What are the symptoms of bronchial asthma?
introduction
The symptoms of bronchial asthma can appear at different times, depending on the severity, the triggering stimulus and the severity of the disease, and it may be affected sporadically, seasonally or throughout the year.
Asthma attacks with the specific symptoms are only the “tip of the iceberg”, even during an apparently symptom-free interval, bronchial asthma can be detected through the underlying chronic airway inflammation.

Typical symptoms of asthma brochiale
The following is an overview of the typical symptoms of asthma. These are then discussed in more detail.
- shortness of breath
- shortness of breath
- Breathing noises such as wheezing (wheezing) and humming
- to cough
- Expectoration
- Chest tightness
- Increased breathing rate
- Increased heart rate
- fear
Shortness of breath
The sudden onset of shortness of breath is the main symptom of an acute asthma attack.
In the interval, i.e. the phase in which there is currently no acute attack, the patients are usually symptom-free, and shortness of breath rarely occurs. Usually in an acute asthma attack shortness of breath develops first, which can increase to significant shortness of breath within a few minutes. In bronchial asthma, it is particularly difficult to breathe out. Breathing noises occur when they exhale, and the patient feels as if they can no longer get the air out of the lungs. Therefore, certain postures are often assumed unconsciously.
In the event of an acute asthma attack, the so-called coachman's seat helps to make exhalation a little easier. The patient is sitting upright with his arms and hands resting on his thighs or knees. In this posture, the so-called auxiliary breathing muscles which are located in the chest, back and stomach area are activated. This makes exhalation a little easier. The use of the so-called lip brake often helps patients with acute shortness of breath in an asthma attack to improve their breathing a little. The lips are pursed when you exhale so that you exhale against resistance. That sounds paradoxical at first, but for many patients it is a little help to improve breathing in an acute attack.
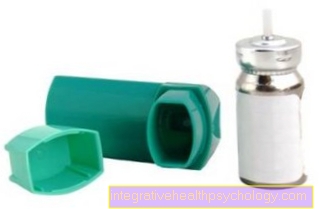
However, in the event of acute shortness of breath in the context of an asthma attack, the immediate use of an appropriate emergency spray is essential.
Further information: Breathing exercises for asthma
Breath sounds
As already mentioned, there are certain breathing noises, especially during an asthma attack, which occur more intensely when exhaling. Wheezing or humming are typical, which are explained below.
Wheezing
In medical jargon, there are two typical breathing sounds that can occur during an acute asthma attack: wheezing and humming. Both sounds arise mainly during exhalation (exhalation).
The wheezing occurs when the airways are narrowed during an acute asthma attack. The air flowing out of the alveoli via the bronchial tubes must therefore come through a narrower path than is normal. The resistance against which the air has to escape is greatly increased. The escape of air against the significantly increased resistance is called wheezing. It is a whistling sound that can be heard as you exhale.
Hum
The humming is also a noise typical of asthma. It can also be heard mainly during exhalation and is caused by the increased production of thick mucus during an asthma attack.
In many cases, the wheezing and humming typical of asthma can only be heard with the stethoscope. However, if the seizure is severe, the sounds can be heard without a stethoscope.
Mucous bronchi
Bronchial asthma is a disease in which the airways react chronically over-sensitive to external stimuli. One speaks of a hyperresponsive bronchial system. Inflammations in the area of the bronchial mucous membrane occur again and again. The hypersensitive airways react to certain triggers with a sudden swelling. This leads to the narrowing of the airways.
In addition to the swelling, there is a massive increase in the production of tough mucus within a short period of time. This mucus also leads to a reduction in ventilation of the lungs. It is usually difficult to cough up the mucus in an acute attack. A relatively recent study has shown that the production of thick mucus may not be just a symptom, but a kind of cause of the development of asthma. In animal models it was shown that a genetically determined dry lung mucosa increases the risk of the production of tough mucus. This mucus, in turn, increases the risk that the airways will become hypersensitive to certain triggers such as allergens in the first place.
