Middle finger pain
definition
Pain in the middle finger (digitus medius) can have many causes and can affect everyday life.
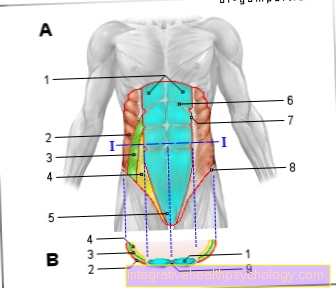
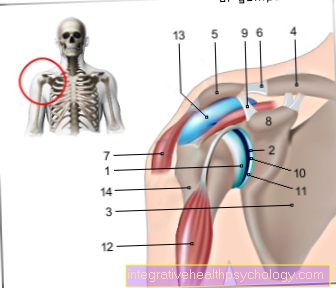
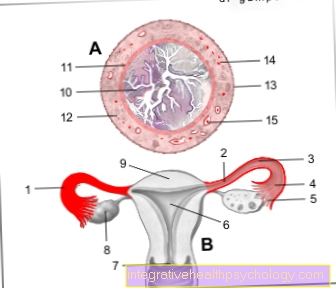
The middle finger - like all fingers with the exception of the thumb - consists of three bones (phalanges). These are also known as the phalanx proximalis (close to the body), phalanx media (middle) and phalanx distalis (far from the body) and are attached to one another by straps. The phalanx proximalis near the body is connected to the metacarpal bones by the metacarpophalangeal joint. Here, too, tapes provide an attachment.
Tendons, muscles, bones or joints can be damaged by injuries or wear and tear and cause pain in the middle finger - and in all other fingers.

causes
On the one hand, so-called degenerative diseases (wear and tear) can be responsible for pain in the middle finger. This includes, for example, osteoarthritis. This leads to damage to the articular cartilage between the individual phalanxes or the base phalanx and the metacarpal bone. The wear and tear on the cartilage causes pain when moving the joints in the middle finger.
Osteoarthritis can appear as a symptom of old age, as a result of hormonal changes (for example during the menopause), genetically or as a result of previous injuries or overload. Joint inflammation (arthritis) can also cause pain in the middle finger. Furthermore, injuries with the following sprains, strains or a broken bone can be responsible for pain in the middle finger. In rare cases, nerve damage - for example from injuries or in the presence of longstanding diabetes mellitus - can cause pain in the middle finger.
Tendinitis
The tendons of the finger muscles run in separate tendon sheaths, which protect the tendons and produce a slimy protective fluid to reduce friction. When the tendons are subjected to extreme stress, the tendon sheath can react irritably and painfully to the unusual movement. This is especially the case when starting new, unfamiliar physical work or rapid increases in stress in sport.
The tendon sheath becomes inflamed due to the friction and causes severe pain with every movement, as well as additional swelling, overheating and redness. To treat tendonitis, the finger must be spared long enough for the irritation to completely subside.
- Tendinitis
Snap finger
The snap finger or “quick finger” is a disease of the flexor tendons of the finger. It is a form of inflammation in which the flexor tendon is thickened at the base joint of the finger and can no longer slide along there. As a result, a snapping finger occurs when trying to slowly flex and extend it.
The disease occurs mainly after particular strain on the fingers, as can occur in certain sports, the use of individual musical instruments or craftsmen. In addition to snapping, the finger can also experience pain, tension, pressure pain and stiffness.
You might also be interested in this topic:
- Therapy of a flickering finger

I would be happy to advise you!
Who am I?
My name is I am a specialist in orthopedics and the founder of .
Various television programs and print media report regularly about my work. On HR television you can see me every 6 weeks live on "Hallo Hessen".
But now enough is indicated ;-)
In order to be able to treat successfully in orthopedics, a thorough examination, diagnosis and a medical history are required.
In our very economic world in particular, there is too little time to thoroughly grasp the complex diseases of orthopedics and thus initiate targeted treatment.
I don't want to join the ranks of "quick knife pullers".
The aim of any treatment is treatment without surgery.
Which therapy achieves the best results in the long term can only be determined after looking at all of the information (Examination, X-ray, ultrasound, MRI, etc.) be assessed.
