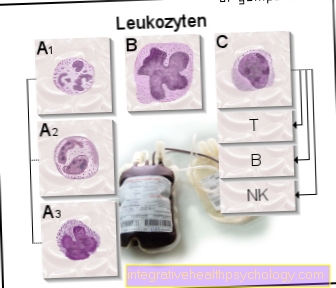
Sturge Weber Syndrome
definition
The Sturge-Weber syndrome, which is also known as encephalotrigeminal angiomatosis, is a chronically progressing disease from the so-called group of neurocutaneous phacomatoses.
It is a group of diseases of the nervous system and skin that are characterized by malformations.

In the case of Sturge-Weber syndrome, angiomas (German: blood sponge) develop. Angiomas are benign vascular tumors that can occur in the face, on the meninges and on the choroid of the eye (choroid). This can lead to further sequelae, which are triggered by the mass in the eye and on the meninges.
Outwardly, affected patients are noticed by a one-sided fire mark (nevus flammeus) on the face. These one-sided, usually dark red spots of different sizes in Sturge-Weber syndrome always also include the eyelid.
therapy
- Symptomatic treatment
- Cortisone therapy
- Anticonvulsants
- operative treatment
- Laser treatment
The Sturge-Weber syndrome cannot yet curative (healing) to be treated. The focus is on the therapy of the accompanying symptoms and regular medical control.
In order to ensure that the child's development is as uncomplicated as possible, special attention should be paid to the detection and treatment of an existing epilepsy disease (especially West syndrome). If the suspicion is confirmed, drug therapy is used Cortisone, cortisone-releasing drugs, or Anticonvulsants (Anti-seizure medication).
If the causal changes can be achieved surgically, epilepsy surgery can also be sought. Glaucoma can largely be treated with intraocular pressure lowering drugs or surgery. However, nerve fibers that have already been lost cannot be saved.
The flame mark can largely be removed by laser treatment, whereby only slight scarring occurs. Since the psychological strain often increases with the intensity of the Naevus flammeus early treatment in childhood is recommended before the mark changes over time.
If the illness has led to neurological or cognitive (mental) losses, it is important to support the children mentally and physically with all possible means. For this purpose, regular psychotherapy as well as physiotherapy and occupational therapy can be sought. A school education appropriate to their level of ability is also very important.
Life expectancy
Life expectancy does not necessarily have to be limited with Sturge-Weber syndrome.
If, above all, the fire mark is in the foreground of the disease and there are no incisive accompanying symptoms, the patient hardly differs from a healthy person.
The eye diseases associated with the syndrome also usually do not change life expectancy, even if they lead to blindness. Especially in countries like Germany nowadays it is no longer a problem to lead an almost unrestricted life even though you cannot see.
Life expectancy is limited primarily by the neurological disorders. The Lightning Nick Salaam fits (West syndrome) lead to death by the age of three in 25% of all affected children - whether they have Sturge-Weber syndrome or not. Due to the poor treatability, the consequences of the seizures and the insufficient supply of the affected hemisphere are very diverse.
Despite the symptoms, one child can go through almost normal development, while another suffers from a severe disability. If one summarizes all cases of Sturge-Weber syndrome, one must assume a reduction in life expectancy. However, each patient must be viewed individually.
Concomitant symptoms
- Eye diseases
- Fire mark on the face
- Neurological disorders
- epilepsy
- mental disability
- Headache attacks
The affected children often suffer from accompanying symptoms that are triggered by the benign vascular tumors. The phenomena are divided into two camps: diseases of the eyes and neurological disorders.
Serious epilepsy can develop in infancy, and it is often difficult to treat. The so-called Lightning Nick Salaam fits (also: West Syndrome) are characterized by a characteristic convulsive picture and are particularly harmful to the young brain. If left untreated, the seizures lead to severe brain damage or even death of the child.
The convulsions and the poor vascular status in the brain (caused by the calcified angiomas) lead to an insufficient supply. Depending on the extent, this can result in a delay in development or even intellectual disability.
If the patients are already a little older, they often describe recurring, migraine-like headache attacks. Damage to the tissue of the affected side of the brain (hemisphere) can also lead to hemiparesis. Since the right half of the body is controlled by the left brain and vice versa, the opposite side of the body is always affected by the paralysis. If this happens early in the course of the disease, it can reduce the development of the relevant extremities or even the entire body growth.
Eye symptoms
The most important accompanying ophthalmic symptom (Ophthalmology = Ophthalmology) is glaucoma. Glaucoma is also known as "glaucoma" and includes all pressure-related damage to the eye nerve. The pressure inside the eye can be increased, but it can also be completely normal.
In Sturge-Weber syndrome, the choroid (vascular layer) of the eye is also affected by angiomas. The outflow system of the eye fluid is obstructed by the proliferating vascular tumors, which in this case increases the intraocular pressure. The nerve slowly takes damage, which manifests itself in so-called visual field defects. The patients do not see “black” in the affected areas, but nothing at all. The area that is normally supplied by the affected nerve fibers is eliminated.
In addition to glaucoma, retinal detachments can also occur, which can also lead to blindness of the eye.
Symptoms on the face
The only characteristic shared by all patients with Sturge-Weber syndrome is the fire mark on the face. The so-called Naevus flammeus represents a cosmetic problem for those affected rather than having an actual disease value. The fire mark is a malformation of tiny vessels below the top layer of skin. The localization is based on the course and the coverage area of the Trigeminal nerve. This pathway belonging to the cranial nerves supplies the face with sensitive nerve fibers for pain and touch sensation. In the case of Sturge-Weber syndrome, the clearly delimited, reddish change always includes the eyelid on the affected side (this does not mean that any accompanying symptoms must appear on the eye).
Read more on this topic at: Fire mark
causes
The cause of the Sturge-Weber syndrome lies on the genetic level. As far as we know today, it is a somatic mutation.
This means that the disease is not inherited, but is triggered spontaneously by errors in the DNA of the disease carrier. The sequence of certain connections in the DNA, so-called base pairs, determines the blueprint for all cell components and enzymes in the human body. In Sturge-Weber syndrome, such a base pair is randomly exchanged, resulting in a defective product. The result is increased signal activity in certain cells, which promotes the growth of vessels - beyond the normal level. This creates benign vascular tumors, the angiomas.
Further information on the development of neurocutaneous syndromes can be found here: Neurocutaneous Syndrome
diagnosis
The fire mark can already be seen on the child's face at birth. The size changes as the patient grows. The color can also increase in intensity or fade. Computed tomography shows a loss of brain tissue (brain atrophy) on the affected side and increased calcification of the vessels. If the changes in the skull are so severe that epilepsy is triggered, this is diagnosed with the help of an EEG (electroencephalogram). An ophthalmological examination should also take place, since various components of the eye can be affected by the vascular changes and thus their function can be restricted.
Read more on the subject under: Brain atrophy (water head) and epilepsy
MRI
Magnetic resonance imaging (MRI) is also used in the diagnosis of suspected Sturge-Weber syndrome.
A contrast agent is used that can display the vessels particularly well. On the one hand, the detailed representation of the vascular system allows malformations to be recognized. Trained eyes - such as those of a radiologist - can then differentiate between natural variants and pathological changes when evaluating the images.
On the other hand, the contrast agent can cross the so-called blood-brain barrier if this is disturbed. This barrier is a cell system that separates the vessels or blood from the brain tissue and only allows selected substances to pass through. If the contrast agent gets through this blood-brain barrier, this indicates damage to the vascular cell system, which can be caused by deformities or severe calcification.