Wegener's granulomatosis
Synonyms in a broader sense
Wegener's disease, allergic angiitis and granulomatosis, Klinger-Wegener-Churg syndrome, Wegener's granulomatosis, giant cell granuloarteritis Wegener-Klinger-Churg, rhinogenic granulomatosis
definition
The Wegner’s granulomatosis is a condition in which the small blood vessels throughout the body become inflamed (systemic vasculitis).
Tissue nodules form (Granulomas).
Mostly the ears are here, respiratory tract, lung and kidney infested. The Blood vessels are doing this necrotic-granulomatous changed.
Epidemiology / incidence in the population
Wegner’s granulomatosis is relatively rare, it occurs in around 5-7 people per 100,000. Women get sick less than men, the disease occurs most frequently around the age of 50, but cases have also been reported in which children and adolescents became ill.
Symptoms
Often the Wegner’s granulomatosis with constant bloody sniff, Epistaxis and chronic nasal congestion. Also Sinus infections can go along with it.
Otitis media (Otitis Media), Earache, dizziness up to numbness can also occur both at the beginning and in the course.
In the course it often comes to hoarseness, dry cough and joint and Muscle aches.
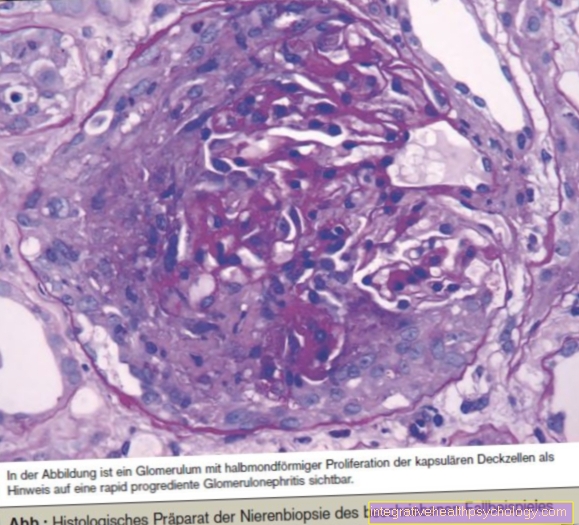
Inflammation of the kidney vessels (Glomerulonephritis) is common in the course of the disease.
It can also cause eye pain, eye inflammation and even visual disturbances, as well as changes in the skinhow bleeding, red spots and nodules come.
Pathogenesis
The exact cause is not yet known. It is certain that it is an inflammation of the vessels in the body (generalized Vasculitis) by Autoimmune antibodies acts. The associated antigen is not known; inhaled allergens and infestation with, among other things, are discussed Staphylococcus aureus.
diagnosis
Since the symptoms can vary greatly, the diagnosis of Wegener's granulomatosis requires laboratory, microscopic (histological) and clinical findings.
A tissue removal (biopsy) possible, in this microscopic examination one can see increased cells in a certain form (Granulomas) as well as dying cells (necrosis) see.
If the kidneys are involved, typically altered kidney cells can be seen in a kidney biopsy.
A blood test for certain auto-antibodies (usually c-ANCA, more rarely p-ANCA) is also required. These antibodies are directed against the body's own white blood cells (Leukocytes, in particular neutrophil granulocytes). The abbreviation ANCA stands for Anti-Neutrophil-Cytoplasmic Antibodies.
Markers of inflammation (such as CRP) may also be increased in the blood. Creatinine can also be increased if Wegner's granulomatosis has involved the kidney.
Changes in the lungs (granulomas and scars) can often be seen on an X-ray or CT scan.
therapy
At the beginning of Wegener's granulomatosis, the antibiotic clotrimazole (broad spectrum antibiotics with the following ingredients) is often used Trimethroprim and Sulfamethoxazole), e.g. available as Cotrim®, prescribed, which leads to an improvement, although the mode of action is still completely unclear here.
In the further course, cortisone (trade names e.g. Prednisolon®, Prednihexal®, Decortin®) is usually treated.
This can be done with immunosuppressive drugs such as Combine methotrexate (trade names: Lantarel®, Metex®, Neotrexat®) and cyclophosphamide (trade names: Endoxan®, Cytoxan®, Procytox®, Neosyn®).
However, these belong to the class of chemotherapy drugs and have corresponding side effects.
For some time now, monoclonal antibodies have also been available, which also dampen the immune system. Infliximab (available e.g. as Remicade®) is such an antibody, it blocks a receptor (TNF-alpha blocker). Since the production of such antibodies is very expensive and the treatment with such antibodies can lead to severe hypersensitivity reactions, it is only used in patients who do not react to methotrexate.
Patients in whom Wegener's granulomatosis does not improve after administration of cortisone in combination with methrotrexate are given the option of mycophenolate mofetil (trade name CellCept®) as a reserve drug.
In very severe cases with kidney failure requiring dialysis or life-threatening lung bleeding, plasmapheresis is the method of choice.
Other drugs that are used less often for therapy are:
- Etanercept (e.g. Enbrel®)
a genetically engineered protein, has an immunosuppressive effect - Ciclospoprin A,
an immunosuppressant - Leuflunomide (e.g. Arava®)
an immunosuppressant - Rituximab (e.g. MabThera®)
Monoclonal antibody similar to infliximab
As maintenance therapy, after the acute condition has improved, cortisone is prescribed in decreasing doses and an immunosupressant such as Azathioprin® (e.g. Collisan®, Imurek®, Zytrim®).
In addition, antibiotics such as Cotrim® are still given to prevent the nasopharynx from being colonized and infected by Staphylococcus aureus.
forecast
Without therapy, the Wegener's granulomatosis almost always closed Kidney failure as a result of kidney inflammation within 6 months and thus death. Targeted therapy improves the condition significantly in more than 90%. Temporary freedom from symptoms can even be achieved in ¾ of all patients. Symptoms may come back in about half of patients and will need to be treated again.
Complications
The Wegner’s granulomatosis can lead to permanent damage such as Hearing loss, one-sided Blindness, impaired kidney function. It can also lead to changes in the shape of the nose due to the frequent inflammation and thus to the development of a Saddle nose.