You can find me at:
- - orthopedics
14
Directly to the online appointment arrangement
Unfortunately, appointments can only be made with private health insurers. I ask for understanding!
Further information about myself can be found at -
Heberden osteoarthritis
Heberden's osteoarthritis is a term used to describe osteoarthritis that occurs for no reason (idiopathic). It usually has a genetic background. In Heberden's osteoarthritis, the joints between the middle and last phalanx (distal interphalangeal joints, DIP) are particularly affected. These can affect not only the middle finger but also every other finger on the hand.
Heberden's osteoarthritis affects women more often than men. In addition to the pain, lumps can develop on the back of the hand at the end joints of the fingers. These are also known as Heberden nodes.
Read more on this topic at:
- Finger osteoarthritis
Bouchard arthrosis
Bouchard arthrosis is also arthrosis without a specific cause. In contrast to osteoarthritis of the heel, this occurs less often and mainly affects the joints between the middle and near-body phalanx (interphalangeal joints, PIP).
Men and women are affected roughly equally often. In Bouchard arthrosis, the middle finger joints of the middle finger can cause pain as well as lumps.
gout
Gout is considered to be a disease of affluence and often occurs when too much purine-containing foods (meat, legumes, fish, beer) are consumed.
The purine from food is converted into uric acid. If a higher uric acid level is reached in the blood, the uric acid salt is mainly deposited in the small joints of the fingers and toes. In an acute attack of gout, inflammation usually affects only one joint, which is known as monarthritis.
The joint in the big toe is most commonly affected, but any other joint can also be affected. Therefore, the joints of the middle finger can be inflamed and swollen from an acute attack of gout. The pain mainly occurs at rest. Recurring attacks in the middle finger joints can wear out the joints and lead to osteoarthritis. Therefore, gout should definitely be diagnosed and treated.
More information on this topic:
- gout
rheumatism
Rheumatoid arthritis is called rheumatism and is a chronic inflammatory autoimmune disease of the joints. Small joints, such as finger joints, are particularly affected. In addition to the middle finger, other finger joints are usually also inflamed, which is called Polyarthritis is called.
It is also important that both hands are symmetrically affected and that the finger end joint (DIP) is almost never affected. In addition, the pain persists even at rest. In the morning the joints are rather stiff and need some time - usually more than half an hour - before they can be moved normally. Even with rheumatism, rough lumps under the skin, so-called rheumatic nodules, can occur.
Read more on the subject at:
- rheumatism
Psoriatic arthritis
Psoriatic arthritis is an inflammation of the joints that occurs primarily in connection with psoriasis, affecting 5-45% of psoriasis patients. If the inflammation in the middle finger is triggered by psoriatic arthritis, it often affects the end and middle joints of the fingers (DIP and PIP). First, swelling of the entire middle finger of one or both hands is often observed.
This swelling is already painful. Joint destruction and possibly bone loss (osteoporosis) occur later.
Pain after an accident
If the finger is overstretched as a result of force, the middle finger can be sprained. Depending on how great the force was, it can lead to an unstable joint or damage to joint-forming structures with tears in ligaments or bony tears.
A finger dislocation or dislocation can also occur after an accident, in which the joint surfaces of the individual phalanges no longer have any contact or no contact at all. In addition to severe pain, the finger can usually no longer be moved normally and appears blocked in movement. Most of these injuries occur during sports, especially ball sports like volleyball or basketball. The middle finger can also break on one of the three bones, causing pain. A finger is often trapped, for example in a car door, leading to a broken bone.
You may also be interested in this topic:
- Bruise of the finger
Assessment of the pain depending on the location
Middle finger joint pain
Rheumatoid arthritis (rheumatism) mainly affects the metatarsophalangeal and median joints. If the middle finger joint (MCP) is affected on one side, the middle finger of the other hand is usually symmetrical.
The arbitrary involvement of the middle finger joint or any other finger joint suggests gout.
Middle finger joint pain
If pain in the middle finger joint (PIP) occurs, it may be rheumatism. The joint of the other hand is usually also affected.
