms on the skin are very common with animal hair allergies. Often no direct contact with the animal is necessary, but spatial proximity is sufficient. This is due to the fact that the allergens can pass into the air due to their small size.
Itching occurs in the accessible areas after just a few minutes. This often affects the skin of the face, hands and forearms. In addition, reddening occurs on the affected areas with so-called "Urtikae". These are wheals, a symptom of hives. If you leave the room in which the animal is, the symptoms on the skin also subside within a few minutes.
With other forms of allergy, which occur much less often, rashes known as "eczema" can occur for hours. The development of the symptoms takes significantly longer and the healing after the end of exposure, i.e. the time of contact with the allergen, can also take several days.
diagnosis
There are various options for diagnosis.
The most famous of these is the so-called Prick test. Here, with a small lancet, various potential allergens are applied to the arm or back and a negative control, for example saline solution, and a positive control, for example histamine. The result is then checked every 5, 10 and 20 minutes. A Redness and a swelling in this case mean that the patient is allergic to the applied allergen. After the test, the allergen samples are of course removed again.
Of the Intracutaneous test is based on the same principle as the skin prick test, except that the test substances are not applied with a lancet, but given under the skin in tiny amounts with a small syringe.
If there is a risk of a violent allergic reaction to the test substances, the Rub test be applied. Here the test substances are simply rubbed onto the underside of the arm; in the event of a positive test result, this is where they form Wheals and redness.
Another variant of the provocation test is to take blood shortly after the patient has been in contact with the allergen, i.e. the protein from the animal's excrement, and then to determine the amount of immunoglobulin E. In principle, this can also be carried out if the patient has not had any previous contact with the allergen. Then the level of immunoglobulin E in the patient's blood is simply determined. It should be noted, however, that the amount of IgE does not have to correlate with the severity of the patient's symptoms and that the IgE concentration is also greatly increased in parasitic diseases. With this type of diagnosis, it must therefore be known whether there are other diseases so that a statement can be made based on the amount of immunoglobulin E.
The allergy test
If there is a suspicion of an allergy, it can now be quickly determined with a so-called "prick test". Many ENT doctors offer this test. The allergy reaction is mainly consciously provoked on the forearm in order to determine the exact trigger. To do this, a structured aqueous solution containing the allergen is dripped onto the skin at various points on the forearm.
In the case of dog hair allergy, the solution contains the protein "Can f1“, In cat hair allergy the protein "Fel d1". A small needle is then used to stab the arm in the same place, just to open the top layer of skin.
If there is an allergy to the applied protein, this area begins to itch in the following minutes and forms a reddish wheal. After about 15 minutes, the symptoms can be read accurately to determine the allergies.
You can find more information here: The prick test
Cost of the test
The cost of the test may vary depending on the amount of substances tested. As a rule, some substances are tested together in order to obtain the largest possible overview of the allergies. Each substance that is tested costs around € 5.
However, if there is already a slight suspicion that allergies are present, the health insurance companies will take over the prick test in any case.
Therapy and prophylaxis
The therapy of an animal hair allergy depends largely on the severity of the allergy. If it is an animal hair allergy that only occurs in direct contact with the animal, then the most important prophylaxis, also for children, is to avoid contact with the animal and to prevent the animal from jumping on furniture such as the bed. This can prevent allergic contact eczema from occurring. If contact eczema has already occurred, it is advisable to soothe the itching first by cooling, for example with cold water. If the contact eczema persists for several days, you can first apply even mild creams, e.g. with hydrocortisone. In more severe cases, the doctor can prescribe stronger creams containing cortisone, but these must not be used on the face and should also be tapered to the so-called Rebound effect to avoid. The rebound effect describes the recurrence of contact eczema without repeated contact with the animal due to the sudden withdrawal of the cortisone cream.
In the case of an allergic conjunctivitis (conjunctivitis), there is no need for direct contact between the conjunctiva and the animal's fur. Here it is enough that the animal was first stroked and then a little later the eyes were rubbed with the appropriate hand. As a prophylaxis, wash your hands thoroughly after every contact with the potential trigger of the animal hair allergy. However, there is also the case in which the mere presence of the animal is sufficient to trigger a reaction of the conjunctiva, in which case it is advisable to avoid the animals. If, despite the precautionary measures, an allergic conjunctivitis has occurred, the eye should first be rinsed very carefully. Even if the eyelashes stick together with pus in the morning, this should first be carefully washed off with warm water without soap. Antiallergenic eye drops are ideal for calming the eyes. If pus develops as described above, an ophthalmologist should be consulted.
