Macular edema
Definition - macular edema
Macular edema is an accumulation of fluid in the area of the macula. The macula is also known as the "yellow spot" and forms the area of sharpest vision on the retina (retina) of the human eye. In the macula, the density of the sensory receptors that enable vision is most dense, which gives us a clear overall picture.
Macular edema can significantly affect the eyesight of the affected eye, as the accumulated fluid causes swelling of the retina. The affected people can no longer focus on objects properly and their vision is blurred. There are various causes for the development of macular edema. The ophthalmologist diagnoses the disease and can then initiate the appropriate therapy.

Recognizing macular edema
What are the symptoms of macular edema?
Characteristically, macular edema is characterized by a slowly advancing, insidious course. In the course of the disease, sudden visual problems can occur. These include blurred vision and color vision problems. In addition, objects can no longer be sharply focused. Occasionally, those affected also suffer from visual impairment or a "gray haze" in their field of vision.
Other symptoms are dark spots that hover over the field of vision and impair vision. Double vision or a red haze can also occur. Due to the visual impairment, the patients are severely restricted in many areas of life. This significantly reduces the quality of life and increases the risk of developing depression.
In particular, diabetic macular edema can be symptom-free for a long time and patients have only slight visual problems during the course of the disease. Over time, the disease progresses and the eyesight deteriorates more and more. If the diabetic macular edema is not treated in time, there is even a risk of blindness in the affected eye.
How is macular edema diagnosed?
If you have visual problems or any other symptoms that may be attributable to macular edema, you should see an ophthalmologist immediately. The doctor discusses the symptoms with the patient and conducts various examinations, such as an eye test and an eye examination (Fundoscopy or Ophthalmoscopy), by. This allows pathological changes to the macula to be determined and a diagnosis of macular edema to be made. In some cases, so-called fluorescence angiography can also be performed to visualize the blood vessels on the retina.
Treating macular edema
How is macular edema treated?
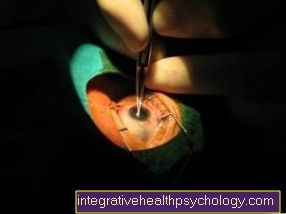
Specific treatment for macular edema depends on the stage of the disease and the cause of the fluid retention. In most cases, laser treatment is used. The ophthalmologist irradiates the affected area on the retina with high-energy laser light, which closes leaky vessels. This treatment also prevents the formation of unwanted new blood vessels.
Another option for treating macular edema is to administer medication. Common active ingredients are non-steroidal anti-inflammatory drugs (NSAIDs), steroids, VEGF inhibitors or carbonic anhydrase inhibitors. These substances are either given in the form of eye drops or injected directly into the eyeball. In rare cases, systemic treatment in the form of tablets or infusions may also be necessary.
Diabetic macular edema is treated with drugs applied directly to the eye and laser treatment. Diabetics who are at risk of developing diabetic macular edema must above all ensure that their blood sugar levels are optimally adjusted. Blood pressure should also be checked regularly and, if necessary, lowered to prevent damage to the retina. Smoking, unhealthy diet and obesity are further risk factors that the patient can reduce at will.
Do I need an injection with macular edema?
Certain conditions underlying macular edema may require that medication be injected directly into the diseased eye. After a local anesthetic, the ophthalmologist injects preparations that contain cortisone or so-called VEGF inhibitors as active ingredients. The injection is made directly into the vitreous humor of the eye.
Cortisone is a steroid hormone that has a general anti-inflammatory effect and is used for various diseases. VEGF inhibitors block the effects of a substance produced by the body that is directly responsible for the formation of new blood vessels. This allows targeted intervention in the cause of the macular edema.
Which homeopathic remedies can help with macular edema?
Homeopathic medications and naturopathic treatments can help treat macular edema. The aim of these alternative treatment methods is to improve the state of health and strengthen the body's own self-healing. Trained homeopaths can judge whether homeopathic treatment makes sense depending on the cause and form of the macular edema.
Homeopathy should not be used alone in this disease, but serves as an accompanying therapeutic measure to conventional medicine, since inadequate treatment can lead to severe damage to the optic nerve.
Prevention of Macular Edema
What are the causes of macular edema?