In rare cases, so-called finger polyarthrosis (Heberden's arthrosis) can cause pain in the middle finger joint of the middle finger and in all other fingers.
Pain in the middle finger joint
Middle finger end joint pain (DIP) is primarily caused by psoriatic arthritis or Heberden's osteoarthritis. Psoriatic arthritis affects either the end joints almost exclusively or the entire joints of the middle finger.
So if the metacarpophalangeal joint, metacarpal joint, and terminal joint are affected, this is also referred to as radiation attack.
Would you like to learn more about this topic? Then read our next article below: Pain in the interphalangeal joints
Fingertip pain
The fingertip is one of the most sensitive areas of the human body. There are numerous nerve endings here, which ensure a particularly well-developed sense of touch. If the fingertip hurts, injuries to the bones, tendons and joints are rarely the cause. Often there are superficial injuries to the skin or abnormal sensations in the nerves, triggered by various diseases.
If there are no minor injuries to the skin, the pain is often harmless, caused by extreme cold or heat, unusual arm positions or heavy strain on the hands. Serious circulatory disorders or nerve disorders are rarely the cause. For example, diabetic polyneuropathy can be a disease of the nervous system that can begin with disorders of the sensory nerves on the fingertip.
Also read:
- Fingertip pain
Pain in the joint capsule
Pain in the middle finger that is triggered by a joint capsule injury is usually caused by a strain and a capsule tear. If the joint on the middle finger is severely overstretched, a joint capsule tear with dislocation of the finger (dislocation) can also occur.
Inflammation of the joint capsule manifests itself as pain, swelling, redness and overheating. This can be caused by overexertion of the joint.
Duration of pain
The duration also depends on the cause of the pain in the middle finger. In the event of a dislocation, the middle finger should be immobilized in the splint for 2-3 weeks.
A break can take up to 6 weeks. In general, physiotherapy should follow. With early treatment of osteoarthritis and rheumatism, the progression of the disease can be delayed, but there is no complete cure. In rheumatism, gout and psoriatic arthritis, there are individual, relapse-free processes that can be positively influenced by lifestyle and medication.
Concomitant symptoms
Accompanying symptoms of an injury to the finger from an accident can be swelling and restricted mobility.
In the event of a broken bone or middle finger dislocation, the individual phalanges of the fingers may be misaligned.
At a Psoriatic arthritis The typical skin appearance of psoriasis usually occurs years before the joint inflammation: These are sharply delimited, red spots that are covered by silvery scales. Preferably the rash occurs on the extensor sides of the arms and legs and on the lower back. Osteoarthritis is most likely characterized by pain.
If inflammation occurs, swelling, overheating and reddening of the affected joint on the middle finger can occur. In rheumatism, general symptoms such as night sweats, a slight fever or muscle pain can become noticeable. In addition to the joints, internal organs can also be affected in rheumatism. For example, if the heart is affected, it can lead to myocarditis, if the blood vessels are infected, it can lead to vasculitis, or if the eye is affected, conjunctivitis.
swelling
With swelling, there is an increased accumulation of fluid in the tissue.
It often occurs after acute injuries, but also with inflammation of any kind and chronic irritation. There can be various causes behind this. Even with minor injuries such as strained tendons, accompanying injuries can occur in the tissue, which lead to small bleeding. The blood flows into the tissue and leads to a bruise and an externally visible and painful swelling.
In order to prevent swelling, the finger must therefore be raised, cooled and compressed after the injury. If there is inflammation or irritation of the joints or tendons, the swelling occurs more slowly. However, these are joint fluids, pus and other inflammatory secretions. Here, too, cooling the finger helps to keep the swelling low.
Pain when moving
Much pain does not exist at rest, but only occurs when moving.
The flexion and extension movements of the middle finger are performed by tendons whose muscle bellies lie in the hand and forearm. The tendons can be painful after injuries but also from inflammation and make any movement difficult. This can be caused by torn tendons, strained tendons or muscle damage after injuries, but also tendonitis, snap fingers and chronic tendon changes with no apparent cause.