These eye drops are often the drug Vividrin® eye drops. You can find more information on this topic at: Vividrin acute eye drops
If there is a sudden shortness of breath due to the animal hair allergy, the doctor should be informed of this event so that he can prescribe a quick-acting spray. These sprays are mostly active ingredients that quickly open the bronchi, so-called beta-mimetics. These act on the beta receptors in the lungs and, by widening the airways, make the supply of oxygen easier. A side effect of these drugs can be a faster heart rate because another beta receptor sits on the heart and is also stimulated by the active ingredient and then reacts by increasing the heart rate.
In addition, an antihistamine should be taken regularly well before any planned exposure to animals known to be allergic to. The histamine release of the mast cells on contact with the allergen is reduced and the reaction to the animal hair is weaker or sometimes even completely.
What medicines are there for a pet hair allergy?
Therapeutically, avoiding the allergen must be the main focus in the treatment of animal hair allergy.
However, if symptoms are already present or if the situation is inevitable, various drugs can be used in different stages of the symptoms.
An important group of drugs is the group of so-called antihistamines. They prevent the release of the messenger substance histamine, which causes the symptoms of the allergy. Antihistamines can be dosed differently and can be associated with side effects.
In the case of severe allergic reactions, other drugs must be used as a priority. Modifications of the cortisone, so-called "glucocorticoids", can suppress the immune response and contain the allergic reaction in the case of severe allergies in tablet form or as an infusion. They are mainly used in everyday clinical practice for allergies that require medical treatment.
In the case of so-called "anaphylaxis", the messenger substance adrenaline may have to be administered as a spray or syringe. This stabilizes the circulation in the event of an exuberant allergic reaction.
Desensitizations can be carried out for long-term therapy of the allergy.
Nowadays this can be done via injections or medication over a long period of time. A weakened allergen is fed into the body so that the immune system gets used to the substance.
homeopathy
The homeopathic treatment of animal hair allergy must be made dependent on the degree of allergy. Acute emergency situations with shortness of breath and severe runny nose cannot be treated with homeopathic remedies. In the case of latent allergies, on the other hand, which occur from time to time with cold symptoms, homeopathic remedies can be used.
In the case of more severe forms of allergy, they can be taken in addition to drug treatment to stimulate self-healing here as well.
Typical remedies that are used here are “Calcium Carbonicum” and “Galphimia Glauca”. In order to have a detailed homeopathic anamnesis carried out, a homeopathically trained doctor should be consulted.
These are highly diluted active ingredients that cannot cause any side effects or damage to the body. This is intended to stimulate the body with certain information in order to stimulate its own self-healing powers in the fight against the allergy.
desensitization
Desensitization is the only therapy method in the treatment of allergies that aims at a long-term cure and alleviation of the disease. The principle behind this is to confront the body with the triggering protein in animal hair and to get it used to it.
The amount should be increased step by step. The confrontation occurs through the injection of a solution that contains the allergen. This is injected every 1-3 weeks over a period of 2-3 years. It is an elaborate therapy method that provides an opportunity to alleviate constant problems and other therapeutic failures.
Further information is available under our topic: desensitization
Since the animal hair allergy can also lead to chronic sinusitis, an ear, nose and throat doctor should be consulted in this case. First expectorant drugs should be taken, if this therapy is frustrating, that is, no longer works, a fenestration of the maxillary sinus, which also belongs to the paranasal sinuses, can be carried out in the turbinates so that the secretion can flow away more easily.
In addition, the animal hair allergy can lead to chronic asthma. This form of asthma is treated with various forms of beta-mimetics and cortisone derivatives. For the basic therapy there are initially either long-acting beta-mimetics or cortisone derivatives and for acute attacks a short-acting beta-mimetic. If the asthma progresses, the long-acting beta-mimetics and cortisone can also be given together.
A variant to get rid of the pet hair allergy forever is the desensitization. The substance that triggers the animal hair allergy is either injected under the skin with a small syringe or placed under the tongue as a tablet. The duration of the desensitization is between 2 and 5 years, during which the patient receives a new dose of the substance every 4 to 6 weeks. The dose will increase over time. This is to ensure that more class G immunoglobulins are formed, which react to the allergen, and less class E immunoglobulins, which of course promote the release of inflammatory mediators such as histamine and leukotrienes. Of course, there are also risks and side effects with such a therapy. On the one hand, there is a risk that the patient will react to the direct ingestion of the allergen with an allergic shock, which is an absolute emergency. Less drastic reactions are the formation of itchy wheals and redness. Anyone who would like to have a desensitization carried out in order to get rid of their animal hair allergy must be aware that this is a long treatment, the termination of which can mean the previous treatment is completely useless. It can also happen that the desensitization has no effect at all on some sufferers. Therefore, when choosing the treatment, one must always weigh the symptoms of an animal hair allergy and its prophylaxis against the possible side effects of a therapy.