More on this under our topic: Slimy Brochia
to cough
Coughing is a typical symptom of an asthma attack.
In an acute attack, the bronchial mucous membrane increasingly produces tough mucus. This leads to additional irritation of the respiratory tract and an urge to cough. The counting, glassy secretion is difficult to cough up. The cough does not only occur in an acute attack but can also be a chronic companion in bronchial asthma. Coughs that show up outside of an acute asthma attack often appear as a dry, irritating cough. Asthma patients suffer more from coughing at night. It is not uncommon for patients who have not yet known asthma to have a chronic cough in the first place for a presentation to the doctor.
You may also be interested in this topic:
- Causes of bronchial asthma
- cough
Expectoration
Much thicker mucus is produced by the bronchial mucosa during an acute asthma attack. Therefore, in an acute attack, a productive cough, i.e. cough with expectoration of mucus, often occurs. Since the mucus produced is relatively tough, it is often difficult to cough up.
In the interval, i.e. outside of an acute asthma attack, the cough of asthmatics is usually rather dry and rarely accompanied by clear expectoration.
Racing heart
Palpitations are not a characteristic symptom of asthma.
However, an acute asthma attack puts a lot of stress on the body. The airways constrict, causing shortness of breath. This often leads to an accelerated heartbeat up to palpitations (tachycardia). The racing heart quickly subsides after adequate treatment of the asthma attack.
fatigue
Nocturnal symptom activity also plays an important role in the therapy of bronchial asthma. The fact that asthmatic symptoms can occur more often at night is due to the fact that the airways are particularly narrow in the early morning hours. During this time, asthma sufferers experience symptoms such as coughing or shortness of breath.
If this is always the case, the clearly disturbed night sleep can lead to chronic daytime sleepiness. It is therefore very important to inform the doctor about the nocturnal symptoms. The asthma therapy must then be adjusted so that nocturnal symptoms disappear as completely as possible.
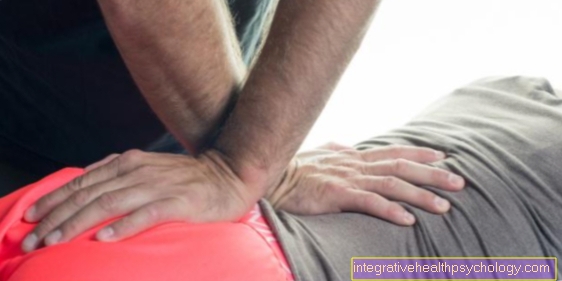
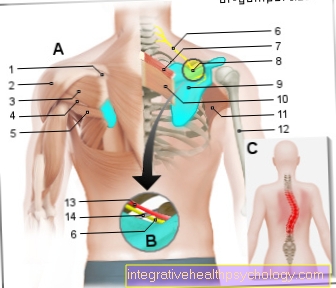
Back pain
Back pain is an atypical symptom of asthma.
If back pain and asthma occur together, this can be an indication of two different causes for the symptoms. Chest pain or tightness in the chest area is more likely to occur during an acute asthma attack. This can be caused by the narrowed airways.
Symptoms of an asthma attack
An acute asthma attack usually begins with a rapidly increasing shortness of breath which ends in a more or less pronounced shortness of breath.
Often there is an accompanying cough which is accompanied by a thick sputum. The shortness of breath can lead to other symptoms such as tightness in the chest or anxiety. Other possible symptoms caused by shortness of breath and the resulting physical stress are an increase in the respiratory rate (tachypnea) and a racing heart (tachycardia). When you breathe out, you can hear the typical asthma breathing noises, the so-called wheezing and humming.
Read about it too Asthma attack
Breathing in bronchial asthma

Exhalation:
The lungs contract like a loose rubber band!
