Ureteral stone
Synonyms
Medical: Ureteral stone
English: ureteral calculus
Ureter disorders
Ureteral stone, urinary stones and kidney stones
Kidney stones affect men and women equally often.
With age, the risk of developing a stone in the kidney increases. Stress can adversely affect the appearance of urinary stones / kidney stones.
The climate can also have an impact on the development of kidney stones. The more water is lost through sweating, the more concentrated the urine.

If the urine is too concentrated or certain substances are in abundance, possibly due to poor nutrition or certain congenital disorders in the breakdown of waste products in the body, the likelihood of urinary stones is greatly increased because these substances can no longer dissolve in the urine and fall out as crystals . The so-called pH value, i.e. the acid content, of the urine plays an important role here. Depending on how much acid there is, some stones / urinary stones form more easily.
An inflammation in the urinary system or if the outflow of urine is disturbed, for example by congenital malformations, can also promote the development of a urinary stone.
The body normally produces substances that inhibit the formation of urinary stones. If there is too little of it, urinary stones can form more easily. You can distinguish between different stones based on their composition and origin.
On the one hand, the urinary stone and kidney stone in the renal pelvis (Pelvis renalis) anchored to the wall. These are called chalices or fixed stones. They can loosen and be washed into the urinary drainage system in the ureter. On the other hand, uric acid and cystine stones arise freely in the urine, simply because the concentration of these substances is too high or because the pH value of the urine has changed. They can arise anywhere in the urinary system.
Figure ureteral stones

Ureteral stones
Ureteral stones
- Right kidney - Ren dexter
- Ureter - Ureter
- Urinary bladder (female / male) -
Vesica urinaria - Ureter orifice -
Ureteral ostium - Female urethra -
Urethra feminine - Renal pelvis -
Pelvis renalis - Prostate gland - prostate
- Male urethra -
Urethra masculina - Common pelvic artery -
Common iliac artery
Ureteral strictures (Ureteral narrowing)
A. - Exit from the renal pelvis
into the beginning ureter
(here the left kidney)
B - crossing the common
Pelvic artery
(Common iliac artery)
C - entry into the urinary bladder
a - Female urinary bladder
with surroundings from the front
b - Male urinary bladder
with surroundings from the front
You can find an overview of all Dr-Gumpert images at: medical illustrations
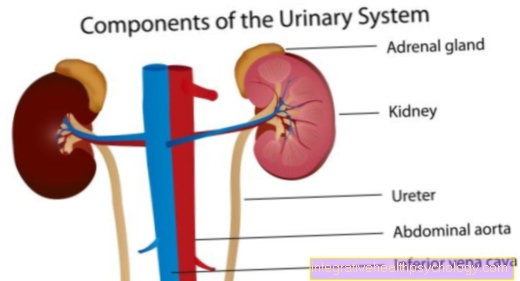
Figure ureter

- Ureter - Ureter
- Transitional epithelium - Urothelium
- Shift layer of the
Mucous membrane - Lamina propria - Inner longitudinal layer -
Stratum longitudinal internum - Outer longitudinal layer -
Stratum longitudinal externum - Middle ring layer -
Circular stratum - Connective tissue covering with
Blood vessels - Tunica adventitia - Aortic fork - Aortic bifurcation
- Rectum - Rectum
- Urinary bladder - Vesica urinaria
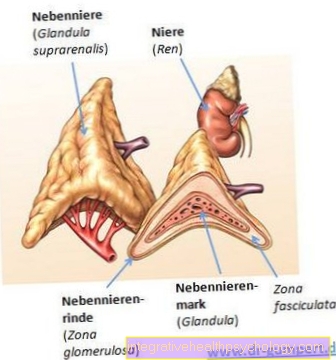
- Adrenal gland -
Glandula suprarenalis - Right kidney - Ren dexter
- Renal pelvis - Pelvis renalis
- Lower vena cava - Inferior vena cava
You can find an overview of all Dr-Gumpert images at: medical illustrations
Most Stones (70%) are made up of calcium oxalate if too much calcium or oxalate im urine is present or there are too few stone formation-inhibiting substances.
Uric acid stones (10-15%) arise when purine accumulates. Purine is a breakdown product of, for example DNSthat we eat in larger quantities when we eat meat. If the breakdown is disturbed, possibly due to a congenital defect or if the kidney is damaged or because of an excessive intake of meat and alcohol is overwhelmed, these stones arise.
Calcium and magnesium phosphate stones (5-10%) are so-called Infection stoneswhich are formed when bacteria change the pH of the urine through their waste materials when they become infected.
Cystine stones are rare (1-2%) and are mainly composed of the protein component Cystine together. They mostly arise due to a hereditary enzyme deficiency.
Xanthine stones and other stones make up less than 0.5% of all kidney stones.
People with Ureteral stone are especially aware of the stones when they are in the ureter and cause pain by stretching the ureter wall.
These pains through a ureteral stone are mostly colic-like (that is, they come and go in the form of waves) with a wave-like spread in the flanks, in the bladder or in the Scrotum (scrotum) at the man or the Labia (Labia majora) in the woman.
In addition, if the urine is blocked, the urge to urinate cannot be resolved. If the urine congestion persists, it may cause inflammation or a Blood poisoning with urine substances that cannot be excreted (Urosepsis).

Ureter stones (ureter stones) can be identified primarily through imaging procedures such as ultrasound or contrast agent examinations (intavenous urogram).
In the ultrasound he can Ureteral stone that are larger than 2 mm. But the urine test can also provide an indication of a ureteral stone if blood or small urinary stone crystals are present.
Depending on the crystals discovered and the pH value, conclusions can also be drawn about the cause.
A blood test can also be informative if so-called urinary substances such as creatinine occur more frequently.
Since 70-80-% of urinary stones pass spontaneously because they are propelled by the above-described peristaltic wave of the ureter, an antispasmodic such as Buscopan® and treat pain medication.
Uric acid stones, which sometimes arise due to the acidity, you give alkalizing drugs that neutralize the urine a little and thus dissolve the stones, e.g. Uralyt U (this is the salt of citric acid).
If the stones cannot be dealt with with medication, one can resort to so-called endourological measures, which are characterized by inserting a special catheter through the ureter past the stone and allowing the blocked urine to drain away. The stone is usually pushed back into the renal pelvis, where it can be smashed more easily (see below).
Stones can be smashed by a special technique from the outside by certain radio waves or electromagnetic waves without having to intervene directly in the body (extracorporeal shock wave lithotripsy). No general anesthesia is required and the small debris can easily be expelled through the ureter and bladder.
In the case of very stubborn or large stones, invasive access to the stone must also be created through the skin (percutaneous nephrolitholapaxy).
Since the Ureteral stone (Ureteral stone) are particularly difficult to localize, they are usually treated endoscopically anesthesia. That means you lead a hose equipped with a camera over the urethra (urethra), the bladder (Vesica urinaria) in the ureter and can then precisely remove the stone with the help of the picture.
You can prevent the formation of urinary stones if you adjust your diet accordingly, exercise a lot and drink plenty of fluids. You can also magnesium and citrate take to prevent the formation of stones. In the case of infection stones, L-methionine is often given a protein component to acidify the urine.
The ureter can be affected as part of a urinary tract infection caused by bacteria moving up the urethra into the bladder. The formation can be promoted by urinary stones.
Is treated with Antibiotics such as timethoprim and sulfamethoxazole (e.g. Cotrim / Cotrim forte) or amoxillin, Cephalosprorins or gyrase inhibitors (e.g. Ciprobay or Tavanic).
You can find further information under our topic: Kidney stones


.jpg)