The finger joints can also cause severe pain when bending and stretching the finger. This can be due to injuries to the cartilage and bones or long-term chronic cartilage wear.
Pain when bending and stretching
The cause of the pain in the middle finger when bending or stretching can be all possible causes. Tendons, which are part of the muscles in the forearm, are responsible for flexing and stretching the middle finger. If these tendons are inflamed or torn, pain can occur, especially when flexing or stretching the finger.
The pain can also radiate to the hand or other fingers. For example, if the finger hurts when stretching in the morning after waking up, it may be the so-called morning stiffness, which often occurs with rheumatism. The pain then tends to be in or around the joint and does not radiate. The pain usually gets better after half an hour to an hour.
Furthermore, a joint misalignment, for example after an accident or a fall, can cause pain when flexing or stretching the finger. In most cases, this disease is also associated with a restriction of movement - i.e. incomplete flexion or extension.
Also read:
- Burning in the fingers
Nocturnal pain
Nocturnal pain can be very uncomfortable and prevent the person from sleeping, which in turn can exacerbate the symptoms. There can be several causes behind this. If the finger is injured, it is often necessary to immobilize and splint the finger. During sleep, in particular, the finger can be strained unnoticed and thus hurt.
Inflammation of the tissue can also be painful at night due to its sensitivity to pressure. Nerve diseases in particular, such as polyneuropathy, often become noticeable at night. The fingers can tingle and pain unbearably when they are at rest and when they are elevated. To improve sleep at night, the pain should be treated with adequate medication.
diagnosis
The suspected diagnosis is usually made through the questioning (anamnesis), symptoms and the clinical picture. In the event of an accident in which the middle finger was broken, for example, the circumstances of the accident are important. To find out where the break is, how strong the break is or whether other structures such as ligaments, tendons or muscles are injured, imaging procedures such as X-rays, CT or MRI can help.
In the case of joint inflammation or gout, a blood count is often necessary. In gout, for example, there is an increased level of uric acid in the blood. In rheumatism, in addition to an increase in inflammation levels such as CRP, antibodies can also be detected. This includes, for example, the so-called rheumatoid factor - an autoantibody which, however, can also be increased in healthy people or during an infection. The measurement of the anti-CCP antibody in the blood, which indicates rheumatoid arthritis, is more reliable. In arthritis and osteoarthritis, x-rays are important for assessing the course and joint wear.
You might also be interested in:
- Diagnosis of osteoarthritis
- MRI of the hand
Treatment of pain in the middle finger
Therapy for pain in the middle finger depends on the cause.
In general, swelling of the finger should be cooled, regardless of the underlying cause. In addition, in almost all cases short or long-term physiotherapy and physiotherapy are necessary to achieve healing (for example after a fracture) or to delay late damage (for example in rheumatism).
If the middle finger is sprained or strained, no further treatment is usually necessary. The finger should be spared, however. In the event of a dislocation, the middle finger is brought back into the correct position as quickly as possible by gently pulling and / or pressing. This is usually done under a local anesthetic. Then the finger is placed in a splint made of plastic or plaster of paris. Immobilization of the middle finger is also necessary in the case of torn ligaments or torn bones.
In some cases - especially with severe instability of the joints or larger tears - surgical treatment of the finger is necessary. This is done using wires or screws that do not necessarily have to be removed after healing.
Various drugs are used for rheumatism. On the one hand, these are NSAIDs (non-steroidal anti-inflammatory drugs) like Ibuprofen®. On the other hand, glucocorticoids are used in acute attacks to contain the inflammation and prevent joint wear. For long-term drug therapy, so-called DMARD used like methotrexate. The DMARDs fight the autoantibodies that cause joint wear and, in the best case, ensure a temporary or permanent one Recovery (remission).
In the case of osteoarthritis, painkillers are also used. In severe cases, surgical therapy can be used. NSAIDs and glucocorticoids are also administered in acute gout attacks. In general, gout should lead to weight reduction. In addition, purine-containing food and alcohol should be avoided. In symptomatic gout, allopurinol, which reduces the formation of uric acid, should be given.