Inhalation:
The diaphragm tightens and pulls the lungs down, air flows
Asthma from medication
Certain medications can trigger an asthma attack.
Certain pain relievers (analgesics) in particular can trigger an acute asthma attack. One therefore speaks of analgesic asthma. In particular, the active ingredients acetylsalicylic acid (ASA in aspirin) and drugs from the group of non-steroidal anti-inflammatory drugs (NSAIDs) such as indomethacin, ibuprofen and diclofenac can provoke an asthma attack in asthmatics.
Beta blockers can also trigger an asthma attack, as some beta blockers have a constricting effect on the bronchial muscles. Therefore, patients with known bronchial asthma should only take beta-blockers under the direction of a doctor and when absolutely necessary.
Asthma after exercise
There are forms of asthma that are triggered by physical exertion. One then speaks of exertion asthma or exertion asthma.
The asthma attack can occur relatively at the beginning of the exercise but also only after the end of the exercise. Desiccation of the bronchial mucous membrane due to increased breathing during exertion is discussed as the cause of exercise asthma. This should lead to irritation of the already hypersensitive bronchi. Another theory behind the development is that inhaling more cold air leads to a cold stimulus in the bronchi.
If stress asthma occurs, asthma therapy should be discontinued. The aim is to have complete control of the asthma even under physical strain. Another option is to take an asthma spray a few minutes before you plan to exercise.
Asthma from stress
Stress is not the sole cause of asthma attacks.
However, patients who suffer from asthma and are exposed to increased stress are often at an increased risk of suffering an asthma attack. This is why mental hygiene with avoiding stressful situations also plays a role in coping with the illness of asthmatics.
Summary
During an asthma attack, the airways narrow in response to external stimuli, there is shortness of breath, breathing is visibly difficult and exhalation (clinically known as expiration) is often accompanied by a whistling sound, which is clinically known as expiratory stridor or wheezing.
In addition, there is a symptom of a lengthening of the breathing phases. While inhalation (clinically known as inspiration) takes longer than exhalation in normal breathing, this ratio is shifted and may even be reversed during an acute asthma attack.
In order to make breathing easier for themselves, the asthmatic usually involuntarily adopts a sitting position and supports his arms during an acute bronchial asthma attack. As a result, muscles that attach to the arm and pull towards the chest are reversed in their actual function and, as auxiliary breathing muscles, can raise and lower the chest (thorax), which makes breathing easier. In addition, the attack is usually accompanied by a pronounced urge to cough and an increase in the heart rate, which can be seen from an increased pulse rate. Symptoms of a blue lip color, clinically known as cyanosis, may also appear, which indicates decreased blood oxygenation.
Exhalation is particularly difficult in the case of a bronchial asthma attack.
This is due to a fundamental difference in the process of inhalation and exhalation. While breathing at rest, the chest expands with the help of the respiratory muscles and a negative pressure is generated in the lungs by the diaphragm, which pulls the breath into the lungs like a suction. (seesee graphic below)
Exhalation, on the other hand, is not supported by muscles, so it is done passively by the restoring force of the lungs. There are also muscles that can support exhalation, but they only play a role in increased breathing and are therefore poorly developed. Asthmatics can, however, train them to relieve their shortness of breath during a bronchial asthma attack.
As the attack lasts, symptoms of exhaustion and confusion set in, caused by the great effort required to breathe and the increasing oxygen supply to the brain.
A bronchial asthma attack can last a few seconds, hours and in extreme cases days. If left untreated, a severe asthma attack can also be fatal; this is called status asthmaticus.
What is often not mentioned is the great fear that a patient develops during an asthma attack. It can go as far as a feeling of annihilation and must be taken into account as an additional factor, since it increases the patient's level of suffering and can additionally worsen the attack.
In the interval between two attacks, asthmatics are often symptom-free, coughing can be the only asthma symptom for a long time and is often misinterpreted as chronic bronchitis! Asthma attacks are therefore only the tip of the iceberg!