Peri-implantitis
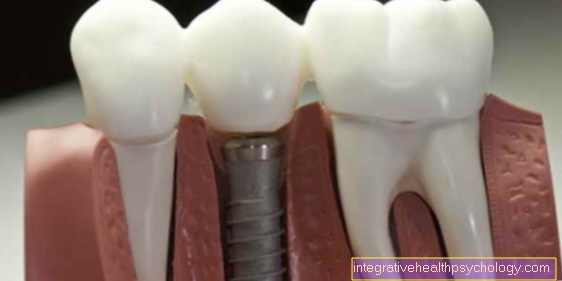
An inflammation on the dental implant is a so-called “peri-implantitis”, which can be described as 2 different types. On the one hand, there is what is known as peri-implant mucositis, in which the inflammation is limited to the mucous membrane surrounding the implant. On the other hand, peri-implantitis is described, which has spread to the bony implant bed. Peri-implantitis is always preceded by peri-implant mucositis. In the worst case, peri-implantitis can lead to implant loss and therefore requires adequate treatment at an early stage.

Causes / Risk Factors
In peri-implantitis, a distinction is made between local and systemic risk factors. The local risk factors are causes that affect the implant itself. The systemic risk factors, however, are causes that affect the patient.
In general, it can be said that a dental implant is in close contact with the intraoral environment and therefore also with the bacteria located there. A firm, connective tissue, peri-implant closure to the oral cavity should be ensured to prevent bacterial colonization in this area. In the area where the implant breaks through the gums or the mucous membrane, a so-called sulcus is formed. This is where plaque and bacteria accumulate and, in the event of improper cleaning or certain risk factors, inflammation and, in the worst case, loss of the implant.
Please also read: Dental implant removal, shelf life of dental implants
Local risk factors
Above all, the lack of the so-called “keratinized gingiva” is described as the cause. This is an area of the gum that is fixed in place on the bone. When placing an implant, it is important that this area is at least 2mm wide so that the implant can heal. The dentist should therefore make sure during the planning that this width is given, as otherwise the gums must be surgically widened at this point before implantation.
Read about this: Gum transplant
In addition, fixed dentures can pose a local risk, as can cement residue. The cement residues can come, for example, from previously inserted dentures. They remain in the oral cavity and eventually lead to inflammation.
Systemic risk factors
There are several causes of inflammation on the dental implant that can be traced back to the patient. The most important example here is the lack of oral hygiene. The patient should practice regular dental care and especially clean the implant with special interdental brushes. On the other hand, smoking has to be mentioned here, because tobacco consumption is the greatest risk factor.
In addition, patients with general illnesses such as diabetes mellitus are increasingly diagnosed with peri-implantitis, as well as in patients with pre-existing periodontitis. Other risk factors are:
- Medication (e.g. immunosuppressants),
- hormonal changes,
- irregular dental check-ups
Read more on this topic at: Proper care of a dental implant
diagnosis
Inflammation on the dental implant can be diagnosed by probing the gums and an X-ray. Both should be done by a dentist, which makes an appointment with them inevitable. No reliable diagnosis can be made without a professional examination.
By carefully probing with a periodontal probe, the dentist moves along the gum line of the implant and checks whether there is any inflammation in this area. If this is the case, an X-ray image is made, which can clearly confirm the suspected diagnosis.
A distinction is again made between peri-implant mucositis and peri-implantitis. By measuring the probing depths and evaluating the x-ray image, the dentist can differentiate between the two clinical pictures.
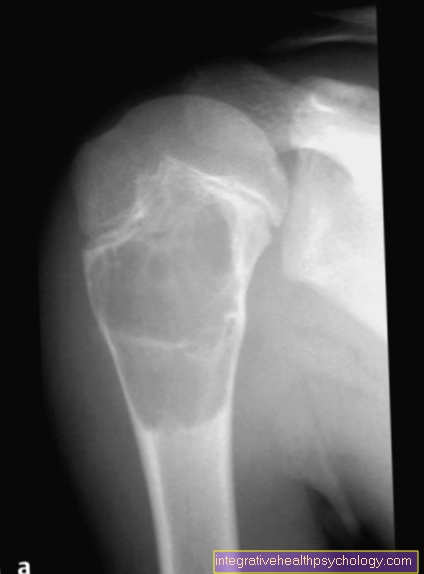
What can you see on the x-ray?
By taking an X-ray, it can be seen whether bone loss has taken place in the area of the implant. It can be extremely helpful to compare current X-ray images with older ones in order to better identify changes in this area.