Which cross allergies are there in a pet hair allergy?
Cross allergies are sensitization to different allergens due to a pre-existing allergy. If two allergens are similar in structure, it is likely that many people will develop an allergy to both substances.
Animal hair allergies can lead to cross allergies, especially among each other. If you have an allergy to cat hair, you probably also suffer from an allergy to the hair of other animals.
However, the severity of cross-allergies varies greatly from person to person, depending on the type of allergen, the animal's hair loss and numerous other factors.
Cat hair allergy
Many people are of one Cat hair allergy affected. An allergy is a sensitive reaction of the body to certain substances that are theoretically harmless. The immune system mistakenly sees these substances as harmful and reacts with defense mechanisms such as sneezing or coughing.
With a cat hair allergy, those affected are not allergic to the cat hair itself. The allergy is directed against a protein found in the cat's saliva. When the cat cleans itself and licks its fur, the proteins get into the animal's hair. This spreads over the hair Allergen anywhere in the household. The proteins are very small and can therefore also pass into the air we breathe. Therefore a thorough cleaning and reduction of the cat hair is hardly of any use.
However, there are some types of cats that are suitable for allergy sufferers. Overall, they produce fewer allergens in the saliva and can therefore be used as "hypoallergenic " are designated. In the case of a strong allergy reaction, however, these also trigger the typical symptoms.
The first sign of cat hair allergy is a sudden sneeze. A cough can also be possible. In close proximity to the cat, the skin can quickly become itchy with rashes and wheals. In an emergency, the mucous membranes in the throat and pharynx can swell and lead to collapse and breathing problems. Such a strong allergic reaction is possible but very rare in cats.
Also read on here: Cat hair allergy
Dog hair allergy
The Dog hair allergy occurs significantly less often than the allergy to cat hair. The mechanism of allergy development is similar in both forms. Again, the allergy is actually directed against a protein from the dog's saliva or superficial scales. It gets into the fur and can spread over it or it can be absorbed into the air.
In dogs, there are some species that are completely free of the allergy-causing protein. Long-haired breeds, for example, have a significantly lower potential for triggering allergies. Again, the most common immediate symptoms are runny nose, itching, itchy eyes and rashes. There are many therapy options for dog hair allergies today. In addition to medicinal methods, desensitizations can also be carried out.
The editors recommend the article: Dog hair allergy
Animal hair allergy in children
Children are particularly often affected by animal hair allergies. There are several factors that can positively or negatively influence the development of the allergy. In children, it is important to recognize and treat the allergy so that no allergic asthma develops as a result. Desensitizations are also a good and important therapeutic alternative in childhood.
One factor influencing the development of allergies is the length of time breastfeeding takes in infancy. Longer breastfeeding in the first few months of life can have a positive effect on the immune system in this regard. Then it is important to feed the child food that causes allergies in many people.
In many cases it is beneficial to expose the child to a variety of allergens before they can develop an allergy.
A proven negative influence on the development of animal hair allergy is cigarette smoke, which is in the air, for example by parents.
Find out more at: Allergies in children
Which animals are suitable for me with an animal hair allergy?
In principle, allergies are very different from person to person and can vary greatly from animal breed to animal breed.
If an allergy is confirmed by experience or an allergy test by the doctor, the only options left are to do without a pet or to purchase a so-called "hypoallergenic" animal.
Animals without hair are the best alternative.
This can for example
- Snakes,
- Turtles,
- Fishes,
- Lizards,
- Be budgies and canaries.
If you still want a dog, cat or other hairy animal, different breeds should be examined in pet shops and any allergic reactions tested.
Different dog and cat species have a slower coat change and thus a lower spread of the allergy-causing protein.
Long-haired animals also have a significantly lower overall hair loss.
However, hypoallergenic animals are not an alternative for people with severe allergies.
Even hamsters, mice, guinea pigs or rabbits can sometimes cause severe allergies.
Even if there is currently only one allergy to cat hair, there is a high probability that allergies to dog hair will also develop after purchasing a dog.
Is a pet hair allergy hereditary?
Allergies and tendencies to pathological reactions of the immune system have an inheritable component.
Even with one affected parent, the probability of developing an allergy is almost 50%.
If there are two affected parents, the probability is even higher.
The mother's diet and behavior during pregnancy can also influence potential allergies in the child.
In this way, children in the womb can be sensitized to certain allergens and react with allergic reactions to the allergens immediately after birth.
The parents' smoking behavior also shows an increase in allergies in children.
However, a longer period of breastfeeding has a positive influence on the child. This can prevent many allergies. Targeted feeding of certain allergens can also reduce the rate of food allergies.












.jpg)