Macular edema can have various causes. Often there is inflammation in the eye, such as retinal inflammation (Retinitis) or inflammation of the middle skin of the eye (Uveitis) is based. The inflammation makes the blood vessels more permeable and fluid is pressed into the surrounding tissue. Calcifications of blood vessels in the eye or a blood clot (thrombus) in an artery or vein lead to blood congestion and, as a result, to swelling of the retina.
Even after operations on the eye, for example after cataract surgery (Cataract surgery), there is an increased risk of developing macular edema. People with high blood pressure (arterial hypertension), increased blood lipid levels (Hyperlipidemia), Diabetes mellitus, or inflammatory eye diseases have an increased risk of developing macular edema.
Course of macular edema
What are the chances of recovery from macular edema?
The chances of recovery from macular edema depend on the type of disease (diabetic or cystic macular edema) and how severe the symptoms are. A doctor should be consulted immediately in the event of complaints, especially if the color vision is changed, as there is a risk of permanent visual damage or even blindness if not treated.
Cystic macular edema, which usually forms as a result of eye surgery, usually has a good prognosis and disappears after a few weeks. The chances of recovery are also good with RCS, which is caused by stress. If macular edema is due to diabetic retinopathy, the prognosis is worse. This is because the symptoms often only appear when the retina is already clearly damaged. Diabetics should therefore visit an ophthalmologist regularly in order to identify and treat pathological changes in the eye as early as possible.
What are the consequences of chronic macular edema?
Despite appropriate treatment, macular edema can recur in some patients (Recurrence) and cause serious damage to the retina. The result is permanent visual impairment and in the worst case even permanent loss of sight in the affected eye.
You might also be interested in this article: Causes of blindness
Can stress cause macular edema?
Mentally stressful situations and chronic stress can lead to the development of macular edema and visual disturbances. This clinical picture is called Central retinopathy serosa (RCS) refers to and often affects young, ambitious men between the ages of 30 and 50. For this reason, the RCS is also called “manager disease”.The exact cause of macular edema is unclear, but fluid leaks from the vessels and the fluid collects behind the macula.
Typical symptoms of RCS are sudden deterioration in vision, distortions, and visual field defects. A distinction is made between an acute course, which usually heals spontaneously within a few weeks, and a chronic form. The chronic form should definitely be treated with laser therapy or medication, otherwise there is a risk of permanent visual impairment.
Further questions about macular edema
Does macular edema occur after cataract surgery?
Cataract surgery is an eye surgery that is used on patients with cataracts. An artificial lens is inserted into the eye. Although this is a routine procedure, there is a risk that, in rare cases, macular edema will develop. About one in a hundred operated on develops a pool of water under the retina within a few weeks after the procedure.
This clinical picture is called cystoid macular edema designated. To prevent this complication, anti-inflammatory drugs (mostly non-steroidal anti-inflammatory drugs or steroids, possibly a combination of these two active ingredients) can be placed directly in the eye. Especially in high risk patients, e.g. This prophylactic therapy is necessary for diabetics.
Read more on the subject below: Cataract surgery
What is cystoid macular edema?
Cystoid macular edema (also known medically as CME) often forms after cataract extraction. A CME caused by cataract surgery is known as Irvine Gass Syndrome. Other causes for the development of a CME are eye injuries, drug side effects or the occlusion of a retinal vein. Cystoid macular edema is characterized by the accumulation of small, fluid-filled vesicles in the area of the macula on the retina. The swelling squeezes the central optic nerve and leads to visual disturbances.
It is unclear why cystoid macular edema mainly occurs after cataract operations. In most cases the swelling subsides successfully after treatment with medication (eye drops containing cortisone or local injections) and the symptoms improve quickly.
What is diabetic macular edema?
Patients with diabetes mellitus may develop macular edema as their disease progresses. This form is called diabetic macular edema (DME). With diabetes, the small blood vessels in the eye are damaged more and more over time and the retina becomes infected. Doctors call this clinical picture "diabetic retinopathy". This disease often affects people with high blood sugar levels in particular. For this reason, optimal blood sugar control is an important factor in reducing the risk of developing diabetic macular edema.
The retinal disease goes unnoticed for a long time. Ultimately, there is a significant deterioration in vision and even blindness. The eye examination reveals macular edema as well as other pathological changes in the eye. The accumulation of fluid presses on the optic nerve, thereby contributing to the deterioration of eyesight. The therapy of diabetic macular edema takes place using special drugs and laser treatment of the retina.
Read more on the subject below: Diabetic retinopathy



.jpg)