Horizontal and vertical bone loss can be verified in the X-ray image, and the severity of the bone loss can also be shown. The more advanced the peri-implant bone resorption, the larger the bone defects on the X-ray.
frequency
The frequency of inflammation in dental implants is very difficult to predict in general terms. However, the current data suggest that up to 43% of patients develop peri-implant mucositis and around 22% develop peri-implantitis. However, the data are difficult to collect because the proportion of patients with healthy peri-implant relationships has not been accurately determined.
Nevertheless, it can be seen from this how important the correct implant and oral care is, so that inflammation in this area can be minimized and the loss of the implant can be prevented.
These symptoms could indicate inflammation on the dental implant
As already mentioned, only the dentist himself can confirm the diagnosis of peri-implantitis. Regular checkups at the dentist are therefore the best protection to prevent inflammation. However, there are symptoms that indicate peri-implant mucositis / peri-implantitis that you can recognize yourself.
- For example, you can perform a close eye inspection to look for plaque in the area of the implant.
- You may also notice spontaneous bleeding and pus secretion, which serve as clues. These can also be provoked by carefully touching with the finger, which would not be the case in healthy conditions.
- There may also be slight pain to the touch in this area, although some patients notice it less than others.
- In the advanced stage of peri-implantitis, the gums recede, which can make the implant surface visible.
- Often a sweetish halitosis is also noticeable, which can be caused by the inflammation.
Pain
If there is inflammation in the area of the implant and thus peri-implant mucositis, the patient may feel a slight pain to the touch. It is also possible that the dentures themselves, for example the crown on the implant, are painful. Often the gums are reddened and with an already existing peri-implantitis there is a secretion of pus in the area of the implant. If there has already been massive bone loss, pain in the jawbone can also occur.
pus
If the peri-implant mucositis has already developed into peri-implantitis, in the course of the inflammatory process, in addition to bleeding on probing (called BOP at the dentist), pus can also be secreted. This is visible and often perceptible to the patient through an unpleasant taste.
therapy
Treatment for inflammation on the dental implant can be surgical or non-surgical depending on the severity. In addition, the therapy for peri-implant mucositis differs from that of peri-implantitis.
Therapy of peri-implant mucositis
Non-surgical therapy:
- First of all, the inflammation should be eliminated. This is done through Reduction of implant surface contamination. Here, the surface of the implant is cleaned by the dentist or oral surgeon with special equipment and the bacterial film is removed.
- In addition, antibiotic therapy is also discussed in the literature. The use of chlorhexidine solutions (CHX) can reduce the probing pockets measured in depth around the implant.
- In addition, the dentist often orders local antibiotic therapy for 10 days, which can also lead to a reduction in inflammation.
Therapy of peri-implantitis
Non-surgical therapy:
- Here, too, the aim is to clean the implant surface using special instruments. The aim is to eliminate the clinical signs of infection. Ultrasound or laser therapies can be used here.
- As with peri-implant mucositis, antibiotic therapy with CHX solutions and local antibiotics are often recommended.
Surgical therapy:
In surgical therapy, in addition to eliminating the infection and reducing the probing depths, the bone level should also be stabilized, since bone loss has already occurred in peri-implantitis. Here it is decided individually with the surgeon which therapeutic measure is most suitable. The following options are used:
- Flap surgery,
- Flap surgery + resective measures,
- Flap surgery + bone grafting materials,
- Flap surgery + resective measures + bone building materials.
What exactly is meant by the various methods and what risks a surgical procedure entails should be discussed in detail with the dentist in each case.
These antibiotics are used
Two different drugs have established themselves in antibiotic therapy.
- Doxycycline and Minocycline (broad-spectrum antibotics from the group of tetracyclines).
In the case of certain allergies and intolerances, the patient should always consult the doctor in order to find a suitable alternative medication.
Read more at: Tetracyclines
Duration
The duration of a treatment cannot be predicted, as it is always individual and depends on the patient. It should be noted, however, that regular, professional tooth cleaning with special cleaning of the implant is essential for maintaining an implant.
With regular check-ups, for example, peri-implant mucositis cannot develop into peri-implantitis in the first place. These regular checks should always be carried out.
More about this topic can be found: Professional teeth cleaning
costs
The implantation is a private service that is not covered by statutory health insurance. It is the same with the therapy of peri-implant mucositis or peri-implantitis. The costs must be borne by a private account.
They depend on the chosen procedure and the necessary additional services depending on the complexity of the case. It always depends on whether a surgical procedure is necessary or whether it is just a mechanical removal of the deposits on the implant (non-surgical therapy). In any case, you should discuss the costs with your dentist in order to avoid a surprise in the invoice amount.
This article might also interest you: Cost of a dental implant